Mis à jour le Lundi, 1er Décembre 2025
15 des meilleures questions posées par les français et les anglais au fil des ans / 15 of the Best Questions asked by French & English people over the years
QUESTION I.
[FR] – En quoi consiste la théorie organique ?
[EN] – What is the Organic Theory About?
[FR] Réponse:
La théorie organique est une théorie du 21ème siècle principalement axée sur la conception de l’individu. Elle s’appuie sur l’école de pensée française après la révolution où l’individu embrasse ses propres choix et se définit par ses capacités, ses désirs et ses réalisations. Elle est également fondée sur la théorie de l’évolution, parce qu’elle considère l’individu comme un organisme façonné par son environnement, capable de s’adapter, d’évoluer et de changer en fonction des environnements psychologiques, sociaux et culturels dont il veut faire partie. Cependant, ce qui est unique dans la théorie organique, c’est que c’est la première théorie qui porte la conception unique de l’organisme individuel à un autre niveau, parce qu’elle reste centrée sur la structure des pensées et l’interprétation du monde en considérant ce qui compte pour l’individu et n’est pas fondée sur des généralisations d’hypothèses comme les théories anciennes, ce qui élimine beaucoup de confusion car elle déplace le point de focalisation sur ce qui compte pour l’organisme individuel unique.
Un autre aspect important de la “Théorie Organique” en tant que théorie scientifique que je voudrais éclaircir dans l’esprit des masses est qu’une théorie scientifique n’a rien à voir avec ce que la plupart des gens ont tendance à appeler des “théories générales”. Une théorie générale est une théorie commune qui est généralement utilisée pour expliquer au quotidien des questions d’importance parfois discutable liées à des questions sociales ; cet usage du terme “théorie” englobe généralement des croyances subjectives et des idées sur des sujets non liés à l’universalité de la vie humaine ou à la psychologie, mais plutôt des conversations sociales que la plupart des gens tiennent dans des endroits comme les cafés pour discuter et expliquer des raisons ou causes possibles sur des sujets communs comme “Pourquoi la Deuxième Guerre mondiale est-elle réellement arrivée ? “Pourquoi Jean a-t-il quitté son travail ?” ou “Pourquoi Jeanne a-t-elle épousé Jean ?”. Les explications à ces questions tendent à être qualifiées par la foule commune de “théorie”, et ce genre de théorie n’a absolument rien à voir avec une “théorie scientifique” telle que la Théorie organique.
Une théorie scientifique repose sur la combinaison de deux méthodes anciennes : le rationalisme et l’empirisme. Ces deux méthodes font de la science un outil puissant. Par exemple, les rationalistes affirment que la validité ou l’invalidité d’une proposition donnée peut être déterminée en appliquant soigneusement les règles de la logique. L’école de pensée empiriste soutient d’autre part que la source de toute connaissance est l’observation sensorielle, de sorte que pour les empiristes rigides, la vraie connaissance ne peut être dérivée de ou validée que par l’expérience sensorielle. Après des siècles d’enquête, nous avons constaté que le rationalisme et l’empirisme avaient tous deux une utilité limitée, de sorte que la science moderne a combiné les deux écoles de pensée, et depuis lors, les connaissances se sont accumulées à un rythme exponentiel.
Par conséquent, le mouvement rationaliste a ajouté son aspect à la science et l’a empêchée de simplement recueillir une gamme infinie de faits empiriques déconnectés, parce que nous, intellectuels, devons en quelque sorte donner un sens à ce que nous observons, donc, nous formulons des théories scientifiques. Une théorie scientifique a deux fonctions principales : (1) il organise les observations empiriques et (2) il sert de guide pour les observations futures et génère des propositions confirmables. En d’autres termes, une théorie scientifique suggère des propositions qui peuvent être testées expérimentalement dans une certaine mesure avec certaines méthodes statistiques réductionnistes. Si les propositions générées par une théorie sont raisonnablement confirmées par l’expérimentation, la théorie gagne en force ; si les propositions ne sont pas confirmées, la théorie perd de sa force. En science, l’observation est souvent guidée par la théorie.
La théorie organique est une théorie que j’ai présentée à la table intellectuelle, mais ses fondements étaient dormants dans la psychologie et la littérature scientifique pendant des décennies. Il semble que je n’ai eu qu’à rassembler ces observations objectives et à les organiser méthodiquement pour en arriver à la déduction et à la réalité qu’elle révèle. Nous ne sommes pas maîtres de notre vie, mais nous avons un grand contrôle sur notre propre conception individuelle basée sur nos désirs, notre éducation, notre direction, nos capacités et nos choix dans la vie.
La théorie organique suit la vision organique du monde qui existait déjà dans les grands débats psychologiques du siècle et j’ai construit sur cette perspective, l’ai affinée et étendue avec la littérature empirique et philosophique des temps modernes pour donner à l’individu plus de pouvoir de définition de soi dans notre société moderne et parfois confuse. En fait, j’ai aussi pris quelques concepts de Jacques Lacan pour donner à l’individu le pouvoir et la capacité de réaliser ses rêves et aussi pour ouvrir l’esprit de la foule environnante pour faire savoir et comprendre à la société que les gens ne sont pas des objets statiques, mais ont la capacité de se créer et de se récréer.
Le seul message fondamental de la théorie organique est que nous ne sommes pas simplement définis par l’endroit où nous sommes nés ou par les personnes qui nous sont liées que nous n’avons pas choisies, ou par les lignées sanguines, mais plutôt par nos propres choix, efforts, capacités, réalisations et orientations, et aussi par le fait que tout organisme peut être conditionné pour faire partie de l’environnement de tout autre organisme par le processus sans fin d’apprentissage et d’adaptation, comme le montrent les exemples d’Adolf Hitler ou de Napoléon Bonaparte, pour ne citer que deux cas célèbres de grands dirigeants issus d’une modeste éducation étrangère, qui ont grandi au plus haut niveau dans des pays où ils ne sont pas nés, mais se sont recréés pour devenir le cœur de ces nations à un moment donné.

Image: Le jeune Napoléon
La Théorie Organique démontre que la construction individuelle [formation], qui ” peut être ” mécanique et structurée dans son application [par exemple l’apprentissage à distance par texte / vidéo / audio], se développe indirectement pour créer et donner une dimension socioculturelle à l’individu une fois que les compétences souhaitées [modèles de communication et de comportement] ont été pleinement adoptées, maîtrisées et déployées dans la vie. Le terme ” social ” est aussi beaucoup trop vague pour être important en tant que tel… le terme ” social ” peut simplement être défini comme l’interaction [de tous types] entre organismes. Le terme ” social ” n’est donc pas vraiment valide sur le plan scientifique et il manque de précision puisqu’il peut se référer à un large éventail de variables. Il ne nous reste alors que les choix, le(s) langage(s) et les capacités de développement personnel de l’individu [par exemple la synthèse culturelle et psycholinguistique] : les facteurs majeurs dans l’explication psychologique et philosophique de sa conception singulière [à noter que chaque conception est unique à l’organisme humain individuel tel que ses empreintes digitales, sa forme crânienne ou sa structure corporelle : singularité]. Ainsi : formation, méritocratie, ordre et amour [simple… en théorie].

Marcel Gauchet l’a bien formulé en expliquant que quand on vit dans un monde structuré par la méritocratie républicaine et quand on est bon élêve, on sait qu’il y a des voies d’ascension sociale. Malheureusement et de façon choquante, dans certaines sociétés préhistoriques, ataviques, mal-informées et barbares encore gouvernées et hantées par des structures obscures, anciennes, peu sophistiquées et non scientifiques des Anciens régimes du Moyen Âge, un grand nombre de personnes sont encore forcées de croire à tort que l’individu est né pour être l’esclave de sa condition de naissance, vivre sur ses genoux dans une infériorité éternelle et être défini par les vues de leurs masses [pour la plupart] apathiques et misérables par conditionnement. Nous restons donc déterminés sur notre mission de changer la perception des esprits, car lorsque nous changeons les esprits, nous avons aussi un impact sur l’esprit de leurs enfants et petits-enfants ; l’impact de la psychanalyse sauve des générations de la misère et a un effet éternel.
“Les hommes de génie sont des météores destinés à brûler pour éclairer leur siècle.”
-Napoléon
Pour comprendre la logique simple de la conception individuelle de l’organisme unique, prenons l’exemple d’un homme profondément ancré dans la culture française et qui est aussi un grand professeur de littérature, mais qui a un fils qui décide de rejoindre un monastère au Tibet, et une fille qui se convertit à l’hindouisme, et une sœur qui apprend l’arabe, épouse un marchand et déménage dans son pays, cela signifie-t-il que cet homme lui-même est maintenant un arabe hindou tibétain ? Bien sûr que non ! Un autre exemple serait d’imaginer un grand philosophe d’Europe de l’Ouest qui a une sœur qui, par manque d’attention, est influencée par un petit cercle social et devient strip-teaseuse dans la banlieue française, est-ce que cela signifie aussi que le philosophe fait maintenant partie de l’industrie du sexe ? Bien sûr que non ! Pourtant, comme la société et, malheureusement, les hommes adultes en 2021 ne comprennent toujours pas la conception individuelle – ce qui vient avec le fait fondamental que chaque organisme est responsable de sa propre conception et de sa destinée et non de celle des autres – je pense que la théorie organique devrait clairement aider la société mondiale à comprendre que le choix de vie d’un organisme individuel ne relève ni de la responsabilité d’autrui, ni du fardeau d’autrui.
C’est une théorie qui apporte des preuves neuroscientifiques pour expliquer la plasticité, des arguments philosophiques pour expliquer la perception et des explications psychanalytiques pour expliquer le fonctionnement de l’esprit, ainsi que la construction et les désirs symboliques qui guident l’individu dans la réalisation de son but dans la vie. Par la suite, il souligne également que ces faits scientifiques et ces arguments philosophiques ne peuvent être ignorés ni par l’individu ni par la société en général, parce que nous sommes une nouvelle génération d’êtres humains et que nous devrions agir comme des organismes éclairés face à la découverte et non comme des êtres ataviques et rigides d’un passé lointain, car nous ne sommes pas prisonniers du passé.
La philosophie et la science font partie de la culture humaine après tout, et les progrès scientifiques et techniques suivent une évolution rapide et c’est donc fondamentale de comprendre leur impactes sur notre réalité sur terre. Comme l’a souligné un des membres de l’Académie des sciences, notamment Sanchez-Palencia, la culture est un élément fondamental de notre vie et n’est pas un luxe de riches; elle nous permet de comprendre les diverses facettes de notre environnement sur terre, nous permettant de nous y situer, de prévoir l’avenirs ou les avenirs possibles et de prendre des décisions responsables en assumant les conséquences. Certes, les connaissances scientifiques ne sont pas exactes, mais approchées. Les théories nous donne une compréhension approximative des fragments de notre réalité et la recherche contribue à l’amélioration des théories. Malgré les limites imposés par la simplicité des modèles dans la recherche scientifique pour étudier la réalité, ces modèles simples nous permettent de comprendre leurs mécanismes de transformation et d’évolution et aussi de les manipuler pour obtenir un but désiré. Il est aussi important de comprendre que les connaissances scientifiques forment un réseau compatible et cohérent qui est toujours en évolution comme notre monde sur terre, et donc, la recherche ajoute de nouvelles connaissances, et en le faisant, elle modifie et restructure les anciennes – la synthèse et l’imagination créative philosophique sont toujours présents dans la recherche de qualité. Sanchez-Palencia cita aussi Francois Jacob:
«Contrairement à ce que j’avais pu croire, la démarche scientifique ne consistait pas simplement à observer, à accumuler des données expérimentales et à en tirer une théorie. Elle commençait par l’invention d’un monde possible, ou d’un fragment de monde possible, pour la confronter, par l’expérimentation, au monde extérieur. C’était ce dialogue sans fin entre l’imagination et l’expérience qui permettait de se former une représentation toujours plus fine de ce qu’on appelle la réalité ».
Ce qu’il faut que la société comprenne, c’est que les nouvelles découvertes de la science ont aussi un impact philosophique et modifient et redéfinissent notre réalité et rend celle du passé obsolète. Donc, notre culture [notre compréhension et notre relation à notre environnement sur terre) évolue en accord avec et grâce au progrès scientifique. Un bel exemple serait le premier essai du phonographe d’Edison, comme l’a aussi souligné Sanchez-Palencia dans son essai à l’Académie des sciences française. Edison dans son essai avait chanté une courte chanson pour tester le phonographe en présence de ses collaborateurs; et le son fut enregistré et reproduit par l’appareil quelques instants après. A ce moment là, toute l’assistance fut saisie d’admiration mais aussi d’effroi, et parmi les auditeurs, certains firent même le signe de la croix; pourtant ils savaient tous qu’Edison travaillait sur l’enregistrement et la reproduction du son, mais la parole humaine semblait trop pour ces auditeurs choqués. A cette époque, reproduire la voix humaine était vu comme une transgression des limites de ce qui était permis aux mortels sur terre, et c’était dans le domaine de la transcendance. Aujourd’hui, au XXIe siècle, quelque 150 ans plus tard, tout cela a été parfaitement oublié, les jeunes d’aujourd’hui sont devenus des connaisseurs de l’informatique, des smartphones et des médias numériques, et les personnes qui publient et regardent des vidéos sur l’internet à haut débit n’ont pas l’impression d’avoir affaire au monde de la sorcellerie – c’est ainsi que la culture humaine a évolué.
Dans ce même essai de l’Académie des sciences, Sanchez-Palencia décrit un sentiment que bon nombre d’innovateurs ont subit; celui de devoir payer pour transgresser les limites de la réalité de l’humain de son époque, un sentiment qu’il pense être ancrée dans la conviction des masses, qui inventent des mythes pour se racheter de dépasser les limites supposées des divinités majoritairement païennes. Comme par exemple, pour l’invention de l’allumage du feu, qui a conduit à forger le mythe de Prométhée, censé en avoir volé le secret aux dieux et qui fut condamné à être éternellement enchaîné pour qu’un aigle vienne chaque jour lui dévorer le foie, qui serait ensuite renouvelé chaque nuit pour que la douloureuse expérience de se faire dévorer continue chaque jour avec l’animal. Une version moins sanglante de la libération de Prométhée a été imaginé par le peintre Carl Heinrich Bloch (1834 – 1890).

La Libération de Prométhée (1864) par Carl Heinrich Bloch (1834 – 1890)
Donc, ce n’est plus surprenant que comme la plupart des innovateurs intellectuels, j’ai rencontré quelques obstacles que j’ai franchis avec succès, en me basant sur des arguments scientifiques et philosophiques sains et forts [Descartes, Lacan, Voltaire, Kant, Nietzsche, Schopenhauer et Rousseau] tout en fusionnant des perspectives objectives et des observations rationnelles basées sur des théories évolutionnaires avancées par Charles Darwin et Jean-Baptiste de Lamarck. En effet, je n’ai commencé à questionner le comportement humain, le cerveau et la construction de nos réalités qu’après avoir sacrifié des années de ma vie dans la recherche et acquis les connaissances et les compétences pour le faire. Les fondements de ma théorie reposent sur des faits empiriques tirés d’un large éventail de revues scientifiques réputées, même si l’empirisme ne peut pas tout saisir précisément lorsqu’il s’agit du fonctionnement interne de l’esprit – comme la plupart des psychologues cognitivo-comportementaux le savent très bien puisqu’ils ont choisi d’entreprendre des recherches qui portent uniquement sur ce qui peut être observé et mesuré, et malheureusement pas tout sur l’esprit peut être, car nous avons trop de variables confusionnelles et de plus le domaine du psychisme est non physique.

Définition du mot “Psychisme” sur le site du Centre National de Resources Textuelles et Lexicales
La théorie organique est pour conclure, une théorie qui vise à libérer l’individu de barrières absurdes et imaginaires et à lui faire savoir qu’il n’est lié par rien ni à personne avec qui il n’a signé aucun accord à respecter. Les individus sont libres de se construire, de créer des liens sociaux autant qu’ils peuvent aussi se défaire des charges sociales et des liens avec tout organisme qui n’est en aucune façon bénéfique ou progressif pour leur développement, et cela s’étend à tout organisme extérieur qui n’est pas sous leur responsabilité ou qui ne fait pas partie de leur réalité choisie (par exemple, les petites connaissances, collègues, famille, etc).
Ce que j’insinue simplement, c’est que les organismes individuels sont maîtres de leur propre destin et que, pour réaliser leurs rêves, ils devraient être assez intelligents pour savoir quoi sacrifier, car ce n’est pas leur fardeau ou leur responsabilité et ce qu’ils doivent créer et/ou conserver. En effet, on m’a toujours dit que la mesure du succès d’une personne est la mesure de son sacrifice, et cela semble être une simple question de raisonnement. Peut-être que d’une certaine manière la “Théorie Organique” met aussi à l’épreuve la notion de “liberté” dans nos sociétés modernes. Si nous vivons vraiment dans des sociétés libres, l’individu devrait être libre dans ses choix, car la liberté elle-même implique des choix. La philosophie de la “Théorie Organique” semble aussi suggérer que dans une société éclairée, éduquée, cultivée, sophistiquée et moderne, un individu libre devrait être capable de dire ce qu’il veut, quand il veut, où il veut, comment il veut, à qui il veut, et selon ses capacités, il devrait aussi pouvoir choisir son propre chemin, identité, domaine et cercle, et lorsque ces actes ne causent la mort à personne, cela semble totalement noble et juste.

« Dans une société éclairée, éduquée, cultivée, sophistiquée et moderne, un individu libre devrait être capable de dire ce qu’il veut, quand il veut, où il veut, comment il veut, à qui il veut, et selon ses capacités, il devrait aussi pouvoir choisir son propre chemin, identité, domaine et cercle, et lorsque ces actes ne causent la mort à personne, cela semble totalement noble et juste. » -Danny d’Purb // Traduction(EN): “In an enlightened, educated, cultivated, sophisticated and modern society, a free individual should be able to say what he wants, when he wants, where he wants, how he wants, to whomever he wants, and according to his abilities, he should also be able to choose his own path, identity, domain and circle, and when these acts do not cause death to anyone, this seems totally noble and right.” -Danny D’Purb | (2019)
Le modèle de communication, aussi connu sous le nom de “langue”, est également un élément fondamental de la Théorie Organique car c’est l’une des plus grandes facettes de l’identité d’une personne. A travers la langue, un individu peut être attribué à une civilisation ou à des civilisations particulières s’il en maîtrise plus d’une, c’est ce que l’on appelle la maîtrise des schémas de communication qui est également liée aux modèles de comportement hérités d’une sphère linguistique particulière. Une discussion publiée dans l’Oxford Journal of Applied Linguistics, basée sur le domaine émergent des études bilingues des locuteurs avec l’héritage linguistique natif, a remis en question la position généralement acceptée dans les sciences linguistiques, consciente ou non, selon laquelle le monolinguisme et la nativité sont exclusivement synonymes ; Les discussions universitaires modernes ont permis de reconnaître que les personnes bilingues et multilingues qui sont des locuteurs avec l’héritage linguistique natif et exposées à une langue dans la petite enfance sont également natives ; elles ont plusieurs langues maternelles et la nativité peut s’appliquer à un état de connaissance linguistique qui se caractérise par des différences significatives par rapport à la base monolingue (Rothman et Treffers-Daller, 2014).
En conclusion, la Théorie Organique est une théorie de la conception et de l’évolution individuelle. En 2021, en ce qui concerne “La théorie organique”[qui se concentre sur la singularité de l’organisme individuel], il n’y a pas de débat entre intellectuels en psychologie, mais simplement la découverte des nouvelles perspectives mécaniques / scientifiques qu’elle introduit pour expliquer la conception psychologique et philosophique de l’individu – comme le disait Carl Sagan, « La science est une manière de penser bien plus qu’un corps de savoir ». J’ai sacrifié des années de ma vie à étudier le cerveau, le développement, la psychologie, l’art, la littérature, le langage, la conception et la singularité, et … et vous, vous croyez en quoi?
Monique de Kermadec : L’adulte surdoué : bien vivre sa douance (2012)
Je crois fermement que nous, intellectuels de la psychologie et de la philosophie, avons encore un travail énorme à faire en ce qui concerne l’éducation des masses à la construction de leur propre monde intérieur qui structure la vie mentale afin d’adapter la société à une réalité moderne et éclairée : un esprit positif aide chacun. Cette procédure aidera aussi à la sophistication de l’esprit des masses en développant un sens fondamental de compréhension scientifique et philosophique, et en saisissant le concept de l’organisme libre sur terre avec plus de similitudes que de différences [Organismes différents dans leurs modèles de communication et leur QI, mais en répétant quotidiennement les mêmes modèles vitaux avec de légères variations géographiques]. Par conséquent, la localisation géographique de la fécondation d’un embryon ne peut sceller son destin si les bons choix sont faits et si les ressources appropriées pour son développement sont fournies. Un organisme biologique a un nombre presque illimité de façons de se reconstruire, de se modifier et de se redéfinir [reprogrammer] en fonction des capacités de l’individu et cela conduit à un produit scientifiquement et psychologiquement valable – les gens ordinaires doivent encore intégrer et partager ce principe pour ouvrir de nouvelles perspectives à leur propre vie et, le faisant, se permettre de se développer psychologiquement et culturellement. Après avoir étudié l’humilité intellectuelle, les psychologues ont constaté que les individus possédant ce trait de personnalité ont des connaissances générales supérieures (Krumrei-Mancuso, Haggard, LaBouff et Rowatt, 2019). L’humilité intellectuelle a des conséquences sur l’apprentissage et les styles de pensée ; le processus d’apprentissage lui-même requiert de l’humilité intellectuelle pour reconnaître que l’on manque d’une connaissance particulière et que l’on a donc quelque chose à apprendre pour continuer à évoluer. Dans la même étude publiée dans le Journal of Positive Psychology, Krumrei-Mancuso et ses collègues ont constaté que l’humilité intellectuelle était associée à une moindre revendication des connaissances que l’on n’a pas, ce qui indique une évaluation plus précise de ses propres connaissances. Dans l’étude, l’humilité intellectuelle était également corrélée à une plus grande inclination à la réflexion, à un plus grand “besoin de connaissance” (c’est-à-dire le plaisir de réfléchir et de résoudre des problèmes), à une plus grande curiosité et à une ouverture d’esprit. Dans la revue Self and Identity, les résultats d’une étude réalisée par Porter et Schumann (2017) suggèrent que l’humilité intellectuelle peut être accrue chez les individus grâce à une croissance de l’intelligence ; nous pourrions donc tous bénéficier de l’humilité intellectuelle dans le développement de notre vie. Les auteurs ont conclu qu’ « enseigner aux gens une vision malléable de l’intelligence peut être un moyen prometteur de favoriser l’humilité intellectuelle et ses avantages associés ».
Si vous voulez en savoir plus sur la théorie organique qui est un projet en cours, faites une recherche sur mon nom “dpurb” ou “danny dpurb” et vous tomberez sur mon site où vous trouverez plus d’informations sur le sujet. Les bases de la théorie organique ont déjà été jetées, mais il s’agit d’un projet de toute une vie qui sera affiné et mis à jour dans une série de livres au cours des prochaines décennies avec d’autres travaux que j’ai l’intention de présenter au grand public du monde entier.
En attendant, je vous recommande de lire les essais académiques:
(ii) Explications psychologiques des préjugés et discrimination ;
(iii) Relativisme moral : N’avons-nous pas tous droit à une opinion laide ? ;
(iv) Conception, sélection et stress en psychologie du travail et de l’organisation ;
(v) Les causes du comportement agressif chez les primates humains ;
(vii) Le monde comme volonté et représentation ;
(ix) Les controverses qui entourent la pratique moderne de la santé mentale ;
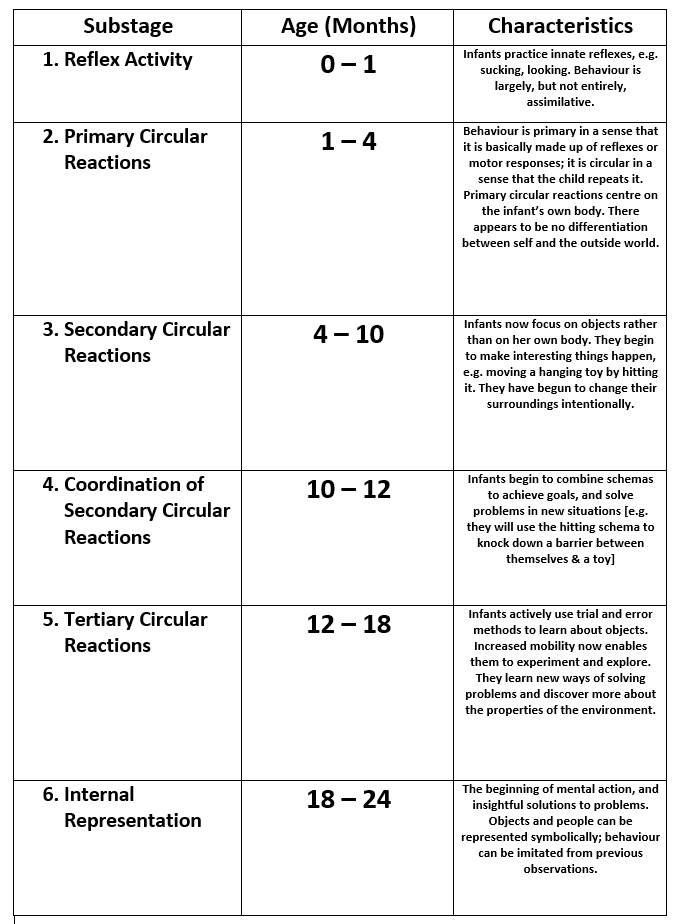
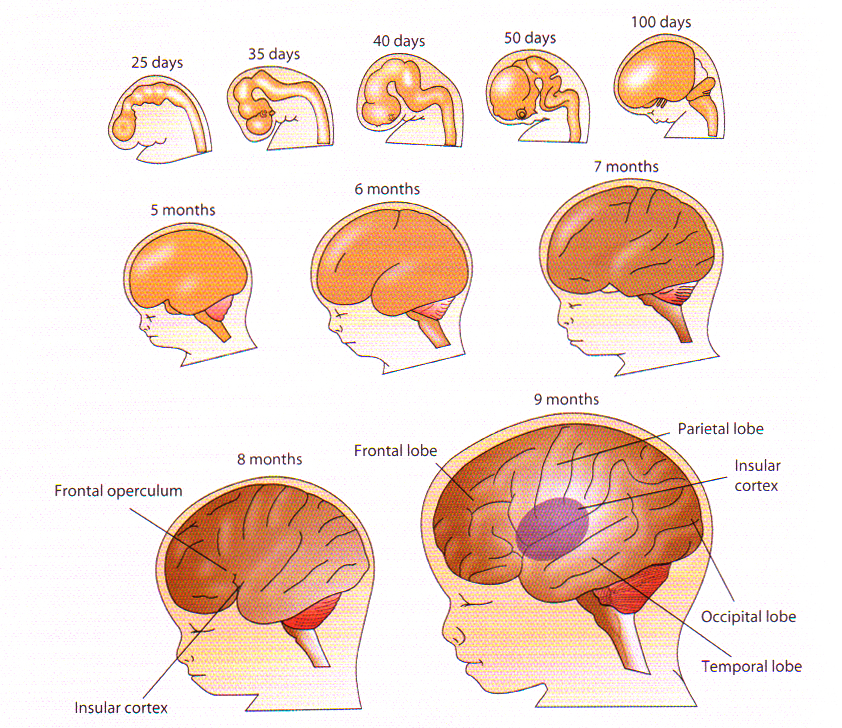
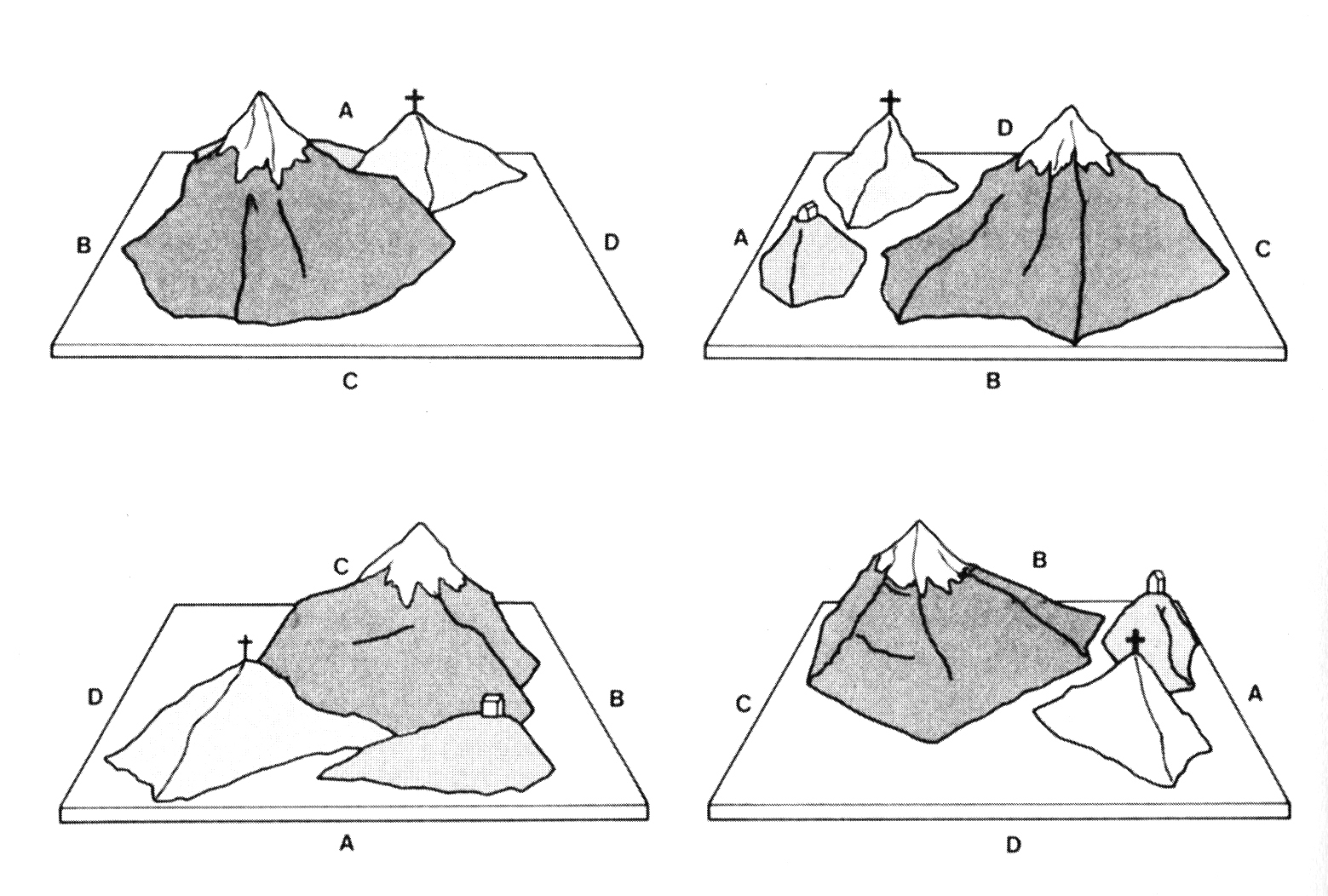
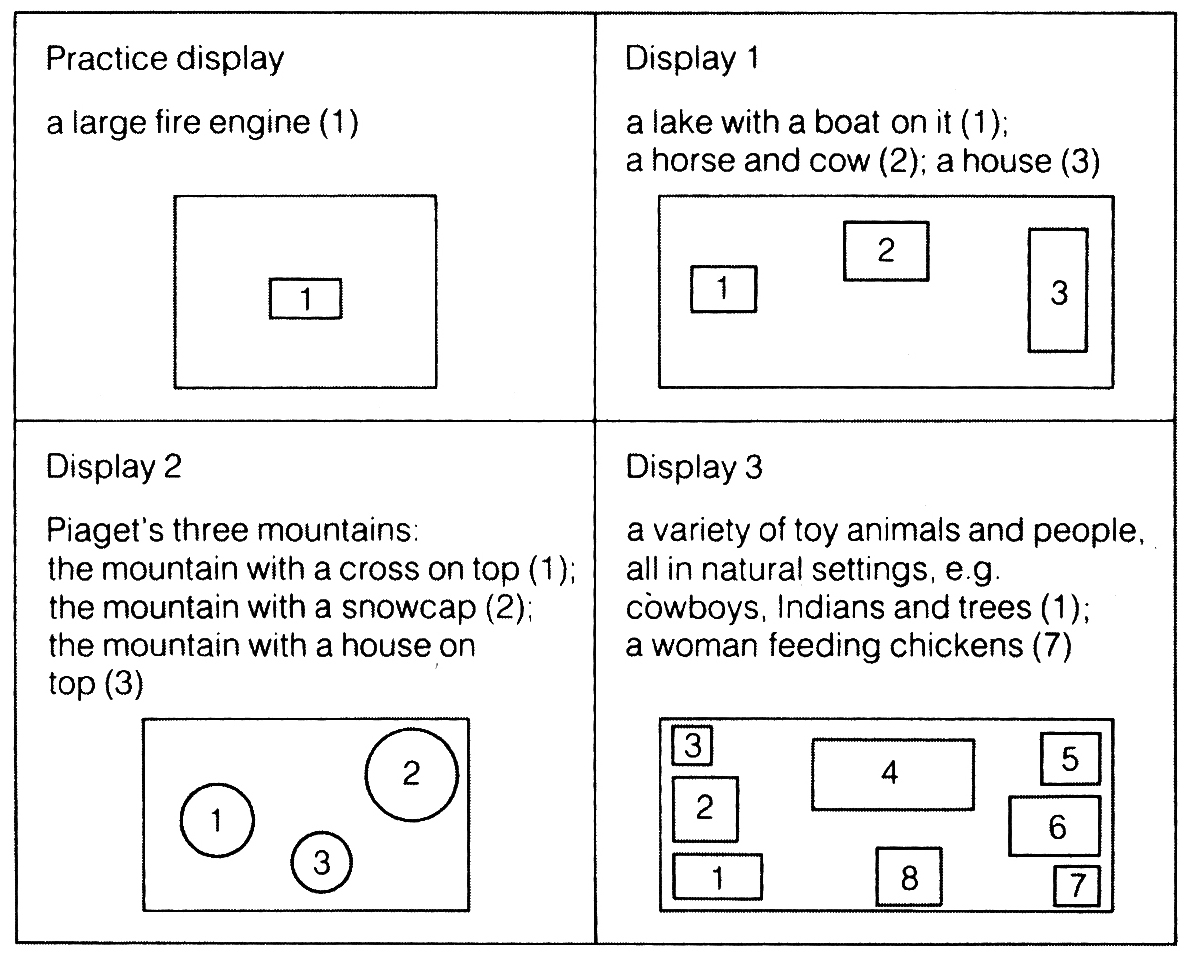
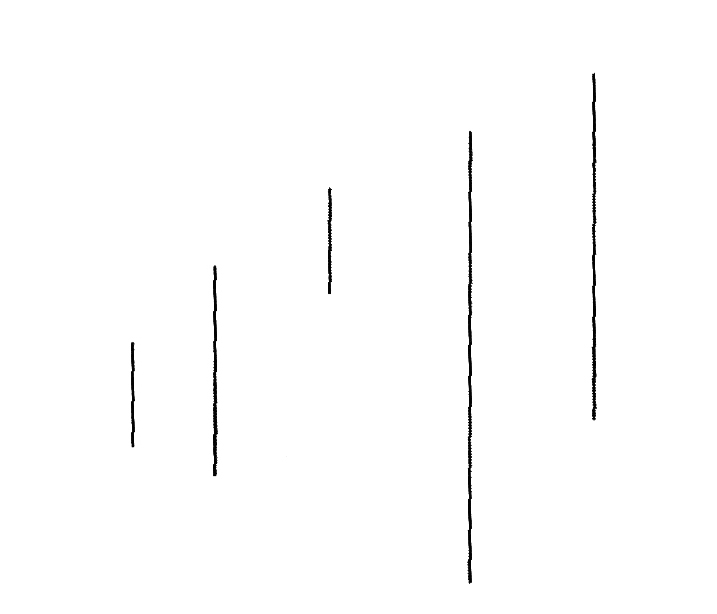
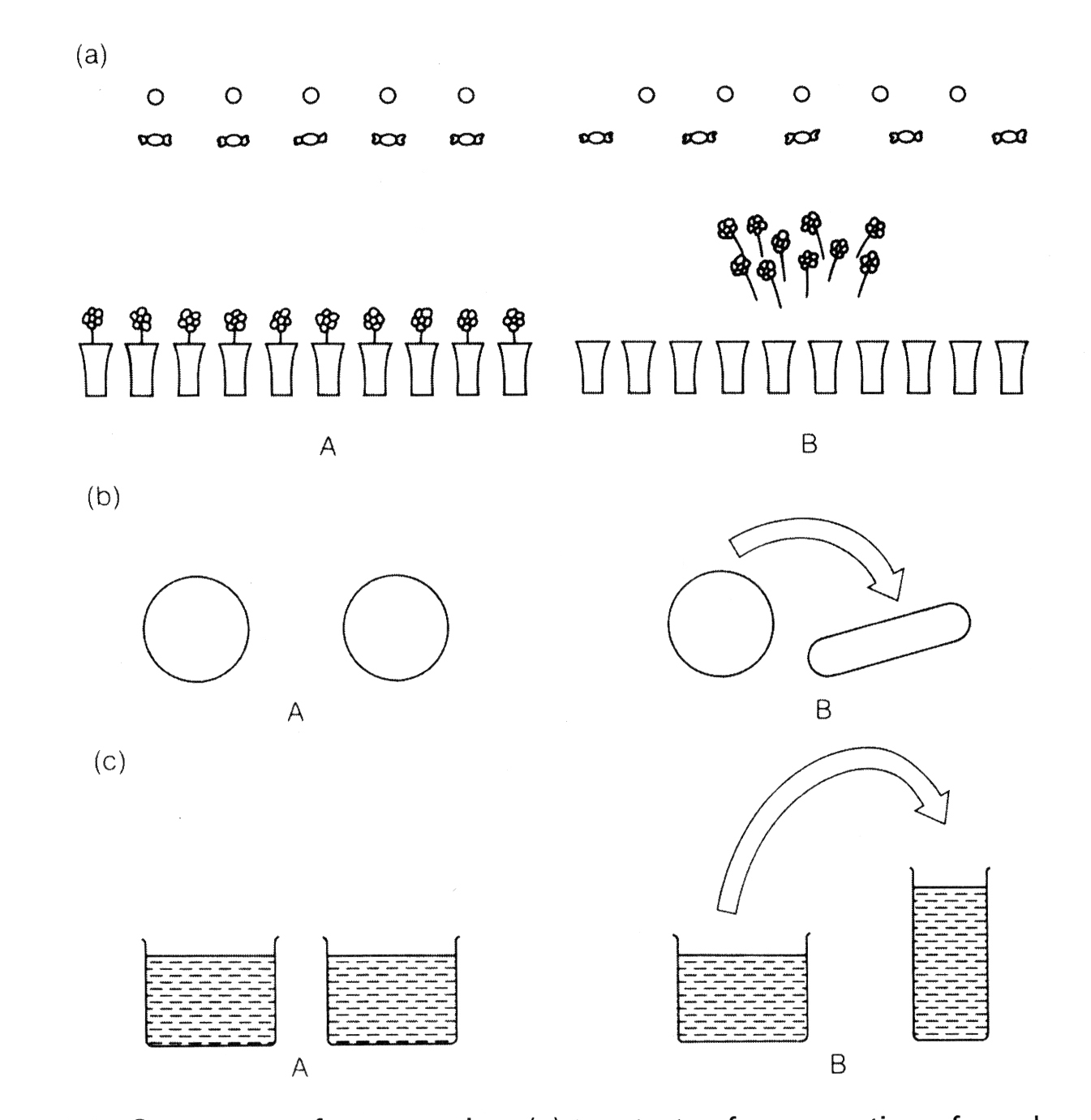
(x) Les trois principales théories du développement de l’enfant ;
(xi) Lobes frontaux, Impulsivité chez l’enfant & La Théorie de Jean Piaget ;
(xii) Comment fonctionnent nos neurones ;
(xiii) Vision, son et conscience ;
(xiv) Le concept de soi et
(xv) Psychanalyse ; Histoire, fondations, héritage, impact et évolution.
Ces essais sont le fruit d’environ 16 ans de recherche indépendante, sont référencés, révisés et mis à jour en permanence; ceux qui ont choisi de travailler pour et sont employés par des entreprises éducatives telles que les universités devraient se sentir libres d’évaluer le nombre de thèses de doctorat que constitue l’ensemble du site dpurb.com, mon opinion modeste semble indiquer environ une demi-douzaine ou plus peut-être ?
L’un des principaux objectifs de la théorie organique est de souligner toutes les choses que nous faisons mal depuis le début des temps; comment le manque de développement philosophique et de gestion de l’ego mènera à la fin de l’humanité: une espèce qui ne peut pas encore gérer sa propre existence, n’ayant toujours pas compris les lois fondamentales de l’évolution environnementale.

vers de meilleures choses / towards better things
—-|—-
[EN] Answer to Question I. “What is the Organic Theory About?”
The organic theory is a theory of the 21st century mainly focussed on the conception of the individual. It is based on the French school of thought after the revolution where the individual embraces his own choices and defines himself through his abilities, desires and achievements. It is also founded on the theory of evolution, because it sees the individual as an organism that is shaped by its environment with the ability to adapt, evolve and change depending on the psychological, social and cultural environments it wants to be a part of. However, what is unique the Organic Theory, is that it is the first theory that takes the unique conception of the individual organism to another level, because it remains focussed on the structure of thoughts and the interpretation of the world by considering what matters to the individual and is not founded on generalisations of assumption like most ancient theories do, hence this discards a lot of confusion because it shifts the focus on what matters to the unique individual organism.
Another important aspect of the “Organic Theory” as a scientific theory that I would like to make clear in the mind of the masses is that a scientific theory is nothing like what most people tend to refer as “general theories”. A general theory is a common theory that generally used to explain every day matters of sometimes questionable importance related to social matters; this usage of the term “theory” generally encompasses subjective beliefs and insights about matters not related to the universality of human life or psychology, but instead tend to occupy social conversations that most people have in places such as coffee shops to discuss and provide explanations about possible reasons or causes on common matters such as “Why did World War II really happen?”, “Why did John quit his job?” or “Why did Jane marry John?”. Explanations to these questions tend to be referred by the common crowd as some “theory”, and this kind of theory has absolutely nothing to do with a “scientific theory” such as the Organic Theory.
A scientific theory is based on a combination of two ancient methods: rationalism and empiricism. These two methods are what make science a powerful tool. The rationalist school of thought go by the belief that mental operations or principles must be employed before knowledge can be attained, for example, rationalists state that the validity or invalidity of a certain proposition can be determined by carefully applying the rules of logic. The empiricist school of thought maintains on the other hand that the source of all knowledge is sensory observation, so for rigid empiricists true knowledge can be derived from or validated only by sensory experience. After centuries of inquiry, we found that by themselves, rationalism and empiricism both had limited usefulness, so modern science combined the two schools of thought, and since then, knowledge has been accumulating at an exponential rate.
Hence, the rationalist movement added its aspect to science and prevented it from simply collecting an endless array of disconnected empirical facts, because we intellectuals must somehow make sense out of what we observe, hence, we formulate scientific theories. A scientific theory has two main functions: (1) it organises empirical observations, and (2) it acts as a guide for future observations and generates confirmable propositions. In other words, a scientific theory suggests propositions that may be tested experimentally to a certain extent with some reductionist statistical methods. If the propositions generated by a theory are confirmed reasonably through experimentation, the theory gains strength; if the propositions are not confirmed, the theory loses strength. In science observation is often guided by theory.
The Organic Theory is a theory that I brought forward to the intellectual table but its foundations were lying dormant in the psychology and scientific literature for decades. It seems that I only had to piece together these objective observations and methodically arrange them to come to the deduction along with the reality it revealed. We are not complete masters of our life, but we do have a great amount of control of our own individual conception based on our desires, education, direction, capabilities and choices in life.
The organic theory follows the organismic worldview that already existed in the great psychological debates of the century and I have built upon this perspective, refined and extended it with modern day empirical and philosophical literature to give the individual more power of self-definition in our modern and sometimes confused society. In fact, I also took some concepts from Jacques Lacan to give the individual the power and the ability to achieve their dreams and also to open the minds of the surrounding crowd to let society know and understand that people are not static objects, but have the ability to create and recreate themselves.

The one fundamental message the Organic Theory brings are that we are not defined simply by where we are born or the people connected to us that we did not choose, or by bloodlines, but rather by our own choices, efforts, abilities, achievements and directions, and also the fact that any organism can be conditioned to become part of the environment of any other organism through the never ending process of learning and adaptation, as we can see from the examples of Adolf Hitler or Napoléon Bonaparte, to name two famous cases of great leaders who came from modest foreign origins and who raised to the highest level in countries where they were not born, but recreated themselves to become the heart of these nations at a given point in time.
The Organic Theory shows that individual construction [training], which ‘can be’ mechanical and structured in its application [e.g. distance learning by text / video / audio], develops indirectly to create and give a socio-cultural dimension to the individual once the desired skills [communicative and behavioural patterns]have been fully adopted, mastered, and deployed in life. The term ‘social’ is also far too vague to be important as such… the term ‘social’ can simply be defined as the interaction [of all types] between organisms. So the term ‘social’ is not really valid scientifically and it lacks precision itself since it may refer to a wide range of variables. What we are left with then is only the individual’s choices, language(s) & abilities of personal development [e.g. cultural & psycholinguistic synthesis]: the major factors in the psychological & philosophical explanation of his/her singular conception [to note that each conception is unique to the individual human organism such as his/her fingerprints, skull shape, or body structure: singularity]. Thus: training, meritocracy, order and love [simple… in theory]. Marcel Gauchet put it well by explaining that when we live in a world structured by republican meritocracy and when we are a good student, we know that there are paths to social ascension. Unfortunately and shockingly, in some prehistoric, atavistic, misinformed and barbaric societies still governed and haunted by obscure, ancient, unsophisticated and unscientific structures of the Ancient regimes of the Middle Ages, many people are still forced to wrongly believe that the individual was born to be a slave to his birth condition, to live on his knees in eternal inferiority and to be defined by the views of their masses, who are [mostly] apathetic and miserable by conditioning. So we remain focussed on our mission to change the perception of minds, as when we do change minds, we also have an impact on the mind of their children and grand-children; the impact of psychoanalysis saves generations from misery and has an eternal effect.
“Men of genius are meteors destined to burn to enlighten their century.”
-Napoleon
To understand the simple logic of individual conception of the unique organism, let us use the example of a man who is deeply embedded in French culture and is a great teacher of literature, but has a son who decides to join a monastery in Tibet, and a daughter who converts to Hinduism, and a sister who learns Arab, marries a merchant and moves to his country, does this mean that the man himself is now a Tibetan Hindu Arab? Of course not! Another example would be to imagine a great philosopher of the Western world who happens to have a sister who due to a lack of attention is influenced by a petty social circle and becomes a strip dancer in the suburbs of France, similarly does this mean that the philosopher is now part of the sex industry? Of course not! Yet since society and sadly fully grown up men in 2021 still do not understand individual conception – which comes with the fundamental fact that each organism is responsible for his/her own conception and destiny and not that of others – I feel that the organic theory should clearly help society worldwide understand that an individual organism’s choice in life is not the responsibility or the burden of another.

Human brain specimen being studied in neuroscience professor Ron Kalil’s Medical School research lab. © UW-Madison News & Public Affairs 608/262-0067 Photo by: Jeff Miller Date: 5/00 File#: color slide
It is a theory that brings neuroscientific evidence to explain plasticity, philosophical arguments to explain perception and psychoanalytic explanations to explain the proceedings of the mind, along with construction and symbolic desires that guide the individual in achieving its goal in life. Subsequently, it is also making the point that these scientific facts and philosophical arguments cannot be ignored by both the individual and societies at large, because we are a new generation of human beings, and we should be acting as enlightened organisms in the face of discovery, not atavistic and rigid beings of a long dead past, because we are not prisoners of the past.
Philosophy and science are part of human culture after all, and scientific and technical progress is evolving rapidly, so it is fundamental to understand its impact on our reality on earth. As one of the members of the Academie des Sciences in France, Sanchez-Palencia, pointed out, culture is a fundamental part of our lives and is not a luxury of the rich; it allows us to understand the various facets of our environment on earth, allowing us to situate ourselves in it, to foresee the future or possible futures and to make responsible decisions while assuming the consequences. Of course, scientific knowledge is not exact, but it is close. Theories give us an approximate understanding of the fragments of our reality, and research contributes to the improvement of theories. Despite the limitations imposed by the simplicity of models in scientific research to study reality, these simple models allow us to understand their mechanisms of transformation and evolution and also to manipulate them to achieve a desired goal. It is also important to understand that scientific knowledge forms a compatible and coherent network that is always evolving like our world on earth, and therefore research adds new knowledge, and in doing so, it modifies and restructures old knowledge – synthesis and philosophical creative imagination are always present in quality research. Sanchez-Palencia also quoted Francois Jacob:
« Contrary to what I had thought, the scientific approach was not simply a matter of observing, accumulating experimental data and deriving a theory. It began with the invention of a possible world, or a fragment of a possible world, to confront it, through experimentation, with the outside world. It was this never-ending dialogue between imagination and experience that made it possible to form an ever finer representation of what we call reality. »
What society needs to understand is that new discoveries in science also have a philosophical impact and change and redefine our reality and make the past obsolete. Thus, our culture [our understanding of and relationship to our environment on earth] evolves in accordance with and through scientific progress. A good example would be the first trial of Edison’s phonograph, as also pointed out by Sanchez-Palencia in his essay to the Académie des Sciences. Edison in his trial had sung a short song to test the phonograph in the presence of his collaborators; and the sound was recorded and reproduced by the apparatus a few moments later. At this point, the whole audience was filled with admiration but also fear, and some of the listeners even made the sign of the cross; yet they all knew that Edison was working on the recording and reproduction of sound, but the human voice seemed too much for these shocked listeners. At that time, reproducing the human voice was seen as a transgression of the limits of what was permitted to mortals on earth, and this was in the realm of transcendence. Today, in the 21st century, some 150 years later, all this has been perfectly forgotten, today’s young people have become connoisseurs of technology, smartphones and digital media, and people posting and watching videos on the high-speed internet do not feel that they are dealing with the world of witchcraft – that is how human culture has evolved.
In the same essay published by the Académie des Sciences’, Sanchez-Palencia describes a feeling that many innovators have suffered from; that of having to pay to transgress the limits of reality of the human of his time, a sentiment that he believes is rooted in the conviction of the masses, who invent myths to redeem themselves from exceeding the supposed limits of the predominantly pagan deities. For example, the invention of the ignition of fire, which led to the myth of Prometheus, who was supposed to have stolen the secret from the gods and who was condemned to be eternally chained so that an eagle would come every day to devour his liver, which would then be renewed every night so that the painful experience of being devoured would continue every day with the flesh eating animal. A less bloody version of Prometheus’ liberation was imagined by the painter Carl Heinrich Bloch (1834 – 1890) [as shown above].
Therefore, it is no longer surprising that like most intellectual innovators, I have encountered some obstacles that I have successfully overcome, basing my arguments on sound and strong scientific and philosophical arguments [Descartes, Lacan, Voltaire, Kant, Nietzsche, Schopenhauer and Rousseau] while merging objective perspectives and rational observations based on evolutionary theories put forward by Charles Darwin and Jean-Baptiste de Lamarck. Indeed, I only started questioning human behaviour, the brain and the construction of our realities after having sacrificed years of my life in research and earned the knowledge and skills to do so. The foundations of my theory are based on empirical facts gathered from a wide range of reputable scientific journals even if empiricism cannot capture everything precisely when dealing with the inner workings of the mind – as most cognitive-behavioural psychologists themselves know very well since they chose to embark in research that only deals with what is observable and measurable, and unfortunately not everything about the mind is measurable since we have too many confounding variables, and the psyche is after all a non-physical domain.
The organic theory is to conclude, a theory that is meant to free the individual from nonsensical and imaginary barriers and to let them know that they are not bound by anything or anyone with whom they did not sign any agreement to abide by. Individuals are free to build themselves, to create social connections just as much as they can also discard of social burdens and links with any organism that is not in any way beneficial or progressive to their development, and this extends to any outside organism that is not their responsibility or part of their chosen reality [e.g. petty acquaintances, colleagues, family, etc].
What I am simply implying is that individual organisms are masters of their own destiny and to be able to achieve their dreams they should be smart enough to know what to sacrifice since it is not their burden or responsibility and what to create and/or keep. Indeed, I was always told that the measure of one’s success is the measure of one’s sacrifice, and this seems to be a simple matter of reasoning. Perhaps in some way the “Organic Theory” is also putting to the test the notion of “freedom” in our modern societies.
If we really do live in free societies then the individual should be free in his or her choices, because freedom itself entails having choices. The philosophy of the “Organic Theory” also seems to be suggesting that in an enlightened, educated, cultivated, sophisticated and modern society, a free individual should be able to say what he wants, when he wants, where he wants, how he wants, to whomever he wants, and depending on his abilities, he should also be able to choose his own path, identity, domain and circle, and when such acts do not cause death to anyone, this seems totally noble and right.
Communicative pattern, also known as “language” is also a fundamental element of the Organic Theory as it is one of the biggest facets of one’s identity. Through language an individual can be allocated to a particular civilisation or civilisations if the individual masters more than one, this is known as the mastery of communicative patters that is also related to behavioural patterns that are inherited from a particular linguistic sphere. A discussion published in the Oxford Journal of Applied Linguistics based on the emerging field of heritage speaker bilingual studies challenged the generally accepted position in the linguistic sciences, conscious or not, that monolingualism and nativeness are exclusively synonymous; from modern academic discussions, it is now being acknowledged that heritage speaker bilinguals and multilinguals exposed to a language in early childhood are also natives; they have multiple native languages, and nativeness can be applicable to a state of linguistic knowledge that is characterized by significant differences to the monolingual baseline (Rothman and Treffers-Daller, 2014).
To conclude, The Organic Theory is a theory of individual conception and evolution. In the 21st century, as far as ‘The Organic Theory’ [which focuses on the singularity of the individual organism] is concerned, there is no debate between intellectuals in psychology, but simply the discovery of the new mechanical / scientific perspectives that it introduces to explain the psychological and philosophical conception of the individual – as Carl Sagan phrased it, ‘Science is a way of thinking much more than it is a body of knowledge’. I have sacrificed years of my life studying the brain, development, psychology, art, literature, language, conception and singularity, and… and you, what do you believe in?
I firmly believe that we, intellectuals of psychology and philosophy, have a tremendous work remaining to be done regarding the education of the masses about the construction of their own inner worlds that structures mental life in order to adjust society to a modern and enlightened reality: a positive mind helps everyone. This procedure will also help in the sophistication of the mind of the masses as it develops a basic sense of scientific and philsophical understanding, and grasp the concept of the free organism on earth with more similarities than differences [Organisms differing in communicative patterns and IQ, but still repeating the similar vital patterns daily with minor variations geographically]. Hence, the geographical location of an embryo’s fertilisation cannot seal its destiny if the right choices are made and the appropriate resources for development are provided. A biological organism has an almost limitless number of ways in which it can be rebuilt, modified and redefined [re-programmed] depending on the individual’s abilities and this leads to a scientifically and psychologically valid product – the mainstream people at large are still to embed and share this principle to open new perspectives to their own lives and in doing so allow themselves to grow psychologically and culturally]. After studying intellectual humility, psychologists have found that individuals with this personality trait have superior general knowledge (Krumrei-Mancuso, Haggard, LaBouff and Rowatt, 2019).

Image: British Psychological Association (BPS)
Intellectual humility has consequences for learning and styles of thinking; the process of learning itself requires intellectual humility to acknowledge that one lacks a particular knowledge and hence has something to learn in order to continue evolving. In the same study in the Journal of Positive Psychology, Krumrei-Mancuso and her colleagues found that intellectual humility was associated with less claiming of knowledge that one does not have, indicating a more accurate assessment of one’s own knowledge. In the study, intellectual humility was also correlated with being more inclined to reflective thinking, and also possessing more “need for cognition” [i.e. enjoying thinking hard and problem solving], greater curiosity, and open-minded thinking. In the journal Self and Identity, the results from a study by Porter and Schumann (2017) suggest that intellectual humility can be increased in individuals through a growth mindset of intelligence; hence we could all benefit from intellectual humility in our lifetime development. The authors concluded that “teaching people a malleable view of intelligence may be one promising way to foster intellectual humility and its associated benefits.”
If you want to know more about the organic theory which is an ongoing project, please do a search of my name “dpurb” or “danny dpurb” and you will come across my website where more information can be found on the topic. The foundations of the Organic Theory have already been laid, but it is a lifetime project that will be refined and updated in a series of books in the coming decades along with other works that I intend to bring to the mainstream audience worldwide.
In the meantime, I recommend reading the academic essays:
(i) History on Western Philosophy, Religious cultures, Science, Medicine & Secularisation;
(ii) Psychological Explanations of Prejudice & Discrimination;
(iii) Moral Relativism: Aren’t we all entitled to an ugly opinion?;
(iv) Design, Selection & Stress in Occupational & Organisational Psychology;
(v) Causes of Aggressive Behaviour in Human Primates;
(vii) The World as Will and Idea;
(viii) Learning Disabilities, Anxiety, Depression & Schizophrenia and the Effectiveness of Psychotherapy;
(ix) Controversies that surround modern day mental health practice;
(x) The 3 Major Theories of Childhood Development;
(xi) Frontal Lobes, Impulsiveness in Children & Jean Piaget’s Theory;
(xii) How our Neurons work;
(xiii) Vision, Sound & Awareness;
(xiv) The Concept of Self, and
(xv) Psychoanalysis; History, Foundations, Legacy, Impact & Evolution.
These essays are the products of about 16 years of independent research, are referenced and constantly revised and updated; those who have chosen to work for and are employed by educational businesses such as universities should feel free to evaluate the number of doctoral theses the whole dpurb.com website constitutes, my modest opinion seems to point to about half a dozen or more perhaps?
One of the main objectives of organic theory is to highlight all the things we have been doing wrong since the beginning of time; how the lack of philosophical development and ego management will lead to the end of humanity: a species that cannot yet manage its own existence, having still not understood the fundamental laws of environmental evolution.
_________________________________
QUESTION II.
[FR] – Le terme “race” que vous qualifiez de “composition organique” semble dénué de sens pour votre théorie mais comment vous classifiez-vous par rapport à la “composition organique” ?
[EN] – The term “race” which you qualify as “organic composition” seems meaningless to your theory but how do you classify yourself in regards to “organic composition”?
[FR] Réponse:
Je me classe comme un organisme avec les schémas de communication et de comportement hérités de la sphère franco-britannique.

Image: Danny D’Purb
La race scientifiquement parmi les êtres humains peut simplement être définie comme un type particulier de “composition organique”. Cela signifie que les gens de différentes parties du monde ont simplement des compositions organiques particulières qui correspondent à leur histoire évolutive. Cependant, du point de vue scientifique universel, tout organisme, quel que soit son type de composition organique, peut procréer avec un autre. Par conséquent, cette observation simple mais fondamentale suggère que si les lois de la nature qui régissent toutes les espèces vivantes sur cette planète avaient des plans différents pour les organismes présents sur cette planète, la procréation entre les membres d’une même espèce avec des compositions organiques différentes ne serait pas possible – ce qui n’est évidemment pas le cas du point de vue de l’évolution.
J’aimerais répondre à votre question sur la composition organique [ce que vous appelez la race] et ma propre classification. Il est fondamental de comprendre que je me suis assimilé à la société d’Europe occidentale qui est une société d’héritage indo-européen, les deux langues que je parle, le français et l’anglais étant également des langues indo-européennes, et parce que j’avais tous les éléments pour faire partie des sociétés française et anglaise pour être plus spécifique quand je parle de l’Europe de l’Ouest, j’ai toujours ressenti une attraction naturelle et un sentiment instinctif d’appartenance à ces sociétés avec les gens qui constituent sa majorité.
Comme c’est moi qui innove avec une théorie scientifique qui aborde la question de l’assimilation et qui a aussi commencé à ébranler les fondements de la psychologie, de la culture et de la perception, ce fut toujours une tâche immense de clarifier cette question de l’assimilation et de la composition organique, que beaucoup de sociétés ataviques appellent “race”, sans réaliser qu’aucune race sur terre n’est “pure” et que notre race humaine actuelle, les “Homo sapiens” sont le résultat de croisements et de l’évolution. J’aimerais aller droit au but pour répondre à votre question et expliquer aussi comment j’ai raisonné pour expliquer mon point sur la composition organique et ma propre classification.
Je suis une personne pleinement assimilée dans la société française et britannique. Et tout en ne cachant pas le fait que mon côté français est dominant, je ne peux pas cacher le fait que j’ai un côté britannique très fort, ayant vécu et côtoyé le peuple anglais en Angleterre pendant des années. Cependant, la France est une société plus avant-gardiste philosophiquement et a toujours permis à des individus talentueux de s’assimiler dans leur société tout au long de leur histoire (par exemple Napoléon qui était corse est devenu l’empereur du peuple français) et est aujourd’hui un pays composé d’un mélange de compositions organiques qui s’est parfaitement adapté aux Français, apportant au patrimoine génétique français leur originalité et leur gènes surdoués. En 2018, une méta-analyse d’association à l’échelle du génome chez 267, 867 individus a identifié 1,016 gènes liés à l’intelligence, qui est un trait hautement héréditaire et un déterminant majeur de la santé et du bien-être humain (Savage, Jansen, Stringer et al., 2018). Ainsi, d’après les découvertes scientifiques actuelles, il semble que la civilisation française ait toujours été en avance sur son temps et beaucoup plus sophistiquée que tout autre empire de sa ligue.

Image: Des jeunes français
Quelle que soit la composition organique ou la nuance de couleur des individus en France, il existe un fort sentiment de préoccupation nationale et d’identité française ancré dans la grande majorité des Français qui sont fiers de leur société en évolution et qui veulent valoriser la France et sont amoureux de son patrimoine et de son peuple. En France, en effet, ce qui semble le plus important, c’est votre identité culturelle et votre loyauté envers la nation et vos sentiments français, votre vision et votre sentiment de connexion et d’amour pour les français de souche, plutôt que la pâleur de votre peau.
Étant quelqu’un qui a été élevé dans la littérature française, qui a lu la bible en français étant d’une mère chrétienne, qui a étudié la littérature française sous la direction d’un tuteur privé nommé Christian Rivalland, un grand maître et une figure paternelle pour moi qui nourrissait de nombreuses élites et personnalités politiques et qui me surnommait “Le Seigneur” [à cause de mes cheveux longs et de ma chemise blanche avec un bouclier de préfet royal doré] et qui me traitait comme son propre fils et m’enseignait Molière, Maupassant, Victor Hugo, Rousseau et la Révolution française dans sa propre maison, en étudiant aussi profondément la littérature shakespearienne et victorienne, il était clair que je me sentirais et me classerais comme une personne appartenant aux sociétés d’Europe occidentale de France et d’Angleterre – on m’appelait même affectueusement “Banane” à cause du ton de ma peau mais avec ce que beaucoup décrivaient aussi comme une forme de “blancheur” à l’intérieur, bien que j’aie toujours dit aux gens qu’il n’y a pas de “blancheur” car chaque pays a sa propre langue et sa propre façon de se comporter et est pour le plus incompatible en valeurs et en philosophie, avec de nombreux pays qui semblent presque sauvagement préhistoriques par rapport à l’empire français, donc être de la même couleur ne signifie certainement pas être du même niveau ou de la même finesse psychologique ou avoir les mêmes sentiments et perspectives sur la vie. J’ai aussi figuré en tant que chanteur principal d’un groupe alternatif indépendant et « underground » (j’ai toujours mis en doute ma flexibilité à le faire quand je portais de la littérature du début du siècle avec des paroles, heureusement le film « La Reine des Damnés » est sorti et m’a fait m’a fait sourire avec le personnage Seigneur Lestat de Lioncourt, qui transcendait les siècles des châteaux et manoirs vers une scène rock contemporaine).

Image: La Reine des Damnés (2002)
L’héritage intellectuel de l’Europe de l’Ouest s’est enraciné en moi tout au long des années où j’ai vécu à Londres et étudié en tant que chercheur profondément imprégné de la psychologie et de la philosophie des grands esprits de l’Europe de l’Ouest [par exemple Darwin, Lacan, Freud, Descartes, Rousseau, Lacan, Voltaire, Nietzsche, Schopenhauer & Kant] et toutes mes interactions professionnelles avec quelques-uns des meilleurs intellectuels du continent au fil des ans, tant personnellement que dans le média moderne que constitue Internet. Le français et l’anglais sont les deux seules langues dans lesquelles je parle et pense, et elles me permettent d’exister, en effet, je rêve même en français et en anglais avec tous les personnages qui sont de ces sphères, donc, je ne pourrais absolument rien faire sans ces langues.
Maintenant, si nous devions poser la simple question de savoir si le français et l’anglais sont des langues d’origine d’Europe de l’Ouest, la réponse serait simplement “oui”. Et comme je suis fait de ces langues, cela conclut que mes propres racines culturelles et psychologiques seraient européennes occidentales. Et comme l’Europe de l’Ouest est principalement composée de personnes de composition organique qui sont communément appelées “Blanches” par la majorité non-sophistiquée scientifiquement [ce qui est faux, puisque personne au monde n’est blanc, sauf les statues, les sculptures de marbre et les clowns dans le cirque qui se maquille], je me considère comme un dérivé de la civilisation de “L’Europe de l’Ouest”, et puisque la majorité des personnes de la classe intellectuelle sont “Blanches”, je me qualifie de “Blanc [Autre]”. Oui, pas les Blancs [britanniques], ou les Blancs [français], mais les Blanc [autres] pour indiquer que je ne suis pas le “Blanc” typique, mais un Blanc qui a subi quelques modifications dans l’histoire de l’expansion et de la conquête impériale de Europe occidentale, d’où la nuance d’olive.

dans la lumière / into the light
D’ailleurs, on ne m’interroge jamais à ce sujet sauf pour remplir des formulaires dans les pays de la sphère anglo-saxonne, alors je coche la case “Blanc [Autre]”. Simplement parce qu’il résume, clarifie, donne la description de quelqu’un qui reflète la langue, la culture, les valeurs et les perspectives de la civilisation française de l’Europe de l’Ouest principalement et la majorité des gens d’une telle civilisation sont caucasiens ou au moins plus clairs dans le teint, et cela ne servirait à rien et n’aurait certainement aucun sens sauf à créer une énorme confusion de me qualifier comme Marsien, Noire, asiatique, indien, hispanique, orientale, juif ou toute autre description empirique qui n’est pas affiliée au patrimoine de l’Europe de l’Ouest et qui ne s’en rapproche en aucune façon en donnant une forme de description de ma personne, de mon identité, de mon patrimoine et de mes capacités – les choses ont changé radicalement et le monde devrait savoir et changer aussi une fois qu’ils comprennent. En effet, ce n’est pas parce que le monde de la politique est à la traîne que je devrais faire de même. La théorie de l’évolution de Darwin révèle qu’il n’y a pas d’essence éternelle et qu’il n’existe aucune idée d’une entité exceptionnellement pure qui serait au-delà de l’évolution – tout est dans un état constant de flux[donc, d’un point de vue évolutionnaire et organique, la race est une absurdité totalement archaïque puisque nous sommes tous simplement de la matière organique sur une petite planète bleue dans le vaste univers, en train d’être recyclée, recrée et transformée en un procédé continu]. La philosophe Barbara Stiegler a sagement suggéré que la tâche de créer le consentement des masses devrait être laissée entre les mains d’experts en psychologie[c’est-à-dire ceux qui comprennent la structure psychique et les philosophies de la façon dont les humains et les sociétés fonctionnent, se développent et évoluent].
On ne m’interroge jamais sur la “race” ou, comme je préfère l’appeler d’un point de vue scientifique, sur la “composition organique” parce que dès que les gens me voient et m’entendent parler, ils arrivent instantanément à la conclusion que c’est un homme qui fait partie intégrante des sociétés française et britannique, et bien qu’il ait un teint d’olive, il parle et représente l’élite des sociétés française et britannique avec son accent et son dialecte cultivé dans les deux langues, et il ne pouvait représenter ou représenter aucun autre peuple que la majorité de ces sociétés, qui s’avèrent être des personnes d’origine indo-européenne et des langues indo-européennes et sont donc ce que la plupart ont tendance à appeler “Blanc” [qui comme je l’ai dit ne sont pas blancs mais vont du rose pâle au jaune rougeâtre] ou les personnes de la “race aryen”.
C’est pourquoi, sans surprise, j’ai répondu à votre question que je me considère comme un “produit” de la civilisation caucasienne de l’Europe de l’Ouest, pour être précis, “blanc” comme on le dit communément et mesquinement [le produit de civilisations où la majorité de la foule intellectuelle est caucasienne], bien sûr j’ai une nuance de peau d’olive, provenant d’un endroit géographique où le soleil est abondant et où un mélange organique sain a eu lieu tout au long de l’histoire de l’expansion impériale et de la conquête de l’Europe occidentale, et après tout, si nous regardons la zone géographique de l’Europe occidentale, nous pouvons observer que les tons de peau varient de très pâle à des teintes olive et jaune rougeâtre. Mais j’aimerais aussi vous donner plus de détails sur la façon dont j’en suis arrivé à cette conclusion et pourquoi je ne suis pas fou après tout, mais plutôt en train de vivre la réalité des quelques élites de la classe intellectuelle de ma génération au XXIe siècle.
Au début, j’ai dû éliminer des possibilités en me posant quelques questions :
La première question est : Suis-je un nègre ? Non
En second lieu, suis-je Indien ? Non, je ne parle pas hindi et je n’ai jamais mis les pieds en Inde.
Troisième, suis-je africain ? Il est clair que non, je n’ai jamais marché en Afrique continentale ou n’ai jamais eu de caractéristiques et de traits africains.
Quatrième être, suis-je asiatique ? Clairement non aussi, parce que je n’ai jamais marché sur le continent asiatique et que je n’ai pas non plus l’air, ni le son, ni la parole d’un Asiatique.
Cinquièmement, suis-je originaire d’un pays avec un héritage d’origine européenne ? Oui, tous les livres que j’ai lus, la musique que j’ai écoutée et les langues dans lesquelles j’ai vécu sont originaire de l’Europe de l’Ouest ! En effet, tous les hommes et les femmes qui m’ont fait ressentir toutes les émotions qui complètent un homme cultivé sont d’origine européenne, principalement de France, d’Angleterre et de quelques autres pays influencés par leur patrimoine linguistique.

Image: Bibliothèque Nationale de France
Alors, comment un homme qui a été fait par l’Europe de l’Ouest et son héritage ne pourrait-il pas ressentir un fort sentiment d’identification et de loyauté envers ces gens qui l’ont fait, et sans qui il ne serait même rien aujourd’hui ? Des gens qui l’ont fait rire, pleurer et évoluer à travers leur travail artistique ? Si vous pouviez trouver un Indien, un Pakistanais, un Asiatique de l’Est, un Africain, un Caucasien[Blanc] en dehors de l’Europe de l’Ouest, un cow-boy sauvage, ou l’héritier d’un vieux clown arriéré avec un handicap linguistique déguisé en chien brun foncé aboyant dans un cirque sur une île, qui connaît tous les albums de Francis Cabrel, qui ont lu la poésie de Stéphane Mallarmé, qui a chanté dans un groupe alternatif bilingue aux influences rock et classiques, qui a étudié Shakespeare, Dickens et parle anglais avec un accent d’Oxford et français comme l’héritier d’Honoré de Balzac, alors faites-moi savoir, je serais stupéfait.

“Chaque civilisation se forge un mythe destiné à expliquer son apparition et construit sa tradition écrite autour d’un support privilégié” / Découvrez (Liens): (i) l’aventure des écritures et (ii) l’aventure du livre | Source: La Bibliothèque Nationale de France (BNF)
Il s’agit simplement de faire valoir avec fermeté l’argument simple mais fondamental que sur cette planète, les individus ne sont pas ce que la foule environnante croit qu’ils sont, mais ce qu’ils sont, deviennent ou sont devenus parce que cela résulte du chemin qu’ils ont choisi ou qui leur a été imposé, consciemment ou inconsciemment.
Je suis né dans un pays relativement petit et nouveau d’environ 1 million d’habitants, fondé par les Français et les Britanniques avant son indépendance, et après cela, il a gardé ses saveurs françaises et britanniques et je fais partie d’une nouvelle génération d’un nouveau petit pays républicain qui a dû définir sa propre identité par rapport à son héritage intellectuel. Et comme toutes les sociétés du monde, la petite île a aussi des classes différentes, des régions différentes et des gens différents avec des langues, des dialectes, des visions et des désirs différents. Ce que je veux dire, c’est que le lieu où je suis né suit aussi une structure similaire à celle de tous les pays modernes du monde, avec des paysans, des villages, des ruraux simples, des régions pauvres, des régions riches, des sauvages, des migrants, des ouvriers étrangers pour les usines[par exemple d’Afrique, du Bangladesh, de Chine, d’autres parties de l’Asie, etc], des gens laids, des gens bons, des gens mauvais, des gens beaux, des gens d’affaires, des touristes [provenant principalement des grandes économies européennes car ils en ont les moyens, qui sont constamment présents partout et qui ont toujours bénéficié d’un accueil chaleureux], des personnalités publiques, des classes dirigeantes, des classes intellectuelles, des villes et différents niveaux d’éducation que les parents peuvent offrir à leurs enfants.
J’ai eu beaucoup de chance, car grâce à mes propres efforts intellectuels, j’ai réussi à me hisser à la toute première place dans l’élite d’une minuscule minorité qui a choisi le meilleur établissement, le Collège royal de Port-Louis, qui est une école pour enfants doués et impitoyablement sélective. Et étant une minorité d’élite d’une petite population d’environ 1 million d’habitants, je suis entrée dans un segment encore plus restreint de ces élites assez courageuses qui ont osé suivre la voie littéraire comme Chateaubriand et Balzac [la majorité veut simplement être comptable, médecin, avocat, banquier, chef d’entreprise, et tous les emplois qui vous garantissent une maison avec une voiture pour impressionner la famille de votre future femme avec une route facile à un parti politique – qui est un groupe dépassé.] J’ai toujours eu des problèmes à cause de la taille de l’île et de la carrière littéraire et philosophique que j’avais envisagée en raison du nombre limité d’esprits [quelques dizaines d’individus solitaires environ] avec mes choix éducatifs et mon niveau de compétence linguistique en français et en anglais [étant une élite universitaire, cela s’étend globalement en fait], et je me suis donc installée sur le continent qui est la base de mon héritage, à savoir l’Europe de l’Ouest [France et Angleterre], avec l’intention de m’inscrire sur un terrain mieux adapté à celui que je voulais être et suis devenu ! Comme Napoléon après avoir décroché une bourse d’étude où le petit corse allait devenir plus français que les français après avoir beaucoup subi dans sa phase d’adaptation.

à la vie éternelle / to eternal life
Et étant d’origine indo-européenne, il était clair que j’avais toutes les chances de m’assimiler dans les sociétés d’Europe de l’Ouest, c’est-à-dire que la France et l’Angleterre qui sont aussi d’origine et de langues indo-européennes, même si mon nuance d’olive me donne une identité très personnelle et ajoute parfois à mon caractère unique. En tant que personne originaire d’un pays relativement petit et nouvellement créé, avec des liens culturels d’origine d’Europe occidentale, il était clair que les élites avaient besoin d’une voix intellectuelle du XXIe siècle pour dissiper toute confusion et remettre les pendules à l’heure pour guider une génération de la classe intellectuelle qui luttait parfois pour trouver un sentiment d’identité et d’appartenance. Je crois que cela dissipe beaucoup de confusion au sujet de la classification et c’était l’un de mes objectifs avec la théorie organique pour les individus perdus et doués ; après tout, beaucoup d’intellectuels avant moi ont aussi donné une voix à ceux qui se sont perdus à travers leurs arguments et découvertes incroyables tout au long de l’histoire de la civilisation, de grands hommes, des penseurs innovants tels que Charles Darwin, Jean-Baptiste de Lamarque, Sigmund Freud, Napoléon Bonaparte, Friedrich Nietzsche, Jean-Jacques Rousseau et Jacques Lacan. Je n’ai fait que marcher dans leurs pas pour poursuivre cette tradition intellectuelle et académique des penseurs d’Europe occidentale. Il est vital de comprendre que lorsque Charles Darwin a formulé sa théorie de l’évolution, il a changé la vie telle que nous la connaissions – c’est peut-être pour cela qu’il a bâti la réputation d’une rockstar de la science et de la biologie – car il a annulé cette erreur du concept stable et permanent, mais a révélé que tout continue à évoluer désormais. Par conséquent, il est d’une importance vitale et fondamentale pour tous les groupes[du monde entier] de considérer le processus continu et sans fin de l’évolution et de la sélection naturelle, un processus qui affecte tous les organismes de la planète Terre de la même manière et aussi l’évolution adaptative singulière de certains organismes supérieurs et génétiquement doués [Voir : (i) Psychologie : Le concept de soi, (ii) Comment fonctionnent nos neurones, (iii) Les lobes temporels : Vision, son et conscience, et (iv) Les trois grandes théories du développement de l’enfant].

Image: Danny D’Purb
Nous devons comprendre l’identité d’une société en termes d’authenticité linguistique, culturelle (surtout les modèles comportementaux et perceptifs) et génétique, mais aussi considérer et suivre le cours progressif de l’évolution en tant qu’êtres modernes et sophistiqués pour inclure les organismes évolués qui s’assimilent, améliorent, stabilisent et renforcent le groupe avec des gènes supérieurs ou doués qui montrent aussi de l’intérêt, un sens d’appartenance, de la fierté, de l’interaction, une certaine parole et une identification à la culture et la nation. Tous les humains sont semblables oui, mais pas égaux… semblables physiologiquement[sang, os, organes, etc] mais pas égaux en tout cas[culture, philosophie, langue(s), QI, génétique, forme physique / santé, intelligence, vocabulaire, sensibilité, compétences, etc].
Après tout, il s’agit d’une question concernant mon identité au XXIe siècle en tant qu’homme faisant partie de la nouvelle génération qui a hérité des technologies d’apprentissage accéléré et qui ne peut parler que pour lui-même et ce en quoi il croit, comment il se sent et comment il voit sa propre histoire intellectuelle que beaucoup n’ont jamais osé analyser dans une perspective systématique et complexe du XXIe siècle, l’évolution psychologique qui a lieu par transmission culturelle, le progrès individuel et l’éducation transmise, mais sont au contraire perdus et confus à leur sujet sans comprendre plus largement le monde et ses divers sphères ; sans aucune direction pour améliorer leur vie et profiter au maximum des opportunités de faire partie de quelque chose de plus grand, comme l’empire français par exemple.
—-|—-
[EN] Answer to Question II. “The term “race” which you qualify as “organic composition” seems meaningless to your theory but how do you classify yourself in regards to “organic composition”?”
I classify myself as an organism with the communicative and behavioural patterns inherited from the Franco-British sphere. Race scientifically among human beings can simply be defined as a particular type of “organic composition”. This means that people from different parts of the world simply have particular organic compositions in line with their evolutionary history. However, from the universal scientific view, any organism of whatsoever type of organic composition can procreate with another. Hence, this simple but fundamental observation suggests that if the laws of nature that govern all living species on this planet had different plans for organisms present on this planet, procreation between members of the same species with different organic compositions would not be possible – yet this is clearly not the case from an evolutionary perspective.
I would like to respond to your question about organic composition [what you call race] and my own classification. It is fundamental to understand that I assimilated into the Western European society which is a society of indo-european heritage, with both languages that I speak, i.e. French and English also being indo-european languages, and because I had all the elements to be part of the French and English societies to be more specific when talking about Western Europe, I always felt a natural attraction and an instinctive sense of belonging to these societies along with the people that constitutes its majority.
Since, I am the one to innovate with a scientific theory that would tackle the issue of assimilation and one that has also started to shake the foundations of psychology, culture and perception, it was always going to be an immense task to clarify this issue about assimilation and organic composition, what many atavistic societies call “race”, still not realising that there is no race on earth that is “pure” and that our current breed of human beings, being the “Homo-sapiens” are the result of interbreeding and evolution. I would like to get straight to the point to answer your question and also explain how I reasoned to explain my point on organic composition and my own classification.
I am a person who fully assimilated in both French and British society. And while not hiding the fact that my French side is dominant, I cannot also hide the fact that I have a very strong British side, having lived and mixed with the English people in England for years. However, French being a more avant-garde society always allowed talented individuals to assimilate in their society throughout their early history [e.g. Napoléon who was Corsican became the emperor of the French people] and is a country today composed of a blend of organic compositions who mixed and adapted perfectly with the native people of France, bringing in their individuality and gifted genes to the French gene pool. In 2018, a genome-wide association meta-analysis in 267, 867 individuals identified 1,016 genes linked to intelligence, which is a highly heritable trait and a major determinant of human health and well-being (Savage, Jansen, Stringer et al., 2018). Hence, going by today’s scientific findings, it seems that the French civilisation is one that was always ahead of its time and far more sophisticated that any other empire of its league. Whatever the organic composition or colour shade of individuals in France, there is a strong sense of national concern and French identity embedded in the vast majority of French people who are proud of their evolving society and who want to enhance France and are in love with its heritage and people. In France, indeed, what seems to matter the most is your cultural identity and your loyalty to the nation and your French sentiments, outlook and sense of connection and love for the native people, rather than the paleness of your skin.

Being someone, who was brought up on French literature, who read the bible in French being from a Christian mother, who studied French literature under a private tutor named Christian Rivalland, a great master and a father figure for me who spoon fed many elites and political figures and who also nicknamed me “Le Seigneur” [meaning The Lord – because of my long hair and white shirt with a golden Royal Prefect shield] and who treated me as his own son and taught me Molière, Maupassant, Victor Hugo, Rousseau and the French Revolution in his own home, while also studying Shakespearean and Victorian literature to its depth, it was clear that I would feel and classify myself as a person belonging to the Western European societies of France and England – I was even affectionately called “Banana” due to the tone of my skin but with the what many also described as a form of “whiteness” within, although I always told people that there is no such thing as “whiteness” as each country have their own language and ways of behaving and are for the most incompatible in values and philosophy, with many countries seeming nearly savagely prehistoric when compared with the French empire, so being of the same colour certainly does not mean being of the same league or of the same psychological finesse or with the same sentiments and outlook on life. On the side I also was performing as the lead singer of an independent and underground alternative band [I always questioned my flexibility in doing this when carrying early century literature with lyrics, luckily the movie Queen of the Damned came out and made me feel better with the character Seigneur Lestat de Lioncourt, who transcended the centuries from castles and manors to a contemporary rock stage].
The Western European intellectual heritage was further embedded in me through the years of living in London and studying as a scholar deeply drenched in the psychology and philosophy of the great minds of the Western European region [e.g. Darwin, Lacan, Freud, Descartes, Rousseau, Lacan, Voltaire, Nietzsche, Schopenhauer & Kant] with all my professional interactions being with some of the finest intellectuals of the continent over the years, both personally and through the now modern medium that is the internet. French and English are the only two languages I speak and think in, and they allow me to exist, indeed, I even dream in French and English with all the characters being from those realms, hence, I would not be able to do absolutely anything without these languages.
Now if we were to ask the simple question of whether French and English are languages of Western European roots, then they answer would simply be “yes”. And since I am made of these languages, this concludes my own cultural and psychological roots would be Western European. And since Western Europe is mostly composed of people of organic composition who are commonly referred to by the unsophisticated majority as “White” [which is untrue, since no one in the world is white, except statues, marble sculptures and clowns in the circus who wear makeup], I see myself as a derivative of the “Western European” civilisation, and since the majority of people from the intellectual classes are “Caucasian” hence I classify myself as “White [Other]”. Yes, not White British, or White French, but “White [Other]” to indicate that I am not the typical “White” but one that has had some modification through the history of Western European Imperial expansion and conquest, hence the olive tone.
Besides, I am never asked about this except when filling forms in countries of the Anglo sphere, so I tick the “White [Other]” box. Simply because it summarises, clarifies, gives the description of someone who reflects the language, culture, values and outlook of the Western European civilisation of France mainly and the majority of people from such a civilisation are Caucasian or at least lighter in complexion, and it would not serve any purpose and certainly would not make any sense except create tremendous confusion to classify myself as Marsian, Black, Asian, Indian, Hispanic, Oriental, Jewish or any other empirical description that is not affiliated with the Western European heritage and does not in any way come even close giving a form of description of my person, identity, heritage and abilities – things have changed drastically and the world should know and change too once they do. Indeed, it is not because the world of policy is lagging behind that I should too. Darwin’s theory of evolution revealed, there is no eternal essence, and any idea of an exceptionally pure entity that would be beyond evolution does not exist – everything is in a constant state of flux [so from an evolutionary and organic standpoint, race is a totally archaic absurdity since we are all simply organic matter on a small blue planet in the vast universe being recycled, recreated and reshaped in a continuous process]. The philosopher Barbara Stiegler wisely suggested that the task of creating the consent of the masses should be left in the hands of experts in psychology [i.e. those who understand the psychic structure and philosophies of how humans and societies operate, develop and evolve].
I never get asked about “race” or as I prefer to call it from a scientific perspective, “Organic Composition” because the moment people see and hear me speak they instantly come to the conclusion that this is a man who is fully part of French and British societies, and while he may have a slight olive tone, he speaks for and represents the elite of both French and British society with his cultivated dialect and accent in both languages, and he could not possibly stand for or represent any other people but the majority of those societies, which turn out to be people of Indo-European heritage and Indo-European languages and hence are what most tend to call “White” [that as I said are not white but range from shades of pale pink to reddish-yellow] or the people of the “Aryan Race”.
Hence, your question answered, unsurprisingly, I see myself as a “product” of the Caucasian Western European civilisation to be precise, “White” as it is commonly and pettily said [the product of civilisations where the majority of the intellectual crowd are Caucasian], of course I have an olive tone, being from a geographical location where the sun is abundant and where some healthy organic blending has taken place through the history of Western European imperial expansion and conquest, and after all, if we look at the Western European geographic area we may observe that skin tones vary from very pale to hues of olive and reddish-yellow. But I would also like to give you some more details of how I also proceeded to come to this conclusion and why I am not insane after all, but rather living the reality of the few elites of the intellectual class of my generation in the 21st century.
At first I had to eliminate possibilities by asking myself a couple of questions:
First question being, am I a negro? No
Second being, am I Indian? No, I do not speak hindi or have ever stepped foot in India.
Third being, am I African? Clearly No, I have never stepped in mainland Africa or have any African features and traits.
Fourth being, am I Asian? Clearly no also, because I have never stepped in the Asian continent and also do not also look, sound or speak like an Asian either.
Fifth being, am I from a country with European intellectual heritage? Yes, all the books I read, music I listened to and languages I lived in are of Western European heritage! Indeed, all the men and women who made me feel all the emotions, that complete a cultured man are of European heritage, mostly from France, England and a few other countries influenced by their linguistic heritage.
So how could a man who was made by Western Europe and its heritage, not feel a strong sense of identification and loyalty to these people who made him, and without whom he would not even be anything today? People who made him laugh, cry and evolve through their art work? If you could find an Indian, a Pakistani, an Eastern Asian, an African, a Caucasian [White] outside of Western Europe, a savage cowboy, or the heir to an old backward clown with a linguistic disability disguised as a dark brown dog barking in a circus on an island, who knows all the albums of Francis Cabrel, who read the poetry of Stéphane Mallarmé, who sang in a bilingual alternative band with rock and classical influences, who studied Shakespeare, Dickens and speaks English with an accent from Oxford and French like the heir of Honoré de Balzac, then please let me know, I would be amazed. This is simply to adamantly make the simple but fundamental argument that on this planet, individuals are not what the surrounding crowd believes them to be, but are what they are, are becoming or have become because it results from the path they chose or that was imposed on them – consciously or unconsciously.
I was born in a relatively tiny and new country of about 1 million in population founded by the French and the British before its independence, and after that it still kept its French and British flavours and I am part of a new generation of a tiny new republican country who had to define his own identity in relation to his intellectual inheritance. And as all societies in the world, the small island too has different classes, different regions and different people with different languages, dialects, visions and desires. What I mean is that the location where I was born also follows a similar structure to all modern countries in the world, with peasants, villages, simple rural people, poor regions, rich regions, savages, migrants, foreign labour for factories [e.g. from Africa, Bangladesh, China, other parts of Asia, etc], ugly people, good people, bad people, beautiful people, business people, tourists [mainly from the major economies of Europe since they can afford to, who are constantly present everywhere and have always enjoyed a warm welcome], public figures, leading classes, intellectual classes, cities and different levels of education that parents are able to afford for their children.
I turned out to be quite lucky, because through my own intellectual efforts, I managed to rise to the very cream of the crop into the elite segment of a tiny minority who took the route of literary studies at the best institution, the Royal College of Port-Louis which is an unforgiving and highly selective elite oriented school for gifted children. And being an elite minority of a small population of about 1 million, I went into an even tinier segment of those elites courageous enough who dared to follow the literary road like Chateaubriand and Balzac [the majority just want to be accountants, doctors, lawyers, bankers, business owners, and all the jobs that land you in a house with a car safely to impress your future in laws with an easy route to joining the obsolete group that is a political party]. I always had problems existing because of the size of the island along with the literary and philosophical career I had envisioned due to the limited amount of minds [about a few dozens of solitary individuals] with my educational choices and level of linguistic proficiency in French and English [being an academic elite, this extends globally in fact], and hence moved to the continent that is the root of the inheritance I am made of, which is Western Europe [France and England], with the intention of being part of a terrain more suited to the person that I wanted to be and today, have become! Quite similar to Napoleon who after having obtained a scholarship to an elite academy in France, the little Corsican would later grown to become more French than the French themselves after having suffered a lot in his early adaptation phase to the culture and people.
And being of Indo-European heritage it was clear that I had all the chances of assimilating in the societies of Western Europe, i.e. France and England being also of Indo-European heritage and languages, although my olive tone does give me a very individual identity and sometimes adds to my unique character. As a person from a relatively tiny and newly created country that is of Western European heritage, it was clear that the elites needed an intellectual voice of the 21st century to clear out all the confusion and set the record straight to guide a generation of the intellectual class sometimes struggling to find a sense of identity and belonging. I believe this clears out a lot of confusion about classification and this was one of my purposes with the organic theory for lost and gifted individuals; after all many intellectuals before me also gave a voice to those who were lost through their amazing arguments and discoveries throughout the history of civilisation, great men, innovating thinkers such as Charles Darwin, Jean-Baptiste de Lamarque, Sigmund Freud, Napoléon Bonaparte, Friedrich Nietzsche, Jean-Jacques Rousseau and Jacques Lacan. I only walked in their steps to pursue this intellectual and academic tradition of Western European thinkers. It is vital to understand that when Charles Darwin formulated his theory of evolution he changed life forever as we knew it – perhaps this is why he built the reputation of a rockstar of science and biology – because he cancelled this once believed fallacy of the stable and permanent concept, but revealed that everything continues to evolve from here on. Hence, it is of vital and fundamental importance for all groups [around the world] to consider the never-ending and ongoing process of evolution and natural selection, a process that affects all organisms on planet Earth similarly and also the singular adaptive evolution of some superior and genetically gifted organisms [See: (i) Psychology: The Concept of Self, (ii) How our Neurons work, (iii) The Temporal Lobes: Vision, Sound & Awareness and (iv) The 3 Major Theories of Childhood Development]
We need to understand the identity of a society in terms of linguistic, cultural [mostly behavioural and perceptive patterns], and genetic authenticity but also consider and follow the progressive course of evolution as modern and sophisticated beings to include evolved organisms that assimilate, enhance, stabilise, and strengthen the group with superior or gifted genes that also care about, have a sense of belonging, take pride, interact, speak for and identify with the culture and nation. All humans are similar yes, but not equal … similar physiologically [blood, bone, organs, etc] but not equal in any case [culture, philosophy, language(s), IQ, genetics, fitness/health, intelligence, vocabulary, sensibility, skills, etc].
After all this is a question about my identity in the 21st century as a man who is part of the new generation who inherited accelerated learning technologies and who can only speak for himself and what he believes in, how he feels and how he sees in regards to his own intellectual history that many have never dared to analyse from a systematic and sophisticated perspective by embracing the 21st century and the psychological evolution that took place through cultural transmission, individual progress and education, but are instead lost and confused about themselves without a wider understanding of the world and its different realms; without any direction to make their lives better and make the most of the opportunities to become part of something bigger, such as the French empire for example.
_________________________________
QUESTION III.
[FR] – Qu’est-ce que cela signifie pour vous d’être franco-britannique ?
[EN] – What does it mean to you to be Franco-British?
[FR] Réponse:
Eh bien, cela signifie être français dans la pensée, les sentiments, la philosophie, les valeurs, l’art et la vision, mais aussi avec un côté britannique fort qui se reflète dans l’anglais parlé et écrit. Être franco-britannique pour moi, c’est pouvoir naviguer dans les deux environnements avec la facilité d’un natif au niveau d’une élite et se sentir à l’aise dans les deux sphères tout en étant capable de voir le monde du point de vue des deux peuples et de parler pour les deux peuples dans les questions liées à la gestion de la société.
La philosophie française enseigne à l’individu à repousser ses limites, tandis que la sphère anglaise semble inculquer la notion de connaître ses propres limites, évidemment le royaume anglais est moins progressiste et décourage l’individu dans des efforts créatifs et favorise plutôt une vie mondaine et captive sans aucune faim pour le type d’innovation qui englobe la grandeur du cerveau humain.
Franco étant devant les Britanniques signifie que le Français est l’identité dominante, et sans manquer de respect au sphère anglaise, il serait impossible pour n’importe quel individu avec mes capacités intellectuelles de prendre la décision de renoncer complètement à leur côté français pour être entièrement anglais, car cela signifierait simplement gâcher la chance de faire partie de la civilisation la plus sophistiquée sur terre avec un amour absolu et un respect admirable des droits des individus dans la société.

Traduction(EN): « A great aggregation of men sane in mind & warm in the heart, creates a moral conscience that is known as a nation » – Ernest Renan / Source: Université Paris 1 Panthéon-Sorbonne
Enfin, être franco-britannique signifie pour moi diffuser progressivement les valeurs françaises et la “joie de vivre” à la société britannique et à la sphère anglo-saxonne afin de changer cette réputation stéréotypée de “rocher froid irréceptif et irréactif” et motiver les gens de tous horizons à croire aux philosophies de l’épanouissement personnel et de l’évolution individuelle, ainsi qu’à une bonne conscience héroïque axée sur la morale, la dignité, le sens des responsabilités, la solidarité civique, la fraternité et la loyauté où les individus se poussent et se motivent mutuellement pour avancer, en considérant le succès comme un bien commun, dans le grand sens d’une société harmonieuse et en phase avec la grandeur de l’être, en harmonie, qui est mieux en accord avec les principes et perspectives françaises. Ce qui est surprenant et malheureux, c’est que cette réputation stéréotypée typique de « l’Anglais misérable, négatif, déprimant et ennuyeux » semble être justifiée par les récents rapports de l’OCDE qui ont placé la Grande-Bretagne parmi les pays les plus déprimés d’Europe occidentale, avec les problèmes de santé mentale coûtant environ 94 milliards de livres par an. Quant à l’autre grand continent de l’anglosphère, les États-Unis, ils sont en tête de liste pour les taux de troubles anxieux et de dépression.
Documentaire: Le Week-end de Benoit Chaumont chez les accros du jeu au Royaume-Uni
Ainsi, en tant qu’intellectuel plongé dans le monde de la psychologie, cette mission de changer le psychisme de l’anglosphère et du reste du monde apparaît comme un effort justifié et noble pour aider progressivement l’évolution du psychisme typique “d’artisan” vers un psychisme “artistique, dynamique, créatif et humain”. Bien sûr, c’est aussi motiver les gens de la sphère anglo-saxonne et le reste du monde à apprendre la langue française, car avec la langue vient la magie de l’âme, les sentiments, la perspective, l’art, la sophistication, la créativité et le courage inhérents au patrimoine alors qu’ils apprennent à naviguer dans le bleu profond de la sphère française en apprenant à se dépasser et à se perfectionner psychologiquement pour modifier leur perception de manière progressive tout en respectant les droits des autres à croître.

Traduction (EN): “Impossible is not French” – Napoleon
—-|—-
[EN] Answer to Question III. “What does it mean to you to be Franco-British?”
Well, it means to be French in thought, sentiments, philosophy, values, artistry and vision, but with also a strong British side that is reflected in spoken and written English. To be Franco-British to me means to be able to navigate both environments with the ease of a native at the level of an elite and to feel at home in both realms along with the ability to see the world from the perspective of both people and speak for both people in matters connected to the management of society.
The French philosophy teaches the individual to push the limits, while the English realm seems to inculcate the notion of knowing one’s own limits, to me the latter is less progressive and discourages the individual into creative endeavours and instead promotes a mundane and captive life without any hunger for the type of innovation that embraces the greatness of the human brain.
Franco being before British means that the French is the dominant identity, and without being disrespectful to the English realm, it would be impossible for any individual with my intellectual abilities to take the decision to completely give up their French side to be fully English, because it would simply mean throwing away the chance to be part of the most sophisticated civilisation on earth with an absolute love and respect for the rights of the individual in society.
French Escape Room Activity For UK Schools
Finally, for me, being Franco-British means gradually spreading French values and “joie de vivre” to British society and the Anglo-Saxon sphere in order to change this stereotyped reputation of “unreceptive and unreactive cold rock” and motivate people from all walks of life to believe in the philosophies of personal development and individual evolution, as well as in a heroic conscience based on morals, dignity, a sense of responsibility, civic solidarity, fraternity and loyalty where individuals push and motivate each other to move forward, considering success as a common good, in the great sense of a harmonious society and in phase with the greatness of humankind, in harmony, which is more in line with French principles and perspectives. What is surprising and unfortunate is that this typical stereotyped reputation of the “Miserable, negative, depressing and boring Englishman” seems to be justified with recent OECD reports that have placed Britain among the most depressed countries of Western Europe, with mental health problems costing about 94 billions pound a year. As for the other major continent of the anglosphere, the US, they are topping the charts for rates of anxiety disorders and depression.

Mental health statistics for England: prevalence, services and funding / Source: www.parliament.uk
So, as an intellectual drenched in the world of psychology, this mission of changing the psyche of the anglosphere and the rest of the world seems like a justified and noble endeavour to gradually help the evolution of the typical “artisan” psyche into an “artistic, dynamic, creative and human” one. Of course, it also means motivating people in the Anglo-sphere and the rest of the world to learn the French language, because with language comes the magic of the soul, the sentiments, the perspective, the artistry, the sophistication, the creativity and the courage inherent to the heritage as they learn to navigate in the deep blue of the French sphere by learning to surpass themselves and to perfect themselves psychologically and modify their perception in a progressive way while respecting the rights of others to grow.

Traduction(EN): “The history of France begins with the French language. Language is the principal sign of a nationality. ” – Jules Michelet
_________________________________
QUESTION IV.
[FR] – Quelle est la meilleure langue entre le français et l’anglais selon vous ?
[EN] – Which one is the best language between French and English according to you?
[FR] Réponse:
C’est une question délicate car le terme “meilleur” est ici assez vague. Ainsi, j’aurai tendance à penser qu’un langage de première classe devrait être clair, précis, pratique, agréable à l’oreille, et les yeux, bien structurés avec la prononciation reflétée dans la structure grammaticale pour empêcher les gens de mal prononcer les mots et aussi tenir une quantité de profondeur qui se reflète lors de l’expression des pensées du penseur de haut niveau, et qui a une valeur artistique qui lui permet de se sentir plein d’émotions lorsque parlé comme langue humaine à travers son timbre et son ton.
La langue anglaise, bien que pratique en raison de son usage répandu, manque de synchronisation entre sa structure grammaticale et la façon dont les mots sont prononcés, ce qui fait que même les anglophones de langue maternelle expérimentés peuvent mal prononcer de nombreux mots, ce qui, dans de rares cas, peut même conduire à considérer les gens comme dyslexiques phonologiques. Pour moi, cela rend la langue anglaise inférieure à la langue française puisque la dernière a un plus grand nombre de “signes accentués” qui indiquent précisément au lecteur comment prononcer les mots. En effet, dans la langue française, la majorité des mots se prononce exactement comme ils sont écrits une fois que l’on apprend les terminaisons des temps verbaux et quelques règles grammaticales.
L’autre facteur, lorsqu’on compare les deux langues les plus répandues dans le monde civilisé, est le fait que la langue anglaise a une variété d’accents provenant des différentes régions où elle est parlée [par exemple Scouse, Geordie, Cockney, Scottish, Irish, etc] et est souvent étouffée dans les vidéos et peut souvent conduire à des malentendus ou exiger de l’auditeur de répéter des segments pour bien comprendre, ce qui est un désavantage de la langue anglaise. Ce n’est guère le cas avec le français, car même dans les différents accents dans lesquels la langue peut être parlée, ils conduisent toujours à un son plus clair en raison de la structure grammaticale et des règles de la langue et donc une audition plus claire et donc une compréhension plus rapide en comparaison de l’anglais.
La langue anglaise a aussi une histoire fondée sur l’empirisme et semble simplement remplir la tâche de communiquer des instructions et des textes scientifiques, mais elle manque de l’émotivité des œuvres d’art [par exemple le romantisme] et des arguments philosophiques [par exemple I think, therefore I am !] par rapport à la langue française. Notez que je n’ai pas dit qu’il ne peut pas être utilisé dans les œuvres d’art, mais seulement qu’il est moins intense que la langue française. L’anglais me semble diminuer l’intensité des arguments philosophiques et des conversations humaines étant une langue assez plate dans sa forme écrite et orale. Cela peut aussi s’expliquer par le fait que l’anglosphère est issue d’une majorité de sociétés où les valeurs de l’humanité, de la fraternité et de l’individu ne sont pas au cœur de la civilisation comme en France, mais plutôt de sociétés industrialisées et mécaniques qui ne peuvent offrir la liberté que comme une forme d’individualité extrême à la limite de l’égoïsme basée sur une formule du type ” chacun pour soi ” dans un jeu sauvage de survie et de préservation à tout prix. C’est bien sûr le principal courant de pensée, parce que nous avons une minorité d’individus incroyables de la sphère anglaise qui se distinguent par leur propre investissement dans la cultivation de leurs personnalités uniques et captivantes et qui n’agissent pas et ne pensent pas comme la majorité commune et on peut le constater par leur comportement, leurs sentiments et leurs œuvres artistiques. De plus, les racines de la langue anglaise sont toujours liées au système monarchique désuet qui semble rendre la société obsédée par les histoires médiévales de capes et d’épées : un système qui semble inculquer à l’individu le sens de connaître les limites de ses droits et une obéissance incontestable ; alors que la langue française est enracinée dans les valeurs de la révolution qui inculque le sens du questionnement et aussi de repousser ses propres limites pour libérer en soi l’Empereur/le Roi/le Maître”, avec la légende de Napoléon comme preuve – la philosophie et les valeurs des deux langues semblent opposées entre elles.
Ainsi, pour moi, étant quelqu’un qui a reçu une bourse et étudié la littérature, la linguistique, la psychologie et la philosophie tout en ayant écrit pendant longtemps et qui a été plongé profondément dans le domaine culturel de l’anglais et du français, l’anglais semble être une langue de communication, alors que le français est une langue qui peut absolument tout faire comme l’anglais, mais qui permet aussi à l’individu non seulement de communiquer, mais aussi de “s’exprimer” [leur profondeur, leurs pensées, leurs émotions] d’une manière que la langue anglaise ne parvient pas à saisir à une telle intensité en raison de son histoire et de sa structure fondatrices qui ne sont pas aussi axées sur le timbre, la philosophie, les arts et l’expression des sentiments que l’est la langue française.
Ainsi, puisque la langue française peut faire tout ce que l’anglais peut faire dans le monde formel, comme les instructions, les écrits scientifiques et la simple communication, mais qu’elle peut aussi aller plus loin pour toucher plus profondément l’être « humain » par sa subtilité dans le timbre et le son qui s’inscrivent dans une histoire de grands poètes, philosophes et penseurs qui se sont imposés dans la pierre, je dois dire que le français est meilleur que l’anglais. Bien qu’il soit important de noter que ces deux langues sont très proches l’une de l’autre dans leur structure puisque beaucoup de mots sont épelés de façon similaire dans les deux langues avec des changements mineurs d’une langue à l’autre [par exemple Psychologie/Littérature est français pour psychology/literature (anglais)]. Comme les deux langues sont d’origine indo-européenne, il est plus facile pour les anglophones d’évoluer et de passer au français que la plupart des autres langues – du moins sous forme écrite puisque le français oral exige de la pratique et du dévouement à la maîtrise ; tandis qu’une “âme” est une autre histoire impliquant une vision métaphorique, des capacités de synthèse, des valeurs, une vision et une profondeur de pensée… et bien sûr la personnalité, les émotions et la sensibilité.
Les personnes qui entendent partager leur sagesse et contribuer au développement du monde auraient un avantage d’adopter et de maîtriser un mode de communication (c’est-à-dire une langue) jugé supérieur par le fait qu’il est accompagné de valeurs humaines modernes et qu’il est tissé dans le tissu d’un patrimoine intellectuel, psychosocial, philosophique et artistique plus raffiné et sophistiqué [par exemple le français, qui est la deuxième langue la plus désirée et la plus parlée au Royaume-Uni et en Allemagne] puisqu’il serait compris par un public plus large du monde civilisé, où se produit la principale évolution/révolution intellectuelle et culturelle.
Je voudrais également faire remarquer à la majorité des anglophones et des compatriotes anglais qui connaissent à peine leur propre évolution culturelle qu’il y a du français sur l’emblème de la monarchie britannique.
Les mots “Dieu et mon droit” sont la devise depuis l’époque d’Henri V (1413 – 1422), et depuis cette époque, le vieil anglais n’est plus la langue de l’élite anglaise, ce qui a entraîné l’utilisation de mots et d’expressions d’origine française et normande qui sont maintenant largement utilisés dans la langue anglaise.
Le français a également été identifié comme une langue importante pour l’avenir du Royaume-Uni. Dans un article publié par le British Council en 2014, le professeur Michael Kelly, qui dirige le département des langues modernes à l’université de Southampton, a décrit le “je ne sais quoi” dans l’apprentissage de la langue française ; les Britanniques considèrent le français comme la langue de l’amour, comme il l’a souligné, et la langue française a une romance à l’oreille de l’anglophone. C’est la culture française qui a suscité l’enthousiasme de Kelly, qui a avoué avoir été “renversé par la profondeur des sentiments” et avoir encore des frissons en découvrant les œuvres de Charles Baudelaire. “L’invitation au voyage” l’a fait voyager dans un pays où “tout n’est qu’ordre et beauté, luxe, calme et volupté” [cité du poème de Baudelaire]. Le professeur Kelly a fait valoir que, pour lui, cela résume la France sous son meilleur jour. Il écrit que lorsque les mots sont dits en français, ils évoquent un monde au-delà de leurs équivalents anglais ordinaires ; ce qui caractérise le français comme une langue romantique pour les Britanniques, c’est qu’elle peut être presque mais pas complètement comprise. Puisqu’elle n’est pas utilisée tout le temps, les Anglais n’ont pas la surcharge de significations quotidiennes qui peuvent faire disparaître la magie pour certains francophones natifs, et selon Kelly, c’est peut-être la raison pour laquelle les Britanniques considèrent le français comme la “langue de l’amour”.
Le français a laissé une impression durable sur la langue anglaise et, comme la plupart des autres pays, les Français parlent, écrivent et chantent sur l’amour. Cependant, les Britanniques, souligne Kelly, soupçonnent les Français de mieux s’exprimer sur l’amour, contrairement aux Anglais plus “coincés”, qui pataugent comme Hugh Grant dans “Quatre mariages et un enterrement”. La différence, fait remarquer M. Kelly, tient à la culture, et pas seulement à la langue. La culture est un facteur essentiel, et une partie du romantisme de la langue française pour les Britanniques est liée au fait qu’elle était la langue de l’aristocratie anglaise au Moyen Âge : les Normands et les Plantagenêts ont régné sur l’Angleterre pendant 300 ans et sont toujours très présents dans l’imaginaire britannique. Dans une courte vidéo réalisée en 2022 pour History Hit, l’historienne britannique Suzannah Lipscomb a confirmé que l’aristocratie anglaise appréciait la langue française, Thomas Boleyn (le meilleur francophone de la cour Tudor) souhaitant que sa fille, l’emblématique Anne Boleyn, maîtrise la langue française. Il faut également noter que la langue française jouit d’un incroyable prestige international puisqu’elle était la langue de culture des élites européennes et aussi la langue de la diplomatie internationale jusqu’à la Première Guerre mondiale. Les négociations de l’armistice de 1918 se sont déroulées en français, avec des interprètes du français vers l’allemand, mais les généraux français et les amiraux britanniques se parlaient en français.
Le français a laissé son empreinte sur la langue anglaise. Depuis le XVIe siècle, les Français sont fiers de la précision et de la clarté de la langue, incarnées dans les œuvres de grands esprits tels que René Descartes et Voltaire. Ces facteurs ont attiré l’écrivain irlandais Samuel Beckett, qui s’est mis à écrire en français, car en utilisant la langue anglaise, il finissait par en dire plus que ce qu’il voulait. Le professeur Kelly observe que le français dispose également d’un large éventail de ressources pour transmettre des nuances subtiles. Par exemple, nous avons l’utilisation délicate du “tu” familier et du “vous” formel pour s’adresser à une autre personne en disant “you” [la seule option en anglais], ce qui permet d’indiquer clairement le degré de familiarité [proximité] que l’on pense avoir [ou avoir développé] avec la personne, ou le statut que l’on pense que la personne a par rapport à nous, ou à la situation sociale spécifique et au contexte de l’interaction (par exemple, dans les affaires formelles/professionnelles ou dans les interactions sociales détendues/personnelles). Pour les anglophones s’intéressant à la langue et la culture française, il serait utile de savoir que l’utilisation du “tu” pour s’adresser à une personne est connue comme l’acte de tutoyer (le tutoiement) et l’utilisation du terme “vous” comme l’acte de vouvoyer (le vouvoiement). Il est généralement poli dans le monde Francophone de demander à une personne qu’on pense être devenue proche : « Permettez-vous qu’on se tutoie? » ou « Ça vous dérangerait si on se tutoyait ? »
Le professeur Kelly a fait remarquer que “Ce qui n’est pas clair n’est pas français”, cette expression inventée par l’écrivain du XVIIIe siècle Antoine Rivarol est devenue une expression favorite dans les écoles françaises : “si ce n’est pas clair, ce n’est pas français”, même si “cela peut être de l’anglais, de l’italien, du grec ou du latin”, Rivarol aurait ajouté. M. Kelly pense que beaucoup craignent que la précision finement aiguisée du français ne soit pas bien adaptée au monde actuel, qui évolue rapidement, où le langage sert souvent d’instrument émoussé et d’outil jetable, où de nombreux nouveaux mots dans les domaines de la science, de la technologie et de la culture populaire sont venus de l’anglais, ce qui a incité les universitaires français à dresser une liste d’équivalents français. Les mots français sont sans aucun doute plus beaux, mais ont tendance à être longs, ce qui, selon M. Kelly, ne convient pas toujours au langage abrégé des médias sociaux de l’ère technologique moderne.
Le professeur Kelly rappelle que le français est une langue importante à apprendre pour l’industrie britannique, car ses proches voisins européens [Belgique, Suisse, Luxembourg, régions du nord de l’Italie, îles Anglo-Normandes] fonctionnent aussi dans cette langue, et avec un empire global comparable et rivalisant à celui des Britanniques dans le passé, la langue Française est également largement répandue dans le monde francophone [par exemple, le Canada francophone, certaines parties de l’Afrique, l’Amérique du Nord, les Caraïbes, l’Amérique du Sud].
Londres est aujourd’hui considérée comme la sixième ville de France, avec un grand nombre de Français vivant au Royaume-Uni. M. Kelly observe que, malheureusement, trop peu d’Anglais ont les compétences linguistiques en français requises pour travailler dans les industries du monde francophone [par exemple, l’aérospatiale (du Concorde à Airbus), la défense, les télécommunications, l’énergie, l’eau (Compagnie Lyonnaise des Eaux), la mode et la beauté (L’Oréal, Chanel) et la finance (BNP Paribas). Le tourisme est également un facteur majeur de l’importance de la langue puisque les Britanniques représentent la plus grande proportion de visiteurs en France et qu’inversement, la Grande-Bretagne accueille plus de visiteurs de France que de n’importe où ailleurs, d’où l’intérêt d’apprendre la langue de l’autre en attendant que le monde devienne complètement francophone. Le français reste la langue la plus populaire auprès des apprenants à l’école, sur le lieu de travail et pour les loisirs au Royaume-Uni ; bien que d’autres langues gagnent également en popularité [comme l’espagnol], le Professeur Kelly souligne que la situation géographique du Royaume-Uni continuera à faire du français une langue vitale et une invitation constante au voyage.
Pour les étudiants avancés du français dans le monde anglo-saxon, l’essai “The «FRANÇAIS»: Verbs & Tenses for Advanced English Learners of French” peut aider.
—-|—-
[EN] Answer to Question IV. “Which one is the best language between French and English according to you?”
This is a tricky question because the term “best” here is quite vague. So, I will tend to think that a first class language should be clear, precise, practical, pleasant to ears, and the eyes, well-structured with the pronunciation reflected in the grammatical structure to prevent people from mispronouncing words and also hold an amount of depth that is reflected when expressing the thoughts of the high-level thinker, and one that holds an artistic value that allows it to be full of emotions when spoken as a human language through its timbre and tone.
The English language although practical because of its widespread use does lack the synchronisation between its grammatical structure and the way words are pronounced which results in even experienced native English speakers to mispronounce many words, in rare cases this could even lead to people being thought of as phonological dyslexics. This to me makes the English language inferior to the French language since the latter has a greater number of “accentuated signs” that precisely instruct the reader how to pronounce the words. Indeed, in the French language the majority of words are pronounced exactly as they are written once we learn the endings of verbal tenses and some grammatical rules.
The other factor when comparing the 2 most widespread languages of the civilised world, is the fact that the English language comes with a variety of accents from the different regions it is spoken [e.g. Scouse, Geordie, Cockney, Scottish, Irish, etc] and is often muffled in videos and can often lead to misunderstanding or may require the listener to repeat segments to fully comprehend, so this is another disadvantage of the English language. This is hardly the case with French because even in the different accents in which the language may be spoken, they always lead to a clearer sound due to the grammatical structure and rules of the language and hence a clearer hearing and hence a faster understanding when compared to English.
The English language also has a history grounded in empiricism and seems to simply fulfil the task of communicating instructions and scientific texts, but lacks the emotionality in works of art [e.g. Romanticism] and in philosophical arguments [e.g. Je pense, donc je suis!] compared to the French language. Note that I did not say that it cannot be used in works of art, but only pointing out that it is less intense when compared to the French language. English to me seems to lessen the intensity of philosophical arguments and human conversations being a fairly flat language in its written and spoken form. This may also be due to the fact that the anglosphere is generated from a majority of societies where the values of humanity, brotherhood and the individual are not at the heart of the civilisation as it is in France, but rather tend to be industrialised and mechanical societies that can only offer freedom as a form of extreme individuality bordering on selfishness based on an “each to their own” type formula in a savage game of self-survival and preservation at whatever cost. This is of course the major train of thought, because we do have a minority of incredible individuals from the English realm who stand out because of their own investment in cultivating unique and captivating personalities and who do not act and think like the common majority where it reflects in their behaviour, feelings and art works. Furthermore, the roots of the English language still connect to the outdated system of monarchy which seems to make the society obsessed with medieval stories of capes and swords: a system that seems to inculcate in the individual a sense of knowing the limits of one’s rights and unquestionable obedience; while the French language is rooted in the values of the revolution which inculcates questioning and a sense of pushing one’s own limits to unleash the “Emperor/King/Master” within ourselves, with the legend of Napoléon as proof – the philosophy and values of these two languages seem to oppose each other.
Hence, to me, being someone who received a bursary and studied literature, linguistics, psychology and philosophy while also having written for a long time and been drenched deeply in the cultural realm of both English and French, English seems like a language for communication, while French is a language that can achieve absolutely everything that English can, but also goes further by allowing the individual to not simply communicate, but also to “express themselves” [their depth, their thoughts, their emotions] in a way that the English language fails to capture at such intensity because of its founding history and structure that is not as focussed on timbre, philosophy, arts and the expression of feelings as the French language is.
So, since the French language can do everything that English can in the formal world, such as instructions, scientific writings and simple communication, but can also go to greater depth to touch humans deeper through its subtlety in timbre and sound embedded in a history of great poets, philosophers and thinkers who set their mark in marble and stone, I would have to say that the French language is superior to English.
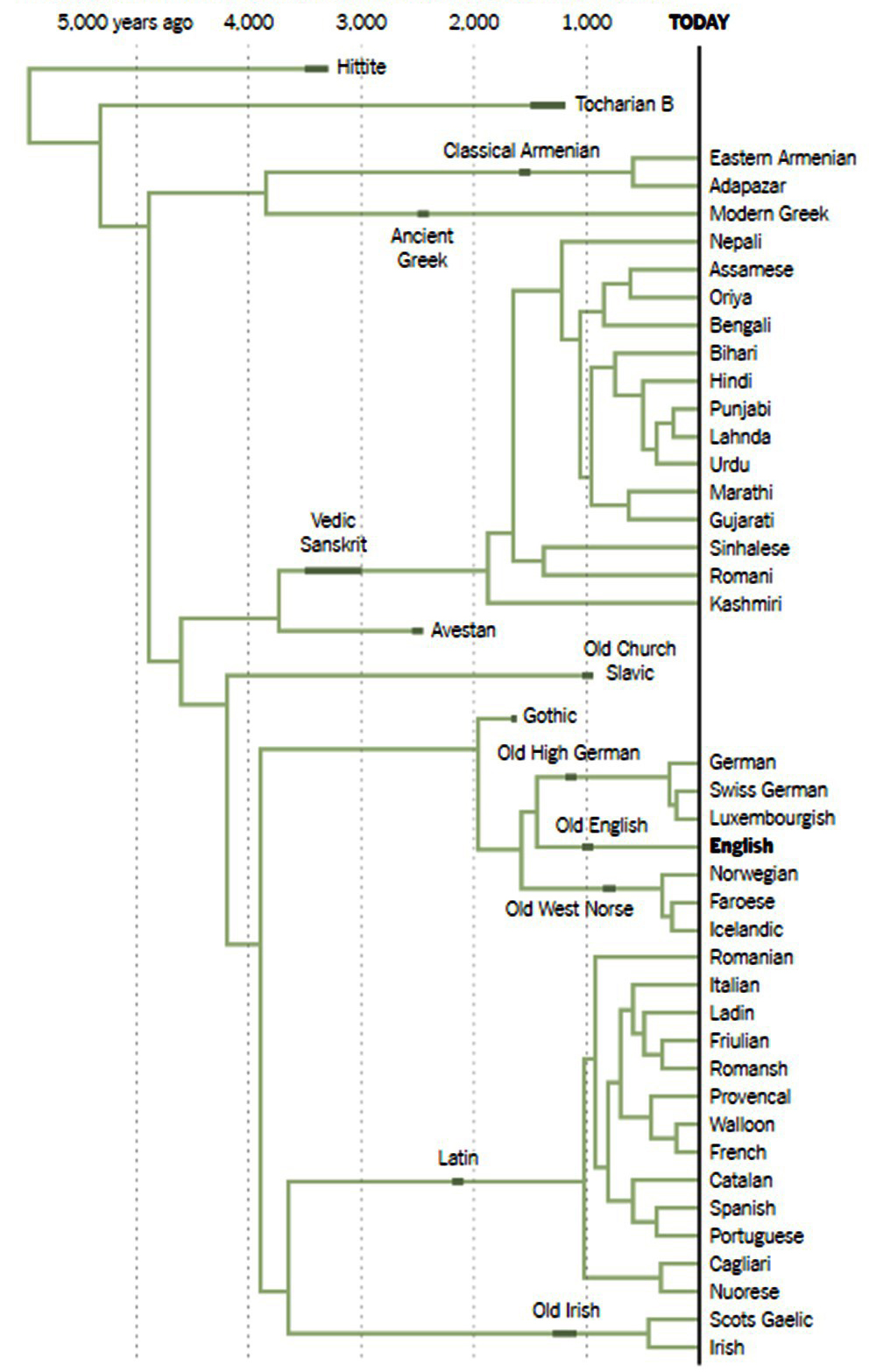
Image: Tree diagram showing the tangled roots of English / Source: NYT
Although it is important to note that these 2 languages are very close to each other in structure as many words are spelled similarly in both languages with minor changes from one to the other [e.g. Psychologie/Littérature is French for psychology/literature (English)]. Since both languages are of Indo-European origin, it is easier for English speakers to evolve and shift to French than most other languages – at least in written form since oral French requires practice and dedication to master; while a “soul” is another story involving metaphorical vision, abilities of synthesis, values, insight and depth of thought… and of course personality, emotions and sensibility.
Individuals who intend to share their wisdom and contribute to the world’s development would have an advantage in adopting and mastering a communicative pattern (i.e. language) deemed superior by the fact that it comes with modern human values and is weaved in the fabric of a more refined and sophisticated intellectual, psychosocial, philosophical and artistic heritage [e.g. French, which is the most desired and most spoken second language in the UK and in Germany] since it would be understood by the wider audience of the civilised world, where the major intellectual and cultural evolution/revolution takes place.
I would also like to point out for the majority of anglophones and fellow English people out there who hardly know their own cultural evolution that there is French on the emblem of the British monarchy.
![Dieu et mon droit [Royal_Coat_of_Arms_of_the_United_Kingdom]](https://dpurb.com/wp-content/uploads/2019/04/dieu-et-mon-droit-royal_coat_of_arms_of_the_united_kingdom.jpg)
Image: The « Français » on the Royal Coat of Arms of the United Kingdom
The words, “Dieu et mon droit” have been the motto since the time of Henry V (1413 – 1422), and since those times old English is not the language of the English elite anymore which resulted to the use of words and expressions of French and Norman origin that are now widely used in the English language.
French has also been identified as an important language for the UK’s future. In an articled published by the British Council in 2014, Professor Michael Kelly, who heads the Modern Langages Department at the University of Southampton described the “je ne sais quoi” in learning to master the French language; the British see French as the language of love as he pointed out, and the French language has a romance to the English speaker’s ear. It is the French culture that sparked the “wow” factor for Kelly who admitted being “bowled over by the depth of feeling” and still getting the tingles when coming across the works of Charles Baudelaire, with “L’invitation au voyage” taking him on a journey to a country where “tout n’est qu’ordre et beauté, luxe, calme et volupté” [French for : “all is order and beauty, luxury, peace, and pleasure” – quoted from Baudelaire’s poem]. Professor Kelly argued that to him, this sums up France at its best. Kelly writes that when words are said in French, they conjure up a world beyond their ordinary English counterparts; what marks French as a romantic language for the British is that it can almost but not fully be understood. Since it is not used all the time, the English do not get the overlay of everyday meanings that may crowd out the magic for some native French speakers, and according to Kelly, this may be why the British see French as the “language of love”.
French has left a lasting impression on the English language and like most other countries, the French do talk, write and sing about love, however, the British, Kelly points out, suspect that the French are more articulate about love, unlike the more ‘buttoned-up English’, who flounder like Hugh Grant in “Four Weddings and a Funeral”. The difference, Kelly observes, is the culture, not simply the language. Culture is a vital factor, and part of the romance of the French language to the British is linked to the fact that it was the language of the English aristocracy in the Middle Ages: the Normans and the Plantagenets ruled England for 300 years and still have a strong presence in the British imagination.
In a short video in 2022 for History Hit, British historian, Professor Suzannah Lipscomb brought in the confirmation that the English aristocracy valued the French language, with Thomas Boleyn [the best French speaker at the Tudor court] wanting his daughter, the iconic Anne Boleyn to master the French language.
It is also to be noted that the French language has incredible international prestige since it was the language of culture for the European elites and also the language of international diplomacy up to the First World War. The negotiations for the Armistice in 1918 were conducted in French, with interpreters of French to German, however, the French generals and British admirals spoke to each other in French.
French left its mark on the English language, and since the 16th century the French have taken pride in the precision and clarity of the language, embodied in the works of great minds such as René Descartes and Voltaire. Those factors attracted the Irish writer Samuel Beckett, who switched to writing in French, since in using the English language, the latter would end up saying more that he intended. French also has a wide range of resources to convey subtle nuances, for example, we have the delicate use of the familiar ‘tu’ and formal ‘vous’ to address another person as ‘you’ [the only option in English], making it clear what degree of familiarity [closeness] one feels one has [or has developed] with the person, or the status one thinks the person has in regards to oneself or the specific social situation and context of the interaction [e.g. in formal/professional matters or relaxed/personal social interaction]. The use of “tu” to address a person is known as the act of “tutoyer” (the “tutoiement”) and the use of “vous” as the act of vouvoyer (the “vouvoiement”). It is generally polite to ask someone in the Francophone sphere whom one believes to have become closer to, “Permettez-vous qu’on se tutoie?” or « Ça vous dérangerait si on se tutoyait ? » [French for: “Would you mind if we used ‘tu’ towards each other?].
Professor Kelly observed that ‘Ce qui n’est pas clair n’est pas français’, coined by the 18th century writer Antoine Rivarol, became a pet phrase in French schools: ‘if it’s not clear, it’s not French’, though ‘it could be English, Italian, Greek or Latin’, Rivarol had added. Kelly points out that many fear that the finely honed precision of French may not be well suited to the fast-moving world of today, where language often serves as a blunt instrument and a disposable tool, where many new words in science, technology and popular culture have come from English, which has sparked the French academics to generate a list of French equivalents; he however admits that French words undoubtedly sounds more beautiful, but tends to be rather long-winded, which Kelly believes does not always fit in the abbreviated language of social media of the modern technological era.
Kelly notes that French is a significant language to learn for the UK industry since close neighbours in Europe [Belgium, Switzerland, Luxembourg, regions of Northern Italy, Channel Islands] also function with it, and with a global empire comparable to and competing with that of the British in the past, the french language is also widely distributed across the Francophone world [e.g. French-speaking Canada, some parts of Africa, North America, the Caribbean, South America].
London is nowadays considered as France’s sixth biggest city with large numbers of French people living in the UK. Kelly observes that unfortunately, not enough English people have the French language skills required to work in industries in the Francophone world [e.g. aerospace (from Concorde to Airbus), defence, telecommunications, energy, water (Compagnie Lyonnaise des Eaux), fashion and beauty (L’Oréal, Chanel) and finance (BNP Paribas). Tourism is also a major factor in the importance of language since the British are the largest proportion of visitors to France and conversely, Britain welcomes more visitors from France than from anywhere else, hence there is every incentive in learning each other’s language until the world becomes fully francophone. French remains the most popular language for learners in school, in the workplace and for leisure in the UK; although other languages are also growing in popularity [such as Spanish], Kelly reminds that the geographical situation of the UK will continue to make French a vital language and a constant invitation to a journey.
For advanced learners of French in the Anglo-Saxon world, the essay “The «FRANÇAIS»: Verbs & Tenses for Advanced English Learners of French” may help.
_________________________________
QUESTION V.
[FR] – De quelle civilisation vous sentez-vous faire partie ?
[EN] – What civilisation do you feel a part of?
[FR] Réponse:
C’est certainement la question la moins compliquée jusqu’à présent car je me suis toujours présenté et décrit comme un Européen occidental franco-britannique qui vit en Angleterre et qui a l’intention d’alterner périodiquement avec la France à l’avenir. Donc, en passant par-là, je peux honnêtement dire que je défends la civilisation de l’Europe de l’Ouest et la France avant tout, avec bien sûr, une forte connexion et une préoccupation pour la société anglaise puisque c’est ici que j’ai vécu et que c’est aussi là que j’ai grandi et évolué pour devenir la personne que je suis aujourd’hui et qui n’est plus qu’à deux pas de la France. Pour moi, en tant qu’individu faisant partie de la classe intellectuelle de sa génération, c’était toujours l’Europe de l’Ouest où mon destin allait se dérouler et où mes œuvres allaient atteindre le public qui leur était dû. Mon passé d’adolescent n’a porté que sur les fondements de mon éducation qui allait toujours être poursuivie et affinée en France ou en Angleterre car l’île où je suis né aujourd’hui est trop petite et compte une population d’environ 1 million d’habitants, et bien plus comme une mini station de vacances 5 étoiles aux paysages naturels à couper le souffle, c’est un endroit parfait pour se déconnecter, méditer dans la solitude, se détendre, réfléchir, créer et écrire, mais pour moi ce n’est pas assez grand en géographie et en population pour favoriser le développement d’une élite littéraire qui a étudié toutes les grandes œuvres européennes et qui a une vision universelle de la psychologie, de la philosophie et de la gestion de la civilisation. C’est une histoire similaire à celle de Napoléon qui a dû quitter la Corse et aller en France pour découvrir et libérer sa propre grandeur et son génie.
Donc, pour en revenir à la question, pour moi, un homme qui vit dans le présent, je suis et je me sens partie de l’empire français avec des liens forts avec la société britannique et surtout les intellectuels d’Oxford qui m’ont soutenu au fil des ans dans mes recherches en tant que consultant indépendant, intellectuel, chercheur, philosophe et écrivain qui trouve son inspiration dans le monde. Je dis donc que je suis un ami du peuple et de la société britannique et le réveil de l’empire français à une époque où la passion est morte et où la corruption et les bureaucrates ennuyeux, inaptes et peu créatifs se sont surtout concentrés sur leurs propres poches sans aucune vision ont mis un terme déprimant à la civilisation. D’une certaine manière, j’ai parfois l’impression qu’il est de mon devoir de consacrer cette vie à remettre la société française et l’Europe de l’Ouest sur sa glorieuse voie.

Image: L’Académie Française, Paris
M’attaquer, c’est attaquer l’empire français et la civilisation d’Europe de l’Ouest ! Parce qu’à l’heure actuelle, il n’y a pas d’autre personne qui ait un cœur entièrement dévoué à son avenir et un cerveau à la hauteur de la grandeur qui l’accompagne ! Il s’agit d’un simple énoncé des faits, et non d’une vantardise insensée !

—-|—-
[EN] Answer to Question V. “What civilisation do you feel a part of?”
This is definitely the less complicated question so far because I have always introduced and described myself as a Franco-British western European who lives in England and who intends to periodically alternate with France in the future. So, going by this I can honestly say that I stand for the Western European civilisation and France primarily, with of course, a strong connection and concern for the English society since this has been my home and also the place where I matured and evolved into the person that I am today and which is only a stone’s throw away from France. To me, as an individual who is part of the intellectual class of his generation, it was always going to be Western Europe where my destiny would unfold and where my works would reach its rightful audience. My teenage past only involved the foundations of my education that was also always going to be pursued and refined in France or England since the island where I was born today is too small in size and a population of 1 million approximately and much more like a mini 5-star holiday resort with stunning natural sceneries, making it a perfect place to disconnect, meditate in solitude, relax, brain storm, create and write, but to me it is not large enough in geography and population, to foster the development of an elite literary man who studied all the great European works and who has a universal outlook on psychology, philosophy and the management of civilisation. It is a similar story to that of Napoleon who had to leave Corsica and go to France to discover and unleash his own grandeur and genius.
So, getting back to the question, for me, a man who lives in the present, I am and I feel part of the French empire with strong links with British society and especially the intellectuals of Oxford who have supported me in my research over the years as an independent consultant, intellectual, researcher, philosopher and writer who finds his inspiration in the world.
So I say that I am a friend of the British people and the awakening of the French Empire at a time where passion has died because corrupt, boring, incompetent and uncreative bureaucrats focused mainly on their own pockets without any vision have brought civilization to a depressing halt. In a way, I sometimes feel that it is my duty to devote this life to putting French society and Western Europe back on its glorious path.
Attacking me, means attacking the French empire and Western European civilisation! Because at this point in time there is no other person with a heart completely dedicated to their future with a brain that matches the grandeur to go along with it! This is a simple statement of facts, not mindless boasting!
_________________________________
QUESTION VI.
[FR] – Êtes-vous un fan d’Hitler ?
[EN] – Are you a Hitler fan?

[FR] Réponse:
Je suppose que cette question m’est posée parce que j’ai souvent lié des vidéos d’Hitler dans mes essais et mes écrits.
Eh bien, pour commencer, je n’ai jamais tout à fait compris le terme “fan”, parce que cela semble impliquer une certaine forme d’obsession pour une personne en particulier. Non, j’ai admiré les œuvres et les valeurs de beaucoup de gens, et si cela me qualifie de “fan”, alors je le suis peut-être. “Admiration” pour “certains” aspects des œuvres de nombreux grands hommes et femmes à travers l’histoire – ce qui fait de moi un admirateur d’œuvres étonnantes avec du respect pour l’artiste ou le créateur. Cela s’étend à Adolf Hitler, qui, je dirais, avait raison sur bien des points en ce qui concerne la gestion d’une civilisation, mais pas sur tout. Lui ou ses conseillers ont commis des erreurs, comme la plupart des humains, qui lui ont tout coûté, à lui et à son régime.
Je dirais donc que j’admire beaucoup de philosophies et de réalisations d’Hitler, comme la nécessité d’unir le peuple en débarrassant le pays des divisions de gauche, du centre et de droite, tout en critiquant certaines de ses procédures, car après tout, il était un être humain qui n’a vécu que la réalité de son époque, alors que je vis en 2021 et vois les choses sous un autre angle car je suis privilégié d’avoir reçu une grande part des connaissances et découvertes scientifiques que l’époque d’Hitler n’avait pas encore mises au point. L’avancement de la technologie a permis aujourd’hui d’être extrêmement mobile puisque la plupart des grands travaux et recherches sont maintenant disponibles sous forme numérique, ce qui a rendu le monde plus connecté sans qu’il soit absolument nécessaire de se rendre dans d’anciennes bibliothèques pour trouver des ressources universitaires, et d’une certaine manière, nous pourrions gérer une équipe ou une entreprise en Europe depuis la jungle amazonienne, depuis une cabane forestière au Mexique ou une tente au Danemark, tant que nous aurons la haute vitesse et la bonne technologie – imaginez ce que de Vinci aurait réalisé si nous avions ceux-là en son temps !

Source: Leonard de Vinci: Accélérateur de Science (2017)
Pour commencer par le dossier hitlérien, ce n’est pas une réponse simple car il y a beaucoup de choses à dire et à expliquer pour que les gens du monde entier puissent comprendre mon point de vue et aussi comprendre toute la controverse entourant le “Führer”. En répondant à cette question, je me référerai également à la “Théorie organique” pour expliquer l’existence, l’adaptation et l’évolution de l’homme et je me référerai également à mon propre cas en tant qu’Européen de l’Ouest franco-britannique assimilé, assez similaire au cas de Hitler ou de Napoléon qui n’étaient tous deux pas originaires de leur société, mais étaient assimilés, étonnamment, il semble que les deux dirigeants les plus puissants d’Europe occidentale aient dû venir d’un autre pays comme envoyés par le destin pour résoudre les problèmes d’une civilisation qui n’avait pas de chef légendaire avec une vision parmi son peuple, et qui a reçu un chef qui a gagné son appartenance et est devenu plus national que les nationaux eux-mêmes. Hitler est né en Autriche, tandis que Napoléon est né en Corse, et peut-être étonnamment 7 ans avant la naissance du futur empereur de France, Rousseau disait que la Corse allait secouer l’Europe.
Je dois dire que, dès mon plus jeune âge, j’ai été fasciné par la réputation d’Adolf Hitler parce que, comme la grande majorité d’entre nous, on nous a tous enseigné qu’il était la personne la plus horrible qui ait jamais existé dans l’histoire humaine, et son obsession meurtrière pour le génocide des Juifs était une chose que tout homme sain ne pouvait justifier. Comme la plupart des gens qui ont grandi entre la fin des années 80 et la fin des années 90, l’information était et est toujours principalement diffusée par les principaux médias à majorité juive, à une époque où l’Internet était encore en plein essor – en particulier les sites de streaming vidéo – j’ai donc été obligé de digérer la seule perspective à ma disposition jusqu’à une décennie dans le millénaire où un grand nombre de fichiers Hitler qui étaient enterrés commençait à apparaître partout sur Internet, donnant une perspective plus claire du monde et ses implications économiques, philosophiques et religieuses des deux côtés du débat.
Il y a aussi la grande confusion, la mauvaise interprétation et la fabrication médiatique de commérages qui existent concernant le prétendu désir de conquête du monde et l’obsession d’Hitler pour la prétendue supériorité de la race caucasienne germanique, particulièrement le sous-type nordique aux cheveux blonds et aux yeux bleus qui devrait à la longue remplacer toutes les autres races qui ne sont pas d’origine allemande – comme beaucoup de sociétés inférieures en Europe de l’Est avec un certain nombre de juifs et musulmans, etc. par e.x. La Pologne, la Bosnie, la République tchétchène et la Russie, qu’il considérait comme bon marché et de culture inférieure, les comparant à des animaux mineurs – du moins c’est ce qu’on disait et faisait croire à la majorité. Si les sociétés d’Europe de l’Est ne sont peut-être pas aussi sophistiquées que les sociétés d’Europe de l’Ouest, cette hypothèse de sous-type inférieur et supérieur ne reposant que sur l’héritage génétique et les attributs physiques n’est pas scientifiquement valable car nous savons maintenant que les organismes peuvent être formés avec les conseils et l’éducation appropriés pour s’adapter à leurs sociétés choisies et cela devrait être le cas si un empire conquiert et prend de l’ampleur, et aussi que le talent et le génie, bien que très rare, peuvent apparaître et a émergé de différentes sociétés et compositions organique, de n’importe quel coin du globe, et cela prouve qu’un organisme supérieur [intellectuellement ou physiquement] peut naître de n’importe quelle société et faire partie de n’importe quel type de composition organique, non seulement le sous-type nordique de la race caucasienne germanique, voire même Mussolini qui était un autre dirigeant fasciste et nationaliste était en désaccord avec Hitler sur cette question du sous-type nordique, et il a dit ne croire à la supériorité d’un seul sous-type particulier mais de la qualité générale de tous les sous-types, dont le sous-type méditerranéen aux cheveux bruns qui crée un mélange sain parmi le peuple national.
Cependant, l’amplification de l’argument d’Hitler en un désir d’extermination a créé beaucoup de confusion et a été encore exagérée et amplifiée par la presse commérageuse majoritairement détenue et gérée par les Juifs pour donner au régime hitlérien une mauvaise publicité et une haine mondiale. En ce qui concerne les enregistrements, nous savons seulement qu’Hitler s’est concentré sur des questions nationales et a clairement demandé à tous les autres pays de le laisser, lui et l’Allemagne, se concentrer seuls sur leur propre société et d’être autorisés à façonner leur société comme ils l’ont souhaité, car ils ont tout hérité de leurs ancêtres et ont voulu préserver leur société après avoir reçu l’autorisation de le faire dans des élections démocratiques, et aussi garder la race nationale allemande “pure”[ce qui n’avait bien sûr aucun sens car aucune race n’est pure puisque nous sommes le résultat de la migration, du métissage et de l’évolution de différents sous-types et Hitler lui-même était le résultat de la consanguinité entre un homme et sa nièce, le type d’union que Charles Darwin, l’homme derrière la théorie de l’évolution, s’opposait lui-même ainsi que le mariage entre cousins qu’il tentait de rendre illicite par loi à cause des nombreuses malformations et de l’incapacité des enfants qu’a entraîné ainsi que les mauvaises gènes que cela propagerait].
Donc, pour commencer à répondre à votre question, je dirai d’abord que Hitler était un patriote convaincu et un défenseur de la société et du peuple qu’il représentait [pas différent de moi et de mes vues pour la France et l’Europe occidentale en fait] et que pour renforcer un pays de plusieurs façons, l’accent devrait d’abord être mis sur ceux qui font partie du peuple natif du pays, s’y reconnaissent et l’aiment, c’est une philosophie qui s’inscrit dans le droit fil de la bonne gestion d’une civilisation et de ma propre philosophie de la “Théorie organique”, mais seulement en partie parce que la solution complète implique aussi la prise en compte de l’afflux de talents et l’adaptation évolutive d’autres organismes qualifiés qui contribuent également au maintien et au progrès de la nation et qui ont acquis leur origine nationale et s’identifient complètement à la nation, en faisant partie intégrante de celle-ci.
Malheureusement, Hitler et ses conseillers ont exagéré et mal interprété la compréhension de l’évolution organique et ont suivi une politique atavique et rétrograde avec une équipe qui a procédé sauvagement, sans considérer attentivement la logique fondamentale qui existe dans tous les domaines de la vie, à savoir que nous avons toujours eu des exceptions aux règles pour les cas exceptionnels – cela s’applique aux mathématiques, aux arts, à la médecine, aux sciences – qui devraient également s’appliquer à tout système jugé pratique, moderne et évolué. Tous les organismes de cette planète s’adaptent et évoluent d’un point de vue organique et sociolinguistique, mais pas de la même façon et comme je l’ai dit, si les lois de la nature et de l’évolution qui contiennent toute vie sur terre en décidaient autrement, alors les organismes de différentes compositions organiques ne seraient pas capables de procréer.
L’équipe d’Hitler était aussi composée de nombreux traîtres avec une éducation assez élémentaire qui ont pris des décisions meurtrières qu’ils ont cachées au “Führer”, entraînant sa chute et l’annihilation complète de ses plans et de son système ; vers la fin ils ont tous mis la faute sur un homme comme si Hitler avait drogué une nation entière et les avait hypnotisés en marionnettes mécaniques – qui est aussi clairement impossible sans la foi, la volonté et le désir de la nation à se diriger vers la vision.

Cette photo de Hitler embrassant une fillette juive s’est vendue 11 520 dollars aux enchères / Source: VanityFair
Il convient également de mentionner qu’à ce jour, pas un seul enregistrement ou message écrit n’a été trouvé de Hitler donnant le feu vert à l’extermination d’un peuple, et ce qui peut être conclu aujourd’hui est que Hitler croyait que toutes les sociétés et races devraient simplement être nationalisées afin que toutes les sociétés et races puissent se comporter mieux et se perfectionner comme le Reich allemand. Sur la question des massacres de masse, le blâme aujourd’hui, selon les faits qui ont été recueillis, est principalement attribué à Göring et Himmler, ce dernier passant par les anciennes écritures aryennes de l’hindouisme se croyant agir comme le grand guerrier Arjuna qui purgeait son peuple et le monde entier du mal et qui croyait qu’à long terme les gens le verraient comme le héros mythologique nettoyant la terre du mal qui était pour lui les Juifs et leurs valeurs étant la cause de toute souffrance humaine sur terre comme ils détruisent les autres civilisations et déforme et contrôle les pensées des masses par leurs activités médiatiques.
Tout d’abord, j’expliquerai ce que je critique à l’égard du régime hitlérien avant d’expliquer ce que je considère comme admirable dans la légende d’Adolf Hitler en tant que leader et être humain sur cette planète. Il y a deux ou trois choses que je pense sincèrement ne sont pas acceptables dans la société éclairée d’aujourd’hui en 2021, et Hitler aurait construit un Reich plus fort s’il avait été mieux conseillé dans des politiques plus intelligentes concernant la gestion, le maintien et la formation d’une population productive et sophistiquée avec des sentiments patriotiques forts et un sentiment de synchronisation et de compréhension. Hitler ne visait pas simplement à créer une entreprise de boulettes de viande roses, mais était un leader cultivé guidé par la philosophie, l’éthique, la morale, la dignité, les valeurs et les arts et voulait que le monde entier regarde l’allemand comme un modèle héroïque à suivre et à être inspiré par. Hitler voulait que les gens voient les honorables SS comme des héros légendaires qui voulaient faire du monde un endroit meilleur. Adolf Hitler n’était pas un porc ou un simple soldat.

Image: Des photos de Henrich Hoffmann, le photographe d’Hitler, numérisés, restaurés et publiés pour la première fois (2019)
Il est fondamental de comprendre qu’à l’époque d’Hitler, l’Allemagne se faisait conquérir par des communistes méthodiquement concentrés sur la prise de pouvoir de l’Allemagne sans véritable sentiment d’appartenance, avec l’intention de la transformer en une forme de zone commerciale et une arrière-cour économique en Europe, semblable à ce que les génies influents du monde des affaires, principalement juifs, ont fait des Etats-Unis aujourd’hui – une société mécanisée, industrialisée, dépourvue d’humanité et de valeurs, où l’individualisme égoïste a laissé chacun dans une lutte constante pour survivre à tout prix, même si cela signifie se tuer mutuellement, ce qui est aussi courant lorsque les armes sont légales là-bas. Les dirigeants de ces groupes communistes en Allemagne à l’époque d’Hitler étaient composés d’une majorité d’étrangers, dont de nombreux Juifs. Alors que le nombre de morts de Juifs a été exagéré et utilisé pour diffamer Hitler, aucune attention particulière n’a été accordée au nombre de morts horribles que les Juifs ont causées pendant la révolution russe et de nombreux historiens révisionnistes ont affirmé que le nombre de morts était beaucoup plus élevé que le régime hitlérien. Cependant, il était clair qu’en plus de l’immigration juive et des influences politiques des communistes juifs qui affaiblissaient et corrompaient progressivement la société allemande, il y avait aussi un énorme problème avec l’immigration de populations qui n’étaient pas des Allemands de souche. Cela impliquait que pour qu’un homme comme Hitler puisse réaliser son rêve d’une Allemagne forte, stable et moderne, il aurait fallu s’attaquer à la question de l’immigration, et comme il avait une vision nationale et d’excellence, le fait de se débarrasser d’une foule excessive, incompatible et étrangère qui ne voulait pas s’assimiler pleinement et devenir citoyen allemand était une chose nécessaire dans sa vision.
Cependant, il ne fait aucun doute qu’Hitler aurait aussi dû se rendre compte qu’il y avait un grand nombre d’êtres humains très talentueux et complètement assimilés dans la société allemande qui devaient être conservés et traités comme des citoyens qui avaient acquis leur origine et un fort sentiment d’identification avec la foule native par leur propre adaptation et évolution. Et comme ce n’était pas le cas, nous nous sommes retrouvés avec la Seconde Guerre mondiale, de nombreuses personnes mourant dans des camps de détention mal approvisionnés après que les alliés eurent bombardé les voies ferrées de liaison et perturbé l’approvisionnement alimentaire et hygiénique, provoquant une épidémie de typhus qui a fait des milliers de morts. En outre, de nombreux Allemands qui avaient un lien lointain avec la population juive ont été traités comme des criminels à déporter, ce qui a conduit à une opération irrationnelle qui a écarté des personnes qui étaient parfaitement aptes à faire partie d’une société fonctionnelle, les normes scientifiques actuelles ayant prouvé, avec une interprétation correcte de la théorie de l’évolution, que nous sommes des organismes qui peuvent adapter et changer leur identité pour qu’elle soit en accord avec les nouveaux environnements, si nous faisons les bons choix et avons les capacités et la motivation pour le faire. Les lois de Nuremberg qui définissaient celui qui devait être qualifié d’allemand sur la base de la généalogie étaient l’une des décisions les plus irrationnelles et les plus stupides du Reich allemand puisqu’elle n’était fondée sur aucune bonne science. Il était alors nécessaire pour les Allemands de prouver que leurs parents et grands-parents n’avaient pas d’ascendance juive ; c’était hypocrite car Hitler lui-même ne pouvait prouver qu’il n’avait aucun lien génétique juif parce que son grand-père[le père de son père] est inconnu ; et beaucoup ont suggéré qu’il était l’enfant illégitime d’un riche membre d’une grande famille juive après une relation adultérine avec sa grand-mère que la famille avait engagée comme servante ou cuisinière. De plus, d’après la définition de l’Aryen soi-disant “parfait” qui est censé être blond, aux yeux bleus, mince, grand, aucun des plus hauts dirigeants nazis ne partageait ces caractéristiques physiques : Hitler n’était pas blond, Goebbels n’était pas grand et Goering n’était pas mince.
L’autre côté, c’était celui de la supériorité du peuple allemand dont Hitler était obsédé et qui s’avéra en fait peu créatif en ne considérant pas les personnes ayant une part d’héritage et d’appartenance culturelle allemande comme un exemple de conquête allemande, car c’était aussi un moyen pour une civilisation de diffuser ses gènes plus largement et d’encourager les personnes résultant de ce mélange à se mélanger avec la civilisation fondatrice qui conduirait à leur future lignée de partager une quantité encore plus importante de gènes allemands. En fait, si la science et l’évolution ainsi que la supériorité en moyenne de la “race aryenne” ont guidé la politique du régime national-socialiste, elles auraient dû également encourager la diffusion du génome aryen en encourageant les hommes et les femmes les plus sains et les meilleurs de la race aryenne à donner des ovules et du sperme et encourager les couples à utiliser des donneurs sains de la race aryenne pour élever leurs enfants, et ce service aurait dû être offert aux couples de toutes conditions sociales pour prévenir la formation de malformations et d’organismes malsains. Cela aurait été une façon sophistiquée et moderne de penser l’évolution humaine et l’évolution sociétale à la manière hitlérienne. Une façon de dire est que pour changer leur société biologiquement, une bonne façon est de s’assurer qu’ils ont assez de “tartelettes à la crème”. Parce qu’après tout, je crois qu’il faut donner aux êtres humains la liberté de choisir leur partenariat, ce qui n’était pas le cas dans le Reich, car les Allemands natifs qui ne se reproduisaient pas avec des Allemands natifs étaient considérés comme des traîtres.
Par conséquent, cette forme d’extrémisme était l’une des principales doctrines qui ont conduit à tant de haine et de ressentiment envers le Troisième Reich de la part d’un grand nombre d’Allemands eux-mêmes, amenant une armée alliée à travailler constamment pour faire tomber tout le spectacle, bien que la partie adverse représente les valeurs d’une société qui ne sont pas meilleures en fournissant une solution à une civilisation harmonieuse mais qui sont surtout alimentés par la haine, de fortes motivations financières juives et le désir de paralyser l’Allemagne à tout prix, mais surtout de faire tomber le charismatique et trop puissant Adolf Hitler, comme c’est souvent le cas quand un homme doué monte au sommet et éclipse sa compétition avec son talent et son magnétisme.

C’est aussi le cas de Napoléon, lorsque l’Europe entière avait rassemblé toutes ses forces pour le faire tomber, cette vieille et sclérosée Europe des Rois unie pour détruire tous les acquis de la Révolution [la liberté et l’égalité des chances pour tous] et rétablir l’Ancien Régime inégalitaire en France. Cela semble être le cas aujourd’hui, comme si la société ne pouvait accepter que certains organismes soient supérieurs à la majorité médiocre. Cela semble hypocrite puisque nous pouvons tous aujourd’hui accepter que nous avons une nourriture supérieure d’un point de vue nutritionnel, des ordinateurs supérieurs, des voitures supérieures, des joueurs de football supérieurs, des montres supérieures, des caméras supérieures, des guitares supérieures, des pianos supérieurs, des chevaux supérieurs, donc cela devrait aussi s’appliquer à l’organisme humain, ce qui signifie que nous avons aussi des individus supérieurs avec une intelligence supérieure, donc une vision et une gestion supérieures. Il est également important de noter que les objets supérieurs sont toujours rares, et donc minoritaires, c’est pourquoi leur valeur est immense. Si les diamants étaient aussi abondants que l’acier et si l’acier était aussi rare que les diamants, alors les bijoux seraient faits d’acier et les diamants seraient utilisés dans la construction. Ainsi, nous semblons vivre dans un monde où la médiocrité des masses semble avoir de la difficulté à accepter que certains individus soient supérieurs dans leur ensemble, et au lieu d’encourager, d’apprendre, d’être inspirés et fiers d’être dirigés par de tels individus, nous semblons plutôt trouver une union de médiocrité qui fait tout son possible pour faire tomber ces individus. C’est quelque chose sur quoi la société doit travailler à l’échelle mondiale, pour favoriser l’excellence ! Le respect et l’appréciation sont après tout des mots qui existent dans tous les dictionnaires, et les êtres nobles et cultivés savent comment les montrer, et ceux qui n’ont jamais considéré ces valeurs peuvent essayer d’apprendre, cela en ferait certainement des êtres plus complets.
Pour en revenir à la gestion de la population de l’Allemagne pour une nation saine, forte et stable, Hitler aurait dû trouver une forme systématique de ” filtration “, impliquant des formes d’interview, d’évaluation de la santé, d’évaluation des compétences et d’évaluation culturelle qui analysaient tout le segment de la population allemande d’origine étrangère en tout ou en partie, et les diviser en deux groupes : ceux qui étaient aptes, sûrs et synchronisés avec la société allemande à garder, et ceux qui constituaient un fardeau en raison de leur incapacité à s’adapter et de leur refus d’être allemands en raison de convictions religieuses ou étrangères fermes d’être transférés diplomatiquement dans un environnement et une société plus adaptés à leurs caractéristiques, de la manière la plus respectueuse qui soit. Ceux qui ont été jugés aptes à la société allemande auraient même pu bénéficier d’une forme de classification [sous-type de la société allemande] s’ils l’avaient jugé nécessaire et auraient également dû prêter serment d’allégeance et de priorité à leur identité nouvellement trouvée et aux personnes qu’ils auraient dû respecter si c’était là où ils pensaient appartenir, sinon, il serait préférable pour un individu de se déplacer et de vivre dans une société compatible avec son patrimoine et avec les personnes dont il se sent membre, car aujourd’hui, en 2021, l’inégalité des revenus a diminué et le monde devient une planète plus égalitaire ainsi que les progrès technologiques qui rendent la vie assez semblable d’une partie du monde à une autre. Les organismes assimilés pourraient également avoir droit à 3 avertissements avant d’envisager de les expulser pour non-respect de leur contrat d’allégeance après des infractions graves, devenant ainsi des “traîtres” à la nation.
La solution de la filtration n’a pas été facile, mais en fait, c’était une solution sophistiquée qui aurait été plus adaptée à une civilisation qui évoluait et devenait de plus en plus complexe, décennie après décennie – nous ne pouvons pas nous attendre à des solutions faciles pour convenir à une civilisation complexe. Ce n’était bien sûr pas la solution choisie par le régime, mais la voie la plus rapide et la plus facile pour déporter tous les Juifs, non allemands et partiellement juifs, ce qui a entraîné tant de souffrances inutiles et de malentendus, alors que beaucoup de ces personnes n’étaient même pas religieuses et se considéraient plus allemandes que toute autre religion, comme Sigmund Freud qui était un produit de la pensée intellectuelle de la tradition allemande et qui, par la suite, a influencé la psychologie globalement, ou encore Albert Einstein qui était également sans sentiments religieux et a dû se rendre aux Etats-Unis pour s’exiler.
Il est également important de rappeler que les politiques conçues par le régime national-socialiste visaient également toutes les personnes considérées comme un fardeau et inutiles au progrès de la société allemande, ce qui a également conduit à l’euthanasie de nombreux Allemands pour des maladies génétiques et autres maladies incurables considérées comme impures pour une société et une race saine, ainsi que de nombreuses personnes âgées considérées comme inaptes à vivre.

Image : Dégénérés / Certains médecins controversés sous le Troisième Reich ont proposé que la malédiction des gènes malades détruisent des familles entières, et que les dégénérés ne peuvent que donner naissance à leurs semblables. Cela a conduit à la stérilisation qui devait les empêcher de répandre leur misère sur des enfants innocents [car l’objectif était un peuple fort et génétiquement sain], ainsi qu’au programme ” Aktion T4 ” qui était l’euthanasie massive involontaire. Certains médecins allemands étaient autorisés à sélectionner des patients ” réputés incurablement malades, après un examen médical des plus critiques ” et à leur administrer ensuite une ” mort par miséricorde ” (Gnadentod). De septembre 1939 jusqu’à la fin de la guerre en 1945, de 275 000 à 300 000 personnes furent euthanasiées dans des hôpitaux psychiatriques en Allemagne et en Autriche, la Pologne occupée et le Protectorat de Bohême et de Moravie (maintenant la République tchèque). Le Saint-Siège annonça le 2 décembre 1940 que cette politique était contraire à la loi divine naturelle et positive et que ” le meurtre direct d’une personne innocente en raison de défauts mentaux ou physiques n’est pas permis ” mais la déclaration ne fut pas confirmée par certaines autorités catholiques en Allemagne. Au cours de l’été 1941, l’évêque de Münster, Clemens von Galen, mena des protestations en Allemagne, dont l’intervention conduisit au ” mouvement de protestation le plus fort, le plus explicite et le plus étendu contre toute politique depuis le début du Troisième Reich “, selon l’historien Richard J. Evans.
Cela montre donc que même un grand nombre d’Allemands ont perdu la vie, pas seulement des Juifs et des étrangers piégés dans des camps de déportation lors d’un bombardement massif des sols allemands.
Je trouve également important d’attirer l’attention sur le fait que l’Allemagne d’Hitler n’était pas une forme de société purement caucasienne, purement native et allemande, où toute autre personne jugée différente était enlevée, enfermée et abattue. Non… bien sûr, Hitler n’était pas un tel idiot, et s’est rendu compte qu’il avait besoin de nombreux travailleurs étrangers pour achever la construction de son pays (routes, bâtiments, etc.) et qu’il avait en effet de nombreux travailleurs d’Europe de l’Est et étrangers sur ses chantiers, il savait aussi que l’économie allemande devrait comme tous les pays adopter le tourisme, et donc les gens de toutes sortes étaient autorisés à visiter l’Allemagne. En effet, Hitler a même accueilli les Jeux Olympiques où des athlètes du monde entier étaient présents. Beaucoup d’historiens modernes qui revisitent la Seconde Guerre mondiale ont tendance à oublier ces détails.

Image: Les Jeux Olympiques de 1936
Hitler voulait en effet se concentrer sur les Allemands, mais il s’est rendu compte qu’il était impossible de diriger un pays sans une part équitable de la population étrangère qui étaient fondamentaux. Et cela se reflète aujourd’hui dans l’exemple de l’amour absolu des Européens de l’Ouest pour la cuisine étrangère, par exemple la cuisine chinoise ou la cuisine indienne qu’ils aiment avoir à portée de main par simple pression d’un bouton. Et en utilisant ces exemples pour expliquer la logique, il serait impossible de fournir des aliments asiatiques de qualité au marché européen sans la présence de certaines personnes de ces régions pour gérer la distribution et assurer la qualité des aliments. Cela s’étend à la cuisine italienne, mexicaine, grecque et/ou française. Un autre exemple serait les bienfaits scientifiquement prouvés du yoga en tant que discipline de santé, qui a été adopté par la société française et de nombreuses autres sociétés occidentales, de même, il serait impossible de s’attendre à la généralisation du style de vie si nous n’avions pas certains des fondateurs du yoga pour former une génération, et logiuement les experts devraient être d’où vient la discipline, qui est en Inde, ce qui conduirait à la formation d’autres experts dans d’autres parties du monde, une logique qui s’applique également pour les disciplines telles que les arts martiaux, également originaires du continent asiatique.
Le fait est que l’Europe de l’Ouest n’est pas une région comme les autres, parce qu’elle est le lieu de naissance de certains des plus grands intellectuels, penseurs et inventeurs qui ont eu un impact majeur sur le monde, ce qui a également conduit à la création des meilleures institutions éducatives dans divers domaines en Europe. Cela attire certains des meilleurs universitaires du monde entier qui paient d’énormes frais de scolarité pour étudier dans ces établissements, ce qui stimule également l’économie de l’Europe et lorsque cela se produit, cela signifie que le gouvernement a plus d’argent à dépenser pour sa propre population, son système et ses infrastructures. Lorsque ces meilleurs universitaires étrangers terminent leurs études, une grande partie d’entre eux retournent dans leur pays d’origine, mais certains sont également employés en tant que spécialistes hautement qualifiés et travailleurs qualifiés dans leur domaine par des géants du monde européen des affaires dans des domaines allant de l’ingénierie à la médecine. Il est également important de comprendre que la contribution de ces personnes aide au progrès des institutions européennes et à leur réputation. Ainsi, ces travailleurs qualifiés, bien qu’ils ne fassent pas partie de la sphère culturelle ou de l’industrie du spectacle ou de l’industrie hollywoodienne majoritairement juive, font parfois partie de l’équipe qui trouve une nouvelle invention, un nouveau moteur, une façon plus propre de récolter l’énergie, une nouvelle cure, un nouveau traitement, et où le monde est en train de se diriger dangereusement en ce moment en avec la perte de utilité des antibiotiques, qui sait si l’un d’entre eux trouvera l’antibiotique ultime, et si c’est le cas, cela permettra de sauver tant de producteurs, compositeurs, méso-sopranos, pianistes, danseurs de ballet et peintres, ainsi que leurs proches et enfants, de mourir de petites infections comme Frédéric Chopin. Il est donc important de noter que certaines choses sont plus grandes que la beauté extérieure, mais ont plus à voir avec la beauté intérieure de l’esprit qui se reflète dans l’intelligence et les capacités académiques. D’ailleurs en répondant à vos questions, et en révisant ces écrits durant la période du confinement en Mars 2020 face à la crise mondiale du Coranavirus (COVID-19) qui a déjà fait des milliers de victimes dans le monde, j’ai encore une fois par « coïncidence », un phénomène spirituel qui est devenu très normale dans ma vie et que ceux qui nous suivent et nous lisent auront aussi remarqué que j’ai appris à vivre avec ces coïncidences et ces similitudes sans fin en interrogeant les étoiles et Dieu, retrouvé mes pensées dans les mots de Didier Raoult dans une de ses présentations faites en 2015 [voir la vidéo ci-dessous].
« Le processus de l’innovation peut-il respecter la règle ? » -Pr Didier Raoult, 2015
L’autre scénario est que, dans de nombreux cas, ces travailleurs qualifiés ayant passé une grande partie de leur vie dans la civilisation occidentale finissent par se marier avec une femme du pays où ils travaillent, par exemple, des médecins étrangers qualifiés qui épousent leur infirmière et lui offrent une vie dont elle n’a jamais rêvé. Donc, ce sont des choses qui se produisent dans le monde humain, et ces mélanges mineurs de gènes se sont toujours produits depuis le début de l’humanité, comme je l’ai expliqué à maintes reprises que notre race actuelle est le résultat du mouvement à travers les plaines de la terre, le croisement et l’évolution. Donc, essayer d’arrêter une telle force qui a façonné notre espèce, semble être une lutte contre la nature elle-même, donc cela semble contre nature. La seule chose que l’on puisse faire est de guider les gens vers une meilleure compréhension de leur propre société, de son peuple et de son identité, ainsi que de sa continuité et des efforts que cela exige de tous ses citoyens – sinon tout système s’écroule et se désintègre – et ceux qui font partie d’une société devraient savoir que s’ils ne s’assimilent pas et ne font pas partie de ce peuple, ils auront toujours une vie mondaine et incomplète, qui pourrait être comparable à celle d’un rat. Dans certains cas, des cas mineurs de fusion génétique ajoutent également des gènes très talentueux au patrimoine génétique d’une civilisation, car l’excellence peut provenir de n’importe quelle composition organique et, lorsqu’elle fait partie d’une civilisation, ne fait que la renforcer, car elle se propage dans la civilisation à travers le temps. La chose décente à faire serait que l’État contrôle toujours le nombre d’étrangers dans le pays en imposant une limite stricte par rapport à la population native, peut-être s’entendre sur un pourcentage qui ne devrait jamais être dépassé, en excluant les étudiants universitaires.
Par conséquent, le régime hitlérien aurait dû savoir qu’il n’allait qu’échouer et créer beaucoup de ressentiment et de haine en essayant de séparer les êtres humains légalement par des formalités rigides et des preuves d’identité génétique par des idées obsolètes telles que la généalogie allemande, comme le faisait le régime national socialiste. En effet, la société avait déjà évolué et de nombreux liens s’étaient tissés entre les personnes qui se sont mariées et ont eu des enfants, entre les différentes confessions religieuses, origines et nationalités de la nation allemande. Et ces types de règles rigides qui expulseraient ceux qui ne s’y conforment pas par le biais de la généalogie et de l’ascendance ne pourraient que conduire à la séparation des familles et même à la déportation des femmes ou des maris de nombreux Allemands, et lorsque ces scénarios se produisent, les humains ont tendance à lutter à mort pour sauver ceux qui leur sont chers. Le régime hitlérien aurait dû savoir que ce genre de politique était vouée à l’échec.
Ce qui, selon moi, aurait plutôt fonctionné, c’est une exécution “informelle” de la vision d’une Allemagne forte. En d’autres termes, Hitler aurait dû créer une société centrée sur les citoyens allemands – à la fois les natifs et ceux qui se sont fermement assimilés et qui se considéraient comme des Allemands de souche – avec une forte identité allemande et un sentiment d’intérêt pour le peuple et la nation, tout en nationalisant les industries et en s’assurant que les gens au sommet se consacrent entièrement sans autre motif que le progrès de la nation et ont les valeurs nationales, la dignité humaine et comprennent l’identité religieuse de la nation en favorisant des personnes aux sentiments allemands forts et reconnus. Après cela, le régime et la nation auraient automatiquement créé un climat qui illustrerait la vision d’une Allemagne nationaliste forte, avec des industries axées sur le peuple allemand, et sans une politique formelle de déportation et de dépistage génétique, le peuple se serait rapidement retrouvé dans une société remodelée pour refléter les valeurs d’une Allemagne nationaliste, avec fierté dans son histoire, son peuple, sa culture et ses valeurs sans attaquer systématiquement les autres. Après cela, les entreprises qui ne pouvaient pas s’adapter fermeraient automatiquement et partiraient si les autorités déclaraient catégoriquement qu’aucune tradition juive ne serait tolérée sur le sol allemand et qu’aucune personne de la religion ou de la communauté juive ne serait autorisée à faire des affaires, sauf celles qui ont abandonné leur identité juive et adopté pleinement la tradition allemande avec la religion officielle comme option. Les personnes qui voulaient rester dans l’Allemagne nationale-socialiste évalueraient automatiquement leurs capacités et leurs possibilités et se forceraient à respecter les règles et à embrasser, à se développer et à apprendre à être citoyens allemands ou à partir. Elle aurait automatiquement généré un sentiment de logique d'”adaptation, de périr ou de partir” dans l’esprit de la population allemande, ce qui aurait conduit les peuples assimilés d’Allemagne à se rapprocher et à renforcer leurs liens avec le peuple natif allemand pour faire partie de la grande vision d’une Allemagne nationaliste, ou ils seraient partis à cause de leur incapacité ou refus de s’adapter, participer et contribuer à l’amélioration de la société.
C’est donc ce qu’il aurait fallu faire, selon moi, les idées et la vision du régime national-socialiste auraient dû être appliquées de manière informelle et non formelle par le biais d’un régime militaire strict, de camps de déportation, d’enquêtes généalogiques et de l’affirmation atavique et non scientifique du “sang”. En effet, il n’existe pas de “sang” comme on l’appelle dans la culture, le sang est un liquide qui coule dans les veines des êtres humains, mais même la famille n’a parfois pas de sang compatible car ils diffèrent par groupe et ont parfois besoin d’étrangers ou des individus d’une société différente pour donner du sang pour sauver la vie des autres qui ne sont pas liés à eux. Ainsi, cette idée de “sang” devrait être utilisée avec soin et convient mieux aux métaphores de “culture et littérature” que la réalité, puisqu’elle semble être utilisée pour expliquer la loyauté, l’unité et la parenté à travers une nation, une société, des valeurs et des perspectives similaires. Avec cet exemple, je peux dire aujourd’hui que j’ai du sang franco-britannique dans les veines et que cela fonctionnerait culturellement, mais médicalement cela n’aurait pas beaucoup de sens, puisque mon sang ne sera compatible qu’avec des individus de mon groupe sanguin qui peuvent être de n’importe quelle partie du monde et de n’importe quelle composition organique ou société, tant qu’ils sont humains et non des animaux.
La dernière chose que je mets aussi en doute dans la situation du régime hitlérien, c’est le véritable pouvoir de la démocratie à notre époque, oui ! Je veux dire, le peuple allemand avait voté pour l’arrivée au pouvoir des national-socialistes après avoir clairement connu leur manifeste et leurs idées d’une Allemagne nationaliste sans présence juive. Par conséquent, je me demande si demain, si je fais campagne et si je dis par exemple – notez que ce n’est qu’un exemple, et non une déclaration d’intention – que je rendrai illégal dans le pays toute forme de lieux de culte islamique, car nous savons par les faits historiques que c’est une religion qui a mené d’énormes guerres violentes contre la civilisation classique occidentale et toutes les autres religions non musulmanes et qui est une secte de guerre, de sang, de conquête et de domination par tous les moyens ; et si je suis élu, je serai bombardé par les alliés et emprisonné pour avoir essayé de le faire ! Cela signifie que même si une forme de référendum démocratique soutenait mes idées, toutes les autres conventions m’en empêcheraient, ce qui semble indiquer que les pays ont perdu leur pouvoir démocratique et ne peuvent plus satisfaire leur propre population, ce qui devrait laisser aux autorités beaucoup à réfléchir.
L’autre question de l’assimilation culturelle, qui consiste à faire partie intégrante de la nation, exige que l’on adopte le thème culturel de la nation, et cela s’applique aux individus et à leurs noms. Ce que je veux dire, c’est que l’assimilation implique généralement de porter un nom en accord avec l’héritage de la société, et beaucoup de Juifs l’ont compris, malheureusement le reste ne semble toujours pas comprendre qu’avec un nom comme “Mangia Fazula”, “Okolo Sambaweh”, “Munjabar Sakalamaktoum”, “Soupovic Boringov”, “Adnan Sawey” ou “Aharon Azriel” ils seront automatiquement considérés comme étrangers dans un pays d’Europe de l’Ouest fondée sur la culture chrétienne occidentale. Ainsi, les personnes qui veulent faire partie intégrante d’une nation par le biais de l’assimilation devraient aussi être assez intelligentes pour comprendre le thème culturel qui s’applique aussi aux noms, ainsi que la combinaison de la condition physique qui facilite simplement le processus et une maîtrise des modèles de communication et de comportement et un fort sentiment de solidarité avec la nation, tout en acceptant également l’identité religieuse de la nation même si cela est facultatif – étant une question de connexion spirituelle et le caractère sacré de son âme et c’est une question entre la personne et sa conscience et “Dieu” si elle croit en lui.
Quant à la rhétorique catholique forte encouragée par Hitler et son régime en faveur de l’éducation des jeunes à la religion et aux valeurs, il est important de se rappeler que Jésus Christ, le Messie qui a conduit à la fondation et à la diffusion du christianisme, n’est pas né d’origine européenne ni ne parlait français, allemand ou anglais. Jésus-Christ est né de la population d’Israël et parle en araméen. Bien sûr, il n’était pas de foi juive, et les textes religieux et l’héritage du christianisme ont été traduits dans les langues occidentales pour atteindre un large public. Par conséquent, cela aurait aussi pu être fait pour n’importe quelle autre religion si c’était celle qui avait été adoptée et répandue en Europe, par exemple l’hindouisme. Si tel était le cas, tous les textes hindous et les hindous d’Europe parleraient et prieraient dans leurs propres langues européennes, pas nécessairement dans la langue maternelle des dieux, c’est-à-dire l’hindi, puisque tous les textes religieux auraient été traduits dans les langues respectives de la région européenne. De même, les chrétiens modernes d’Europe occidentale ne parlent pas l’araméen, la langue que Jésus parlait.
Le fait est que, comme l’explique la théorie organique, les modèles de communication des primates humains peuvent varier d’une région à l’autre, mais la créativité et le QI ne varient pas, et par conséquent, une fois que l’héritage de l’humanité est traduit dans le langage approprié [modèle de communication], la société devrait être immédiatement soulagée dans sa capacité à se comprendre mutuellement.

La synchronisation linguistique devrait donc être une chose qui apaiserait un monde en désaccord, même si les valeurs et les croyances religieuses sépareront toujours les groupes, de sorte que le débat aujourd’hui vers une civilisation harmonieuse devrait certainement commencer sur le langage global de l’humanité à adopter. Un bon exemple serait de voir le succès commercial et l’influence créative de la forme d’art moderne connue sous le nom de “manga” – qui vient d’Asie – sur la France et les autres sociétés d’Europe de l’Ouest une fois qu’elles sont doublées dans la bonne langue. Par exemple, un des grands classiques de la littérature française, le roman écrit en 1844 par Alexandre Dumas, « Le compte de Monte Cristo », un titre qui a fait l’objet de nombreuses reprises cinématographiques, télévisuelles, musicales et animées a aussi reçu une interpretation graphique en manga.

« Le Comte de Monte-Cristo » d’Alexandre Dumas interprété graphiquement par le mangaka Ena Moriyama (2017) / Image: Kurokawa
Et maintenant, après avoir parlé de la Théorie Organique ci-dessus, j’aimerais expliquer son application à une civilisation humaine moderne ainsi qu’à l’évolution et à l’assimilation organiques individuelles, afin que la plupart des non-académiques et des non-initiés qui lisent ceci puissent avoir une vision claire de ce qu’est l’assimilation d’un point de vue objectif et rationnel et aussi de ce que cela implique et exige pour un organisme de considérer si elle a le potentiel et les exigences pour être assimilée dans une société particulière, et comment cela renforce une société sophistiquée, et ici, comment cela aurait aidé dans la politique d’Hitler à créer une Allemagne moderne ou la vision de n’importe quel dirigeant à créer un pays moderne.
En parlant d’évolution, il faut tenir compte de l’évolution et de la condition physique de chacun, car toutes les formes d’Homo Sapiens évoluent ensemble sur cette minuscule planète qu’est la Terre d’une manière si rapide que les manuels scolaires ne peuvent espérer l’expliquer et l’égaler, d’où l’importance des ressources et la créativité de penseurs d’avant-garde dotés d’une intelligence fluide.
Tout d’abord, je voudrais aborder la question de l’assimilation d’un point de vue organique et, étant donné que je suis un parfait exemple de l’école de pensée française avec un côté britannique fort, je vais expliquer ce processus en m’en servant moi-même comme exemple. Maintenant, j’ai hérité des connaissances, de la langue, des valeurs et des philosophies de l’empire français et de l’empire britannique par la transmission culturelle après que ces empires aient conquis des terres et étendu leur royaume. Je ne me suis donc pas réveillé un matin, parlant soudainement français et anglais tout en connaissant l’histoire et la littérature de ces langues. Et si l’île minuscule que je suis née était située près de l’Europe occidentale, elle ferait partie de l’Europe, je n’aurais probablement pas à répondre à toutes ces questions, car elle aurait été considérée comme un produit de la civilisation européenne, à la simple différence que certaines des personnes qui constituent sa nation viennent avec une variété de tons de peau dont beaucoup ont une couleur et une texture très différentes de la majorité commune du rose clair à cause d’un mélange qui a été fait pendant la conquête occidentale européenne. Pourtant, cela n’aurait pas été un tel problème parce qu’il y a beaucoup de pays d’Europe où les gens ne sont pas aussi pâles que la majorité commune, par exemple l’Espagne, le Portugal, l’Italie et la Grèce – c’est simplement une légère similitude dans les attributs physiques, pas la langue, ou autre chose, donc il ne serait d’aucun sens de placer ces nations dans un groupe ! Mais, comme le lieu de ma naissance est un lieu éloigné de l’Europe géographiquement bien que né sur le patrimoine de l’Europe de l’Ouest, et que j’ai voyagé pour rejoindre les racines de mon héritage culturel en Europe occidentale puisque je fais partie des élites littéraires de la nouvelle génération née dans une république indépendante avec un nouveau système culturel et éducatif, une langue et des valeurs française, je pense être un bon exemple pour expliquer le processus de l’assimilation dans une perspective individuelle, en m’aidant de ma propre Théorie organique.
Maintenant que j’ai expliqué que l’organisme individuel né sur la planète terre selon les lois de la nature et de l’évolution est libre et évolue encore puisque l’évolution est un processus sans fin. J’attirerai également l’attention du public sur le fait que, selon les lois de la nature, les barrières érigées par l’homme ne font pas partie des lois naturelles, ce sont simplement des barrières érigées par les groupes politiques. Ainsi, l’organisme individuel naît sur une planète et peut s’adapter et changer en fonction de ses capacités et de son choix d’environnement. Grâce aux progrès d’aujourd’hui grâce à la technologie et à ses installations d’apprentissage accéléré, les organismes peuvent apprendre et se façonner linguistiquement et philosophiquement en fonction de l’environnement dont ils veulent faire partie. Cependant, il y a aussi des limites à ce processus, car un haut niveau de compétence en termes de modèles comportementaux et de communication sera nécessaire pour qu’un organisme s’assimile parfaitement à un environnement choisi et soit vu comme une partie intégrante de celui-ci tout en étant synchronisé avec les natifs. Par exemple, j’avais hérité des modèles communicatifs, comportementaux et sociaux de la France et de l’Angleterre, qui étaient enracinés en moi et j’ai également fait des choix pour approfondir ma compréhension de ces sociétés à travers mes choix éducatifs et, dès mon plus jeune âge, j’ai toujours voulu poursuivre ma carrière et terminer ma vie en Europe de l’Ouest : France et Angleterre. Cela signifie que j’ai investi beaucoup d’efforts pour me redéfinir en tant que Franco-Britannique d’Europe occidentale parce que rien n’arrive à personne sans sacrifice, travail et dévouement.
Il s’agit maintenant d’expliquer que pour qu’un organisme sur terre puisse envisager de s’assimiler dans un environnement choisi, ce n’est pas un processus facile, mais il comporte d’immenses défis et sacrifices. Si nous voulons faire partie d’une nouvelle société, nous ne pourrons pas le faire en restant ce que nous sommes, mais nous devrons nous remodeler et nous ajuster à la société et nous efforcer de ne faire qu’un avec son peuple, et d’une certaine façon les voir comme notre propre “sang” – métaphoriquement. En outre, il y a aussi la question de la condition physique, qui n’a rien à voir avec la “beauté”, mais plutôt avec la capacité de se fondre dans les organismes de cette société par une certaine forme de synchronisation physique. Ce n’est qu’une partie et non le seul facteur qui définit l’assimilation, mais c’est un facteur qui facilite le processus d’assimilation, bien que ce ne soit pas tout. Par exemple, en utilisant l’organisme que je suis, je suis né avec un héritage indo-européen et bien que je sois peut-être un peu moins pâle que la majorité moyenne des organismes de la sphère occidentale européenne, j’ai encore plus de similitudes physiques avec ces gens puisqu’ils sont aussi d’origine indo-européenne et de ce qui est aussi connu comme la “race aryen”. Ce que j’essaie de dire, c’est que j’ai choisi une société où l’assimilation était réalisable parce qu’il y avait des liens forts dans mon propre patrimoine génétique, linguistique et culturel avec ces pays : Je parlais la langue, lisais la littérature, connaissais l’histoire, chantais, jouais et écoutais la musique, partageais la même religion et étudiais et comprenais la philosophie de ses plus grands esprits. Cela signifie donc que l’organisme que je suis a eu toutes les chances de s’assimiler dans la sphère de l’Europe de l’Ouest, en France comme en Angleterre.
Cela n’aurait peut-être pas été aussi facile si, par exemple, j’avais décidé de m’assimiler dans la civilisation négrière de l’Afrique parce que pour commencer, la forme physique entre l’organisme que je suis et le peuple négrier est incroyablement loin l’un de l’autre ; mais encore plus, je n’ai aucun lien avec la culture, les langues, l’histoire ou la philosophie négrière. Cela ne veut pas dire que ce serait impossible, mais cela aurait été très difficile en raison des différences de civilisation et de mode de vie.
Puisqu’il s’agit du sujet des nègres, si dans les années 1950 une personne avait déclaré que les nègres sont une race et un patrimoine inférieurs, les gens autour d’elle auraient pu dire que l’homme est partial et raciste. Cela ne signifie pas pour autant que tous les nègres sont inadéquats ou non qualifiés, bien sûr, nous avons de grands nègres qui excellent dans la plupart des disciplines physiques comme le sport et quelques autres qui sont devenus des professeurs dans des domaines spécifiques. Mais ce qu’il est généralement sous-entendu par l’affirmation que “les nègres sont une race inférieure” semble suggérer qu’en moyenne, c’est-à-dire que si nous prenons tous les nègres et faisons la moyenne de leurs réalisations et les comparons à toutes les autres civilisations, nous arriverons au fait qu’ils sont en retard sur tout, d’où le terme “inférieur”. Aujourd’hui, si nous regardons toutes les statistiques mondiales concernant les nègres, nous verrons qu’ils sont en effet derrière toutes les autres civilisations. Pourtant, chaque fois que ce sujet revient sur le tapis, nous voyons soudain tous les médias à majorité juive, jetant soudain tous les nègres singuliers des États-Unis qui ont fait de l’argent ; nous voyons des joueurs de basket-ball, des rappeurs avec des diamants dans la bouche, et tous les autres nègres qui ont réussi financièrement grâce aux industries des médias à capitaux juifs des États-Unis. Ce n’est donc pas encore une fois la question, car je ne dis pas que tous les nègres sont inférieurs, mais simplement que la civilisation négrière est en moyenne inférieure à toutes les autres civilisations de la planète Terre. Et comme si cela ne suffisait pas, ils sont aussi physiquement incroyablement uniques en termes de caractéristiques et de traits par rapport à toutes les autres civilisations de la Terre, ce qui en fait une énigme en matière d’assimilation dans toutes les cultures. Donc, pour moi, les nègres devraient en tenir compte et avec le monde développé dans lequel nous vivons maintenant et avec la technologie qui rend le monde beaucoup plus connecté et qui rend la vie assez semblable sur n’importe quelle partie de la Terre, je crois fermement qu’ils devraient commencer à s’unir et s’organiser pour combler le fossé avec le reste du monde et envisager le développement du continent africain où ils pourraient tous trouver assez de place pour vivre.
S’installer en Afrique: les clés pour réussir ses projets sur le continent

Dons de charité par pays / Source: GDTB
Le monde a été très charitable envers les causes négrières, mais il est temps pour eux de commencer à s’aider eux-mêmes. L’autre point avec les nègres, c’est qu’eux aussi sont assez semblables aux Juifs lorsqu’ils déménagent dans d’autres sociétés, parce qu’ils se concentrent généralement sur les questions négrières et les nègres, et ainsi forment un groupe de personnes qui cherchent davantage à accroître leur nombre dans un pays qui n’est pas le leur, et ne se concentrent pas sur les questions nationales et les peuples natifs, ce qui ne constitue pas une assimilation, et ce n’est pas une solution avantageuse pour un système. Donc, encore une fois du point de vue de la théorie organique, cela ne fait que générer et créer des organismes plus problématiques qui ne font pas partie d’un système et qui ont des problèmes d’assimilation en raison d’énormes différences dans la composition organique, les modèles comportementaux, les objectifs et les perspectives et ne fait que ralentir et affaiblir tout système.
Reportage: Paris-Jerusalem, Alya.
En 2021, il semble juste d’expliquer ce qu’est la véritable assimilation, et aussi avec le monde plus développé, plus égal et plus connecté, de guider ceux qui ne peuvent ou ne veulent pas s’assimiler en leur expliquant comment des organismes partageant des compositions organiques, valeurs, culture, vision et histoire similaires ont tous les facteurs pour créer des sociétés harmonieuses en étant ensemble. Les nègres et les juifs devraient tous les deux y réfléchir, et peut-être méditer sur la question de savoir s’ils seraient plus heureux dans une société composée de leur propre espèce, ce qui pourrait générer moins de tensions et un sentiment d’être à l’aise dans une atmosphère noire ou juive reflétant leurs croyances et rituels. Parce que la civilisation occidentale est loin d’être parfaite et elle a aussi ses propres problèmes à résoudre, son propre peuple et ses propres questions de gestion à cibler, et si la nation a une foule qui n’est pas déterminée à y contribuer, elle ne fait qu’aggraver ces problèmes.
Reportage: La vie dans la rue
Nous voyons parfois des gens de la foule occidentale se comparer aux membres des foules du tiers monde et des tribus étrangères pour générer un faux sentiment de supériorité. Je voudrais rappeler aux gens que cela n’améliore en rien leur vie. La société occidentale a beaucoup de problèmes qui sont profondément enracinés et qui ne peuvent pas être perçus à l’œil nu depuis la surface, puisque c’est une société qui semble amoureuse de tout emballer proprement, mais étant un intellectuel qui a étudié la psychologie, je peux dire avec confiance qu’il y a d’immenses problèmes en Occident concernant la culture de l’esprit pour le bien de nos vies. Beaucoup de gens sont malades dans leur esprit et ne s’en rendent pas compte et il reste énormément de travail à faire pour fixer les mentalités et inculquer des valeurs pour une société harmonieuse et saine.
Documentaire: Le désastre de l’aIcool chez les jeunes ! [Cliquez pour regarder]
Un regard inédit sur le monde de la toxicomanie
Les personnes qui ne s’assimilent pas n’ont généralement pas ces questions à cœur et ont tendance à se garer en Europe occidentale pour un revenu tout en restant étrangères dans leur identité. Ces gens devraient comprendre que s’ils ne s’assimilent pas, ils ne devraient pas s’attendre à être traités comme les organismes natifs qui font partie intégrante du système parce que le système dépend de ses organismes pour sa continuité et son existence, et cela arrivera aussi à leurs enfants s’ils sont élevés selon des croyances, une identité et des valeurs étrangères qui sont incompatibles avec la nation où ils vivent.
Les gens qui sont en Occident en tant que travailleurs hautement qualifiés et qui ne veulent pas s’assimiler devraient clairement se qualifier d’organismes temporaires qui n’ont pas l’intention de rester pour toujours et d’accepter la vie d’un étranger et le fardeau qui l’accompagne, car je ne dis pas que les natifs sont parfaits ou que tous sont supérieurs puisque nous avons des classes et différents niveaux de scolarité dans toutes les sociétés, mais ce que je répète, c’est que les problèmes de l’Occident ont besoin de la contribution et des préoccupations de sa population pour être résolus et que ceux qui n’y contribuent pas ne contribuent pas à améliorer leur vie et celle du pays, qu’ils soient natifs ou non-natifs. Ce n’est bien sûr pas un problème pour les touristes qui ne visitent que pour des photos et retournent dans leur pays après le voyage – sans problèmes.
Chine, chez les Maoïstes – Cinquante ans après la Révolution culturelle en Chine
Maintenant que j’ai parlé de l’exemple de moi essayant de m’assimiler dans la civilisation noire, une situation similaire se présenterait si, par exemple, je décidais de m’assimiler dans la sphère orientale asiatique, car les différences tant physiques que culturelles sont immenses et, bien que pas impossible, je me heurterais à d’énormes obstacles avec de telles différences qui rendraient ma tâche difficile pour être considéré comme membre de leur société en accord avec leurs propres natifs – et il est inutile de discuter des autres obstacles avec des énormes différences de choix alimentaire, de comportement, de communication et de style de vie.
Documentaire: Inde: Auroville, le Lien d’Or
Comme troisième exemple, une situation similaire se produirait si je décidais de m’assimiler en Inde, parce que bien qu’ils puissent être liés au peuple indo-européen, ils sont clairement une civilisation distincte qui s’est divisée et a acquis ses propres modèles de communication et de comportement, que je ne connais pas un seul mot et ne comprends ni ne gère, pour empirer les choses, je n’ai pas non plus l’air d’un Indien parce que bien évidemment je ne le suis pas, même si certains peuvent partager une teinte de peau olive, et pour finir, ils sont une civilisation principalement hindoue qui se reflète à travers leur culture et leur art, alors que je suis un chrétien profondément enraciné dans l’art de la civilisation française et de l’Europe de l’Ouest.
Le quatrième exemple, c’est celui d’une tentative d’assimilation dans une civilisation musulmane, l’Algérie par exemple. Encore une fois, je ne pourrais pas, parce que je ne parle pas la langue, je ne reflète pas les valeurs, je ne crois pas en l’islam et enfin, ma vision et mon style de vie sont totalement incompatibles avec les cultures du monde musulman, et pour couronner compliquer le tout je ne ressemble pas vraiment aux Algériens non plus.
Par conséquent, si je devais être jeté en Inde, en Asie de l’Est, en Afrique ou dans une société musulmane, regarder dans les yeux de ces organismes serait comme regarder dans les yeux d’un cerf, que je crois être une très bonne métaphore que j’utilise ici pour décrire une créature complètement ignorante, en partie à cause de son innocence, car elle n’a jamais été jetée et n’aura jamais à connaître le drame angoissant et incessant de devoir résoudre les problèmes du monde prétendument moderne de la civilisation occidentale tout en devant constamment endurer l’insécurité et la petitesse de “certains” des plus vils reptiles et cannibales immoraux comme des personnalités publiques vêtues d’un costume que personne n’aurait envie de présenter à ses proches ou d’inviter à dîner une fois qu’ils auront découvert la vérité sur les possibilités illimitées de leur profondeur sauvagement hédoniste et de leur esprit obscur, immoral et pourri.

En fait, en tant qu’élite littéraire, je crois que ce sentiment d’être toujours entouré de cerfs de toutes les couleurs, formes, tailles et origines dans la plupart des endroits de la terre, d’ouest en est, doit être partagé par les autres esprits littéraires, car la plupart des organismes existent simplement, alors que les gens de lettres dans des domaines tels que la psychologie et la philosophie doivent porter le fardeau de penser pour la société et c’est une tâche morale énorme qui vient avec beaucoup de pression et de responsabilité, tout en étant rarement en mesure de communiquer avec les esprits simples que nous rencontrons parfois sur notre route méditative, qui nous laisse seulement l’option soit de sourire, soit de dire quelque chose de doux et anodin, comme de parler du temps.

Traduction [EN]: “Deep-thinking men, in their dealings with other men, always feel like actors, because they are forced, in order to be understood, to simulate a superficiality.” -Nietzsche
Donc, pour en revenir à la question de la synchronisation physique, comme je l’ai répété, la condition physique [qui a à voir avec de légères similitudes et non avec la “beauté” comme on le croit communément] ne fait qu’aider et faciliter le processus d’assimilation mais n’est qu’une indication peu profonde d’appartenance, car la profondeur de l’individu est un point encore plus déterminant, car la véritable valeur de l’organisme est dans le mental, la vision et les valeurs. Pour aller plus loin dans cette logique, je donnerai l’exemple de quelques autres organismes à peau blême de certaines sociétés étrangères qui, malgré leur ton pâle, sont absolument incompatibles avec la société française, ce n’est donc pas parce qu’ils se fondent de manière trompeuse en donnant une impression superficielle d’appartenance à la majorité par une couleur de peau qu’ils sont parfaitement adaptés pour s’y intégrer car ils ne reflètent ni le patrimoine linguistique ni les valeurs, ni les principes fondamentaux des libertés individuelles, la pensée chrétienne qui, même sans être religieux, ont marqué la civilisation et le caractère humain et récepteur de la France.
Sibérie: Les Enfants du Bagne / Tomsk, colonie pour filles, et Mariinsk, camp pour garçons, voici un aperçu de l’univers carcéral en Sibérie où règne le désespoir. Les conditions de vie dans ces bagnes contemporains sont régulièrement dénoncées par les organisations humanitaires. Un témoignage unique.
Un bon exemple serait de considérer les Juifs, les Européens de l’Est, les Russes, les mennonites ou certains segments de la population syrienne qui ont des fois une peau blême. Et puisque nous sommes sur le sujet, je n’ai aussi jamais remarqué “Juif” comme une catégorie séparée empirique dans les formulaires ataviques du monde Anglo-Saxon, pourquoi ?

Image: Des Juifs Haredim
Jérusalem:le pouvoir des ultra orthodoxes
Après tout, les Juifs sont une race distincte, comme ceux qui semblent obsédés par la recherche empirique l’ont découvert – moi ça ne me dérange pas puisque je vois les choses de la perspective évolutionnaire avancée de la « Composition Organique », mais je me pose la question pour les obsédés du laboratoire. Ce que la génétique semble avoir révélé, c’est qu’il existe de puissants marqueurs génétiques de la judéité, de sorte que l’intuition d’Hitler s’est avérée vraie. Ainsi, les juifs ne sont pas nés de conversions en Europe parce que les juifs géographiquement et culturellement éloignés ont encore plus de gènes en commun qu’avec les non-juifs et ces gènes sont d’origine levantine [région où se trouve Israël] ce qui indique un mélange de sociétés caucasiennes de l’est [région entourant la Russie, la Géorgie, l’Azerbaïdjan, l’Arménie, l’Europe de l’Est et l’Asie de l’Ouest], européennes et sémitiques qui semblent compléter le lien manquant de la descendance européenne des juifs. On croit maintenant que les juifs ashkénazes descendent d’une population iranienne hétérogène qui s’est ensuite mélangée à des peuples slaviques orientaux et occidentaux et peut-être même à des Turcs et des Grecs sur le territoire de l’Empire khazar vers le VIIIe siècle après J.-C. Bien que ma perspective sur la race se résume à une simple question de “compositions organiques différentes”, c’est simplement une petite observation pour les scientifiques obsédés par la génétique. Encore une fois, il est important de considérer l’évolution globale de tous les organismes, et aussi de ne jamais oublier qu’un organisme supérieur peut venir de n’importe où sur terre – l’évolution de la race humaine est continue et sans fin.
Je ne dis pas que certaines personnes sont des animaux ou qu’elles devraient être exterminées, alors ne considérez pas mes observations comme discriminatoires, car j’ai déjà expliqué que l’organisme individuel a tous les pouvoirs d’auto-création et d’auto-définition et que du point de vue de l’évolution, les organismes humains de n’importe quelle “composition organique” [race] peuvent procréer avec qui ils veulent, et l’organisme supérieur peut apparaître de n’importe où, mais cette réalité scientifique n’est pas suffisant pour s’assimiler. Ce que je dis, c’est que “s’assimiler” dans une civilisation sophistiquée ne se résume pas à une simple forme physique, il ne s’agit pas simplement d’accepter les “Gros jambons roses” comme le disait Christian Clavier dans la mini-série “Napoléon” de Yves Simoneau en 2002, car on ne cherche pas simplement à créer une société sans structure, dont le seul point fort serait une peau blême et ensuite d’inonder la société de boules de chair roses non civilisées…pour la photo !
TOTALEMENT ISOLÉS : Les Mennonites, communauté coupée du monde
Seule l’industrie hollywoodienne, majoritairement juive, semble voir les choses de cette façon et c’est peut-être parce que les Etats-Unis sont simplement une colonie d’Europe bâtardisée composée principalement de migrants et de juifs de la sphère allemande et anglo-saxonne qui ont tendance à être très pâles pour ne pas dire blême en termes de teint contrairement à beaucoup d’européens.

Ils ont été forcés de trouver un moyen de survivre dans le Far West et ont dû s’unir autour de quelque chose en commun, ce qu’ils ont fait autour du whisky, des armes à feu, du poulet frit, des affaires et de la langue anglaise qu’ils ont également bâtardisé dans leur propre version, tout en restant un groupe industrialisé et mécanique sans aucune structure culturelle – pour la grande majorité bien sûr qui semble avoir une profonde frustration qui se reflète par un mépris des Européens modernes parfaitement assimilés aux sociétés qui forment leur racine.
D’ailleurs en 2021 mes opinions sur la démocratie américaine fondées sur des années de recherches et de preuves empiriques, mais aussi sur des observations fondées sur les valeurs discutables que certains des produits de leurs industries entendent donner au monde, semble presque similaires aux perspectives des grands esprits de la famille intellectuelle française du XIXème et du XXème siècle.
Jacques Derrida sur l’«American Attitude»
Pour Charles Baudelaire (1821 – 1867), le système mis au point en Amérique pour transformer une foule de migrants en un sorte de nation synchronisée artificiellement causait le déracinement des Européens en Amérique. Baudelaire allait trouver ses pensées dans les textes d’Edgar Poe (1809 – 1849), qui était un écrivain moraliste américain qui était lui-même anti-américain et qui peignit un portrait littéraire macabre et sombre sur le thème de la vulgarité américaine. L’Amérique n’est pas libre culturellement et Edgar Poe était pour Baudelaire un des rares cas de rafinnement et de sensibilité au milieu de cette jungle sauvage; l’écrivain américain qui nous permit de percer le mensonge médiatique et cinématographique, le coeur révélateur de l’Amérique – comme le feront certains artistes plus modernes après lui tel que Hunter Thompson et Chuck Palahniuk. C’est une façon de laisser l’Amérique elle-même à travers ses écrivains nous montrer ses côtés sombres et répugnants. Pour Poe, qui avait une acuité de vision incroyable, l’Amérique était l’endroit où étaient réunis les génies mécaniques et les forces animales. Quant à Jules Verne (1828 – 1905), il pensait que les américains étaient des mécaniciens, tout comme les italiens sont des musiciens et les allemands des méta-physicistes. Chez Jules Verne, un des auteurs qui a beaucoup influencé les esprits littéraires de son époque dans leur enfance, l’Amérique a toujours été la nation de la violence et il était particulièrement dégouté par les “Gun Club” qui pour lui était l’image des États-Unis: une nation impérialiste et militaire et un pays d’extrême. Pour Jules Verne l’Amérique était le pays de la brutalité et de la vitesse des moyens de transport. D’ailleurs dans “Le Tour du monde en 80 jours” nous voyons le train utilisé par Verne comme un de ces lieux mobiles où on va rencontrer des échantillons différents de la population humaine sur terre. Paul Claudel (1868 – 1955) avait décrit Chicago comme la ville du sang. Apollinaire avait fait un tour du monde en paroles sur la “machine” qu’est l’Amérique, une terre d’immigrants ou l’européen sauvage est connecté à l’indien sauvage et était particulièrement intéressé par la moralité sexuelle des Mormons de l’état d’Utah qui avaient transformé la polygamie en une activité permit religieusement et faisait des États-Unis un pays avec une sexualité violente. Apollinaire décrivit les gens de Utah comme des Scandinaves en culottes, des Russes en blouse rouge, des anglais étalant leur barbes en collier, avec des Américains, des Juifs, des Allemands, etc. Le continent Américain était vénéré mais aussi repoussé. Guillaume Apollinaire trouvait que Montparnasse à l’époque de la guerre était une projection de l’Amérique à Paris: une juxtaposition des gens du monde entier. Dans ses écrits Apollinaire décrivit aussi la froideur des gens d’Utah ou il comparait les yeux rigides d’un spectateur lors de la pendaison d’un nègre à celui d’un mangeur d’opium. Apollinaire pensait que la démocratie Américaine était insuffisante et aurait toujours besoin de l’Europe malgré leur symbole maçonnique adopté du triangle avec l’oeil qui était supposé tout voir. Pour Apollinaire, à cause de la culture mormone et la polygamie, l’Amérique apparaissait comme le pays des femmes pour les Européens. L’Europe était masculine et l’Amérique féminine [LE rope & LA mérique / jeu de mots], et donc Apollinaire voyait l’Amérique comme une femme qui attendait le conquérant Européen, alors que la France était le pays des hommes debout qui devrait se méfier de la démocratie Américaine. Blaise Cendrars (1887 – 1961) qui était comme Guillaume Appolinaire (1880 – 1918) un grand admirateur de la peinture nouvelle qui était la peinture cubiste de cette époque [les artistes de cette forme, les Delaunay créèrent un mouvement culturel à eux tout seul], qui réunissait des vues différentes d’un même objet, avait lui aussi conclut que New-York avait échoué comme le nouveau Rome parce que le le côté nouveau [new] l’avait emporté sur le côté Romain. L’autre écrivain français André Breton (1896 1966), qui était avant-garde et un grand poète de la ville avait refusé de visiter New York pendant son séjour à l’époque où la France était sous l’occupation allemande, souffrant d’une nostalgie de Paris et avait constaté que les États-Unis étaient devenu beaucoup plus étranger en seulement 5 ans.

Une majorité de 80% des citoyens français se méfient des Etats-Unis et n’approuvent pas leur politique / Source: Le Figaro
Et Jean-Paul Sartre (1905 – 1980) qui comme beaucoup avait un rêve transmit par le cinéma américain allait voir son rêve tourner en cauchemar le moment où il découvrit la vérité sur l’Amérique durant son visite juste après la libération. Sartre comme Breton décrit l’Amérique comme un pays mystérieux qu’on connaissait moins bien qu’auparavant et un pays qui était profondément différent des villes Européennes, qui malgré fascinante, était dangereux et dont il fallait s’en méfier. Pendant la guerre l’Amérique s’était imposé comme la nation la plus puissante militairement, et l’enthousiasme initial des Européens occidentaux de leur arrivée allait vite s’éteindre après la découverte de leur esprits simples et ignorants. Les États-Unis subirent les attaques de Jean-Paul Sartre pour être une société fragmentée, que Sartre décrivit comme ayant plus d’acier et d’aluminium que d’êtres humains: la ville la plus mécanique du monde où l’hiver est beaucoup plus froid et l’été est beaucoup plus chaud. Sartre trouvait que New-York ressemblait beaucoup plus à une ville d’Afrique du nord comme Dakar qu’une cité Européenne. En Amérique, Sartre cherchait et pensait trouver une cité Européenne avec ses sentiments, comme une mère qui voyait les habitants comme ses enfants qui devaient être couvés et gardés, mais ne l’a pas trouvé, puisque pour lui les États-Unis n’ont pas la même tradition historique où la nature Européenne, ce qui s’avéra décevante pour une colonie d’Europe. Sartre trouva New-York terriblement étranger.
Et finalement, une figure qui est presque paternel pour moi, Michel Butor (1926 – 2016), un des grands professeurs de la littérature moderne française visita les États-Unis inspiré par la curiosité des grands écrivains Européens en Amérique constata qu’on pouvait faire de l’argent, qu’on pouvait voir certaines choses intéressantes, mais qu’on ne pouvait pas vivre aux États-Unis, et que l’étrangeté de l’autre côté de l’Atlantique faisait que la plupart des livres semblaient mensongers – les anecdotes de Simone de Beauvoir (1908 – 1986) étaient exactes.

Où perd-on foi dans le capitalisme ? / Source: Statista France
Remarquons ici toute littérature est une oeuvre collective car les mots n’ont pas été inventé par les écrivains puisque la langue est une création collective et crée donc un lien social; les villes aussi sont des créations collective, tout comme le paysage autour de ces villes et les noms des grands hommes et femmes qui marquent les lieux [le génie du lieu], et ce, dans l’espoir que l’esprit de ces hommes marquera les générations futures.
Beaucoup d’Américains semblent également excités de souligner leur longue ascendance européenne perdue, tout en étant déconnectés de celle-ci en termes de valeurs et de philosophie, et ils semblent aussi ignorer l’évolution sociétale des grands empires européens tels que la France. Cette perspective Hollywoodienne peut marcher pour qu’une agence d’escorte, un bar de strip-tease, pour que certains puissent travailler en tant que femmes de loisirs ou répondre aux critères de travailleuses du sexe, mais en dehors de ces entreprises, une société exige davantage de ses citoyens, et ici des organismes avec un sens d’appartenance et de responsabilité ainsi que les comportements et les noms appropriés qui correspondent au domaine thématique pour être en parfaite synchronisation avec les exigences de la société – donc la condition physique ne suffit pas mais facilite simplement le processus d’assimilation, surtout parmi le cerveau courant et non pensant.
En effet, les juifs ont longtemps utilisé cette illusion visuelle pour se fondre parmi ceux qu’ils qualifient de “gentils” ou de “goy” de la sphère européenne, les non-juifs qui, selon leurs écritures, sont des êtres inférieurs nés pour servir les juifs et qui, selon leurs textes religieux, peuvent être traités en animaux et même tués si nécessaire. Il s’agit simplement d’une observation factuelle de ce qui est écrit dans les textes religieux des juifs. Ce sont des écritures qui ont façonné la pensée des sociétés juives depuis l’antiquité, et c’est un fait dont les gens devraient être conscients pour comprendre le train principal de pensée d’un groupe particulier, il est important de connaître les faits des écritures qui les ont façonnées, leurs valeurs et perspectives et pourquoi une grande partie de leurs industries saignent les civilisations et sont desséchées de toute humanité. Cela semble tout à fait contraire au concept de karma que l’on trouve dans l’hindouisme, par exemple, qui croit en la causalité à travers un système où les effets bénéfiques sont dérivés des actions bénéfiques passées et les effets néfastes des actions néfastes passées, créant un système d’actions et de réactions dans la vie réincarnée d’une âme (Atman), formant un cycle de renaissance. La causalité de l’hindouisme s’applique non seulement au monde matériel, mais aussi à ses pensées, ses paroles, ses actions et celles que d’autres font selon nos instructions. Tout au long de l’histoire, les juifs utilisant leur peau pâle pour se répandre et se cacher au sein de la civilisation chrétienne de l’Europe occidentale, ont souvent eu un parcours plus facile, et lorsqu’ils changent de nom pour adopter des noms chrétiens pour leur intégration thématique, il est parfois difficile de les distinguer des peuples natifs de la civilisation occidentale née de la pensée et des arts chrétiens.
Le problème avec les Juifs est que, bien qu’ils se mélangent, agissent, s’habillent et se nomment comme les natifs des nations européennes dans lesquelles ils se déplacent, ils se classent toujours clairement comme Juifs, se concentrent sur l’amélioration des autres Juifs, et travaillent systématiquement ensemble dans les affaires pour promouvoir les intérêts des Juifs, et même ont des conventions mondiales entre Juifs, et présentent avec fierté les réalisations des Juifs. Si nous remarquons que tous les groupes étrangers le font, sauf les chrétiens occidentaux qui semblent préférer s’entretuer et vivre une vie d’hédonisme égoïste.
Pourtant, ce que font ces groupes étrangers n’est pas l’assimilation, mais simplement le mélange et l’intégration pour dominer systématiquement une société ou un système, et les juifs ont été connus pour le faire méthodiquement et habilement dans de nombreux pays européens à travers l’histoire, avec de violents sacrifices religieux à leurs dieux assoiffés de sang, qui impliquent le sacrifice des enfants chrétiens, comme ils ont fait au fil des ans à travers l’histoire européenne avec de nombreux corps d’enfants chrétiens jeunes mutilés trouvés à travers toute l’Europe vidés de leur sang. C’est pourquoi les Juifs sont le seul groupe qui, tout au long de l’histoire de l’humanité, a été persécuté et banni de tant de pays. Oui, beaucoup de gens ne connaissent pas ces faits car la plupart d’entre eux n’ont pas d’autre choix que de prendre leurs informations dans les industries des médias grand public appartenant aux Juifs, alors apprenez quelque chose de nouveau ici !
Documentaire: Dans la tête des SS (2017)
Le régime hitlérien n’a pas été le premier régime à interdire et persécuter les Juifs, les Juifs ont même été bannis d’Angleterre en 1290 par Edouard Ier, et aussi en 1306 de France par Philippe IV et ce ne sont que 3 exemples. Les Juifs ont été interdits dans un grand nombre de sociétés où ils se sont installés en raison de leur insolence, de leur manque de respect pour la nation et les valeurs de leur patrimoine qui ont encouragé la destruction systématique et l’asservissement de toutes les civilisations non-juives, de leur habitude de monopoliser la presse pour déformer la perception et aussi de leurs rituels occultes et violents impliquant le meurtre de jeunes enfants chrétiens pour offrir leur sang à leur Dieu païen violent, Baal dont le terme “Holocauste” est tiré – qui a conduit au sacrifice des personnes dans un Tophet de flammes. En fait, les Juifs ont été interdits dans un grand nombre de pays depuis l’an 1 200 AVANT J.-C. jusqu’en 2014 où ils viennent d’être banni au Guatemala, ce qui conduit à environ 3213 ans de persécutions constantes et d’interdictions dans les pays où ils ont migré. En fait, ils ont été interdits à Carthage, à Rome, en Égypte, en Espagne, en Italie, en Suisse, en Hongrie, en Belgique, en Autriche, aux Pays-Bas, en Pologne, en République tchèque, en Lituanie, dans les États baltes et en Russie, pour ne citer que quelques exemples. Si les gens veulent connaître la liste complète, ils peuvent utiliser Internet et chercher “Pays où les Juifs ont été bannis/expulsés” [aussi voir: Les Résolutions contre Israël].
Voici ce qui, à mon avis, a suscité tant de dégoût et de ressentiment envers les Juifs des nations chrétiennes. Et si quelqu’un avait le temps de lire le Talmud, il comprendrait pourquoi les Juifs ont été persécutés dans tant de pays chrétiens et haïs par le Pape Innocent III lui-même. De même que dans nos langues les chrétiens tirent leur nom du Christ, de même dans la langue du Talmud les chrétiens sont appelés Notsrim, de Jésus le Nazaréen. Mais les chrétiens sont aussi appelés par les noms utilisés dans le Talmud pour désigner tous les non-juifs : Abhodah Zarah, Akum, Obhde Elilim, Minim, Nokhrim, Edom, Amme Haarets, Goim, Apikorosim, Kuthrim.
Hilkhoth X, 2 : Les juifs baptisés doivent être mis à mort.
Les juifs enseignent que, puisque les chrétiens suivent les enseignements de cet homme[Jésus], que les juifs considèrent comme séducteur et idolâtre, et qu’ils l’adorent comme Dieu, il est clair qu’ils méritent le nom d’idolâtres, qui ne diffèrent en rien de ceux parmi lesquels les juifs ont vécu avant la naissance du Christ, et qu’ils ont appris à exterminer par tous les moyens possibles.
Dans le même livre Sanhedrin (107b) nous lisons :
« Mar a dit : Jésus a séduit, corrompu et détruit Israël. »
Le livre Zohar, III, (282), nous dit que Jésus est mort comme une bête et a été enterré dans ce ” tas de terre… où ils jettent les cadavres des chiens et des ânes, et où les fils d’Ésaü[les chrétiens] et d’Ismaël[les Turcs], Jésus et Mahommed, incirconcis et impur comme des chiens morts, sont enterrés. »(25)
Dans Iore Dea (81,7, Hagah) il est dit : ” Un enfant ne doit pas être nourri par un Nokhri, si un Israélite peut être eu ; car le lait du Nokhrith durcit le cœur de l’enfant et construit en lui une nature mauvaise. »
Dans Iore Dea (153,1, Hagah) il est dit : ” Un enfant ne doit pas être donné à l’Akum pour apprendre les bonnes manières, la littérature ou les arts, car ils le conduiront à l’hérésie. »
Dans Zohar (1,25b) il est dit : ” Ceux qui font du bien à l’Akum… ne ressusciteront pas des morts. »
Hilkhoth X, 6 : Nous pouvons aider les goyim dans le besoin, si cela nous évite des problèmes plus tard.
C’est ainsi qu’ils expliquent les paroles du Deutéronome (VII,2)… et tu ne leur montreras aucune pitié[Goim], comme cité dans la Gémarah. Rabbi S. Iarchi explique ce passage de la Bible comme suit : “Ne leur faites pas de compliments, car il est interdit de dire : combien il est bon ce Goi. »
Le rabbin Bechai, expliquant le texte du Deutéronome sur la haine de l’idolâtrie, dit : ” L’Écriture nous apprend à haïr les idoles et à les appeler par des noms ignominieux. Ainsi, si le nom d’une église est Bethgalia – “maison de la magnificence”, elle devrait s’appeler Bethkaria – une maison insignifiante, une porcherie, une latrine. Pour ce mot, karia, désigne un bidonville en bas de l’échelle. »
JÉSUS est ignominieusement appelé Jeschu – ce qui signifie, que son nom et sa mémoire soient effacés. Son nom propre en hébreu est Jeschua, qui signifie Salut.
MARIE, LA MERE DE JESUS, s’appelle Charia-dung, excrément (épave allemande). En hébreu, son nom propre est Miriam.
Les SAINTS CHRÉTIENS, dont le mot hébreu est Kedoschim, sont appelés Kededchim (cinaedos) – hommes féminins (fées). Les femmes saintes s’appellent Kedeschoth, les putes.
Une FILLE CHRETIENNE qui travaille pour les Juifs le jour de leur sabbat s’appelle Schaw-wesschicksel, Sabbath Dirt.
Eben Haezar 44, 8 : Les mariages entre goyim et juifs sont nuls.
Puisque les Goïm servent les Juifs comme des bêtes de somme, ils appartiennent à un Juif avec sa vie et toutes ses facultés : “La vie d’un Goi et tous ses pouvoirs physiques appartiennent à un Juif. “(A. Rohl. Die Polem. p.20)
C’est un axiome des rabbins qu’un juif peut prendre tout ce qui appartient aux chrétiens pour quelque raison que ce soit, même par fraude ; on ne peut pas non plus parler de vol, car il ne fait que prendre ce qui lui appartient.
Dans Babha Bathra (54b), il est dit : ” Tout ce qui concerne le Goim est comme un désert ; la première personne qui l’emporte peut le réclamer pour le sien. »
Dans Babha Kama (113b) il est dit : ” Il est permis de tromper un Goi. »
Le Babha Kama (113b) dit : ” Le nom de Dieu n’est pas profané quand, par exemple, un Juif ment à un Goi en disant : ” J’ai donné quelque chose à ton père, mais il est mort ; tu dois me le rendre ” tant que le Goi ignore que tu mens. »
(4) cf. supra, p.30, Un texte similaire se trouve dans Schabbuoth Hagahoth of Rabbi Ascher (6d) : “Si le magistrat d’une ville oblige les Juifs à jurer qu’ils ne s’échapperont pas de la ville et n’en sortiront rien, ils peuvent jurer faussement en se disant qu’ils ne s’échapperont pas aujourd’hui et qu’ils ne sortiront rien de la ville aujourd’hui. »
Dans Zohar (I, 160a) il est dit : ” Rabbi Jehuda lui dit[Rabbi Chezkia]:’Il faut louer celui qui est capable de se libérer des ennemis d’Israël, et les justes sont beaucoup à louer ceux qui s’en libèrent et combattent contre eux’. Rabbin Chezkia a demandé : “Comment devons-nous les combattre ? Rabbi Jehuda a dit : ” Par de sages conseils, tu leur feras la guerre ” (Proverbes, ch. 24, 6). Par quel genre de guerre ? Le genre de guerre que chaque fils de l’homme doit mener contre ses ennemis, que Jacob a utilisé contre Esaü par tromperie et ruse chaque fois que possible. Il faut les combattre sans cesse, jusqu’à ce que l’ordre soit rétabli. C’est donc avec satisfaction que je dis que nous devons nous libérer d’eux et régner sur eux. »
Dans Choschen Ham. (425,5) il est dit : ” Si vous voyez un hérétique qui ne croit pas en la Torah, tombez dans un puits dans lequel il y a une échelle, dépêchez-vous immédiatement de l’emporter et de lui dire : ” Je dois descendre mon fils d’un toit ; je vais vous ramener immédiatement l’échelle ” ou autre chose. Les Kuthaei, cependant, qui ne sont pas nos ennemis, qui prennent soin des brebis des Israélites, ne doivent pas être tués directement, mais ils ne doivent pas être sauvés de la mort. »
Et dans Iore Dea (158,1) il est dit : ” Les Akum qui ne sont pas nos ennemis ne doivent pas être tués directement, cependant ils ne doivent pas être sauvés du danger de mort. Par exemple, si vous voyez l’un d’eux tomber à la mer, ne le sortez pas à moins qu’il ne vous promette de vous donner de l’argent. »
Enfin, le Talmud ordonne que les chrétiens soient tués sans pitié. Dans l’Abhodah Zarah (26b), il est dit : ” Les hérétiques, les traîtres et les apostats doivent être jetés dans un puits et non sauvés. »
Et dans Choschen Hamm. encore une fois (388,15) il est dit : ” S’il peut être prouvé que quelqu’un a trahi Israël trois fois, ou a donné l’argent des Israélites à l’Akum, un moyen doit être trouvé après une réflexion prudente pour l’effacer de la surface de la terre. »
Même un chrétien qui étudie la loi d’Israël mérite la mort. Dans le Sanhédrin (59a), il est écrit : ” Rabbi Jochananan dit : Un Goi qui prêche dans la Loi est coupable de mort. »
Dans Hilkhoth Akum (X, 2) il est dit : ” Ces choses[supra] sont destinées aux idolâtres. Mais les Israélites[Juifs] aussi, qui abandonnent leur religion et deviennent épicuriens[Chrétiens], doivent être tués, et nous devons les persécuter jusqu’au bout. Car ils affligent Israël et détournent le peuple de Dieu. »
A Choschen Hamm. (425,5) il est dit : “Les juifs qui deviennent épicuriens[chrétiens], qui adorent les étoiles et les planètes et péchent malicieusement ; aussi ceux qui mangent la chair d’animaux blessés, ou qui s’habillent en vain, méritent le nom d’épicuriens ; de même ceux qui renient la Torah et les prophètes d’Israël – la loi veut que tous soient tués ; et ceux qui ont le pouvoir de vie et de mort doivent les faire tuer ; et si cela ne peut être fait, ils doivent être conduits à leur mort par des moyens trompeurs. »
Le rabbin David Kimchi écrit dans Obadiam : ” Ce que les prophètes ont prédit sur la destruction d’Édom dans les derniers jours était destiné à Rome, comme l’explique Ésaïe (ch. 34,1) : Approchez, nations, pour entendre … Car quand Rome sera détruite, Israël sera racheté. »
UN JUIF QUI TUE UN CHRISTIEN NE COMMET PÉCHER, MAIS OFFRE UN ACCEPTABLE SACRIFICE À DIEU / En Sépher Ou Israël (177b) il est dit : ” Prenez la vie du Kliphoth et tuez-les, et vous plairez à Dieu comme celui qui lui offre l’encens. »
Et dans Ialkut Simoni (245c. n. 772), il est dit : ” Quiconque verse le sang des impies est aussi agréable à Dieu que celui qui offre un sacrifice à Dieu. »
APRÈS LA DESTRUCTION DU TEMPLE DE JÉRUSALEM, LE SEUL SACRIFICE NÉCESSAIRE EST L’EXTERMINATION DES CHRÉTIENS
Dans Zohar (III, 227b), le Bon Pasteur dit : ” Le seul sacrifice exigé est que nous retirions de nous les impurs. »
Abhodah Zarah 22a : Ne pas s’associer avec les goyim, ils versent du sang.
Rashi Erod.22 30 : Un goy est comme un chien. Les Écritures nous enseignent qu’un chien mérite plus de respect qu’un goy.
Kerithuth 6b p. 78 : Les Juifs sont des humains, pas des goyim, ce sont des animaux.
Dans Kallah (1b, p.18), il est écrit : ” Elle (la mère de la mamzer) lui a dit:’Jure-moi’. Et Rabbi Akibha jura de ses lèvres, mais dans son coeur il invalida son serment. »(4)
Tout Juif est donc tenu de faire tout ce qui est en son pouvoir pour détruire ce royaume impie des Édomites (Rome) qui règne sur le monde entier. Mais comme il n’est pas toujours et partout possible de procéder à cette extermination des chrétiens, le Talmud ordonne qu’ils soient attaqués au moins indirectement, à savoir : en les blessant de toutes les manières possibles, et en réduisant ainsi leur pouvoir, aider à leur destruction finale. Partout où c’est possible, un Juif devrait tuer les chrétiens, et le faire sans pitié. Les Juifs ne doivent pas ménager leurs moyens pour combattre les tyrans qui les détiennent dans cette quatrième captivité afin de se libérer. Ils doivent combattre les chrétiens avec astuce et ne rien faire pour empêcher le mal de leur arriver : leurs malades ne doivent pas être soignés, les femmes chrétiennes en couches ne doivent pas être aidées, ni être sauvées quand elles sont en danger de mort.
Zohar I, 28b : Les goyim sont les enfants du serpent de la Genèse.
Yebamoth 98a : Tous les enfants de goyim sont des animaux
Abhodah Zarah 35b : Toutes les filles de non-croyants sont niddah (sales, impures) depuis leur naissance.
Sanhédrine 52b : L’adultère n’est pas défendu avec la femme d’un goy, parce que Moïse n’a interdit que l’adultère avec “la femme de ton prochain”, et les goy s ne sont pas des prochains.
Abhodah Zarah 4b : Vous pouvez tuer un goy de vos propres mains.
Hilkhoth goy X, 1 : Ne pas faire d’accord avec un goy, ne jamais montrer de pitié à un goy. Vous ne devez pas avoir pitié des goyim parce qu’il dit : “Vous ne les regarderez pas avec pitié”.
Hilkkkkoth X, 1 : ne pas sauver les goyim en danger de mort.
Orach Chaiim 57, 6a : Pas plus de compassion devrait être montré pour les goyim que pour les porcs, quand ils sont malades de l’intestin.
Jalkut Rubeni Gadol 12b : Les âmes des goyim viennent des esprits impurs appelés cochons.
Babha Kama 113a : Les Juifs peuvent mentir et se parjurer eux-mêmes, si c’est pour tromper ou condamner un goy.
Choschen Ham 26, 1 : Un Juif ne devrait pas être poursuivi devant un tribunal goy, par un juge goy, ou par des lois non-juives.
Babha Kama 113a : Les incroyants ne bénéficient pas de la loi et Dieu a rendu leur argent disponible à Israël.
Pesachim 49b : Il est permis de décapiter goyim le jour de l’expiation pour les péchés, même si elle tombe également un jour de sabbat.
Rabbin Eliezer : “Il est permis de couper la tête d’un idiot, un membre des peuples de la Terre (Pranaitis), c’est-à-dire un animal charnel, un chrétien, le jour de l’expiation des péchés et même si ce jour tombe un jour de sabbat”. Ses disciples répondirent : “Rabbi ! Vous devriez plutôt dire “sacrifier” un goy. “Mais il répondit : “En aucun cas ! Car quand un sacrifice est fait, il faut prier pour demander à Dieu de l’accepter, alors qu’il n’est pas nécessaire de prier quand on décapite quelqu’un.”
Sanhédrine 58b : Si un goy frappe un Juif, il doit être tué, parce que c’est comme frapper Dieu.
Chagigah 15b : Un Juif est toujours considéré comme bon, malgré les péchés qu’il peut commettre. C’est toujours sa coquille qui se salit, jamais son propre derrière.
Zohar I, 131a : Les Gentils souillent le monde. Le Juif est un être supérieur
Chullin 91b : Les juifs possèdent la dignité que même un ange n’a pas.
Iore Dea 151, 11 : Il est interdit de donner un cadeau à un goy, il encourage l’amitié.
Orach Chaiim 20, 2 : Les Gentils se déguisent pour tuer les Juifs.
Shabbath 116a (p. 569) : Les Juifs doivent détruire les livres goyim (Nouveau Testament).
Sanhédrin 90a : Ceux qui lisent le Nouveau Testament (chrétiens) n’auront pas de place dans le monde pour venir.
CEUX QUI TUENT LES CHRÉTIENS AURONT UNE HAUTE PLACE DANS LES CIEUX
Dans Zohar (I, 38b, et 39a) il est dit : ” Dans les palais du quatrième ciel se trouvent ceux qui se sont lamentés sur Sion et Jérusalem, et tous ceux qui ont détruit les nations idolâtres… et ceux qui ont tué les gens qui adorent les idoles sont revêtus de vêtements pourpres afin qu’ils soient reconnus et honorés. »
LES JUIFS NE DOIVENT JAMAIS CESSER D’EXTERMINER LES GOIM ; ILS NE DOIVENT JAMAIS LES LAISSER EN PAIX ET NE JAMAIS SE SOUMETTRE À EUX
Dans Hilkhoth Akum (X, 1) il est dit : ” Ne mangez pas avec les idolâtres, et ne leur permettez pas d’adorer leurs idoles, car il est écrit : Ne faites pas d’alliance avec eux, et n’ayez pas pitié d’eux (Deut. ch. 7, 2). Soit vous vous détournez de leurs idoles, soit vous les tuez. »
Ibidem (X,7) : ” Là où les Juifs sont forts, aucun idolâtre ne doit être autorisé à rester… “

Image: Une affiche du Reich Allemand durant l’occupation Allemande en France
Le 25 juin 1940, l’armistice divise la France en deux, livrée au Nord à l’occupation allemande. Paris, ville ouverte, voit sur la Tour Eiffel se dresser le drapeau du Reich.
Les Juifs de France seront la première cible, tant dans la zone occupée où est appliquée la politique raciale du Reich, que dans la zone libre où la Révolution nationale prônée par le maréchal Pétain permet l’instauration d’un antisémitisme d’État. En France, à la veille de la guerre, on dénombre environ 300.000 Juifs, divisés en deux groupes bien distincts :
– 150.000 “Israélites” citoyens français (bourgeois et professions libérales)
– 150.000 “Juifs” étrangers (majoritairement en bas de l’échelle sociale) Ces derniers seront les victimes privilégiées de Vichy.
La communauté juive en France: Si la France est le foyer de la plus grande communauté juive en Europe, de nombreux juifs de France sont tentés de partir, victimes d’actes de vandalisme ou d’agressions antisémites.
Maintenant, nous pouvons nous poser quelques questions simples : “Est-ce que tous ceux qui ont banni les Juifs pourraient être sans raison de le faire ?” et “Est-ce que les gens pourraient simplement se promener et soudainement décider sans raison de haïr les Juifs ?” et aussi “Si cela leur arrive depuis tant d’années, n’est-il pas probable que le problème soit en fait avec les Juifs eux-mêmes ? Je crois qu’il vaut mieux laisser le public répondre à ces questions et y réfléchir seul.
Je voudrais qu’il soit clair que je parle de la mentalité et de la pensée juive dans son ensemble, mais je ne dis pas que chaque Juif est mauvais ou n’a rien à offrir aux sociétés dans lesquelles il vit. Bien sûr, il y a des personnes étonnantes, admirables et aimables qui s’assimilent complètement, et même abandonnent leur identité juive et se convertissent au christianisme, ou deviennent athées. Il y a bien sûr des gens décents d’origine juive qui deviennent des citoyens à part entière de leurs nouvelles sociétés, qui parlent au nom des natifs et se considèrent comme faisant partie de la nation, et cela se voit en France, où certains sont devenus plus français que les natifs et se sont intégrés au cœur de la nation. Il s’agit cependant d’une très petite minorité de juifs qui, après l’avoir fait, considèrent souvent les juifs étrangers comme inadéquats pour la France parce qu’ils se considèrent comme faisant partie du peuple français et comprennent l’identité religieuse du pays qu’est le christianisme. Cependant, la majorité des Juifs ne suivent pas l’exemple des nobles qui s’assimilent, mais ils restent distincts et travaillent pour leurs camarades et organisations juives tout en adoptant leurs valeurs et croyances de circoncision et de supériorité.
Le fait que tous les organismes étrangers doivent comprendre, c’est que pour faire partie de la civilisation de l’Europe occidentale, il faut accepter le fait que le christianisme fait partie de la culture fondatrice, et bien que de nombreuses personnes ne soient pas religieuses, on ne peut ignorer que l’histoire, l’héritage et la littérature ont été fondés par des hommes et des femmes chrétiens, dont certains ne sont pas religieux mais qui étaient indéniablement influencés directement et indirectement par les pensées et l’héritage chrétiens, ce que peuvent refléter les nombreuses allégories et métaphores relatives à la Bible dans les écrits. C’est aussi une immense coïncidence qu’au moment même où je réponds à vos questions que la cathédrale de Notre Dame vient d’être mystérieusement frappée par un incendie le 15 avril 2019, certains y voient peut-être un signe des fondements d’une civilisation en feu – et les coïncidences avec ma vie ne me surprennent plus. Quand le hasard multiplie les coïncidences, ce n’est plus le hasard.
En fait, être pleinement assimilé signifie renoncer à son identité étrangère et adopter l’histoire, la langue, le thème linguistique, la nation et la religion de la nouvelle société comme une option supplémentaire si possible. Les juifs devraient réfléchir à ceci : le fait que l’Europe occidentale est une civilisation chrétienne, tout comme Israël est une société juive et les Etats arabes sont une civilisation musulmane, les gouvernements de ces deux derniers pays considérant la religion comme une question de culture sérieuse sans jamais faire de compromis sur les priorités et les nécessités religieuses par rapport à toute autre religion étrangère. En effet, dans de nombreux États arabes, le crucifix en tant que symbole du christianisme est interdit et illégal, et ils n’y trouvent aucune excuse, parce qu’ils sont de fermes musulmans et que cela fait partie intégrante du tissu de leur gouvernement et de leur culture. Pour compléter cet exemple, il est également ridicule que la Grand-Croix de l’Ordre national de la Légion d’honneur qui est le plus haut ordre français du mérite militaire et civil, établi en 1802 par Napoléon Bonaparte, ait été remise au sultan de Brunei en 1997, un homme qui a récemment institué un nouveau code pénal qui applique aussi strictement que possible la charia – la loi islamique : la mort par lapidation pour punir les homosexuels et l’adultère, l’amputation d’une main ou d’un pied pour les voleurs, la peine de mort pour insulte au prophète. Être juif ou musulman se présentera toujours comme une personne aux valeurs étrangères issues de l’histoire et des valeurs de ces religions les plus incompatibles avec celles de la civilisation européenne de l’ouest.
Lorsque des personnes qui ont la capacité de s’assimiler choisissent de le faire, elles devraient d’abord trouver leur place dans la nouvelle société en fonction de leurs choix, de leurs désirs, de leurs compétences, et de leurs aptitudes [par ex. de synthèse psychosociale et culturelle]. On attendra d’eux des efforts et un désir sincères d’assimilation et cela commence normalement par un nom occidentale de culture chrétienne. Les personnes qui ne s’assimilent pas complètement, qui ne se reconstruisent pas, qui ne se remodèlent pas et qui n’adoptent pas une identité complètement nouvelle doivent toujours se rappeler qu’elles ne sont pas chez elles et ne doivent pas s’attendre à être traitées de la même manière que celles qui le sont – c’est une simple question de bon sens. Ceux qui s’assimilent correctement feront automatiquement partie du peuple natif et partageront une existence avec des opportunités similaires, parce qu’ils sont devenus natifs par leurs efforts et leur décision d’être loyaux et dévoués à leur nouvelle société et à son peuple, en respectant l’héritage fondateur et les sensibilités religieuses, et bien sûr en maîtrisant les modèles comportementaux et de communication. Cela ne veut pas dire qu’après s’être assimilés, ils doivent être soumis et ne peuvent pas faire une observation critique pour aider à développer le pays et à le faire avancer, mais leur allégeance devrait être à la nation et aux peuples natifs parce qu’ils devraient se considérer comme faisant partie de ce peuple. Après tout, l’objectif est de créer des citoyens loyaux qui se sentent concernés par la société, pas des esclaves ! Les natifs aussi devraient apprendre à agir comme des êtres humains et adopter les valeurs de la décence pour comprendre qu’une société fonctionne mieux quand la population est en harmonie et heureuse tout en voyant les citoyens véritablement et convenablement assimilés comme leur propre “sang”.
Ainsi, comme l’explique la théorie organique, un autre facteur est plus fondamental que la condition physique pour l’assimilation, comme nous pouvons le voir en utilisant les Juifs comme exemple pour expliquer que la similarité dans le ton de la peau n’est pratiquement rien, sauf un petit facteur qui aide avec la majorité qui pense rarement. La partie la plus importante et la plus déterminante de l’assimilation concerne la gestion des modèles de comportement et de communication appropriés de la société dont l’organisme veut faire partie intégrante. Pour une assimilation réussie et complète, les organismes doivent aussi intégrer la philosophie, comprendre le cœur du peuple en fonction de son histoire, maîtriser la langue, ne faire qu’un avec la nation, ressentir la joie et la douleur du peuple et aussi être capables d’utiliser le terme “nous” pour se décrire eux-mêmes et les natifs ; en d’autres termes voire le peuple comme leur propre “sang”, et c’est ainsi que cela se passe dans la civilisation la plus complexe, cad. La France, où le peuple est prêt à vous aimer et à vous considérer comme son propre sang si vous manifestez le désir sincère de faire partie de la patrie nationale et la loyauté envers la nation.
L’assimilation n’est malheureusement pas facile à réaliser et c’est pourquoi l’assimilation ne doit pas être confondue avec l’intégration, car l’intégration est simplement l’acquisition d’un passeport pour la légalité ; mais l’assimilation, c’est sculpter son cœur et son âme pour être un avec les gens et faire partie du sang national par loyauté et engagement tout en jouant son rôle de citoyen avec ses devoirs civiques. En effet, dans la Grèce antique, tous les membres de la société qui ne participaient pas aux affaires communes ou qui ne s’impliquaient pas et ne s’intéressaient pas aux questions concernant le fonctionnement du pays et l’harmonie du peuple étaient considérés comme des “parasites”, et cela inclut tous les citoyens – natifs et non-natifs – car toute société a besoin que ses membres travaillent ensemble pour résoudre ses problèmes et suivent la voie sans fin du changement positif pour l’amélioration d’une civilisation.
En France, la plupart des gens comprennent qu’être citoyen est un devoir, et c’est pourquoi, jusqu’à aujourd’hui, ils sont la seule civilisation qui a défendu la fraternité de l’humanité comme individus à traiter avec respect, ils font partie des rares civilisations qui écoutent l’opinion du peuple et font l’éloge d’un empereur à un homme du peuple s’ils estiment que cet homme a la grandeur de ses arguments et le mérite – nous le savons par la légende de Napoléon – et enfin le peuple français est un des plus réceptifs qui est toujours disposé à raisonner avec de nouveaux arguments, quels que soient leurs origines. En fait, la France est la civilisation la moins atavique et la plus sophistiquée du monde moderne, et accomplir une tâche aussi glorieuse sans monarchie est étonnant – cela montre que lorsque les gens se considèrent comme un et se traitent mutuellement avec respect tout en ayant un sens moral et de dignité, ils incarnent un empire ensemble, sans ou avec un empereur – la tête avec une couronne étant simplement une option si nécessaire et jugé assez ingénieux pour guider une civilisation en conquête, mais non une nécessité ! Pour atteindre ce sens de l’harmonie, il faut des organismes qui peuvent trouver un fort sens de la synchronisation en tant que peuple et se considérer comme une nation et ressentir la douleur et la gloire des uns et des autres pour raisonner comme un. Bien sûr, comme n’importe quelle société sur terre, nous trouvons de mauvaises pommes, des hommes d’État corrompus et immoraux et des arguments mesquins, surtout parmi les petites classes, mais dans l’ensemble, c’est une société construite sur des valeurs et des philosophies conçues pour favoriser le développement des êtres humains où tout individu peut atteindre le sommet par son propre désir, ses efforts et son engagement. Ce qui est malheureux, c’est qu’à mesure que le temps passe et que la génération passionnée qui a participé à la fondation de ce nouveau monde meurt, ces valeurs s’estompent parfois dans l’esprit de la nouvelle génération et des médiocres hommes d’État “Fisher Price” qu’elle nous a donnés. Ce sont de grands hommes et femmes au caractère admirable qui ont eu le courage, au cours de l’histoire, de prendre la parole pour rappeler au peuple combien de personnes ont perdu la vie et se sont battus pour la société actuelle et combien il est urgent de poursuivre notre route du progrès humain sur la même direction à prendre.
Résistances, héros de la première heure (2016)
Témoignage du Waffen-SS inculpé pour le massacre d’Oradour-sur-Glane (2014)
Étant moi-même plus français qu’allemand, je dois dire que je crois en la supériorité de la langue, du patrimoine, des valeurs, du peuple et de l’industrie française sur l’Allemagne et tout autre patrimoine. Cela ne signifie pas que je ne respecte pas ou ne reconnais pas l’Allemagne et les autres pays et leurs réalisations, car des personnes compétentes dans des domaines spécifiques peuvent apparaître de n’importe où dans le monde en raison des capacités étonnantes de la technologie biologique qu’est le cerveau humain, un organe sur lequel j’ai fait des recherches et que j’ai étudié pendant des années. L’Allemagne a toujours été l’un des grands rivaux de la France, une rivalité qui a duré des siècles, bien avant Napoléon, étant parmi les autres vastes empires à vocation universelle. Certains universitaires allemands, tels que Kant, Freud, Schopenhauer et Nietzsche ont influencé d’autres dans le monde entier, notamment la philosophie et la psychologie française comme on peut le voir dans la théorie de la vie mentale de Jacques Lacan, tout comme d’autres ont influencé la pensée allemande, par exemple, Schopenhauer qui, après avoir été initié à la philosophie indienne par Friedrich Majer, s’y intéressa beaucoup et médita même sur l’Upanishad, partie des Védas (l’écriture sacrée des hindous) dans ses vieux jours, pour en associer une partie fondamentale à sa théorie sur le monde des représentations ; le concept hindou de “Maya”, qui définit le monde comme une illusion, c.a.d. en fin de compte, les sujets et les objets étaient tous “Maya” (illusion). Schopenhauer a quitté Berlin lorsque la Prusse s’est rebellée contre Napoléon, car il n’a jamais développé de forts sentiments patriotiques allemands, se considérant comme un cosmopolite sans aucune affiliation nationale, et son concept adopté de sujet, d’objet et d’imaginaire (illusion) réapparaît également dans les écrits de Freud, et a été développé plus tard par Jacques Lacan. Les écrits de Schopenhauer ont également éveillé l’intérêt de Nietzsche, dont les écrits ont été initialement falsifiés par sa sœur, Elizabeth, pour les ajuster à sa propre idéologie nationaliste allemande, adoptée par le régime nazi. La véritable philosophie de Nietzsche était explicitement opposée à l’antisémitisme et au nationalisme puisqu’il préconisait une perspective plus globale et individuelle ; heureusement, des éditions révisées ont été publiées après que des universitaires du XXe siècle eurent contesté cette interprétation incorrecte de son œuvre. Par conséquent, certains intellectuels individuels des institutions allemandes ont contribué à la philosophie moderne et à la pensée de l’Europe occidentale ; nous trouvons donc un certain respect et une certaine coopération dans certains domaines universitaires qui profitent à toutes les sociétés et économies, mais nous ne pouvons ignorer le fait qu’il existe également une concurrence dure et intense avec la France et d’autres pays dans toute une série de secteurs, par exemple, les industries scientifiques, médicales, du transport et technologiques.
La France face aux coalitions européennes (presque toute l’Europe) (2013)
Mais du point de vue d’un produit de la France et de son héritage intellectuel et linguistique avec une influence britannique indéniable, je ne me serais jamais plié à la vision d’Hitler d’un empire allemand gouvernant le monde avec toutes les langues progressivement éteintes pour un monde germanophone complet, donc je préférerais voir un monde francophone. L’empire français a aussi la sophistication et la flexibilité d’accueillir tous les patrimoines étrangers[ce qui est digne d’être conservé] sans les détruire ou les brûler, en traduisant simplement le patrimoine étranger pour qu’il fasse désormais partie du répertoire des savoir-faire de l’empire français. Ainsi, la France ne détruit pas le patrimoine des autres cultures, mais absorbe ce qui est digne d’être conservé (ex. gastronomie, technologie, industries, philosophie, arts, autres pratiques bénéfiques, etc), le partage avec la famille francophone et l’intègre à son propre sang dans son évolution constante. Je préférerais donc voir le monde devenir français comme l’empire absorbe et embrasse l’humanité entière comme une mère dans ses bras d’une manière harmonieuse, humaine, sophistiquée et stratégique plutôt qu’allemande.
Pour terminer, après avoir parlé de ce que je pensais ne pas avoir été bien planifié sous le régime hitlérien, et expliqué en profondeur la théorie organique et l’assimilation, voici les choses qui inspirent dans l’histoire d’Hitler, et cela commence avec le grand exemple que le peuple allemand a donné à l’époque en donnant le pouvoir absolu à un individu méritant en montrant au monde qu’un artiste en faillite pouvait devenir le tout premier dans une société moderne. Ce qui signifie que nous avons finalement vu un garçon aux prises avec des difficultés financières qui était le premier de sa classe à l’école primaire et qui n’a pas réussi à démarrer sa carrière artistique après avoir échoué à un examen à l’une des meilleures écoles d’art d’Europe de l’Ouest, l’Académie des beaux-arts de Vienne, puis par ses propres efforts après avoir été sans abri et en lutte pendant la guerre, monter au sommet. Cela démontre une mobilité sociale absolue, mais aussi comment un homme peut être un artiste, un soldat et un homme cultivé par ses propres efforts pour ensuite diriger une civilisation moderne et atteindre le sommet. C’est pour moi un exemple moderne clair de la Théorie Organique sur le processus d’autodéfinition et de développement progressif d’un organisme individuel basé sur ses propres désirs et capacités.
La deuxième facette étonnamment inspirante de l’histoire d’Hitler est la façon dont il a donné au monde un exemple avant-gardiste de la réponse à un environnement harmonieux, en étant un végétarien qui a été le premier à initier des lois de protection animale.
Le troisième côté admirable d’Hitler était son charisme et sa loyauté envers sa société, mais aussi sa modestie et sa confiance envers les gens de tous les milieux, étant la seule personnalité publique de son niveau à se promener librement dans son pays et à rencontrer des gens de tous horizons et de toutes classes sans aucune protection, tout en gagnant leur confiance absolue pour les guider.
Le quatrième côté d’Adolf Hitler était qu’il avait du style dans son goût pour l’architecture de son pays, comme on peut le constater aujourd’hui à travers les plans qu’il a élaborés avec Albert Speer. On peut imaginer ce qu’aurait été l’avenir de l’Allemagne et de Berlin. Ces plans révèlent les bâtiments et les plans d’une ville qui reflétait la grandeur de l’humanité et même les uniformes de son personnel ont été confiés à Hugo Boss – montrant un homme qui vénérait la perfection. Et si nous regardons les uniformes et les costumes du gouvernement national-socialiste, nous devrons peut-être accepter qu’il s’agît de certains des costumes les plus stylés et les plus beaux jamais vus dans l’histoire moderne, peut-être seulement égalés par des couturiers français comme Yves Saint Laurent.
Le cinquième côté étonnant avec Hitler était son amour pour la science et l’évolution et sa passion pour garder une perspective mise à jour de toutes les dernières découvertes. Il serait donc assez partial de supposer qu’Hitler est un homme rigide qui n’a aucun goût pour le changement. Cela se reflète dans son empressement à encourager la recherche afin de reconstruire les installations médicales, technologiques et militaires de l’Allemagne. Cela ajoute aussi à mon opinion qu’Hitler aurait été disposé à écouter les nouvelles découvertes et à changer ses opinions en conséquence s’il avait été conseillé et convaincu par des gens authentiques, avant-gardistes et honnêtes – il aurait dû me consulter. Haha ! Mais bien sûr, l’entourage proche du Führer n’était pas particulièrement composé des esprits les plus éthiques ou les plus sophistiqués où beaucoup se sont révélés déloyaux et maléfiques, ce qui a probablement conduit aux horreurs du régime sans aucun lien avec Hitler lui-même.
La sixième chose admirable à propos d’Hitler, c’est le fait qu’il était un leader qui voyait vraiment les gens comme des organismes qui avaient besoin des mêmes chances de réussir et de s’élever et non comme une foule qui devait être divisée en segments gauche, droite et centre. Hitler considérait tous ses citoyens comme des gens de son système et s’efforçait de synchroniser l’ensemble de la société pour travailler comme une machine singulière. C’est certainement admirable en comparaison avec les personnes corrompues et immorales à la tête de la plupart des systèmes actuels où les critères utilisés pour gouverner les êtres humains sont des facteurs économiques et commerciaux. Diriger une civilisation d’êtres humains sans valeurs, sans philosophie et sans morale est un moyen sûr d’échouer à long terme parce que les êtres humains ne sont pas des objets ou des biens, mais des organismes complexes qui nécessitent un système très sensible pour vivre harmonieusement, et toute personne qui se dit leader et ne comprend pas la psychologie, la philosophie et les éléments qui conduisent à un environnement humain moderne harmonieux se mentent à eux-mêmes et la société.

Il faut aussi se rappeler comment Hitler a même proposé de démanteler l’armée allemande et de détruire toutes les armes si tous les autres pays faisaient de même, ce à quoi ils n’ont jamais répondu. Ainsi, nous comprenons maintenant pourquoi Hitler a même été présenté comme la personne de l’année par le magazine Time, et cela ne pourrait pas être pour transformer les Juifs en viande hachée. Et l’autre question énigmatique est de savoir pourquoi tant d’argent est consacré aujourd’hui à la défense et à l’armée alors qu’il est clair que nous sommes une civilisation solitaire sur une planète solitaire qui devrait chercher à étendre sa portée en commençant une nouvelle civilisation sur une planète de réserve pour obtenir le statut de civilisation spatiale ? Ces partis qui dépensent tant d’argent pour l’équipement et la technologie militaires n’ont-ils que la défense et rien d’autre à l’arrière de leur esprit, peut-être inconscient ? Est-ce simplement pour la décoration ?
La septième chose inspirante à propos d’Hitler, c’est qu’il n’était pas d’origine allemande, mais comme moi, pleinement assimilé dans la société allemande et de gagner aussi le cœur de toute une nation et de s’élever au sommet et finalement devenir plus d’Allemands que les Allemands eux-mêmes, est quelque chose d’assez spectaculaire. Peut-être, une autre chose admirable a été la réponse d’Hitler dans une procédure judiciaire après l’échec de son coup d’État contre pour prendre le pouvoir, où il a répondu après qu’on lui ait demandé s’il était allemand en demandant si cela est prouvé sur un morceau de papier ou dans le cœur d’un homme ; car bien qu’il avait déjà gagné le cœur de la nation, il n’avait toujours pas de passeport allemand. Dans ses premières années en Allemagne, alors qu’il luttait financièrement et qu’il était sans abri, certains Allemands lui ont également dit qu’il ressemblait à un Juif et qu’ils pensaient qu’il en était un, puis de surmonter tout cela pour atteindre le sommet est tout à fait admirable.

Des photos de Henrich Hoffmann, le photographe d’Hitler, numérisés, restaurés et publiés pour la première fois (2019)
Le huitième côté inspirant d’Hitler était sa capacité unique d’ouvrir complètement son cœur à la nation et de prononcer des discours bouleversants qui hypnotisaient les foules, avec son langage corporel passionné qui dépeignait son honnêteté et son dévouement envers les Allemands en les mettant devant son propre confort.
Documentaire: Les Waffen SS, unités d’élites d’Hitler (2013)
Le neuvième et dernier point que je crois inspirant pour Hitler, c’est qu’il ne semble pas avoir vu les choses du point de vue d’un cadre moyen ordinaire, d’un économiste, d’un banquier, d’un médecin ou d’un autre cadre financier qui a tendance à se frayer un chemin dans un parti politique simplement pour apparaître à la télévision ou dans un journal sans aucune présence, vision ou valeurs fortes et voir une civilisation comme une boutique à gérer.

Hitler avait une vision plus profonde comme les empereurs légendaires l’avaient, et voulait guider une nation avec la philosophie, l’architecture inspirante, les œuvres d’art intemporelles et voulait mélanger et synchroniser tous les départements allant des affaires, l’économie, l’éducation, la science, la recherche, l’histoire et les arts pour créer le genre de civilisation éternelle comme il est souvent décrit dans la littérature mythologique qui tient le test du temps en marbre et pierre.
Plus important encore, Hitler semblait être d’avis que si une civilisation n’est pas en expansion, elle ne progresse pas et cela reflétait les qualités d’un conquérant, rappelant celles d’Alexandre le Grand ou encore Napoléon.

Image: Alexandre Le Grand vainqueur du lion de Bazaria, sculpté par Jacques Dieudonné, Jardin des Tuileries, 1er arrondissement, Paris | Source: Les Musées de la Vile de Paris
Aujourd’hui, des cadres pathétiques et médiocres qui dirigent une équipe qu’ils appellent un parti politique sont guidés par le seul désir de rester au pouvoir, et en raison de leur allégeance aux donateurs de leur parti, ils doivent respecter et satisfaire certaines demandes pour rester financés, cela détruit une civilisation car elle n’est pas dirigée avec la liberté et les valeurs qu’elle exige, et donc, cela conduit à une atmosphère mondaine d’une société statique et ennuyeuse où le même genre d’hommes agissent et parlent d’une manière noble en public, mais se comportent comme des personnages ignobles et immoraux dans leur décision et leur gestion – ce cycle est déprimant et répétitif depuis des décennies sans qu’aucun personnage légendaire ne semble se dresser contre une telle absurdité et changer les choses. Aujourd’hui, avec tant de conventions, il n’est guère possible pour un grand empire de prendre les choses en main et d’envisager l’expansion et la conquête à cause de croyances hypocrites d’égalité absolue de toutes les sociétés et langues et de politiques du tiers monde qui ont piégé les grands empires occidentaux comme la France en soumission et à genoux pour se conformer à des règles irrationnelles, les exigences ridicules et hypocrites qui l’ont contraint à respecter les conventions et l’ont progressivement transformée, lui et bien d’autres empires, en pépinières paralysées par les exigences des sociétés inférieures, alors qu’elle a toutes les ressources pour transformer le monde entier en colonies et mieux le gérer tout en donnant à tous les peuples de la Terre le rêve de faire partie de son patrimoine, comme le faisaient autrefois les grands empires.
Il est également juste de noter qu’au cours de la Seconde Guerre mondiale, toutes les parties ont commis des atrocités sur des civils innocents, tant les Alliés que les Allemands, de sorte qu’aujourd’hui, lorsque nous regardons la plus grande guerre des hommes du XXe siècle, nous réalisons qu’aucun parti ne peut proclamer être des anges, car de nombreuses atrocités commises par les Alliés ont été ignorées jusqu’à récemment ; comme le massacre de Katyn commis par Staline, qui a été attribué à tort au Reich allemand, sans parler de l’horrible quantité de viols commis sur des femmes innocentes de tous bords en Allemagne occupée entre 1944 et 1954 [Anglais: 45 000 viols, Français 50 000 viols, Américains 190 000 viols et Soviétiques 430 000 viols]. Il ne faut aussi pas oublier les viols au cours de la libération de la France à la fois pendant et après l’avancée des forces armées des États-Unis à travers la France. Selon l’historien américain Robert Lilly, il y aurait eu 3 500 viols commis par des soldats américains en France entre juin 1944 et la fin de la guerre. Le nombre de viols est difficile à établir car de nombreuses victimes de viol n’ont jamais rapporté les faits auprès de la police. Les troupes américaines engagées ont commis 208 viols et une trentaine de meurtres dans le département de la Manche. Pour le seul mois de juin 1944, en Normandie, 175 soldats américains sont accusés de viol. [Voyez: Viols durant la libération de la France] Du fait du nombre important de cas de viols recensés et de la dégradation de l’image des soldats américains en France, le commandement américain juge entre le 14 juin 1944 et le 19 juin 1945, 68 cas de viol ordinaire concernant 75 victimes; au moins 50 % des soldats-violeurs sont ivres au moment de leur crime; sur les 152 accusés, 139 sont des Noirs, alors qu’ils ne forment que 10 % des troupes sur le théâtre européen [Voyez l’article: À l’automne 1944, Français et troupes américaines au bord de l’affrontement]
Donc, pour conclure avec une réponse à votre question, je ne suis ni un fan d’Hitler, ni un haineux Hitler, mais un homme qui voit “Le Führer” comme l’une des grandes figures du siècle dernier avec des éléments à s’inspirer et des erreurs à apprendre à ne pas commettre aussi. Un mouvement silencieux mais croissant d’Aryens modernes commence à réévaluer les idéologies du Führer avec une exposition récente à Montpellier présentant 200 photographies de son photographe Heinrich Hoffman.
Enfin, j’aimerais souligner que si personne ne parle, rien ne change… alors j’ai choisi de parler, qu’avez-vous choisi de faire ?
—-|—-
[EN] Answer to Question VI. “Are you a Hitler fan?”
I guess this question is being asked to me because I have often linked Hitler videos throughout my essays and writings.
Well, to begin I have never quite understood the term “fan”, because this seems to involve some form of obsession to a particular person. No, I have admired many people’s works and values, and if this qualifies me as being “fan”, then perhaps I am. “Admiration” for “some” aspects of many great men and women’s works throughout history – that makes me an admirer of amazing work with respect for the artist or creator. This extends to Adolf Hitler, whom I would say had many things right in regards to managing a civilisation, but not everything. He, or his advisors did make some mistakes like most humans do, that cost him and his regime everything.
So, I would say, I do admire a lot of Hitler’s philosophies and achievements such as the need to unite the people by ridding the country of the divisions of left, centre and right, while also critical of some of his proceedings, because after all he was a human being who only went by the reality of his era, while I am living in 2021 and today see things from another perspective because I am lucky to have inherited a great amount of knowledge and scientific findings that were not yet available in the times of Hitler. The advancement of technology has today made it possible to be extremely mobile since most of the major works and research are now available in digital form and this has made the world more connected without the absolute need to travel to ancient libraries to find academic resources, and in some way, we could be managing a team or a company in Europe from the Amazonian jungle, from a tree house in Mexico or a tent in Denmark, as long as we have high speed broadband and decent technology – imagine what Da Vinci would have achieved if he had those in his time!
To begin with the Hitler dossier, this cannot be a simple answer since there are many things to say and explain so that people from the world over may understand my views and also have an understanding of all the controversy surrounding the “Fuhrer”. While answering this question I will also refer to the “Organic Theory” in explaining human existence, adaptation and evolution and also refer to my own case as an assimilated Franco-British Western European fairly similar to the case of Hitler or Napoleon who were both also not natives from the society they led, but were assimilated, surprisingly it seems that the two most powerful leaders in Western Europe had to come from another land as if sent by fate to solve the problems of a civilisation that had no legendary leader with vision among their own natives, and received a leader who won his nativity and became more national than the natives themselves. Hitler was born in Austria, while Napoleon was born in Corsica, and perhaps surprisingly 7 years before the birth of the future Emperor of France, Rousseau said that Corsica would shake Europe.
I have to say that from a very young age I was fascinated with the reputation of Adolf Hitler because like the great majority we were all taught that he was the most-evil person to have existed throughout human history, and his murderous obsession with the genocide of the Jews was something no sane human could possibly justify. Being just like most of people who grew up in the late 80s to the late 90s, information was and is still mainly distributed through the mainstream majority Jewish owned media outlets, a time when the internet was still blooming – specially video streaming websites – so, I was forced to digest the only perspective available to me until of course 10 decades into the millennium where a tremendous amount of Hitler files that were buried started to surface all over the internet, giving the world a clearer perspective of the war and its economic, philosophical and religious implications from both sides of the argument.
There is also the great confusion, misinterpretation and gossip media fabrication that exists regarding Hitler’s supposed desire for world conquest and obsession with the assumed superiority of the Germanic Caucasian race, especially the Nordic subtype with blond hair and blue eyes being one that should in the long run replace all the other races who are not of German descent – such as many inferior Slavic Eastern European societies with a fair amount of Jews & Muslims e.g. Poland, Bosnia, Chechen Republic and Russia, which he considered as cheap and inferior in culture, comparing them to minor animals – at least this is what the majority were told and made to believe. While the societies of Eastern Europe may not be as sophisticated as Western European societies, this assumption of inferior and superior subtype going only by genetic inheritance and physical attributes is not scientifically valid since we now know that organisms can be shaped with the right guidance and education to adapt to their chosen societies and this would have to be the case if an empire conquers and expands, and also that talent and genius, although very rare, can appear and have appeared from any corner of the earth in any society and of any organic composition, so a superior organism [intellectually or physically] can be born from any society and be part of any type of organic composition, not only the Nordic subtype of the Germanic Caucasian race, indeed even Mussolini who was another fascist and nationalist leader disagreed with Hitler on this Nordic subtype issue, and said that he did not believe in the superiority of just one particular subtype but in the overall quality of all subtypes, including the Mediterranean subtype with dark hair that creates a healthy mix among the nation.
However, the amplification of Hitler’s argument into a desire for extermination created a lot of confusion and which was further exaggerated and amplified by the mainstream gossip press mostly owned and managed by Jews to give the Hitler regime some bad publicity and worldwide hatred. As far as the recordings go, we only know of Hitler being focussed on national matters and clearly asking all other countries to leave him and Germany alone to focus on their own society and to be allowed to shape their society as they so wished since they inherited everything from their ancestors and wanted to preserve their society after having been given the authority to do so in democratic elections, and also keep the national German race “pure” [which of course made no sense because no race is pure since we are the result of migration, interbreeding and evolution from different subtypes and Hitler himself was the result of inbreeding between a man and his niece, the type of union that the man behind the theory of evolution, Charles Darwin was himself against along with marriage between cousins which he tried to make illegal by law due to the amount of deformities and disabled infants this led to and the dangerous genes this would spread].
So, to begin answering your question I will first say that Hitler was a firm patriot and a defender of the society and people he represented [not different from myself and my views for France and Western Europe in fact] and saw that to strengthen a country in more ways than one, the emphasis should first be on those who are part of, identify with and love the native people of the country, the latter being those who created the individual identity of the nation and those who represent the majority who drive the country and contribute to its functioning and continuation – this is a philosophy in line with the good management of a civilisation and my very own philosophy of the “Organic Theory” but only in part because the complete solution also involves taking into consideration the influx of talent and the evolutionary adaptation of other skilled organisms who also contribute to the maintenance and progress of the nation and who gained their nativity and completely identify with the nation, being a part of it.
Unfortunately, Hitler and his advisors exaggerated and misinterpreted the understanding of organic evolution and followed an atavistic and retrograde policy with a team who proceeded savagely, without carefully considering the fundamental logic that exist in all fields of life, which is that we have always had exceptions to the rules for exceptional cases – this applies to mathematics, arts, medicine, and science – which should also apply to any system deemed practical, modern and evolved. All organisms on this planet adapt and evolve from an organic and socio-linguistic standpoint, although not in equal measures and as I have said, if the laws of nature and evolution that contain all life on earth decided otherwise, then organisms from different organic compositions would not be able to procreate.
Hitler’s team was also composed of many traitors with fairly basic education who took murderous decisions that they hid from the “Fuhrer”, resulting in his downfall and the complete annihilation of his plans and system; towards the end they all placed the blame on one man as if Hitler had drugged a whole nation and hypnotised them into mechanical puppets – which is also clearly impossible without a nation’s faith, will and desire to go into the directions of his vision. It should also be mentioned that to date, not a single recording or written message has been found from Hitler giving the green light to the extermination of any people, and what can be concluded today is that Hitler believed that all societies and races should simply be nationalized so that all societies and races could behave better and perfect themselves like the German Reich. On the issue of mass murder, the blame today according the facts that have been collected are mainly attributed to Göring and Himmler, the latter going by ancient Aryan scriptures of Hinduism believing himself to be acting like the great warrior Arjuna who was purging his people and the whole world from evil and who believed that in the long run people would see him as the mythological hero cleaning the earth of evil which to him were the Jews and their values being the cause of all human suffering on earth as they destroy other civilisations and bend and control the minds of the masses through their media businesses.
First of all, I will explain what I am critical of the Hitler regime before also explaining what I believe is admirable about the legend of Adolf Hitler as a leader and a human being on this planet. There are a couple of things that I sincerely think are not acceptable in today’s enlightened society of 2021, and Hitler would have built a stronger Reich if he was better advised into smarter policies regarding the management, maintenance and shaping of a productive and sophisticated population with strong patriotic sentiments and a sense of synchronisation and understanding. Hitler did not simply aim to create a pink meatball company, but was a cultured leader guided by philosophy, ethics, morality, dignity, values and the arts and wanted the whole world to look to the German as a heroic role model to follow an be inspired by. Hitler wanted people to see the honourable SS men as legendary heroes who wanted to make the world a better place. Adolf Hitler was no pig or just a simple soldier.
It is fundamental to understand that at the time of Hitler, Germany was being taken over by communists who were methodically focussed in taking over Germany without any real sense of belonging to it, with the intention to simply turn it into a form of trading area and an economic backyard in Europe, similar to what the influential mainly Jew business geniuses have turned the United States into nowadays – a mechanised an industrialised society lacking a human touch and values, where selfish individualism has left everyone in a constant struggle to survive at whatever cost even if it means killing one another which is also common with firearms being legal there.
The Collapse of the American Empire?
The leaders of these communist groups in Germany at the time of Hitler were composed of a majority of foreigners which included many Jews. While the death count of Jews has been exaggerated and used to vilify Hitler, no major focus has been placed over the amount of horrific deaths that Jews caused in the Russian revolution and many revisionist historians have been claiming a much higher death count than the Hitler regime. However, it was clear that besides Jewish immigration and political influences from Jewish communists gradually weakening and corrupting German society, there was also a huge problem with the immigration of populations who were not native Germans. This implied that for a man like Hitler to achieve his dream of a strong, stable and modern Germany, the immigration issue would have had to be addressed, and being one with a vision of national focus and excellence, the offloading of excessive, incompatible and alien crowds who did not want to fully assimilate and become German citizens was something necessary to his vision.
However, there is no question also about the fact that Hitler should also have realised that there was a great amount of human beings who were highly talented and had completely assimilated in German society that had to be kept and treated as citizens who gained their nativity along with a strong sense of identification with the native crowd through their own adaptation and evolution. And since this was not the case, we ended up with World War II, many people dying in badly supplied detention camps after the allied bombed the connecting railways and disrupted food and hygienic supplies leading to an outbreak of typhus which killed thousands. Also many Germans who happened to have some distant link to the Jewish population where treated as criminals to be deported and this lead to an irrational operation that discarded people who were perfectly fit to be part of a functional society as today’s scientific standards have proven along with a proper interpretation of the theory of evolution: that we are organisms who can adapt and change identities to fit new environments if we make the choice and have the abilities and desire to do so. The Nuremberg laws which defined who should be qualified as a German based on genealogy was one of the German Reich’s most irrational and stupid decisions since it was not based on any good science. It was necessary for Germans then to prove that their parents and grand-parents had no Jewish ancestry; this was hypocritical since Hitler himself could not prove that he had no Jewish genetic links because his grand-father [the father of his father] is unknown; and many have suggested that he was the illegitimate child of a rich Jewish family’s member after an adulterous relationship with Hitler’s grandmother whom the family employed as a handmaid or a cook. Furthermore, from the defintion of the supposedly “perfect Aryan” who is supposed to be blond, blue-eyed, slim, tall, none of the top Nazi leaders shared these physical characteristics: Hitler was not blond, Goebbels was not tall, and Goering was not slim.
The other side, was that of the superiority of the German people that Hitler was obsessed about and who in fact turned out to be fairly uncreative by not considering people who had part German inheritance and cultural affiliation as an example of a form of German conquest, as it was also a way for a civilisation to spread its genes further and wider, and encourage the people resulting from this blending to mix with the founding civilisation which would lead to their future lineage to share an even greater amount of German genes. In fact, if science and evolution along with the average superiority of the “Aryan Race” was what guided the policy of the National Socialist regime, then they should have also encouraged the widespread of the Aryan genome by encouraging the healthiest and finest men and women from the Aryan race to donate eggs and sperm and encourage couples to use healthy donors of the Aryan race in breeding children, and this service should have been offered to couples from all walks of life to prevent the creation of malformations and unhealthy organisms. This would have been a sophisticated and modern way of thinking of human evolution and societal evolution in a Hitlerian way. A way of saying is that to change their society biologically, one great way is to make sure that they have enough “cream tarts”. Because, I believe that after all, human beings should be given the freedom of their choice of partnership, which was not the case in the Reich; as native Germans who did not breed with native Germans were considered as traitors.
Hence, this form of extremism was one of the major doctrines that lead to so much hate and resentment to the Third Reich from a large amount of Germans themselves, leading to an allied army to work consistently to bring down the whole show, although the opposing side represented values of a society that were not any better in providing a solution to a harmonious civilisation but were mostly fuelled by hate, strong Jewish financial motives and the desire to cripple Germany at any cost, but mostly to bring down the charismatic and overly powerful Adolf Hitler, as it is often the case whenever a gifted man rises to the top and dwarfs his competition with his talent and magnetism. This was also the case of Napoleon, when the whole of Europe had gathered all its forces to bring him down, this old and sclerosed Europe of the United Kings to destroy all the achievements of the Revolution [freedom and equal opportunities for all] and restore the unequal Ancien Régime in France. This seems to be the case nowadays, as if society cannot accept that some organisms are superior to the mediocre majority. This seems hypocritical since we can all nowadays accept that we have superior food from a nutritional standpoint, superior computers, superior cars, superior football players, superior watches, superior cameras, superior guitars, superior pianos, superior horses, so, this should also apply to the human organism; meaning we do also have superior individuals with superior intelligence, and hence superior vision and managerial skills. It is important to also note that superior objects are always rare, and hence a minority, in fact, that is why they have immense value. If diamonds were as abundant as steel and steel was as rare as diamonds, then jewellery would be made of steel and diamonds would be used in construction. So, we seem to live in a world where the mediocrity of the masses seem to find it hard to accept that some individuals are superior as a whole, and instead of encouraging, learning from, being inspired by, and being proud of being led by such individuals, we seem to instead find a union of mediocrity trying whatever they can to bring those individuals down. This is something society has to work on globally, to nurture excellence! Respect and appreciation are after all words that exist in all dictionaries, and noble and cultivated beings know how to display them, and those who have never considered these values may try to learn, it certainly would turn them into more complete beings.
Getting back to the management of the population of Germany for a healthy, strong and stable nation, Hitler should have found a systematic form of “filtration”, involving forms of interview, health assessment, skill assessment & cultural assessment that analysed the whole segment of German population who were of foreign origin in whole or in part, and divided them into 2 groups: those that were fit, safe and synchronised with the German society to keep, and those that were a burden due to their inability to adapt and unwillingness to be German due to firm religious or foreign convictions to be diplomatically relocated to an environment and society more suited to their characteristics in the most respectful of ways. Those who were deemed fit for German society could even have been given a form of classification [subtype of the German society] if deemed necessary and should also have been made to swear allegiance and priority to their newly found identity and people which they should have respected if this is where they thought they belonged, otherwise it would be best for an individual to move and live in a society compatible with their heritage and with people they feel a part of, after all nowadays in 2021, income inequality has gone down and the world is becoming a more equal planet along with the technological advances that make life fairly similar from one part of the world to another. The organisms who assimilated could also have the right to 3 warnings before considering deporting them for not respecting their contract of allegiance after serious offences, and hence becoming “traitors” to the nation.
The filtration solution was not an easy one but was in fact a sophisticated solution that would have been more apt for a civilisation that was evolving and getting more complex decade after decade – we cannot expect easy solutions to suit a complicated civilisation. This was of course not the solution the regime opted for, but instead chose the fastest and easiest route to deport all Jewish, non-German and part-Jewish people which resulted in so much unnecessary suffering and misunderstanding, when many of these people were not even religiously affiliated to any religion and considered themselves more German that anything else, such as Sigmund Freud for example who was a product of the intellectual thought of the German tradition who later influenced psychology globally and Albert Einstein, another great man of science who was also without any religious sentiments, and had to flee to the United States.
It is also important to remember that the policies devised by the National Socialist regime also targeted all the people who were deemed as burden and unnecessary to the progress of the German society, which also led to many Germans being euthanised for genetic and other incurable diseases that was seen as impure to a healthy society and race, along with a lot of elderly people who were thought as unfit to live. So, this shows that even a great amount of Germans lost their lives, not only Jews and foreigners trapped in deportation camps during a heavy bombardment of German soils.
I find it also important to bring to the discussion here the fact that Hitler’s Germany was not some form of 100% pure native-German Caucasian only society where any other person found to be different were taken away, locked and shot. No… of course, Hitler was not such an idiot, and realised that he needed many foreign workers to complete the construction of his country [roads, buildings, etc] and indeed had many Eastern European and foreign workers on his construction sites, he also knew that the German economy should like all countries embrace tourism, and hence people of all kinds were allowed to visit Germany. Indeed, Hitler even hosted the Olympic Games where athletes from all around the world were present. Many modern historians who revisit World War II tend to leave out those details.
Hitler indeed wanted to concentrate on the Germans, but did realise that it was impossible to run a country without a fair share of foreign population that were fundamental. And this can be reflected nowadays in the example of Western Europeans’ absolute love for foreign cuisine, for example Chinese food or Indian food that they love to have at hand with the touch of a button.

Image: Chart showing the areas in England which enjoy the hottest curries / Source: The Telegraph

The single most important feature of Britons’ ideal pub is that it would serve meals (67%). Having a beer garden (63%) / Source: YouGov
And using those examples to explain the logic, it would be impossible to provide quality Asian food to the European market without some people from these regions present to manage the distribution and ensure the quality of the food. This extends to Italian food, Mexican food, Greek and/or French cuisine. Another example would be the scientifically proven benefits of Yoga as a health discipline, that has been adopted by the French society and many other Western societies, similarly, it would be impossible to expect the widespread of the lifestyle if we did not have some of the founders of Yoga to instruct a generation, and it is without doubt that the experts would have to be from where the discipline originates, which is India, who would lead to the training of other experts from other parts of the world, this also applies to other disciplines such as Martial Arts which also originates from the Asian continent.
The point is that Western Europe is not a region like any other, because it is the birth place of some of the greatest intellectuals, thinkers and inventors who have had a major impact on the world, and this has also led to the best learning institutions in various fields being in Europe. This attracts some of the finest academics from all over the world who pay huge fees to study in those institutions, which also bolsters the economy of Europe and when this happens, it means that the government has more money to spend on its own people, system and infrastructures. When these top foreign scholars complete their studies, a great amount move back to their homeland but some are also employed as highly trained specialists and skilled workers in their fields by giants of the European business world in fields ranging from engineering to medicine. It is important to also realise that these people’s contribution lead to the progress of European institutions and their reputation. Hence, these skilled workers while not part of the cultural sphere or show business or the mainly Jewish-owned Hollywood industry, are sometimes part of the team who find a new invention, a new engine, a cleaner way of harvesting energy, a new cure, a new treatment, and where the world is dangerously heading at the moment with antibiotics becoming useless, who knows whether one among them will find the ultimate antibiotic, and if they do, this will lead to saving so many producers, composers, meso-sopranos, pianists, ballet dancers and painters, along with their loved ones and children throughout time from dying from petty infections such as Frédéric Chopin. So, it is important to also note that some things are bigger than outer beauty, but has more to do with the inner beauty of the mind reflected in intelligence and academic abilities. Moreover, in answering your questions, and in reviewing these writings during the period of containment in March 2020 in the face of the global crisis of the Coranavirus (COVID-19) that has already claimed thousands of lives globally, I have once again by “coincidence“, a spiritual phenomenon that has become very normal in my life and and those who follow and read us will have also noticed that I have learned to live with these never-ending coincidences and similarities by questioning the stars and God, found my thoughts in the words of Didier Raoult in one of his presentations given in 2015 [See: Le processus de l’innovation peut-il respecter la règle ?].
The other scenario is that in many cases these skilled workers having spent so much of their life in the Western civilisation end up in a marriage with a wife from the countries they work, for example, skilled foreign doctors marrying their nurse, offering the latter a life that she never dreamt of. So, these are things that happen in the human world, and these minor blending of genes has always happened since the beginning of mankind, as I have repeatedly explained since our current breed is a result of movement across the plains of the earth, interbreeding and evolution. So, trying to stop such a force that has shaped our kind, seems like a fight against nature itself, hence it seems unnatural. The only thing that can be done is to guide people into a better understanding of their own society, its people and its identity along with its continuity and the efforts this requires from all its citizens – otherwise any system crumbles and disintegrates – and those who become part of a society should know that if they do not assimilate and become part of the people they will always live a mundane and incomplete existence, that could be compared to that of a rat. Minor cases of genetic fusion in some cases also adds highly talented genes to the gene pool of a civilisation since excellence may stem from any organic composition and when made part of a civilisation only strengthens it, because it spreads among the civilisation throughout time. The decent thing to do would be for the State to always control the amount of foreign people in the country by imposing a strict limit in relation to the native population, perhaps agree on a percentage that should never be exceeded, excluding university students.
Hence, the Hitler regime should have known that it was only going to fail and create a lot of resentment and hate by trying to separate human beings legally through rigid formalities and proof of genetic identity through obsolete ideas such as German genealogy as the National Socialist regime did. This is because, society had already evolved and many links had been made among people who married and had children, some of different religious faiths, origins and nationalities among the German nation. And these types of rigid rules that would expel those not conforming to them through genealogy and ancestry could only lead to families being separated and even many German individuals having their wife or husband deported, and when these scenarios happen, humans tend to fight to the death to save those who are dear to them. Hitler’s regime should have known that this kind of policy was doomed to fail.
What I believe would have instead worked, was an “informal” execution of the vision of a strong Germany. That is, Hitler should have created a society, focussed on German citizens – both natives and those who firmly assimilated and saw themselves as native Germans – with a strong German identity and sense of concern for the people and nation, while nationalising the industries and ensuring that the people at the top are completely dedicated without any other motive than the progress of the nation and have national values, humane dignity and understand the religious identity of the nation by favouring people with proven strong German sentiments. After doing this, the regime and the nation would automatically have generated a climate that would portray the vision of a strong nationalist Germany, with industries focussing on the German people, and without any formal policy of deportation and genetic screening, the people would have soon found themselves in a society that had been reshaped to reflect the values of a nationalist Germany, with pride in its history, people, culture and values without systematically attacking others. After this, the businesses that could not adapt would automatically close and leave if the authorities adamantly declared that no Jewish tradition will be tolerated on German soil and no person of the Jewish religion or community would be allowed to run any form of business except those who have given up on their Jewish identity and fully embraced German tradition with the official religion as optional. The people who wanted to remain in the National Socialist Germany would automatically evaluate their abilities and possibilities and would either force themselves to abide by the rules and embrace, develop and learn to be German citizens or leave. It would automatically have generated a sense of “adapt, perish or leave” logic in the minds of the population of Germany, which would have led to assimilated people of Germany to get closer and strengthen their links with the German native people to be part of the great vision of a Nationalist Germany, or they would have left due to their inability or refusal to adapt, take part and contribute in the betterment of society.
So, this is what I think should have been done, the ideas and vision of the National Socialist regime should have been applied informally and not formally through strict military regime, deportation camps, genealogy investigation, and the atavistic and unscientific claim of “blood”. Indeed, there is no such thing as “blood” as it is referred to in culture, blood is a liquid that runs in the veins of human beings, yet even family sometimes do not have compatible blood since they differ by group and sometimes need complete foreigners or individuals from a different society to donate blood to save the lives of others who are not related to them. So, this idea of “blood” should be carefully used and best suits metaphors in “culture and literature” than reality, since it seems to be used to explain loyalty, togetherness and relatedness through a similar nation, society, values and outlook. Using this example, I can today say that I have Franco-British blood running in my veins and that would work culturally, but medically it would not make much sense, since my blood will only be compatible to individuals of my blood group who may be from any part of the world and of any type of organic composition or society, as long as they are humans beings and not animals.
The last thing I also question in the Hitler regime situation is the true power of democracy in our times, yes! I mean, the people of Germany had voted for the National Socialists to come into power after clearly knowing their manifesto and ideas of a nationalist Germany without Jewish presence. Hence, I question whether if tomorrow I campaign and for example say – note that this is just an example, not a statement of intention – that I will make it illegal in the country to have any form of Islamic worship areas because we know from historical facts that it is a religion that has waged tremendous amounts of violent wars upon Western Classical civilisation and all other non-Muslim religions and is a cult of war, blood, conquest and domination by all means; and if I am elected, I guess I would be bombarded by allies and jailed for trying to do so! This means that even if a form of democratic referendum supported my ideas, all other conventions would prevent me from doing it, hence this seems to suggest that countries have lost their democratic power and cannot satisfy their own people anymore, and this should leave authorities out there with a lot to ponder about.
The other issue of cultural assimilation which involves becoming fully part of the nation requires embracing the cultural theme of the nation and this applies to individuals and their names. What I mean is that assimilating generally involves carrying a name in line with the society’s heritage, and many Jews understood that, unfortunately the rest still do not seem to understand that with a name like “Mangia Fazula”, “Okolo Sambaweh”, “Munjabar Sakalamaktoum”, “Soupovic Boringov”, “Adnan Sawey” or “Aharon Azriel” they will automatically be seen as outsiders in a country of Western Europe founded on Western Christian culture. So, people who want to be fully part of a nation through assimilation should also be intelligent enough to understand the cultural theme that also applies to names, along with the combination of physical fitness that simply eases the process and a mastery of communicative and behavioural patters and a strong sense of togetherness with the nation, while also accepting the religious identity of the nation even if this is optional – being a matter of spiritual connection and the sanctity of one’s soul and it is between the individual and his own conscience and “God” if he believes in him.
As for the strong Catholic rhetoric encouraged by Hitler and his regime towards the education of religion and values to the youth, it is somehow important to remember that Jesus Christ, the messiah who led to the foundation and widespread of Christianity was not born of European stock or speak French, German or English. Jesus Christ was born out of the population of Israel and spoke in Aramaic. Of course, he was not of Jewish faith, and the religious texts and inheritance of Christianity was translated to the Western languages to reach a wide public. Hence, this could have also been done to any other religion if it was the one to have been adopted and spread in Europe, e.g. Hinduism. If that was a scenario that took place, then all Hindu texts and hindus of Europe would sill be speaking and praying in their own European languages, not necessarily the native language of the gods, i.e. Hindi, since all the religious texts would have been translated into the respective languages of the European region. Similarly, modern day Christians of Western Europe do not speak Aramaic, the language that Jesus spoke.
The point is that as the Organic Theory explains the communicative patterns of human primates may vary from one region to the other, but creativity and IQ do not, and hence, once the legacy of humanity is translated into the appropriate language [communicative pattern], society should instantly be relieved in the ability to understanding one another. So linguistic synchronisation should be one thing that would appease a world in disharmony although values and religious beliefs will always separate groups, so the debate today towards a harmonious civilisation should certainly begin on the global language of humanity to adopt. A good example would be to see the commercial success and creative influence of the modern art form known as “manga” – which originates from Asia – on France and other Western European societies once they are dubbed into the right language. For example, one of the great classics of French literature, the novel written in 1844 by Alexandre Dumas, “Le compte de Monte Cristo”, a title that has been the subject of numerous film, television, musical and animated adaptations, has also received a graphic interpretation in manga [see the picture above].
And now, having spoken of the Organic Theory above, I would like to explain its application to a modern human civilisation along with individual organic evolution and assimilation, so that most non-academics and lay people reading this out there may have a clear vision of what assimilation is from an objective and rational standpoint and also what it involves and requires for an organism to consider whether it has the potential and requirements to assimilate in a particular society, and how it enhances a sophisticated society, and here, how it would have helped in the policy of Hitler to creating a modern Germany or any leader’s vision to creating a modern country.
When talking evolution, the evolution and fitness of everyone should be taken into consideration, because all forms of Homo Sapiens are evolving together on this tiny planet called Earth in ways that are so fast that the textbooks cannot hope to match and explain – hence the importance of resourcefulness and creativity from avant-garde thinkers gifted with fluid intelligence.
First of all I would like to address the issue of assimilation from the organic stand point and since I am a perfect example of the French school of thought along with a strong British side, I will be explaining this process using myself as an example. Now, I have inherited the knowledge, language, values and philosophies of the French empire and the language of the British empire through cultural transmission after these empires conquered lands and expanded their realm. So, I did not wake up one morning, suddenly speaking French and English while also knowing the history and literature of these languages. And if the tiny island that I was born was near Western Europe, it would be part of Europe, then I probably would not have to answer all those questions, because it would have been seen as a product of European civilisation with the simple difference that some of the people that constitutes its nation come with a variety of skin tones with many being high in colour and texture differing from the common majority of pale pink because of some blending that happened through the course of Western European conquest. Yet, this would not have been such an issue because there are many countries of Europe where the people are not as pale as the common majority, for example Spain, Portugal, Italy and Greece – this is simply a slight similarity in physical attributes, not language, or anything else, so it would not make any sense to place those nations in one group! But, since the location of my birth is a place far from Europe geographically although born on Western European heritage, and I travelled to join the roots of my cultural inheritance in Western Europe since I am among the literary elites of new generation that was born in an independent republic with a new culture and educational system, language and French values, I feel that I am a good example to explain the process of assimilation from the Individual Organism’s perspective using my very own Organic Theory.
Now since I explained that the individual organism born on planet earth according to the laws of nature and evolution is free and is still evolving since evolution is a never-ending process. I will also bring to the attention of the public that according to the laws of nature, man-made barriers are not part of natural laws, they are simply barriers that have been erected by political groups. Hence, the individual organism is born on a planet and can adapt and change according to its abilities and its choice of environment. With today’s advancements due to technology and its accelerated learning facilities, organisms can learn and shape themselves linguistically and philosophically for the environment that they want to be a part of. However, there are some limits to this process too, as a high level of proficiency in terms of behavioural and communicative patterns will be required for an organism to assimilate perfectly with a chosen environment and be seen a complete part of it while being synchronised with the natives. For example, I had inherited the communicative, behavioural and social patterns of France and England, these were embedded in me and I also made the choices to deepen my understanding of these societies through my educational choices and from a very early age always intended to pursue my career and end my life in Western Europe: France and England. This means that I invested a lot of effort in redefining myself as a Franco-British Western European because nothing happens to anyone without sacrifice, work and dedication.
The point now is to explain that for an individual organism on earth to consider assimilating into a chosen environment, it is not an easy process, but comes with immense challenges and sacrifices. If we are to become part of a new society, we will not be able to do it by remaining who we are, but we will have to reshape our selves and adapt to the society and strive to become one with its people, and in some ways see them as one’s own “blood”- metaphorically. Furthermore, there is also the issue of fitness, which has nothing to do with “beauty” but rather the ability to blend in with the organisms of this society through some form of physical synchronisation. This is only one part and not the sole factor that defines assimilation but it is one factor that eases the assimilation process, although it is not everything. For example, using the organism that I am, I was born with an Indo-European heritage and although I may be slightly less pale that the average majority of organisms from the Western European sphere, I still have more physical similarities with these people since they are also of Indo-European heritage and of what is also known as the “Aryan Race”. What I am trying to say is that I chose a society where assimilation was achievable because there were strong links in my own genetic, linguistic and cultural heritage with those countries: I spoke the language, read the literature, knew the history, sang, played and listened to the music, share the same religion and studied and understand the philosophies of its greatest minds. So, this means that the organism that I am had all the chances of assimilating in the Western European sphere of both France and England.
This may not have been as easy if for example I decided to assimilate in the Negro civilisation of Africa because to begin with the physical fitness between the organism that I am and the Negro people is incredibly far from each other; but even more, I do not have any links with Negro culture, languages, history or philosophy. This does not mean that it would be impossible, but it would have been very hard due to the difference in civilisation and ways of living.
Since we are on the negro topic, if in the 1950s a person had made the statement that negroes are an inferior race and heritage, people around may have said that the man is biased and racist. Yet, this is not implying that every single negro is inadequate or unskilled, of course we do have some great negroes who excel in mostly physical disciplines such as sports and a couple of others who have become professors in specific fields. But what it is generally implied through the statement that “negroes are an inferior race” seems to suggest that on average, meaning that if we took all the negroes and averaged their achievements and compared it to all other civilisations, we will come to the fact that they are lagging behind in everything, hence the term “inferior”. Nowadays, if we look at all the statistics globally concerning the negro people, we will see that indeed they are behind all other civilisations. Yet, every time this topic surfaces, we suddenly see all the mainly Jewish owned media, suddenly throwing all the singular negros in the United States that have made money; we see basketball players, rappers will grills in their mouth, and all the other negroes that have succeeded financially through the Jewish-owned media industries of the United States. Hence it is once again, not the point, because I am not saying that all negroes are inferior, but simply pointing to the fact that on “average” the negro civilisation is inferior to all other civilisations on planet Earth. And if this is not enough, they are also physically incredibly unique in terms of features and traits compared to all the other civilisations on Earth, which makes them a conundrum in matters of assimilation into any culture. So, for me, the negro people should take this into account and with the developed world that we now live in and with technology making the world a much more connected place that makes life fairly similar on any part of the Earth, I firmly believe that they should start uniting and organising themselves to bridge the gap with the rest of the world and consider the development of the African continent where they would all find enough space to live. The world has been very charitable to negro causes, but it is time for them to start helping themselves. The other point with negro people is that they too are fairly similar to Jews when they move to other societies, they are generally focussed on negro matters and negro people, they are a group of people who are more focussed on expanding their numbers in a country that is not theirs, rather than focussing on the national matters and the native people, this is not assimilation and if it is not, it is not beneficial to any system. So, once again from the Organic Theory’s perspective, this only generates and creates more problematic organisms that are not part of a system and that has problems with assimilation due to immense differences in organic composition, behavioural patterns, goals and outlook and only leads to slowing and weakening any system. In 2021, it seems fair to explain what true assimilation is, and also with the world more developed, more equal and more connected, to guide those who cannot or do not want to assimilate by explaining them how organisms sharing similar organic compositions, values, culture, vision and history have all the factors to create harmonious societies by being together. Negroes and Jews should both consider this, and perhaps meditate on whether they would be happier in a society composed of their own kind, which may generate less tension and a feeling of being at home in a negro or Jewish atmosphere reflecting their beliefs and rituals. Because, the Western civilisation is far from perfect and also has its own problems to tackle, its own people and matters of management to be focussed and if the nation has a crowd that is not focussed in contributing to this it only worsens the problems.
The Enemies Of Reason – The Irrational Health Service
We do sometimes see people of the Western crowd comparing themselves to members of third world crowds and foreign tribes to generate a fake sense of superiority. I would like to remind people that this by no means leads to the betterment of their lives. The Western society has a lot of problems that are deeply rooted and cannot be perceived with the naked eye from the surface, since it is a society that seems in love with packaging everything neatly, but being an intellectual who studied psychology, I can confidently say that there are immense problems in the West regarding the cultivating of minds for the betterment of our lives. Many people are sick in their minds and do not realise it and tremendous amounts of work remains to be done is fixing mentalities and instilling values for a harmonious and healthy society.
People who do not assimilate generally do not have these matters at heart and tend to simply park themselves in Western Europe for an income while remaining foreign in their identities. These people should understand that if they are not assimilating, they should not expect to be treated as the organisms that are native and are fully part of the system because the system relies on its organisms for its continuity and existence, and this will also happen to their children if they are raised on foreign beliefs, identity and values that are incompatible with the nation they live in.
People who are in the west as highly skilled workers and do not want to assimilate should clearly classify themselves as temporary organisms who do not intend to stay forever and accept the life of a foreigner and the burden that goes with it, because I am not saying that the natives are perfect or that all of them are superior since we do have classes and different levels of education in all societies, but what I am repeating is that the problems of the West need contribution and concern from its population to be resolved and those who do not contribute are not helping to make life better for themselves and the country – natives and non-natives alike. This is of course not a problem for tourists who are only visiting for photos and return to their countries after the trip is over – no problems.
Now having spoken of the example of me trying to assimilate in the negro civilisation, a similar situation would be faced if for example I decided to assimilate in the Eastern Asian sphere, since the differences both physical and cultural are immense, and although not impossible, it would come with huge hurdles with such differences that would make it a hard task for me to be seen as a member of their societies in line with their very own natives – and there is no point discussing the further hurdles with huge differences in eating, behavioural, communicative and living patterns.
As a third example, a similar situation would occur if I decided to assimilate in India, because although they may be linked to the Indo-European people, they are clearly a distinct civilization that has divided itself and acquired its own models of communication and behaviour, which I do not know a single word and do not understand or manage, to make matters worse, I don’t look like an Indian either because of course I’m not, even if some may share an olive skin tone, and finally, they are a mainly Hindu civilization that is reflected through their culture and art, while I’m a Christian deeply rooted in the art of French civilization and Western Europe.
The fourth example is an attempt at assimilation in a Muslim civilization, such as Algeria. Again, I couldn’t, because I don’t speak the language, I don’t reflect the values, I don’t believe in Islam and finally, my vision and lifestyle are totally incompatible with the cultures of the Muslim world, and to complicate things further, I don’t look like the Algerians either.
Hence, if I was to be thrown in India, Eastern Asia, Africa or a Muslim society looking in the eyes of these organisms to me would be like looking into the eyes of a deer, which I believe is a very good metaphor that I am using here to describe a completely ignorant creature partly because of its innocence since it has never been thrown into and will never have to know the agonising and non-stop drama of having to solve the problems of the supposedly modern world of the western civilisation while constantly having to endure the insecurity and pettiness of “some” of the vilest and immoral cannibalistic reptilian-like public figures dressed in suit whom no one with a sane mind and enough insight would ever want to introduce to their close ones or have over for dinner once they discover the truth about the limitless possibilities of their savagely hedonistic depth and immoral and rotting dark minds.

Image: Fear and Loathing in Las Vegas (1998)
In fact, as a literary elite, I believe this feeling of always being surrounded by deer of all colours, shapes, sizes and origins in most places, all over the Earth from the West to the East, must be shared among other literary minds, because most organisms simply exist, while literary people into fields such as psychology and philosophy have to carry the burden of thinking for society and it is a huge moral task that comes with a lot of pressure and responsibility, while rarely being able to connect with the simple minds we sometimes come across on our meditative road, which only leaves us with the option of either smiling, or saying something insignificant and sweet, such as talking about the weather.
So, getting back to the issue of physical synchronisation, as I have repeated, physical fitness [which has to do with slight similarities and not “beauty” as it is commonly believed] only helps and eases the process of assimilation but is only a shallow indication of belonging, since the depth of an individual is an even more defining point, because the true worth of an organism lies in the mind, the outlook and the values.

Image: Bobak, A., Hancock, P. and Bate, S. (2015). Super-recognisers in Action: Evidence from Face-matching and Face Memory Tasks. Applied Cognitive Psychology, 30(1), pp.81-91.
To further this logic, I will give the example of a few other pale skinned organisms from some foreign societies who despite a pale skin tone are absolutely incompatible with the society of France, so it is not because they blend deceptively by giving a surface impression of being part of the majority through their skin tone that it means they are perfectly adapted to assimilate, because they do not reflect the linguistic heritage, the values, the founding philosophies of individual freedom, the Christian thought that shaped the civilisation even if they are not religious, and the receptive and human character of France.
A good example would be to consider Jews, Eastern Europeans, Russians, Mennonites or some segments of the Syrian population who sometimes happen to share a paler skin tone. And since we are on the topic, I have also never noticed “Jew” as a separate empirical category in the atavistic forms of the Anglosphere, why? After all, Jews are a distinct race, as those who seem obsessed with empirical research have discovered – this is not a cause for concern to me because I see things from the advanced evolutionary perspective of “Organic Composition”, but I ask myself the question for those obsessed with the laboratory. What genetics seem to have revealed is that there are powerful genetic markers of Jewishness, so Hitler’s intuition seem to have been right. So, the Jews did not arise from conversions in Europe because geographically and culturally distant jews still have more genes in common than they do with non-jews and these genes are of Levantine origin [area where Israel is located] which points to a mixture of Eastern-Caucasus [area around Russia, Georgia, Azerbaijan, Armenia, Eastern Europe and Western Asia], European, and Semitic societies that seem to complete the missing link of the Jewish European Ancestry. It is now believed that the Ashkenazi jews descent from a heterogenous Iranian population that later mixed with Eastern and Western slavic people and possibly some Turks and Greeks in the territory of the Khazar Empire around 8th century A.D. Although my perspective on race comes to a simple matter of “different organic compositions”, it is simply a small observation for those scientists obsessed with genetics. Once again, it is important to consider the global evolution of all organisms, and also never forget that a superior organism can come from anywhere on earth – the evolution of the human race is continuous and never-ending.
I’m not saying that some people are animals or that they should be exterminated, so don’t consider my comments as discriminatory, because I’ve already explained that the individual organism has all the powers of self-creation and self-definition and that from an evolutionary point of view, human organisms of any “organic composition”[race] can procreate with whomever they want, and the superior organism can appear from anywhere, but this scientific reality is not enough to be assimilated.

Image: Yves Simoneau / Napoléon (2002)
What I am saying is that to “assimilate” in a sophisticated civilisation requires more than only physical fitness, it is not simply a matter of accepting “Big pink sausages” as Christian Clavier termed it in the mini-series “Napoléon” by Yves Simoneau in 2002, because we are not simply trying to create a society that has no structure, with the only defining point being a pale skin tone and then to flood the society with uncivilised pink balls of meat for the photo… no! Only the mainly Jewish Hollywood industry seems to see it that way, and perhaps because the United States is after all nothing more than a simple bastardised European colony composed mainly of migrants and Jews from the German and Anglo-Saxon sphere who tend to be very pale, if not pallid in terms of complexion, unlike many Europeans. They were forced to find a way to survive in the Wild West and had to unite around something in common, which they did around whiskey, guns, fried chicken, business and the English language that they also bastardized in their own version, while remaining an industrialised and mechanical group without any cultural structure – for the vast majority of course, which seems to have a deep frustration that is reflected in a contempt for modern Europeans who are perfectly assimilated to the societies that form their roots.
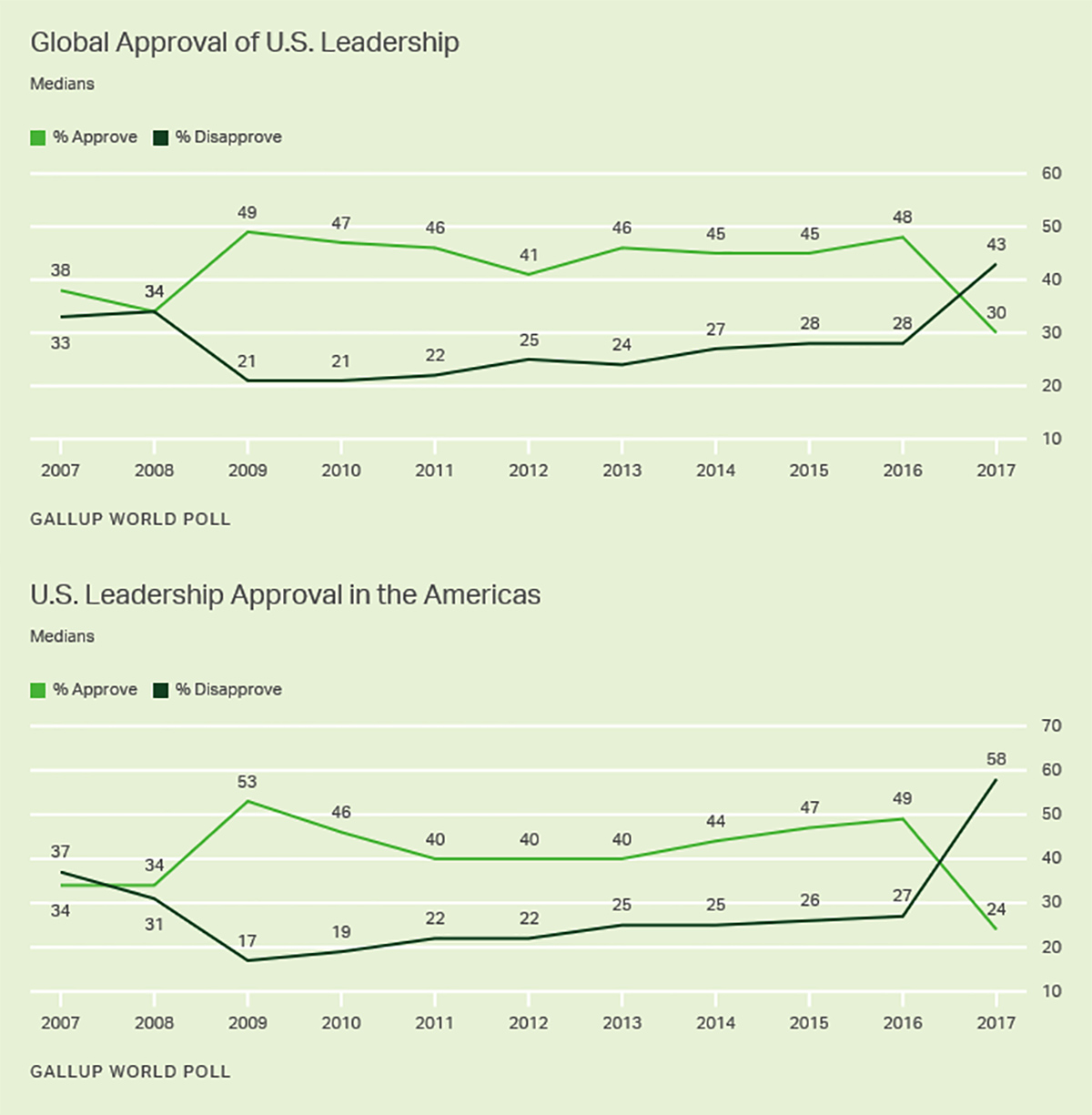
World’s Approval of U.S. Leadership Drops to New Low (Source: GALLUP)
Moreover, in 2021, my opinions on American democracy, which are based on years of research and empirical evidence and also observations based on the questionable values that some of the products of their industries intend to give to the world, seem almost similar to the perspectives of the great minds of the French intellectual family of the 18th and 19th centuries. For Charles Baudelaire (1821 – 1867), the system developed in America to transform a crowd of migrants into a kind of artificially synchronized nation caused Europeans to be uprooted in America. Baudelaire would find his thoughts in the texts of Edgar Poe (1809 – 1849), who was an American moralist writer who was himself anti-American and who painted a macabre and dark literary portrait on the theme of American vulgarity. America is not culturally free and Edgar Poe was for Baudelaire one of the few cases of refinement and sensitivity in the middle of this wild jungle; the American writer who allowed us to pierce the media and cinematographic lie, the revealing heart of America – as will some more modern artists after him such as Hunter Thompson and Chuck Palahniuk also turn out to be. It is a way of letting America itself, through its writers, show us its dark and repulsive sides. For Poe, who had incredible acuity of vision, America was the place where mechanical geniuses and animal forces were gathered. As for Jules Verne (1828 – 1905), he thought that Americans were mechanics, just as Italians are musicians and Germans are metaphysicists. For Jules Verne, one of the authors who greatly influenced the literary minds of his time in their childhood, America was always the nation of violence and he was particularly disgusted by the “Gun Club” which for him was the image of the United States: an imperialist and military nation and a country of extremes. For Jules Verne, America was the land of brutality and speed of means of transport. Moreover in “Around the World in 80 Days” we see the train used by Verne as one of those mobile places where we will meet different samples of the human population on earth. Paul Claudel (1868 – 1955) described Chicago as the city of blood. Apollinaire had traveled around the world in words on the “machine” that is America, an immigrant land where the savage European is connected to the savage Red Indian and was particularly interested in the sexual morality of the Mormons of the state of Utah who had transformed polygamy into a religiously permitted activity and made the United States a country with violent sexuality. Apollinaire described the people of Utah as Scandinavians in panties, Russians in red coats, English people wearing beards in collars, with Americans, Jews, Germans, etc. The American continent was revered but also repelled. Guillaume Apollinaire thought that Montparnasse at the time of the war was a projection of America in Paris: a juxtaposition of people from all over the world. In his writings Apollinaire also described the coldness of the people of Utah where he compared the rigid eyes of a spectator when a negro was hanged to those of an opium eater. Apollinaire thought that American democracy was insufficient and would always need Europe despite their Masonic symbol adopted from the triangle with the eye that was supposed to see everything. For Apollinaire, because of Mormon culture and polygamy, America appeared to be the country of women for Europeans. Europe was masculine and America feminine [LE rope & LA meric / French wordplay of masculine and feminine words], and so Apollinaire saw America as a woman waiting for the European conqueror, while France was the country of standing men who should beware of American democracy. Blaise Cendrars (1887 – 1961) who was like Guillaume Appolinaire (1880 – 1918) a great admirer of the new painting which was the cubist painting of that time [the artists of that form, the Delaunays created a cultural movement on their own], which brought together different views of the same object, had also concluded that New York had failed as a new Rome because the new side had won over the Roman side. The other French writer André Breton (1896 1966), who was an avant-garde and a great poet of the city, refused to visit New York during his stay when France was under German occupation, suffering from a nostalgia for Paris and noted that the United States had become much more foreign in only 5 years. And Jean-Paul Sartre (1905 – 1980) who like many had a dream transmitted by American cinema would see his dream turn into a nightmare when he discovered the truth about America during his visit just after the liberation. Sartre as Breton describes America as a mysterious country that was less well known than before and a country that was profoundly different from European cities, which despite its fascination, was dangerous and to be wary of. During the war America had established itself as the most militarily powerful nation, and the initial enthusiasm of Western Europeans for their arrival would soon fade after the discovery of their simple and ignorant minds. The United States suffered attacks from Jean-Paul Sartre for being a fragmented society, which Sartre described as having more steel and aluminium than human beings: the most mechanical city in the world where winter is much colder and summer is much hotter. Sartre thought that New York looked much more like a North African city such as Dakar than a European city. In America, Sartre was looking for and thought he would find a European city with his feelings, like a mother who saw the inhabitants as her children who had to be sheltered and cared for, but did not find it, since for him the United States did not have the same historical tradition or European nature, which proved disappointing for a European colony. Sartre found New York terribly foreign. And finally, a figure who is almost paternal to me, Michel Butor (1926 – 2016), one of the great professors of modern French literature visited the United States, inspired by the curiosity of great Western European writers in America, and found that one could make money, that one could also see some interesting things, but that one could not live in the United States, and that the strangeness on the other side of the Atlantic made most of the books seem false – Simone de Beauvoir’s anecdotes (1908 – 1986) were correct. Let us note here that all literature is a collective work because words were not invented by writers because language is a collective creation and hence creates a social bond; cities are also collective creations, as are the landscapes around these cities and the names of the great men and women who mark the places [the genius of the place], and this is done with the hope that the spirit of those men mark the future generations.

Charles Baudelaire (1821 – 1867), Jules Verne (1828 – 1905), Paul Claudel (1868 – 1955), Guillaume Apollinaire (1880 – 1918), Blaise Cendrars (1887 – 1961), André Breton (1896 – 1966), Jean-Paul Sartre (1905 – 1980) & Michel Butor (1926 – 2016)
Many Americans also seem eager to point out their long lost European ancestry while being disconnected from it in terms of values and philosophy, and they seem to be unaware of the social evolution of major European empires such as France. The Hollywood perspective may be fairly sufficient for an escort agency, a strip bar, to work as ladies of leisure or meet the criteria as sex workers, but apart from these businesses, a society requires more from its citizens, and here organisms with a sense of belonging and responsibility along with the appropriate behavioural and communicative patterns and names that fit the thematic sphere to be in complete synchronisation with the requirements of the society – so physical fitness is not enough but it simply eases the assimilation process especially among the common brains that do not think.
Indeed, the Jews have long used this visual illusion to blend among those they quality as “gentiles” or “Goy” of the European sphere, the non-Jews who according to their scriptures are inferior beings who were born to serve the Jewry and that can, according to their religious texts, be treated as animals and even killed if necessary. This is simply a factual observation of what is written in the religious texts of Jews. These are scriptures that have shaped the thought of Jewish societies since ancient times, and it is a fact that people should be aware of to understand the leading train of thought of a particular group, it is important to know the facts of the scriptures that shaped them, their values and outlook and why a great deal of their industries bleed civilisations dry of all their humanity. This seems completely opposite to [for example] the concept of Karma found in Hinduism which believes in causality through a system where beneficial effects are derived from past beneficial actions and harmful effects from past harmful actions, creating a system of actions and reactions throughout a soul’s (Atman’s) reincarnated lives – forming a cycle of rebirth. The causality in Hinduism is said to be applicable not only to the material world but also to one’s thoughts, words, actions and actions that others do under our instructions. Jews using their pale skin to spread and hide among the Christian Western European civilisation, have often throughout history had an easier ride, and when they change their names to adopt Christian ones in the process of blending in, it is sometimes hard to differentiate a great amount of them from the native people of the Western European civilisation that was born out of Christian thought and artistry.
The issue with Jews is that although they blend, act, dress and name themselves as the natives of the European nations they move to, they always clearly classify themselves as Jews, and focus on the betterment of other Jews, and work systematically together in business to further the interests of Jews, and even have worldwide conventions among Jews, and parade the achievements of Jews with pride. If we notice all foreign groups do this, except Western Christians who seem to prefer killing each other and live a life of selfish hedonism.
Yet, what these foreign groups do is not assimilation, but simply blending and integrating to systematically dominate a society or system, and Jews have been known to methodically and skilfully do this in many European countries throughout history, along with violent religious sacrifices to their blood thirsty gods that involve the sacrifice of Christian children, which they have done over the years throughout European history, with many mutilated corpses of young Christian children found across Europe drained of all their blood. This is why the Jews are the only group who throughout human history has been persecuted and banned from so many countries. Yes, many people do not know these facts since most people are without any choice but to take their information from Jewish owned mainstream media industries, so learn something new here!
The Hitler regime was not the first regime to ban and persecute the Jews, the Jews have even been banned from England in 1290 by Edward I, and also in 1306 from France by Philippe IV and these are only 3 examples. The Jews have been banned throughout a wide range of societies they moved to due to their insolence, their disrespect to the nation and the values of their heritage that encouraged the systematic destruction and enslavement of all non-Jewish civilisations, their habit of monopolising press business to distort perception and also their occult and violent rituals involving the killing of young Christian children to offer their blood to their violent pagan God, Baal from which the term “Holocaust” itself derives – which involved throwing people to their death in a burning Tophet. In fact, Jews have been banned in a wide range of countries since 1200 B.C until 2014 where they have recently been banned from Guatemala, which leads to about 3213 years of constant persecution and bans from countries they migrated to. In fact, they have been banned from Carthage, Rome, Egypt, Spain, Italy, Switzerland, Hungary, Belgium, Austria, Netherlands, Poland, Czech Republic, Lithuania, the Baltic States, and Russia to name a few. If people want to know the full list, they can use the internet and search “Countries where Jews were banned/expulsed” [also: Resolutions aganst Israel].
Here is what I believe created so much disgust and resentment towards the Jews from Christian nations. And if anyone had the time to read the Talmud, they would come to understand why the Jews have been persecuted in so many Christian countries and hated by the Pope Innocent III himself. As in our languages Christians take their name from Christ, so in the language of the Talmud Christians are called Notsrim, from Jesus the Nazarene. But Christians are also called by the names used in the Talmud to designate all non-Jews: Abhodah Zarah, Akum, Obhde Elilim, Minim, Nokhrim, Edom, Amme Haarets, Goim, Apikorosim, Kuthrim.
Hilkhoth X, 2: Baptized Jews must be put to death.
The jews teach that since Christians follow the teachings of that man [Jesus], whom the Jews regard as a Seducer and an Idolater, and since they worship him as God, it clearly follows that they merit the name of idolaters, in no way different from those among whom the Jews lived before the birth of Christ, and whom they taught should be exterminated by every possible means.
In the same book Sanhedrin (107b) we read:
« Mar said: Jesus seduced, corrupted and destroyed Israel. »
The book Zohar, III, (282), tells us that Jesus died like a beast and was buried in that « dirt heap…where they throw the dead bodies of dogs and asses, and where the sons of Esau [the Christians] and of Ismael [the Turks], also Jesus and Mahommed, uncircumcized and unclean like dead dogs, are buried. »(25)
In Iore Dea (81,7, Hagah) it says: « A child must not be nursed by a Nokhri, if an Israelite can be had; for the milk of the Nokhrith hardens the heart of a child and builds up an evil nature in him. »
In Iore Dea (153,1, Hagah) it says: « A child must not be given to the Akum to learn manners, literature or the arts, for they will lead him to heresy. »
In Zohar (1,25b) it says: « Those who do good to the Akum . . . will not rise from the dead. »
Hilkhoth X, 6: We can help goyim in need, if it saves us trouble later on.
In this way they explain the words of Deuteronomy (VII,2) . . . and thou shalt show no mercy unto them [Goim], as cited in the Gemarah. Rabbi S. Iarchi explains this Bible passage as follows: « Do not pay them any compliments; for it is forbidden to say: how good that Goi is. »
Rabbi Bechai, explaining the text of Deuteronomy about hating idolatry, says: « The Scripture teaches us to hate idols and to call them by ignominious names. Thus, if the name of a church is Bethgalia— »house of magnificence, » it should be called Bethkaria—an insignificant house, a pigs’ house, a latrine. For this word, karia, denotes a low-down, slum place. »
JESUS is ignominiously called Jeschu—which means, May his name and memory be blotted out. His proper name in Hebrew is Jeschua, which means Salvation.
MARY, THE MOTHER OF JESUS, is called Charia—dung, excrement (German Dreck). In Hebrew her proper name is Miriam.
CHRISTIAN SAINTS, the word for which in Hebrew is Kedoschim, are called Kededchim (cinaedos)—feminine men (Fairies). Women saints are called Kedeschoth, whores.
A CHRISTIAN GIRL who works for Jews on their sabbath is called Schaw-wesschicksel, Sabbath Dirt.
Eben Haezar 44, 8: Marriages between goyim and Jews are void.
Since the Goim minister to Jews like beasts of burden, they belong to a Jew together with his life and all his faculties: « The life of a Goi and all his physical powers belong to a Jew. » (A. Rohl. Die Polem. p.20)
It is an axiom of the Rabbis that a Jew may take anything that belongs to Christians for any reason whatsoever, even by fraud; nor can such be called robbery since it is merely taking what belongs to him.
In Babha Bathra (54b) it says: « All things pertaining to the Goim are like a desert; the first person to come along and take them can claim them for his own. »
In Babha Kama (113b) it says: « It is permitted to deceive a Goi. »
The Babha Kama (113b) says: « The name of God is not profaned when, for example, a Jew lies to a Goi by saying: ‘I gave something to your father, but he is dead; you must return it to me,’ as long as the Goi does not know that you are lying. »
(4) cf. supra, p.30, A similar text is found in Schabbuoth Hagahoth of Rabbi Ascher (6d): « If the magistrate of a city compels Jews to swear that they will not escape from the city nor take anything out of it, they may swear falsely by saying to themselves that they will not escape today, nor take anything out of the city today only. »
In Zohar (I, 160a) it says: « Rabbi Jehuda said to him [Rabbi Chezkia]: ‘He is to be praised who is able to free himself from the enemies of Israel, and the just are much to be praised who get free from them and fight against them.’ Rabbi Chezkia asked, ‘How must we fight against them?’ Rabbi Jehuda said, ‘By wise counsel thou shalt war against them’ (Proverbs, ch. 24, 6). By what kind of war? The kind of war that every son of man must fight against his enemies, which Jacob used against Esau—by deceit and trickery whenever possible. They must be fought against without ceasing, until proper order be restored. Thus it is with satisfaction that I say we should free ourselves from them and rule over them. »
In Choschen Ham. (425,5) it says: « If you see a heretic, who does not believe in the Torah, fall into a well in which there is a ladder, hurry at once and take it away and say to him ‘I have to go and take my son down from a roof; I will bring the ladder back to you at once’ or something else. The Kuthaei, however, who are not our enemies, who take care of the sheep of the Israelites, are not to be killed directly, but they must not be saved from death. »
And in Iore Dea (158,1) it says: « The Akum who are not enemies of ours must not be killed directly, nevertheless they must not be saved from danger of death. For example, if you see one of them fall into the sea, do not pull him out unless he promises to give you money. »
Lastly, the Talmud commands that Christians are to be killed without mercy. In the Abhodah Zarah (26b) it says: « Heretics, traitors and apostates are to be thrown into a well and not rescued. »
And in Choschen Hamm. again (388,15) it says: « If it can be proved that someone has betrayed Israel three times, or has given the money of Israelites to the Akum, a way must be found after prudent consideration to wipe him off the face of the earth. »
Even a Christian who is found studying the Law of Israel merits death. In Sanhedrin (59a) it says: « Rabbi Jochanan says: A Goi who pries into the Law is guilty to death. »
In Hilkhoth Akum (X, 2) it says: « These things [supra] are intended for idolaters. But Israelites [Jews] also, who lapse from their religion and become epicureans [Christians], are to be killed, and we must persecute them to the end. For they afflict Israel and turn the people from God. »
In Choschen Hamm. (425,5) it says: « Jews who become epicureans [Christians], who take to the worship of stars and planets and sin maliciously; also those who eat the flesh of wounded animals, or who dress in vain clothes, deserve the name of epicureans; likewise those who deny the Torah and the Prophets of Israel—the law is that all those should be killed; and those who have the power of life and death should have them killed; and if this cannot be done, they should be led to their death by deceptive methods. »
Rabbi David Kimchi writes as follows in Obadiam: « What the Prophets foretold about the destruction of Edom in the last days was intended for Rome, as Isaiah explains (ch. 34,1): Come near, ye nations, to hear . . . For when Rome is destroyed, Israel shall be redeemed. »
A JEW WHO KILLS A CHRISTIAN COMMITS NO SIN, BUT OFFERS AN ACCEPTABLE SACRIFICE TO GOD / In Sepher Or Israel (177b) it says: « Take the life of the Kliphoth and kill them, and you will please God the same as one who offers incense to Him. »
And in Ialkut Simoni (245c. n. 772) it says: « Everyone who sheds the blood of the impious is as acceptable to God as he who offers a sacrifice to God. »
AFTER THE DESTRUCTION OF THE TEMPLE AT JERUSALEM, THE ONLY SACRIFICE NECESSARY IS THE EXTERMINATION OF CHRISTIANS
In Zohar (III,227b) the Good Pastor says: « The only sacrifice required is that we remove the unclean from amongst us. »
Abhodah Zarah 22a: Do not associate with the goyim; they shed blood.
Rashi Erod.22 30: A goy is like a dog. The Scriptures teach us that a dog deserves more respect than a goy.
Kerithuth 6b p. 78: Jews are humans, not goyim, they are animals.
In Kallah (1b, p.18) it says: « She (the mother of the mamzer) said to him, ‘Swear to me.’ And Rabbi Akibha swore with his lips, but in his heart he invalidated his oath. »(4)
Every Jew is therefore bound to do all he can to destroy that impious kingdom of the Edomites (Rome) which rules the whole world. Since, however, it is not always and everywhere possible to effect this extermination of Christians, the Talmud orders that they should be attacked at least indirectly, namely: by injuring them in every possible way, and by thus lessening their power, help towards their ultimate destruction. Wherever it is possible a Jew should kill Christians, and do so without mercy. Jews must spare no means in fighting the tyrants who hold them in this Fourth Captivity in order to set themselves free. They must fight Christians with astuteness and do nothing to prevent evil from happening to them: their sick must not be cared for, Christian women in childbirth must not be helped, nor must they be saved when in danger of death.
Zohar I, 28b: The goyim are the children of the Genesis serpent.
Yebamoth 98a: All children of goyim are animals
Abhodah Zarah 35b: All daughters of unbelievers are niddah (dirty, impure) since birth.
Sanhedrin 52b: Adultery is not forbidden with the wife of a goy, because Moses only forbade adultery with “the wife of your similar”, and a goy is not a Hebrew’s similar.
Abhodah Zarah 4b: You can kill a goy with your own hands.
Hilkhoth goy X, 1: Do not make any agreement with a goy, never show mercy to a goy. You must not have pity on the goyim because it says: “You shall not look at them with pity”.
Hilkkkoth X, 1: do not save the goyim in danger of death.
Orach Chaiim 57, 6a: No more compassion should be shown for goyim than for pigs, when they are sick of the intestines.
Jalkut Rubeni Gadol 12b: The souls of the goyim come from impure spirits called pigs.
Babha Kama 113a: Jews can lie and perjure themselves, if it is to deceive or convict a goy.
Choschen Ham 26, 1: A Jew should not be prosecuted before a goy court, by a goy judge, or by non-Jewish laws.
Babha Kama 113a: Unbelievers do not benefit from the law and God has made their money available to Israel.
Pesachim 49b: It is permissible to behead goyim on the day of atonement for sins, even if it also falls on a Sabbath day.
Rabbi Eliezer: “It is lawful to cut off the head of an idiot, a member of the people of the Earth (Pranaitis), that is, a carnal animal, a Christian, on the day of atonement for sins and even if that day falls on a Sabbath day”. His disciples replied, “Rabbi! You should rather say “sacrifice” a goy. “But he replied: “In no way! For when a sacrifice is made, it is necessary to pray to ask God to accept it, whereas it is not necessary to pray when you behead someone.”
Sanhedrin 58b: If a goy hits a Jew, he must be killed, because it is like hitting God.
Chagigah 15b: A Jew is always considered good, despite the sins he may commit. It is always his shell that gets dirty, never his own bottom.
Zohar I, 131a: Goyim defile the world. The Jew is a superior being
Chullin 91b: Jews possess the dignity that even an angel does not have.
Iore Dea 151, 11: It is forbidden to give a gift to a goy, it encourages friendship.
Orach Chaiim 20, 2: Goyim dress up to kill Jews.
Shabbath 116a (p. 569): Jews must destroy the goyim books (New Testament).
Sanhedrin 90a: Those who read the New Testament (Christians) will have no place in the world to come.
THOSE WHO KILL CHRISTIANS SHALL HAVE A HIGH PLACE IN HEAVEN
In Zohar (I,38b, and 39a) it says: « In the palaces of the fourth heaven are those who lamented over Sion and Jerusalem, and all those who destroyed idolatrous nations … and those who killed off people who worship idols are clothed in purple garments so that they may be recognized and honored. »
JEWS MUST NEVER CEASE TO EXTERMINATE THE GOIM; THEY MUST NEVER LEAVE THEM IN PEACE AND NEVER SUBMIT TO THEM
In Hilkhoth Akum (X, 1) it says: « Do not eat with idolaters, nor permit them to worship their idols; for it is written: Make no covenant with them, nor show mercy unto them (Deuter. ch. 7, 2). Either turn away from their idols or kill them. »
Ibidem (X,7): « In places where Jews are strong, no idolater must be allowed to remain… »
Now, we can ask ourselves a few simple questions here, which is “Could all the people who have banned the Jews be without any reason to do so?” and “Could people simply walk around and suddenly without any reason decide to hate Jews?” and also “If this has happened to them for so many years, is it not likely that the problem is in fact with the Jews themselves?” I believe it is best to leave the audience to answer these questions and reflect on them alone.

War has always been a part of human civilisation: studies show that human societies in the past were very violent with the share of people killed often greater than 10% / Source: OurWorldinData
I would like to make it clear, that I am talking of the Jew mentality and train of thought as a whole, but I am not saying that every single Jew is evil or has nothing to offer to the societies they move to. Of course, there are some amazing, admirable and loveable individuals who completely assimilate, and even give up their Jewish identity and convert to Christianity, or become atheists. There are of course, some decent people of Jewish heritage who become fully citizens of their new societies, speak for the natives and see themselves as part of the nation, and this can be seen in France, where some have become more French that the natives and have embedded themselves in the heart of the nation. However, this concerns a very tiny minority of Jews who after doing so, often see foreign Jews as inadequate for France because they see themselves as part of the French people and understand the religious identity of the country being Christianity. However, the majority of Jews do not follow the example of the noble ones who assimilate, instead they remain distinct and work for their Jew comrades and organisations while embracing their values and beliefs of circumcision and superiority.
The fact that all foreign organisms need to grasp is that to be part of the Western European civilisation, means accepting the fact that Christianity is part of the founding culture, and while many people are not religious, it cannot be ignored that the whole history, inheritance and literature were founded by Christian men and women with some not being religious but who were undeniably directly and indirectly influenced by Christian thoughts and inheritance and this can be reflected in the large amount of allegory and metaphors related to the bible in the literature. It is also an immense coincidence that right at the same period when I am answering your questions that the Notre Dame cathedral has been mysteriously struck by a fire on the 15th of April 2019, some may see it as a sign of the foundations of a civilisation burning – and coicidences with my life are today not suprising anymore to me. When hasard multiplies coincidences, it is not hasard anymore.
In fact, to be fully assimilated means giving up on one’s foreign identity and embracing the new society’s history, language, linguistic theme, nation and religion as an added option if possible. Jews should reflect on this: the fact that Western Europe is a Christian civilisation, just like Israel is a Jewish society and the Arab states are a Muslim civilisation, with the governments of the latter two countries taking religion as a serious matter of culture without ever compromising on religious priorities and necessities over any other foreign religion. Indeed, in many Arab states, the crucifix as a symbol of Christianity is banned and illegal, and they make no excuses for it, because they are firm Muslims and this is embedded in the fabric of their government and culture. To further this example, it is also ridiculous that the Grand Cross of the National Order of the Legion of Honour which is the highest French order of merit for military and civil merits, established in 1802 by Napoleon Bonaparte, was given to the Sultan of Brunei in 1997, a man who recently instated a new penal code that applies the sharia – Islamic law – as strictly as possible: death by stoning to punish homosexuals and adultery, amputation of a hand or foot for thieves, death penalty for insulting the prophet. Being Jewish or Muslim will always portray oneself as a person with foreign values derived from the history and values of those religions that are for the most incompatible with those of Western European civilisation.
When people who have the ability to assimilate choose to do so, they should first find their place in the new society based on their choices, desires, skills, and abilities [for e.g. psychosocial and cultural synthesis]. Genuine efforts and desire of assimilation will be expected of them and this normally starts with a Western name of Christian culture. People who do not assimilate fully, rebuild and reshape themselves and adopt a completely new identity should always remember that they are not at home and should not expect the same treatment as those who are – this is a simple question of common sense. Those who assimilate properly will automatically become part of the native people and share an existence with similar opportunities, because they have become natives through their efforts and decision to be loyal and dedicated to their new society and its people, by respecting the founding heritage and religious sensibilities, and of course by mastering the behavioural and communicative patterns. This does not mean that after assimilating, they have to be subservient and cannot make a critical observation to help develop the country and push it forward, but their allegiance should be to the nation and the native people because they should consider themselves as part of that people. The objective after all is to create loyal citizens with a strong sense of concern for the society, not slaves! Natives too should learn to act like human beings and adopt the values of decency to understand that a society works better when the population is in harmony and happy while seeing genuinely and properly assimilated citizens as their own “blood”.
So as the Organic Theory explains, another factor is more fundamental than physical fitness for assimilation as we can see using Jews as an example to explain that similarity in skin tone is hardly anything except a tiny factor that helps with the majority who rarely think. The most important and defining part of assimilation concerns handling the appropriate behavioural and communicative patterns of the society that the organism wants to fully be a part of. For successful and complete assimilation, organisms need to also embed the philosophy, understand the heart of the people according to their history, master the language, feel at one with the nation, feel the joy and pain of the people and also be able to use the term “us” to describe themselves and the natives; in other words see the people as their own “blood”, and this is how it is done in the most sophisticated civilisation, i.e. France, where the people are willing to love you and see you as their own blood if you show the genuine desire to be part of the people and loyalty to the nation.
Assimilation unfortunately is not easily achieved and this is why assimilation should not to be confused with integration, because integration is simply the acquisition of a passport for legality; but assimilation is sculpting one’s heart and soul to be one with the people and be part of the national blood through loyalty and dedication while playing one’s part as a citizen with civic duties. Indeed, in Ancient Greece, all members of society who did not partake in communal matters or get involved and take interest in matters concerning the running of the country and the harmony of the people were seen as “parasites”, and this includes all citizens – natives and non-natives alike – because all societies need its people to work together to address its problems and follow the never-ending course of positive change for the betterment of a civilisation.
In France, most people understand that being a citizen is like a duty, and hence until today they are the only civilisation who stood up for the brotherhood of mankind as individuals to be treated with respect, they are among the rare civilisations who listen to the opinions of the people and give the praise of an emperor to a common man if they feel the man has the grandeur in his arguments and deserves so – we know this from the legend of Napoléon – and finally the French people are one of the most receptive people who are always willing to reason with new arguments in the noblest of ways no matter who the arguments are from. In fact, France is the least atavistic and most sophisticated civilisation of the modern world, and to achieve such a glorious task without a monarchy is amazing – it shows that when people see themselves as one and treat each other with respect while having a sense of moral and dignity, they embody an empire together, without or with an emperor – the head with a crown being simply an option if needed and deemed ingenious enough to guide a conquering civilisation, but not a necessity! To achieve this sense of harmony requires organisms that can find a strong sense of synchronisation as a people and see themselves as a nation and also feel each other’s pain and glory to reason as one. Of course, just like any society on earth, we do find some bad apples, and corrupt and immoral statesmen along with petty arguments, especially among the minor classes, but as a whole, it is a society that was built on values and philosophies devised to foster the development of human beings where any individual can rise to the very top through his or her own desire, efforts and dedication. The unfortunate thing is that as time passes, and the passionate generation who were part of the foundation of this new world dies, these values sometimes fade in the minds of the new generation and the mediocre “Fisher Price” statesmen it has given us and it is great men and women with admirable character that throughout history have had the courage to stand up, speak and remind the nation of the number of people who fought and lost their lives for the society we now have and the need to push in the same direction to continue on the route of human progress.
Being more French myself than German, I have to say that I believe in the superiority of the French language, heritage, values, people and industry over Germany and all other heritage. This does not mean that I do not respect or acknowledge Germany and other countries and their achievements, since skilled individuals in specific fields can appear from anywhere on the globe due to the amazing abilities of the biological technology that is the human brain, an organ that I have researched and studied for years. Germany has always been one of the great rivals of France, a rivalry that lasted centuries, long before Napoleon, being among the other vast empires with a universal outlook. Some German academics, such as Kant, Freud, Schopenhauer and Nietzsche have influenced others worldwide including French philosophy and psychology as can be seen in Jacques Lacan’s theory of mental life, just as others have influenced German thought, for example, Schopenhauer who after being introduced to Indian philosophy by Friedrich Majer, maintained a great interest in it and even meditated on the Upanishad, part of the Vedas (the sacred script of the Hindus) as an old man, to associate a fundamental part from it to his theory on the world of ideas; the Hindu concept of “Maya”, which defines the world as illusion, i.e. in the end subjects and objects were all “Maya” (illusion). Schopenhauer left Berlin when Prussia rebelled against Napoleon since he never developed strong German patriotic sentiments, regarding himself as a cosmopolitan without any national affiliation, and his adopted concept of subject, object and imaginary (illusion) is also found in Freud’s writings, and was later further developed by Jacques Lacan. Schopenhauer’s writings also aroused Nietzsche’s interest, whose writings were initially falsified by his sister, Elizabeth, to fit her own German nationalist ideology which was adopted by the Nazi regime. Nietzsche’s true philosophy was explicitly opposed to antisemitism and nationalism since he promoted a more global and individual perspective; fortunately, revised editions were released after 20th century scholars contested this incorrect interpretation of his work. Hence, some individual intellectuals from German institutions contributed to modern philosophy and Western European thought; so we find some respect and cooperation in some academic fields that benefit all societies and economies, but we cannot ignore the fact that there is also tough and intense competition with France and other countries on a range of industries, for example, the scientific, medical, transportation and technological industries.
Presentation: Napoleon crushes Prussia: Jena, 1806
But from the perspective of a product of France and its intellectual and linguistic heritage with an undeniable British influence, I would never have complied with Hitler’s vision of a German empire ruling the world with all languages being extinguished gradually for a complete German speaking world, hence I would rather see a French speaking world. The French empire also has the sophistication and the flexibility to accommodate all foreign heritage [what is worthy of keeping] without destroying or burning them, by simply translating foreign heritage so that it now becomes part of the repertoire of skills of the French empire. Hence France, does not destroy the heritage of other cultures, but absorbs what is valuable from it [e. g. gastronomy, technology, industries, philosophy, arts, other beneficial practices, etc], share it with the francophone family and make it a part of its own blood in its constant evolution. So, I would rather see the world turn French as the empire absorbs and adopts the whole of mankind as a mother would in her arms in a harmonious, humane, sophisticated and strategic way instead of German.
So now to finish off, having already spoken of what I thought was not well planned in Hitler’s regime, along with a fairly deep explanation of the Organic Theory and assimilation, here are the couple of things that are inspiring with Hitler’s story, and it starts with the great example the German people set at the time in terms of giving power to the deserving individual by showing the world that a failed artist could rise to the very top of a modern society. Which means that we eventually saw a financially challenged boy who was the top of his class in primary school who then failed to kickstart his artistic career after failing an exam to one of the finest art school in Western Europe, the Academy of Fine Arts in Vienna, and then through his own efforts after being homeless and struggling through the war, rise to the very top. This to me shows absolute social mobility, but also how a man can be an artist, a soldier, and a cultivated man through his own efforts to then lead a modern civilisation and rise to the very top. This to me is a clear modern example of the Organic Theory on the process of self-definition and progressive development of an individual organism based on his/her own desires and abilities.
The second amazingly inspiring side to the story of Hitler is how he gave the world an avant-garde example of the answer to a harmonious environment; by being a vegetarian who was the first to initiate animal protection laws.
The third admirable side to Hitler was his charisma and his loyalty to his society, but also his modesty and confidence with people of all walks of life, being the only public figure of his level to freely walk around his country and meet the crowd from all walks of life and classes without any protection, while also gaining their absolute trust to guide them.
The fourth side to Adolf Hitler was that he had style in his taste in architecture for his country as we can today find through the blueprints he devised along with Albert Speer. We can imagine what would have been the future Germany and Berlin. These plans reveal buildings and plans of a city that reflected the grandeur of mankind and even the uniforms of his staff were contracted to Hugo Boss – showing a man who revered perfection. And if we take a look at the uniforms and the suits of the National Socialist government, we may have to accept that they were some of the sharpest and best-looking suits ever seen throughout modern history, perhaps only matched by French couturiers such as Yves Saint Laurent.

Adolf’s Agenda
The fifth amazing side with Hitler was his love for science and evolution and his passion to keep an updated perspective of all the latest discoveries. So, it would be fairly biased to assume Hitler to be a rigid man who had no taste for change. This can be reflected is his eagerness to foster research in order to rebuild Germany’s medical, technological and military facilities. This also adds to my view that Hitler would have been willing to listen to new discoveries and shift his opinions accordingly if advised and convinced by genuine, avant-garde and honest people – he should have consulted me. Haha! But of course, the close entourage of the Fuhrer was not particularly composed of the most ethical of minds or the most sophisticated where many turned out to be disloyal and evil, which likely led to the horrors of the regime without any link to Hitler himself.
The sixth admirable thing about Hitler, is the fact that he was a leader who really saw people as organisms requiring the similar chances to succeed and rise and not as a crowd to be divided into segments of left, right and centre. Hitler saw all his citizens as people of his system and worked to synchronise the whole society to work as one machine. This is certainly admirable in comparison to the corrupt and immoral people at the head of most systems today where the criteria used to govern human beings are economic and business factors. To run a civilisation of human beings without values, philosophy and morals is a sure way to fail in the long run because human beings are not objects or goods, but are complex organisms that require a very sensible system to live harmoniously, and any person who calls himself a leader and does not understand psychology, philosophy and the elements that lead to a modern harmonious human environment are fooling themselves and lying to society. It is also to be remembered how Hitler even proposed to dismantle the German military and destroy all weapons if all other countries did the same, which they never responded to. So, we now understand why Hitler was even paraded as person of the year by Time magazine, and it could not possibly be for turning Jews into minced meat. And the other enigmatic question is why so much today is being spent on defence and military when it is clear that we are a lonely civilisation on a lonely planet that should be looking to extend its reach by starting a new civilisation on a backup planet to gain the status of a space civilisation? Do these parties spending so much on military equipment and technology only have defence and nothing else in the back of their perhaps unconscious minds? Is it simply for decoration?
The seventh inspiring thing about Hitler is that he was not a native German, but just like me, fully assimilated in German society and to also win the heart of a whole nation and rise to the very top and eventually become more Germans that the Germans themselves, is something quite spectacular. Perhaps, another admirable thing was Hitler’s reply in a court proceeding after his failed coup against the state to take power, where he responded after being asked if he was German by asking whether this is proved on a piece of paper or in a man’s heart; because although he had already won the heart of the nation, he still did not have a German passport. In his early years in Germany as he struggled financially and was homeless, he was also told by some Germans that he looked like a Jew and that they thought he was one, to then overcome all this to rise to the top is quite frankly admirable.
The eighth inspiring side to Hitler was his unique ability to open his heart completely to the nation and deliver shattering speeches that hypnotised the crowds, with his passionate body language that portrayed his honesty and dedication to the Germans by placing them before his own comfort.
The ninth, and final point that I believe is inspiring with Hitler is that he did not seem to have seen things from the perspective of the regular average exec, economist, banker, doctor or other financially motivated executive who tend to claw their way in a political party just to appear on television or newspaper without any presence, greater vision or strong values and see a civilisation as a store to manage. Hitler had a deeper view like legendary emperors had, and wanted to guide a nation with philosophy, inspiring architecture, timeless artworks and wanted to blend and synchronise all the departments ranging from business, economy, education, science, research, history and arts to create the kind of timeless civilisation as it is often depicted in mythological literature that stands the test of time in marble and stone. Most importantly, Hitler seemed to be of the opinion that if a civilisation is not expanding then it is not progressing and this reflected the qualities of a conqueror, reminiscing of those like Alexander the great or Napoleon. Nowadays, pathetic and mediocre execs who lead a team that they call a political party are guided by the sole desire to stay in power, and because of their allegiance to donors to their parties, they need to abide and meet some demands to remain funded, this destroys a civilisation because it is not being managed with the freedom and the values that it requires, and hence, this leads to a mundane atmosphere of a static and boring society where the same kind of men act and speak in a noble way public, but behave like ignoble and immoral characters in their decision and management – this has been a depressing and repetitive cycle for decades now without any legendary character appearing to stand against such absurdity and turn matters around. Today, with so many conventions, it is hardly possible for any great empire to take matters into their own hands and consider expansion and conquest because of hypocritical beliefs of absolute equality of all societies and languages along with third world policies that have trapped great empires of the West such as France into submission and onto its knees to comply with irrational, ridiculous and hypocritical demands that bound it to comply with conventions and gradually has today transformed it and many other empires into nurseries paralysed by the demands of inferior societies, when it has all the resources to turn the whole world into its colonies and manage it better while giving all the people on Earth the dream of being part of its heritage, like great empires once did.
It is also fair to note that during World War II, all sides committed atrocities on innocent civilians, both the Allies and the Germans, so today, when we look back at the greatest war of men of the 20th century, we realise that not a single party can proclaim to be angels because many atrocities comitted by the Allies were ignored until recently revised; such as the Katyn massacre comitted by Stalin which was wrongly attributed to the German Reich, not to mention the horrific amount of rapes comitted on innocent women from all parties in Occupied Germany from 1944 to 1954 [English: 45,000 rapes, French: 50,000 rapes, American: 190,000 rapes and Soviet: 430,000 rapes]. We must also not forget the rapes during the liberation of France both during and after the advance of the United States armed forces through France. According to the American historian Robert Lilly, there were 3,500 rapes committed by American soldiers in France between June 1944 and the end of the war. The number of rapes is difficult to establish because many rape victims have never reported the facts to the police. The American troops involved committed 208 rapes and about 30 murders in the department of Manche. In June 1944 alone, in Normandy, 175 American soldiers were accused of rape [See: Viols durant la libération de la France]. Due to the large number of reported cases of rape and the deterioration of the image of American soldiers in France, the American command judged 68 cases of ordinary rape involving 75 victims between 14 June 1944 and 19 June 1945; at least 50% of the rapist soldiers were drunk at the time of their crime; of the 152 accused, 139 were black, although they made up only 10% of the troops on the European theatre [Read the article: À l’automne 1944, Français et troupes américaines au bord de l’affrontement]

Company of Allied Rapists: Estimated no. of rapes from 1944 – 1954 in Occupied Germany by the Allies / See: The Real Genocide of the German people during World War 2
Hitler’s Shadow: In The Service Of The Führer [This is the personal story of Karl Wilhelm Krause, who was the valet. of the Fuehrer from 1934 to 1939, and was also responsible for his personal safety and security. Through his daily contact with Adolf Hitler, and those of his most intimate circle, both in his public life, as well as, inside the Fuehrer’s private quarters, no one had access like Herr Krause.]
So, to conclude with an answer to your question, I am neither a Hitler fan, nor a Hitler hater, but a man who sees “The Fuhrer” as one of the great figures of the last century with elements to be inspired by and mistakes to also learn from. A silent, yet growing movement of modern Aryans are beginning to re-evaluate the ideologies of the Fuhrer with a recent exposition at Montpellier showcasing 200 photographs from his photographer Heinrich Hoffman.
Finally, I would like to point out that if nobody speaks, nothing changes… so I chose to speak, what did you choose to do?
_________________________________
QUESTION VII.
[FR] – Qui est votre leader préféré de tous les temps et pourquoi ?
[EN] – Who is your all-time favourite leader and why?
[FR] Réponse:
Après avoir beaucoup réfléchi et éliminé d’une liste constituée de Chirac, Sarkozy, Hitler, De Gaulle, Alexandre le Grand et Napoléon Bonaparte, j’ai dû aller avec ce dernier, l’Empereur du peuple français, car il s’avère être un des chefs les plus énigmatiques jamais vu dans l’histoire des hommes. Je crois que l’humanité n’a pas eu de dirigeants de ce calibre depuis. Nous avons eu surtout des cadres médiocres qui ont dirigé des partis politiques et ont joué avec la civilisation jusqu’à ce que leur temps passe, tout en faisant le maximum pour assurer une retraite financièrement confortable et assez de photos encadrées avec des célébrités pour les accrocher à leurs murs.
Avant d’en arriver à Napoléon, je dois dire qu’il y a quelques personnalités publiques assez décentes qui avaient des éléments à leur sujet que je trouve inspirants. Nous avons l’ancien président français Chirac, qui, je crois, avait une personnalité incroyablement charismatique et magnétique, qui incarnait également la joie de vivre française et qui avait une touche de jeunesse éternelle dans son caractère, et cette touche d’humanité est admirable car je crois que être humain est un facteur fondamental pour gérer les autres humains. Chirac aimait la foule et était à l’aise avec les gens de tous les milieux tout en ayant un grand sens de l’humour.
Un autre président français que je trouve également inspirant est Nicola Sarkozy, qui est aussi un grand exemple d’assimilation et quelqu’un qui a également rencontré de nombreux obstacles dans ses premières années en tant que fils de Hongrois et petit-fils d’un Juif mais qui a finalement tout surmonté pour se prouver comme un vrai français qui avait la France dans son cœur. Sarkozy est aussi celui qui inspire les autres à monter, contrairement à beaucoup de personnalités égoïstes d’aujourd’hui qui, une fois au sein d’un parti, semblent haïr les jeunes générations et agissent en animaux vils et frustrés envers les personnalités de demain.
Hitler aussi a été un cas de grande assimilation et après avoir parlé de ce que je trouve inspirant à son sujet ci-dessus, je pense que nous pouvons passer au dernier, qui est Charles de Gaulle.

Ce dernier, pour moi, est un grand exemple d’un homme qui savait ce qu’il voulait et qui avait la grande vision d’une civilisation. De Gaulle faisait aussi preuve d’une modestie exemplaire et ne se noyait pas égoïstement dans le luxe mais pensait à l’Etat et au peuple avant son propre confort. De Gaulle a également joué un rôle essentiel dans la libération de la France, et il a tout fait depuis l’Angleterre sans être présent sur le sol français, étant le premier à montrer comment la technologie du XXe siècle pouvait être utilisée pour gérer, organiser et motiver tout un empire. L’autre chose admirable de Gaulle, c’est qu’il avait gagné la confiance de la France pour diriger librement comme un monarque et est peut-être aujourd’hui connu comme le dernier “roi démocratique de France”.
Le dernier avant Napoléon est Alexandre le Grand, qui fut la seule personne d’origine indo-européenne à avoir presque conquis le monde, de la Grèce au fleuve Indus. C’était un général et un explorateur qui était aussi incroyablement cultivé de ses enseignements par le grand Aristote qui lui avait enseigné la science, la philosophie, la littérature et les techniques de combat – toutes les compétences nécessaires pour un futur grand leader.

Image: Aristote instruisant Alexandre / Alexandre le Grand (2011) . Arte
Dès ses premières années, il a enduré un père incroyablement exigeant qui s’attendait à ce qu’il ne soit jamais faible et qu’il soit le plus grand dans tous les domaines. Alexandre était assoiffé de connaissances et était inspiré par le modèle grec et voulait être le meilleur comme Achille, le héros légendaire de la mythologie grecque à qui son père avait dit que pour se comporter comme un homme, il devait être le meilleur et avoir un meilleur jugement.

Après avoir été enseigné par Aristote pendant 3 ans, Alexandre dira plus tard qu’il aimait Aristote comme un père et si son père biologique lui a donné la vie, c’est Aristote qui lui a montré comment vivre. Ce dernier lui raconta comment l’empire perse s’est étendu jusqu’à la fin du monde jusqu’en Inde, et comment leur roi avait envahi la Grèce il y a environ 100 ans, détruisant toutes les villes, prenant Athènes et brûlant l’Acropole avant que les Grecs puissent s’unir et chasser les Perses. Aristote avait également dit à Alexandre comment les Perses étaient une menace permanente avec leurs troupes amassées aux portes de la Grèce avec le tombeau du valeureux Achille encore dans leurs mains, et que le rêve de gloire éternelle réside dans l’acte d’unir les Grecs et de poursuivre les troupes persanes comme ce serait l’acte d’un héros. Son père lui avait dit qu’il devait trouver un empire à sa taille car la Grèce est trop petite.

Image: Alexandre le Grand (2011) . Arte
Après avoir commencé à conquérir la Perse, il vainquit l’armée de Darius III, bien qu’en infériorité numérique, et fit prisonniers la mère, l’épouse et les sœurs. Dans un acte de chevalerie, il leur promettait même qu’elles seraient traitées avec respect et qu’aucun de ses hommes ne serait impuni s’ils manquaient de respect aux femmes persanes, à la colère et à la frustration d’un de ses généraux les plus proches et les plus doués, Philotas. Il dira à ce dernier qu’après leur bravoure et leur victoire héroïque contre l’armée persane, comment pourraient-ils se comporter en lâches avec leurs femmes ? Alexandre a continué son exploration et a presque pris le monde avec de nombreuses villes, y compris Babylone le recevant comme un libérateur – il voulait surpasser ses ancêtres. Mais l’une de ses déclarations les plus nobles fut peut-être son désir d’avoir été Diogène de Sinope s’il n’avait pas été Alexandre. Diogène de Sinope était l’un des philosophes les plus célèbres de l’école de philosophie cynique dont le caractère a profondément marqué les Athéniens à travers une multitude d’anecdotes légendaires. Cela montre qu’au fond de son cœur, Alexandre n’était pas motivé par le luxe ou l’argent, mais voulait vraiment construire une civilisation noble de gens sophistiqués et humains. Cela montre aussi sa sensibilité et sa capacité à établir des relations avec les gens modestes, mais surtout sa sagesse dans l’évaluation de la grandeur d’un homme, non pas en fonction de ses possessions ou de ses vêtements, mais uniquement en fonction de son intelligence et du contenu de son discours; parce que Diogène de Sinope vivait dehors, dans la misère, vêtu d’un simple manteau, avec un bâton, un sac et un bol. Dénonçant l’artifice des conventions sociales, Diogène prônait une vie simple, plus proche de la nature, et se contentait d’un grand pot couché sur le côté pour dormir.

Diogène (Diogenes) par John William Waterhouse, 1882
Diogène avait l’art de l’invective et de la parole mordante. Il semble qu’il n’ait pas hésité à critiquer ouvertement les grands hommes et autres philosophes de son temps (dont Platon). Les apostrophes les plus célèbres qui lui sont attribuées sont :
«Je fus un jour chez un adolescent d’une richesse considérable. On m’installe dans une salle à manger ornée de toute part de peintures et de dorures au point qu’il n’y avait même pas un endroit pour cracher. Comme une glaire me montait à la gorge, je l’expectorai et promenant les yeux autour de moi sans trouver un endroit où cracher, je crachai sur le jeune homme lui-même. Il m’en fit le reproche. A quoi je répondis en l’appelant par son nom: ‘Quoi, tu me reproche ce qui vient de se passer, et tu ne le reproche pas à toi qui a fait décorer les murs et le pavée de ta salle à manger et n’as laissé sans décoration que ta personne, invitant par là à cracher dessus’.» -Diogène
«Les autres chiens mordent leurs ennemis, tandis que moi je mords mes amis, de manière à les sauver.» -Diogène
«Je suis à la recherche d’un homme» – (c’est-à-dire un homme vrai, bon et sage), une phrase qu’il prononçait à la stupéfaction de ses concitoyens en marchant dans les rues, brandissant sa lanterne allumée en plein jour et approchant les visages des passants.
(réponse éblouissante à Alexandre le Grand, roi de Macédoine, qui était venu le voir pour lui demander s’il avait besoin de quelque chose, s’il pouvait l’aider d’une manière ou d’une autre…). – Oui, sortez de mon soleil, répondit Diogène.
Plusieurs anecdotes témoignent du mépris de Diogène pour la richesse et les conventions sociales. Selon Diogène Laërce, il n’a pas hésité à mendier avec les statues pour «s’habituer au refus». Il a abandonné son bol après avoir vu un enfant boire à la fontaine dans ses mains. Interrogé sur la façon d’éviter la tentation de la chair, Diogène aurait répondu “en se masturbant”, et aurait ajouté : «Il vaudrait mieux pour le ciel qu’il suffise aussi de se frotter le ventre pour ne plus avoir faim». Diogène aurait également été vu se promenant dans les rues d’Athènes en plein jour, avec une lanterne à la main, disant à ceux qui lui demandaient ce qu’il faisait : «Je cherche un homme.» (parfois traduit par «je cherche l’homme» ou «je cherche un vrai homme»). Cet «homme» désignerait celui théorisé par Platon, l’idéal de l’être humain, et Diogène aurait voulu réfuter son existence, puisque seuls des hommes concrets existent. Une autre anecdote rapporte que, Platon ayant défini l’homme comme un «bipède sans cornes et sans plumes», le lendemain Diogène se promenait dans la ville, tenant dans sa main un coq déplumé avec des ergots coupés, et déclarant : «C’est l’homme de Platon !» Diogène a d’abord vécu comme un homme libre, mais comme il se dirigeait vers Égine par bateau, ce dernier avait été pris par des pirates. Mis en vente comme esclave à Corinthe, il déclara au marchand qui lui demandait ce qu’il pouvait faire qu’il savait «gouverner les hommes», et qu’il devait donc être vendu à celui qui cherchait un maître. Il finit par être acheté par un riche Corinthien qui admirait son indépendance d’esprit, et qui lui donna sa liberté.

La rencontre d’Alexandre le grand et de Diogène de Sinope / Pierre Pujet, vers 1680, Musée du Louvre
C’est à Corinthe, où Diogène vivait lorsqu’il n’était pas à Athènes, que s’est déroulée la célèbre rencontre du vieux clochard philosophe avec le jeune roi de Macédoine, Alexandre le Grand. Cet épisode est raconté en particulier par Plutarque dans la Vie d’Alexandre, XVIII, par Cicéron dans les Tosculans, 5, XXXII, et par Diogène Laertius dans la Vie des philosophes, Livre VI.
Voici la version la plus complète de leur conversation :
– Demande-moi ce que tu veux, je te le donnerai.
– Sors de mon soleil (littéralement : “Reste loin de mon soleil pendant un moment.”)
– Tu n’as pas peur de moi ?
– Qu’est-ce que tu es ?……… Un bon ou un mauvais ?
– Un bon, un bon.
– Qui pourrait craindre le bien ?
Diogène avait demandé qu’après sa mort, son corps soit jeté dans la rue, mais ses amis lui ont donné des funérailles honorables. Une colonne surmontée d’un chien de marbre a été placée sur sa tombe et sur laquelle les versets suivants ont été écrits :
“Même le bronze subit le vieillissement du temps,
Mais votre renommée, Diogène, l’éternité ne la détruira pas.
Car vous seul avez montré aux mortels la gloire d’une vie indépendante
Et le chemin le plus facile à suivre pour une vie heureuse.”

Traduction(EN): “The world suffers from not having enough beggars to remind men of the gentleness of a fraternal gesture.” -Marcel Aymé
Aujourd’hui, l’héritage d’Alexandre le Grand est présent en politique aux côtés des légendes et dans la littérature. Il envisageait un empire universel où les sociétés auraient une administration autonome et pourraient coexister pacifiquement sous un gouvernement impérial. Alexandre n’a pas seulement conquis le monde, il a changé le cours de son histoire pour toujours.
Mais mon chef préféré de tous les temps est Napoléon. Napoléon pour sa grandeur en presque tout et sa présence motivante et inspirante qui a touché des hommes et des femmes du monde entier. Napoléon est quelqu’un à qui je semble me lier parce qu’il est peut-être l’une des plus grandes histoires d’assimilation étonnante et qu’il est passé d’un simple militaire à général, ensuite consul pour terminer comme empereur et tout cela avec à la reconnaissance du pays tout entier. Napoléon est un homme et un enfant de la Révolution et de la Première République et en est le plus célèbre héritier; c’était un Républicain et n’avait rien à voir avec l’Ancien Régime fait de castes et d’inégalités.

Image: Bonaparte au pond d’Arcole (1796) par Antoine-Jean Gros (1771 – 1835)
Napoléon m’inspire parce que, comme moi, il n’est pas né en France, mais a quitté sa maison en Corse et est parti étudier en France. Dans ses premières années, il ne maîtrisait même pas la langue française et avait un fort accent corse, et il a également été intimidé au collège alors qu’il était à Brienne, une académie d’élite et a été traité comme un petit immigrant étranger dans ces premières années. Pourtant, avec un tel dévouement, en tant qu’étudiant déjà étonnant et grand autodidacte solitaire, il a lu tous les grands esprits de l’Europe, s’est cultivé et est devenu l’un des plus grands Français à avoir jamais vécu. En effet, du petit étranger à l’accent louche, devenir alors plus français que les Français, et s’élever au rang d’Empereur est vraiment inspirant.

Traduction(EN): “I accept this title that you believe is useful to the glory of the nation… The life of a citizen belongs to his motherland, the French people want mine to be fully devoted to them, I obey their desire.” -Napoleon
Avant de recevoir sa couronne le jour de son couronnement après que le peuple français eut décidé de le faire empereur de la République française, il se retourna et regarda son frère en disant, en corse “sì u nostru babbu ci hà vistu”, qui signifie “si notre père pouvait nous voir”. Cela montre que bien qu’il ait incarné la France dans son cœur, il était respectueux de son humble passé alors qu’il est passé de simple lieutenant à empereur en seulement 11 ans.

Source: Napoleon: La Conquête du Pouvoir, Les Grandes Réformes & Les Grandes Victoires (Cliquez pour regarder le documentaire)
Les exploits de Napoléon ont aussi inspiré les grands écrivains du courant Romantique, et surtout un des plus grands génies de l’écriture qu’était Honoré de Balzac. Lui qui comme Napoléon avait un côté mathématique dans l’organisation de tout ses œuvres, notamment une des plus fondamentale, «La Comédie Humaine» qui est divisé en trois parties: Études de Mœurs, Études Philosophiques et Études Analytiques. La Comédie Humaine montre que toute l’existence peut être interprétée avec tous les éléments du théâtre puisque le rôle que l’on joue dans la société et le rôle dans lequel un certains nombres d’acteurs différents pourront se succéder. Dans la nouvelle formant partie des études philosophique, «Adieu», nous voyons un épisode sur la retraite de Russie des troupes impériales Napoléoniennes en 1812 lors du passage de la Bérézina. Napoléon était un personnage mythique que Balzac voulait rivaliser avec dans son domaine, puisqu’il le voyait comme un génie qui nous avait montré l’avenir impérial mais qui avait aussi réussi a sauver les nobles de la terreur et trouver un moyen pour synchroniser harmonieusement la France toute entière en instaurant un système de progression par l’effort et la méritocratie [créant L’ordre national de la Légion d’honneur en 1802] pour tous après la pagaille, l’instabilité et la confusion qu’avait laissé la terreur juste après la révolution.

Image: Croix d’Officier de la Légion d’Honneur (1806-1808) / “Au nom du peuple français,
BONAPARTE, premier Consul, proclame loi de la République le décret suivant, rendu par le Corps législatif, le 29 Floréal an X, conformément à la proposition faite par le gouvernement, le 25 du dit mois, communiquée au Tribunat le 27 suivant. DÉCRET.
TITRE PREMIER. Création et organisation de la Légion-d’Honneur.
Art. 1er. En exécution de l’article 87 de la constitution, concernant les récompenses militaires, et pour récompenser aussi les services et les vertus civiles, il sera formé une Légion d’Honneur…” / Source: La légion d’Honneur : ordre impérial, royal et national. La fondation
L’Ordre de la Légion d’honneur créé par Napoléon pour récompenser les services rendus à la Nation était un insigne avec sa propre figure qu’il épinglait sur la poitrine de ses sujets, ce qui était un signe très fort puisque les souverains d’Europe avaient plutôt les fondateurs de leur dynastie ou le symbole de leur pays, mais Napoléon, en tant qu’homme qui détruisit l’ancien régime, épingla son propre profil sur la poitrine de ses sujets avec l’aigle impérial au revers de l’insigne, ce qui était unique et universel comme Anne de Chefdebien l’a souligné, car ici le tambour et le prince recevaient la même décoration, l’intellectuel et le soldat qui ne pouvaient lire aussi ; c’était égalitaire, universel et très fort parce que tous ceux qui ont servi la Nation de tout leur cœur ont eu la même récompense, c’est exceptionnel parce qu’avant la révolution tous les pays y compris la France avaient plusieurs ordres qui la plupart du temps exigeaient des conditions de naissance. Napoléon avait aussi l’audace et le courage de vouloir unifier toute l’Europe sous le drapeau Français et ses valeurs sans intermédiaire, pour étendre les idées et acquis de la Révolution à tous les autres peuples d’Europe plongés eux aussi dans l’obscurantisme depuis des siècles par une caste minoritaire dirigeante qui se nomme elle-même “Noblesse”. Avec la République et l’Empire désormais tout le monde peut enfin – après tant de siècles – à travers ses qualités accéder à l’ascenseur sociale. L’Empire avait été créé par le peuple pour lutter contre les attaques incessantes contre la France [seule représentante en ce temps de l’Europe des Peuples] par la vieille et sclérosée Europe des Rois unie pour rétablir l’Ancien Régime et détruire les acquis de la révolution: la liberté et l’égalité des chances pour tous. L’Empire était surtout pour éloigner toujours plus loin le danger de ces incessantes attaques des frontières de la France et de calmer les velléités des rois et empereurs de l’Ancien Régime rétrograde et non progressif, car en ces temps la diplomatie n’existait que sous cette forme sauvage et l’on ne pouvait obtenir la paix que par elle [ce que voulait en premier la France et Napoléon I qui ont TOUJOURS été forcé à faire la guerre face aux attaques des rois, contrairement à ce qu’une perfide propagande veut faire croire depuis 200 ans] : “La diplomatie des canons”, seule diplomatie existante en ces temps agités et barbares tout simplement.
Le jour où Napoléon a mis la Prusse à genoux

Des soldats napoléoniens lors de la reconstitution d’une bataille / (illustration)Crédit : CESAR MANSO / AFP / Source: RTL (Russie : le corps d’un général de Napoléon identifié 207 ans après sa mort)
En étudiant «Adieu», nous voyons que Balzac pensait que l’erreur principale de Napoléon était d’avoir mal planifié et lancé ses troupes en Russie, un pays que Balzac associa à la froideur de la neige et peignit littérairement comme une vision d’un enfer blanc: un pays de blancheur, de froid et de châtiment qui signifiait la fin du monde. Donc, pour Balzac la retraite de Russie était bouleversante pour la France, et c’est un événement qu’il voulait décrire comme une perspective de l’histoire qui se dirige vers un enfer froid, entre autres, ce qui risque d’arriver à notre société si nous baissons notre garde. La rivière Bérézina que devront traverser les troupes pour survivre dans «Adieu» devient la figure du déluge biblique et pour la traverser Balzac semblait insinuer qu’on devrait construire une arche de Noé qui était représentée par un radeau dans le récit, et Michel Butor a fait valoir qu’il semble suggérer que si nous ne sommes pas en mesure de mener des travaux de recherche et d’invention, alors la société perdra la générosité de la noblesse et la chaleur du cœur ancien et deviendra un lieu où les hommes se fragmentent.
Napoléon était aussi un exemple parfait de la théorie organique dans la création, le développement, l’évolution et la définition de soi dans une société sophistiquée qui croit en la force créatrice de l’individu pour réaliser ses rêves. C’est aussi tout l’oeuvre de Balzac, le thème de l’homme seul abandonné par presque tout où l’homme recommence et réécrit l’histoire du monde; Michel Butor l’a bien souligné: l’homme de génie est celui pour qui la terre se fait île déserte, parce que tout s’écarte de lui. Sa présence en tant que chef était unique et légendaire, ce qui a conduit le Maréchal Bon-Adrien Jeannot de Moncey après sa mort de dire: “Maintenant rentrons mourir!” Napoléon était un homme qui personnifiait le courage, tant sur le champ de bataille que dans les affaires officielles de l’État qui était guidé par des valeurs et non par l’argent, entièrement dévoué à la France, il plaçait le peuple et la grandeur de sa nation avant sa propre santé et son confort. Dans la mémoire de Sainte-Helène, Napoléon avait même prédit l’opposition future entre les États-Unis et l’Empire Russe, mais avait aussi essayé de faire comprendre à l’opinion que les coalitions qui se sont acharnées sur la France étaient des coalitions politiques et non pas militaires, qui cherchaient à abattre la République Française et ses valeurs et non pas l’Empereur.

Traduction (EN): “When he has made a mistake or been a victim of misfortune, the man of genius always manages to recover.” -Napoleon
En plus d’être un génie militaire et politique, il prouva qu’un homme pouvait être un intellectuel, un soldat, un grand bâtisseur tout en étant amoureux des arts et de la musique. L’empereur avait aussi un sens de la dignité et des valeurs et voulait permettre aux gens de toutes les classes en France de croire en la capacité de grandir et de s’élever par leurs propres efforts – il voulait que tous les membres de sa société puissent rêver. Pour Napoléon, l’impossible n’était pas français !

Traduction(EN): “We have a master. Napoleon Bonaparte does everything. He can do everything. He wants everything.” – Abbé Siéyès
Jean-Marie Rouart l’a aussi souligné, qu’il y a une religion Napoléonienne, un culte de Napoléon parce que les gens du peuple ont compris qu’a travers cet homme, ils sont tous devenus plus grands, et ce mythe Napoléonien parlera toujours parce que personne dans l’époque moderne n’a pu atteindre à ce point ses rêves; mais il y a aussi une leçon morale qui est une leçon d’espérance et si Napoléon est toujours présent c’est parce qu’il y aura toujours des gens pour aller se ressourcer dans son exemple, dans ses mots, dans le mémorial de Sainte-Hélène pour trouver dans la vie de Napoléon, un moment ou vraiment ils reprennent de l’optimisme, et donc c’est une leçon d’optimisme puisqu’il a ramené la politique à l’homme pour prouver qu’un homme peut être exceptionnel! Chateaubriand semble avoir bien décrit Napoléon comme “le plus puissant souffle de vie qui jamais anima l’argile humaine”.
Napoléon avait une vision instinctive de ce que devait être un pays moderne et fit des réformes d’une ampleur extraordinaire dans les domaines juridique, politique et économique pour les droits et les devoirs des citoyens afin de rendre fonctionnel la société d’après la révolution. Le Code civil, devenu plus tard le Code Napoléonien a aussi été écrit par lui, et il a influencé des pays du monde entier en donnant à la société française une structure nécessaire pour l’ordre et la sécurité après la révolution et la terreur. De nombreux autres pays se sont inspirés du code napoléonien et l’ont utilisé pour moderniser la vie dans leurs sociétés.

Traduction(EN): “To make the republic dear to the citizens, respectable to foreigners and formidable to enemies.” -Napoleon
Napoléon croyait que tout devait être reconstruit sur des bases saines et c’est pourquoi il restera à jamais dans l’histoire de l’Europe comme une figure fondamentale de la conquête militaire et en essayant d’imposer un nouveau système[un Etat moderne, une nouvelle administration, un nouveau gouvernement central, une nouvelle législation et une nouvelle jurisprudence] qui avait créé un héritage rendant impossible un retour a l’ancien régime dans tous les territoires occupés par ses troupes ou influencé par ses idées.

Le Code Civil ou Code Napoléonien a inspiré et aidé des sociétés du monde entier a trouver leur structure et leurs valeurs / Source: Toute L’Histoire (2011)
Après avoir été accueilli en héros et en sauveur de la République par une foule extatique, en seulement 3 mois au pouvoir en France, Napoléon avait instauré la paix civile, créé de nouvelles institutions et réformé le système fiscal, ce qui avait conduit à un redressement spectaculaire des finances publiques sous la direction du consulat. Il n’a pas seulement attaqué les institutions, il a aussi pris la responsabilité de moderniser et d’agrandir les infrastructures du pays [nouveaux navires construits, ports et arsenaux agrandis et modernisés]. Dans l’éducation, on a vu la naissance des lycées et une réforme profonde de l’enseignement et de l’université. Dans le secteur industriel, il a créé la chambre de commerce, modernisé le service postal avec de nouvelles lignes télégraphiques optiques qui relient les 29 grandes villes et créé et amélioré près de 50 000 km de routes avec des œuvres d’art et des ponts réalisés partout. Comme l’a expliqué Charles-Maurice de Talleyrand-Périgord, l’empire a créé une vraie dynamique des peuples, et a apporté un grand nombre d’avancés tant humaines qu’institutionnelles, les conquêtes Napoléoniennes en bouleversant les ordres établis, ont jetés les bases de nombreux changements étatiques qui ont servies a beaucoup d’autres pays pour accéder a leur unité ou indépendance; la vision du grand empire de Napoléon était unificatrice et avant tout une vision européenne universelle dépouillée de son caractère autoritaire ou elle apparaît résolument moderne, méthodiquement organisée; et n’avait rien à voir avec les vieux mouvements xénophobes nationalistes et racistes qui se font appeler “identitaires” de nos jours et qui encouragent le renfermement sur soi, la division, le communautarisme et la haine envers les autres et une Europe unie sous le drapeau Français que rêvait tant Napoléon. Ces anciens mouvements nationalistes non progressif, statique et atavique salissent l’héritage de Napoléon.

Image: « Le Premier Consul franchissant les Alpes au col du Grand Saint-Bernard » par Jacques-Louis David (1801)
L’empereur avait donc la grande vision d’étendre la France, sa langue et ses valeurs et semblait suivre les traces d’Alexandre le Grand comme un conquérant qui était à deux doigts de conquérir toute l’Europe. Napoléon était pour moi le vrai chef des hommes et pouvait les motiver avec son honnêteté ancrée dans ses discours électrisants et il était aussi quelqu’un qui avait les qualités d’un conquérant et qui croyait qu’un empire avait besoin d’expansion pour progresser. Je pense que Napoléon Bonaparte est l’exemple de la grandeur de la civilisation française et aussi la preuve que la France est la civilisation qui incarne la grandeur de l’humanité, ses rêves et les valeurs de méritocratie et d’excellence. “Napoléon grandira, à mesure qu’on le connaîtra mieux!”, disait Johann Wolfgang von Goethe.

“La Grande Armée” par Richard Grégoire / BO Napoléon (2003)

Traduction(EN): “”I found a crown in the stream, wiped off the mud that covered it, put it on my head.” -Napoleon
—-|—-
[EN] Answer to Question VII. “Who is your all-time favourite leader and why?”
After a great amount of thinking and eliminating from a list constituted of Chirac, Sarkozy, Hitler, De Gaulle, Alexander the Great and Napoléon Bonaparte, I had to go with the latter, the Emperor of the French people because he turns out to be one of the most enigmatic leaders ever seen throughout the history of mankind. I believe that humanity has not had leaders of this calibre since. We have had mostly mediocre execs who became the head of political parties and played around with civilisation until their time passed while making the most to ensure a financially comfortable retirement and enough framed photographs with celebrities to hang on their walls.
Before getting to Napoleon, I have to say that there are somehow a couple of fairly decent public figures that had some elements about them that I find inspiring. We have the former French president Chirac, who I believe had an incredibly charismatic and magnetic personality who also embodied the French “joie de vivre” and had a touch of an eternal youth about his character, and this touch of humanity about him is admirable because I believe being human is one factor that is fundamental to manage other humans. Chirac loved the crowds and was at home with people from all walks of life while also having a great sense of humour.
Another French president that I also find inspiring is Nicola Sarkozy, who also is a great example of assimilation and someone who also faced many obstacles in his early years as the son of Hungarian and the grandson of a Jew but who eventually overcame everything and everyone to prove himself as a true Frenchman who had France in his heart. Sarkozy is also the one who inspires others to rise up, unlike many of today’s selfish personalities who, once within a party, seem to hate the younger generations and act as vile and frustrated animals towards tomorrow’s prominent figures.
Hitler too was also a case of great assimilation and having spoken about what I find inspiring about him above, I think we can skip to the last one, which is Charles de Gaulle. The latter, is to me a great example of a man who knew what he wanted and who had a grand vision of a civilisation along with an exemplary modesty who did not selfishly drown himself in luxury but thought of the state and the people before his own comfort. De Gaulle also played an integral part in the liberation of France, and he did it all from England without being present on French soil, being the first to show how technology in the 20th century could be used to manage, organise and motivate a whole empire. The other admirable thing about de Gaulle was that he had gained the confidence of France to lead freely like a monarch and is perhaps today known as the last “democratic King of France”.
The last one before Napoleon is Alexander the Great, who was the only person of Indo-European heritage to have nearly conquered the world starting from Greece to the Indus River. He was a general and an explorer who was also incredibly cultivated from his teachings by the great Aristotle who had taught him science, philosophy, literature and combat techniques – all the necessary skills for a future great leader. From his early years he endured an incredibly demanding father who expected him to never be weak and to be the greatest in all fields. Alexander had a thirst for knowledge and was inspired by the Greek model and wanted to be the best like Achilles the legendary hero of Greek mythology who was told by his father that to behave like a man he would have to be the best and have a better judgement. After being taught by Aristotle for 3 years, Alexander would later say that he loved Aristotle as a father and if his biological father gave him life, it was Aristotle who showed him how to live. The latter told him how the Persian empire extended to the end of the world until India, and how their king had invaded Greece about a 100 years ago, destroying all the cities, taking over Athens and burning down the Acropolis before the Greeks could unite and drive out the Persians. Aristotle had also told Alexander how the Persians were a permanent menace with their troops amassed at the doorsteps of Greece with the tomb of the valorous Achilles still in their hands, and that the dream of eternal glory lies in the act of uniting the Greeks and chasing the Persian troops as this would be the act of a hero. His father had told him that he should find an empire to his size since Greece is too small.
After he started conquering Persia, he defeated the army of Darius although outnumbered by the latter and made the mother, the wife and sisters prisoners. In an act of chivalry he would even promise them that they would be treated with respect and that none of his men would be unpunished if they disrespected Persian women, to the anger and frustration of one of his closest and most talented generals, Philotas. He would tell the latter that after their bravery and heroic win against the Persian army, how could they act like cowards with their women? Alexander continued his exploration and nearly took over the world with many cities including Babylon receiving him as a liberator – he wanted to surpass his ancestors. But perhaps one of his noblest declaration was his desire to have been Diogenes the Cynic if he had not been Alexander. Diogenes was one of the most famous philosophers from the school of cynic philosophy whose character had a profound impact on the Athenians through a mass of legendary anecdotes. This shows that deep in his heart, Alexander was not motivated by luxury or money, but truly wanted to build a noble civilisation of sophisticated and humane people. It also shows his sensibility and ability to relate to modest people but more importantly his wisdom in assessing the greatness of a man not based on his possessions or clothes but solely based on his intelligence and the contents of his discourse; because Diogenes lived outside, in destitution, dressed in a simple coat, with a stick, a bag and a bowl. Denouncing the artifice of social conventions, Diogenes advocated a simple life, closer to nature, and was satisfied with a large jar lying on its side to sleep.
Diogenes had the art of invective and biting speech. It seems that he did not hesitate to openly criticize the great men and other philosophers of his time (among whom Plato). The most famous apostrophes attributed to him are:
“I was once in the home of a teenager of considerable wealth. I was installed in a dining room decorated with paintings and gilding on all sides to the point that there was not even a place to spit. As a mucus rose to my throat, I expectorated it out and looking around me without finding a place to spit, I spat on the young man himself. He reproached me for it. To which I replied, calling him by his name: “What, you blame me for what just happened, and you don’t blame yourself for having the walls and floor of your dining room decorated while leaving only your person without decoration, thus inviting to spit on it’.” -Diogenes
“The other dogs bite their enemies, while I bite my friends, in order to save them.” -Diogenes
“I am looking for a man” – (meaning a true, good and wise man), a phrase he used to utter to his amazed fellow citizens as he walked the streets, brandishing his lantern lit in broad daylight and approaching the faces of passers-by.
“Get out of my sun” – (dazzling reply to Alexander the Great, King of Macedonia, who had kindly come to see him and asked him if he needed something, if he could help him in any way… – Yes, get out of my sun, Diogenes replied.)
Several anecdotes testify to Diogenes’ disregard for wealth and social conventions. According to Diogène Laërce, he did not hesitate to beg with the statues in order to “get used to the refusal”. He abandoned his bowl after seeing a child drinking at the fountain in his hands. When asked about how to avoid the temptation of the flesh, Diogenes would have replied “by masturbating”, and would have added: “It would be better for heaven that it is also enough to rub your stomach to no longer be hungry!” Diogenes was also reportedly seen walking the streets of Athens in broad daylight, with a lantern in his hand, saying to those who asked him what he was doing: “I am looking for a man. “(sometimes translated as “I am looking for man” or “I am looking for a real man”). This “man” would designate the one theorized by Plato, the ideal of the human being, and Diogenes would have wanted to refute his existence, seeing only concrete men exist. Another anecdote reports that, Plato having defined man as a “biped without horns and feathers”, the next day Diogenes walked around the city holding in his hand a deplumed rooster with dewclaws cut off, and declaring: “This is Plato’s man!” Diogenes first lived as a free man, but as he was heading for Aegina by boat, the latter was taken by pirates. Put up for sale as a slave in Corinth, he declared to the merchant who asked him what he could do that he knew how to “govern men”, and that he must therefore be sold to someone who is looking for a master. He ended up being bought by a rich Corinthian who admired his independence of mind, and who gave him his freedom.

Alexander visits Diogenes at Corinth by W. Matthews (1914)
It is in Corinth, where Diogenes lived when he was not in Athens, that the famous meeting of the old bum-philosopher with the young king of Macedonia, Alexander the Great, took place. This episode is told in particular by Plutarch in the Life of Alexander, XVIII, by Cicero in the Tusculans, 5, XXXII, and by Diogenes Laertius in the Lives of Philosophers, Book VI.
Here is the most complete version of their conversation:
” – Ask me what you want, I’ll give it to you.
– Get out of my sun (literally: “Stay away from my sun for a while.”)
– Aren’t you afraid of me?
– What are you?….. A good or a bad?
– A good one.
– Who could fear good?
Diogenes had asked that after his death, his body be thrown on the streets, but his friends gave him an honorable funeral. A column surmounted by a marble dog was placed on his tomb and on which the following verses were written:
“Even bronze undergoes the ageing of time,
But your fame, Diogenes, eternity will not destroy it.
For only you have shown mortals the glory of an independent life
And the easiest path to happy life to follow.”
Alexander the Great: Mutiny at Opis
Today Alexander the Great’s heritage is present in politics along with legends and in literature. He envisioned a universal empire where societies would have an autonomous administration and could co-exist peacefully under an imperial government. Alexander did not only conquer the world; he changed the course of its history forever.
But my all-time favourite leader is Napoleon. Napoleon for his grandeur in nearly everything along with his motivating and inspiring presence that touched men and women from all around the world. Napoleon is someone I seem to connect to because he is perhaps one of the greatest stories of amazing assimilation and rose from a simple military, to general, consul then emperor and all through the acknowledgement of the whole country. Napoleon was a man and child of the Revolution and the First Republic and was its most famous heir; he was a Republican and had nothing to do with the Ancient Régime made up of castes and inequalities.
Napoleon is inspiring to me because like myself he was not born in France, but left his home in Corsica and went to study in France. In his early years, he did not even handle the French language properly and had a strong Corsican accent, and he was also bullied in college while at Brienne, an elite academy and was treated as a little foreign immigrant in these early years. Yet, with such dedication, as an already amazing student and a great self-educated solitary, he would read all the great minds of Europe, cultivate himself and become one of the greatest Frenchmen to ever live. Indeed, from the little foreigner with a dodgy accent, to then become more French than the French, and rise to become the Emperor is truly inspiring. Before receiving his crown on the day of his coronation after the people of France had decided to make him Emperor of the French republic, he turned around and looked to his brother saying, in Corsican « sì u nostru babbu ci hà vistu », meaning « if our father could see us ». This shows that although he embodied France in his heart he was respectful of his humble past as he rose from simple lieutenant to Emperor in only 11 years.

“You dare order me to give up my conquest? And to restore the old boundaries? So hundreds of thousands of French men will have suffered and died for nothing? You’re insane! Your emperor is insane!”, Napoléon puts Austrian statesman, Klemens Wenzel von Metternich in his place (From: Napoleon (2002) by Yves Simoneau, with Christian Clavier as Napoléon – Click HERE to watch the extract)
Napoleon’s exploits also inspired the great writers of the Romantic movement, and especially one of the greatest writing geniuses of all time, Honoré de Balzac. He who, like Napoleon, had a mathematical side to the organization of all his works, notably one of the most fundamental, “La Comédie Humaine” which is divided into three parts: Studies of Manners, Philosophical Studies and Analytical Studies. La Comédie Humaine shows that the whole of existence can be interpreted with all the elements of the theatre since the role we play in society is the role in which a certain number of different actors can succeed each other. In the short story forming part of the philosophical studies, “Adieu”, we see an episode on the retreat from Russia of the Napoleonic imperial troops in 1812 during the passage of the Berezina. Napoleon was a mythical character whom Balzac wanted to compete with in his field, since he saw him as a genius who had shown us the imperial future but who had also succeeded in saving the nobles from the terror and finding a way to synchronize the whole of France harmoniously by establishing a system of progression by effort and meritocracy [creating the National Order of the Legion of Honour in 1802] for everyone after the mess, instability and confusion that the terror had left just after the revolution.
The Order of the Legion of Honour created by Napoleon to reward services to the Nation was a badge with his own figure that he pinned on the chest of his subjects, which was a very strong sign as the Sovereigns of Europe instead had the founders of their dynasty or the symbol of their country, but Napoleon as a man who destroyed the ancient regime pinned his very own profile on the chest of his subjects with the imperial eagle on the reverse of the badge, this was unique and universal as Anne de Chefdebien pointed out, as here the drummer and the prince received the same decoration, so did the intellectual and the soldier who could not read; this was egalitarian, universal and very strong because all those who served the Nation with all their heart had the same reward, this is exceptional because before the revolution all countries including France had several orders which most of the time required birth conditions. Napoleon also had the audacity and courage to want to unify all of Europe under the French flag and its values without intermediaries, to extend the ideas and achievements of the Revolution to all the other peoples of Europe, who had also been plunged into obscurantism for centuries by a ruling minority caste that calls itself “Nobility”; with the Republic and the Empire now everyone can finally access the social ladder based on their abilities after so many centuries. The Empire was created by the people to fight against the incessant attacks against France, the only representative in those times of the Europe of the People, by the old and sclerosed Europe of the United Kings to restore the Ancient Régime and destroy the achievements of the revolution: freedom and equal opportunities for all. The Empire was above all to keep the danger of these incessant attacks further and further away from France’s borders and to calm the desires of the kings and emperors of the retrograde and non-progressive Ancient Régime, because in those days diplomacy existed only in this wild form and peace could only be achieved through it[what France and Napoleon I wanted first and foremost, who were ALWAYS forced to wage war against the attacks of kings, contrary to what a treacherous propaganda has wanted to make us believe for 200 years]: “Cannon diplomacy”, the only existing diplomacy in these turbulent and simply barbaric times.
By studying “Adieu”, we see that Balzac thought that Napoleon’s main mistake was to have badly planned and launched his troops in Russia, a country that Balzac associated with the cold of the snow and literally painted as a vision of a white hell: a country of whiteness, cold and punishment that meant the end of the world. So, for Balzac, the Russian retreat was shocking for France, and it is an event that he wanted to describe as a perspective of history that is heading towards a cold hell, among other things, which could happen to our society if we lower our guard. The Berezina River that the troops will have to cross to survive in “Adieu” becomes the figure of the biblical deluge and to cross it Balzac seemed to imply that we should build a Noah’s Ark that was represented by a raft in the story and Michel Butor argued that it seems to suggest that if we are not able to conduct works of research and invention, then society will lose the generosity of the nobility and the warmth of the ancient heart and become a place where men fragment one another.

Image: (From: Napoléon (2002) by Yves Simoneau, with Christian Clavier as Napoléon – Click HERE to watch an extract in French
Napoleon was also a perfect example of organic theory in creation, development, evolution and self-definition in a sophisticated society that believes in the creative power of the individual to realise his dreams. It is also the whole work of Balzac, the theme of the lonely man abandoned by almost everything where man begins again and rewrites the history of the world; Michel Butor has clearly underlined it: the man of genius is the one for whom the earth becomes a deserted island, because everything deviates from him. His presence as leader was unique and legendary, which led Marshal Bon-Adrien Jeannot de Moncey after his death to say: “Now let’s go home and die!” Napoleon was a man who personified courage, both on the battlefield and in the official affairs of the state, he was guided by values and not money, entirely devoted to France, he placed the people and the greatness of his nation before his own health and comfort. In The Memorial of Saint Helena, Napoleon had even predicted the future opposition between the United States and the Russian Empire, but had also tried to make the public understand that the coalitions that attacked France were political and not military coalitions, seeking to bring down the French Republic and its values and not the Emperor.
In addition to being a military and political genius, he proved that a man could be an intellectual, a soldier, a great builder while being in love with the arts and music. The emperor also had a sense of dignity and values and wanted to allow people of all classes in France to believe in the ability to grow and rise through their own efforts – he wanted all members of his society to be able to dream. For Napoleon, the impossible was not French! Jean-Marie Rouart also pointed out that there is a Napoleonic religion, a cult of Napoleon because the people have understood that through this man, they have all become greater, and this Napoleonic myth will always speak because no one in modern times has been able to achieve his dreams to such an extent; but there is also a moral lesson that is a lesson of hope and if Napoleon is always present it is because there will always be people to go and recharge their batteries in his example, in his words, in the memorial of Saint Helena to find in Napoleon’s life, a time when they really regain optimism, and so it is a lesson in optimism since he has brought politics back to the Man to prove that a man can be exceptional. Chateaubriand seems to have described Napoleon well as “the most powerful breath of life that ever animated human clay”.
10 Tips From Napoleon
Napoleon had an instinctive vision of what a modern country should be and made extraordinary reforms in the legal, political and economic fields for the rights and duties of citizens in order to make society functional after the revolution. The Civil Code, which later became Napoleonic code was also written by him, and he influenced countries all over the world by giving French society a necessary structure for order and security after the revolution and terror. Many other countries were inspired by the Napoleonic code and used it to modernise life in their societies.
Napoleon believed that everything had to be rebuilt on a sound foundation and this is why he will forever remain in the history of Europe as a fundamental figure in military conquest and by trying to impose a new system [a modern state, a new administration, a new central government, a new legislation and a new jurisprudence] that created a heritage which made a return to the ancient regime impossible in all the territories occupied by his troops or influenced by his ideas.
After being welcomed as a hero and savior of the Republic by an ecstatic crowd, in only 3 months in power in France, Napoleon had instated civil peace and created new institutions and reformed the tax system which had led to a spectacular recovery of public finances under the consulate. He did not only attack the institutions but also took the responsibility to modernise and enlarge the country’s infrastructures [new ships manufactured, port and arsenals enlarged and modernised]. In education, we have seen the birth of high schools and a profound reform of education and the university. In the industrial sector, he created a chamber of commerce, modernised the postal service with new optical telegraph lines that linked the 29 major cities together and created and upgraded nearly 50 000 km of roads with artworks and bridges made everywhere. As Charles-Maurice de Talleyrand-Périgord explained, the empire created a real dynamic of peoples, and brought a great number of human and institutional advances, the Napoleonic conquests by disrupting established orders, laid the foundations for many state changes that served many other countries to achieve their unity or independence; Napoleon’s vision of the great empire was unifying and above all a universal European vision stripped of its authoritarian character where it appears resolutely modern, methodically organized; and had nothing to do with the old xenophobic nationalist and racist movements that preach “identity” nowadays and that encourage self-confinement, division, communitarianism and hatred towards others and a united Europe under the French flag that Napoleon dreamed of so much. These ancient non-progressive, static and atavistic nationalist movements stain Napoleon’s legacy.
Video: Writer Andrew Roberts shows his admiration and defends the Emperor, arguing that if any ruler deserves the epithet ‘the Great’ it should be Napoleon
The emperor therefore had the great vision to extend France, its language and values and seemed to follow in Alexander the Great’s footsteps as a conqueror who was on the brink of conquering all of Europe. Napoleon was for me the true leader of men and could motivate them with his honesty rooted in his electrifying speeches and he was also someone who had the qualities of a conqueror and who believed that an empire needed expansion to progress. I think that Napoleon Bonaparte is an example of the greatness of French civilization and also the proof that France is the civilization that embodies the greatness of humanity, its dreams and the values of meritocracy and excellence. “Napoleon will grow, as we get to know him better,” said Johann Wolfgang von Goethe.

Ce billet de 100 Nouveaux Francs Bonaparte de la Banque de France a été imprimé du 5 mars 1959 au 2 avril 1964 et mis en circulation à partir du 4 janvier 1960. / Source: Bourse du Collectionneur
_________________________________
QUESTION VIII.
[FR] – Avez-vous l’intention de vous lancer en politique?
[EN] – Do you plan in getting into politics?
[FR] Réponse:
Après avoir constamment critiqué les systèmes politiques mondiaux et la race des politiciens pour la plupart médiocres, corrompus et désagréables qui ont fait surface au cours des 5-6 dernières décennies, il serait certainement controversé que je réponde “oui” à cette question. Cela semblerait hypocrite à mon auditoire. J’ai toujours pensé qu’il était de mon devoir de guider la civilisation sur la bonne voie et je crois fermement que le modèle actuel de gouvernement politique n’est pas approprié pour atteindre un tel objectif.
La démocratie est un concept qui donne une voix au peuple, mais la politique est quelque chose de très différent qui n’est pas à l’abri des âmes immorales et corrompues et de leur égoïsme. En plus d’avoir constamment critiqué la politique comme un concept dépassé et mal appliqué qui découle d’une mauvaise application de la démocratie, ainsi que les politiciens qui, tout au long de la civilisation, ont joué un rôle significatif dans les tragédies de la civilisation humaine, ce ne serait certainement pas ma fierté de devenir un homme politique.

Là où la corruption fait rage dans le monde / Source: Statista
Les organisations connues sous le nom de “partis politiques” sont à l’origine d’un grand nombre de problèmes auxquels la civilisation humaine est confrontée, puisqu’il s’agit de diviser la population en segments qui correspondent à leurs politiques de gauche, du centre et de droite. Je ne voudrais donc jamais être considéré comme un “politicien”, mais plutôt comme un leader d’êtres humains sans affiliation politique parce qu’ils imposent trop à la vision créative d’un grand leader et conduisent à trop de concessions pour satisfaire les donateurs et satisfaire des motifs financiers qui ne sont pas vraiment dans l’intérêt de la nation et du pays. Je crois en la science et la philosophie et je considère les gens comme des organismes d’un système que nous devons trouver un moyen de synchroniser pour réaliser le rêve d’une civilisation noble et sophistiquée. Même la logique de ma théorie organique conduit à la même conclusion.
Ainsi, aujourd’hui, en 2021, j’ai pu toucher les esprits et les cœurs des gens grâce aux outils technologiques extraordinaires que notre civilisation moderne nous a donnés, et il y a peut-être 200 ans, il serait impossible de se bâtir une réputation publique et de se faire un nom en tant que leader sans un parti, des donateurs et des fonds.
Pourtant, pour changer la vie des gens et le système qui est utilisé pour les gérer aujourd’hui, il n’est malheureusement pas possible de le faire sans emprunter la voie sale de la politique. Je ne peux donc pas dire avec certitude que je n’emprunterai jamais cette voie, car c’est peut-être la seule, jusqu’à ce que quelqu’un de sophistiqué et de juste change le système et en crée un nouveau qui puisse gouverner les hommes et apporter la stabilité dans la gestion de la civilisation tout en appliquant la démocratie de manière optimale.
Pourtant, si jamais je me lance en politique, je veux que les gens sachent que je ne me qualifierai jamais comme politicien, mais comme un homme qui veut conduire sa civilisation et ses hommes et femmes à la grandeur. Les termes “politique” et “homme politique” sont aujourd’hui des symboles d’inadéquation, de corruption, de méchanceté, de mesquinerie, de division, d’égoïsme, de mensonge, de tromperie et bien d’autres choses qui ne sont pas dans l’intérêt du genre humain.

Image: « Etude de trente-cinq têtes d’expression », vers 1825 par Louis Léopold Boilly
Je m’efforcerai de faire de tout cela une histoire morte et de construire un nouveau système.
Aujourd’hui, nous vivons dans un monde où la corruption fait rage et même les associations connues sous le nom de “presse libre” se sont transformées en outils politiques qui n’ont absolument aucune valeur et aucun respect pour la société et ses citoyens. Bien sûr, je ne dis pas que tous les journalistes sont des êtres méchants et vils parce que nous avons une petite section d’écrivains et de chroniqueurs vraiment travailleurs, nobles, authentiques et professionnels qui sont des maîtres dans leur domaine spécialisé, mais pour la majorité, ils semblent être simplement des outils d’écriture médiocres dans la couverture d’événements et des pantins de diffamation appartenant entièrement aux entreprises pour lesquelles ils travaillent – des écrivains du dimanche sans âme, sans art littéraire, amour des mots, profondeur de réflexion, vision, style ou philosophie.

Image : Les travailleurs de l’Agence France-Presse (Août 1944)
Cette race particulière d’ordure a tendance à jeter de la saleté sur les gens par ordre et s’ils le font avec moi aujourd’hui, ils le feront demain avec vous, vos enfants et les enfants de vos enfants.
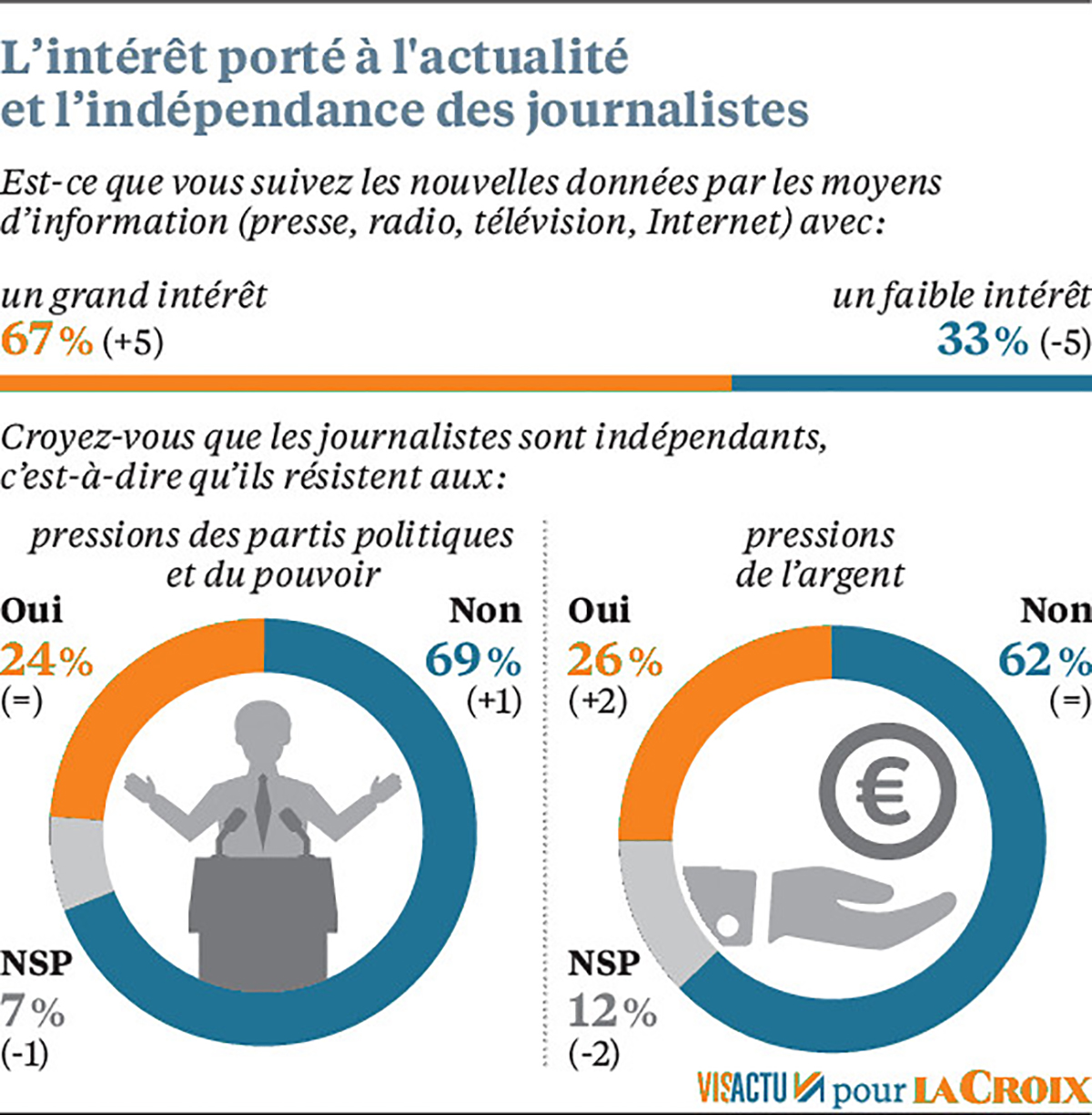
L’indépendance des journalistes / Source: LaCroix
Par conséquent, nous ne pouvons pas rester dociles en tant que société si nous voulons créer un système équitable et transmettre à nos enfants la liberté pour laquelle beaucoup sont morts et aussi le droit de s’élever par leurs propres efforts dans une société juste et noble qui croit aux débats et aux arguments sophistiqués et non à l’intimidation et aux moqueries sans raison qui étouffe les idées incroyables et détourne l’attention aux bêtises. En effet, j’ai été l’objet de beaucoup de méchanceté de la part de la presse qui sert ses maîtres politiques.

L’inévitable chutes des Présidents auprès des Français / Source: Statista
La seule question qui me frappe toujours quand ces imbéciles essaient de se moquer de moi, c’est « Qu’est-ce que je pourrais apprendre de toi ? », c’est-à-dire « Avec quelles connaissances concrètes et intelligentes pourraient-ils m’éclairer ? » Probablement pas grand-chose ! La plupart du temps, c’est moi qui ai envie de dire « Si les limites de votre intelligence et de votre cerveau empêchent la compréhension en raison du niveau de l’écriture, une question poliment posée en levant la main semble être une démarche productive. »

Traduction(EN):”If the limits of your intelligence and brain prevent understanding because of the level of the writings, a politely asked question while raising one’s hand seems like a productive move.”
Ainsi, il semble assez évident qu’une grande métaphore pour expliquer la façon dont je perçois les outils corrompus, vils et bas de gamme de la presse, serait un “insecte”, oui, dans son propre cirque avec d’autres insectes, dans une sorte de comédie où la médiocrité par frustration essaie de noyer le noble débat académique, scientifique, philosophique, psychologique et logique dans une mesquinerie absolue. Pour citer Aymeric Caron: «Un ver de terre n’a évidemment pas le même rapport au monde qu’un humain», et à cela j’ajouterai qu’il n’as pas non plus la connaissance culturelle des différents milieux, la maîtrise linguistique, la compréhension et la perception du monde qu’un humain.
Heureusement la société est devenue plus intelligente en 2021 et les gens brillants savent maintenant que plus rien ne peut suffoquer la véritable intelligence, la science, la philosophie, la psychologie et la raison. En fait, je ne peux pas permettre qu’une telle mesquinerie me fasse perdre mon temps, en effet je sais que j’ai affaire à des insectes inférieurs parce que je suis un personnage assez connu dans le monde depuis près d’une décennie maintenant et ils n’ont toujours pas eu le cran et le courage de me faire face devant une audience publique avec leurs voix tremblantes et leurs arguments paysans auxquels je ne pense pas même devoir me préparer, du moins dans la majorité des cas.
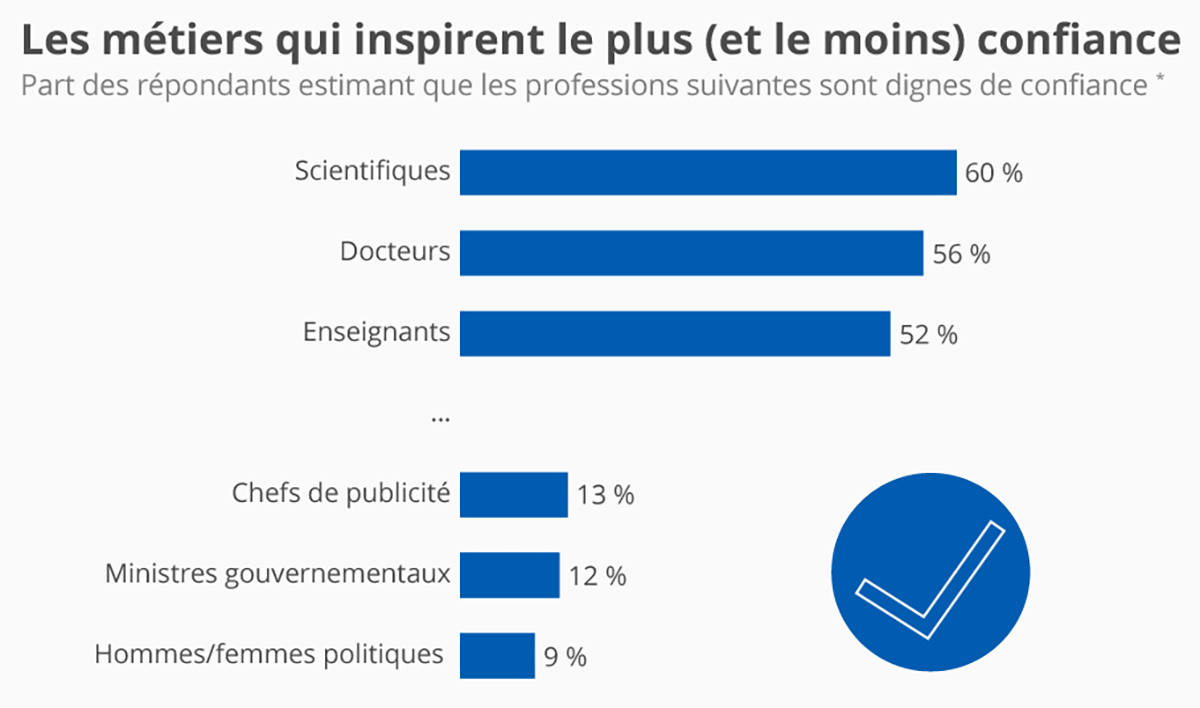
Les métiers qui inspirent le plus (et le moins) confiance / Source: Statista France
Mes arguments sont donc une façon de dire que la noblesse d’esprit, l’intelligence et la classe ne s’inclineront jamais devant des insectes frustrés. Je crois qu’ils devraient aussi arrêter de rêver parce que je ne leur dois absolument rien, à eux et à leur cirque comique. Les seuls domaines auxquels je dois des choses sont ceux de la recherche, de la psychologie, de la philosophie, de la littérature, de la poésie et des arts et il y a des livres sur lesquels je travaille actuellement. Il semble que ces personnes puissent souffrir d’une certaine forme légère de trouble d’apprentissage parce qu’elles ne cessent de répéter des débats qui ont déjà été scellés, comme si elles jetaient constamment leur propre insécurité sur les autres pour voir comment elles réagissent. J’ai déjà expliqué que les insécurités d’une personne n’affectent pas le monde entier, mais seulement cette personne qui peut avoir besoin d’une intervention psychologique pour évoluer vers un être éclairé. C’est comme s’ils ne pouvaient pas lire et comprendre la bonne science et le bon raisonnement, ou peut-être ne veulent-ils pas “comprendre”. Ils ne réalisent pas non plus que chacune de leurs tentatives enfantines de dénigrer les gens décrit leur insécurité et leur peur de gérer des débats intelligents et que de plus en plus de gens commencent à comprendre leur routine sale et abjecte, ce qui peut se refléter dans le nombre croissant de personnes qui ne font plus confiance à la presse du monde entier et qui ont récemment été vandalisées par le mouvement courageux et défiant “Gillet Jaune” qui donne un exemple à la foule mondiale et leur explique comment résister à la politique stupide, à l’injustice et aux idioties médiatiques.

Image : Des journalistes au siège de l’agence Havas en 1930 à Paris (AFP Archives)
Personnellement, en ce qui concerne la presse corrompue, j’aimerais qu’ils comprennent qu’ils ne sont pas au niveau ou à la ligue pour me faire la leçon ou me conseiller parce que la plupart d’entre eux manquent d’intelligence, de culture et de langue, alors que je suis parmi et m’engage dans des discussions sérieuses avec l’esprit des gens qui leur accordent des diplômes universitaires. Oui, je suis au cœur des choses et j’extrais des documents de revues académiques renommées, tout en étant lié à des départements à Oxford, Londres, Paris, Grenoble et même aux Etats-Unis en termes de psychologie, santé mentale, philosophie et société, et je leur explique comment se construire, s’éduquer, se cultiver, s’améliorer, gérer leur vie, leur stress, leurs perceptions, leurs comportements, leurs relations, leurs carrières et comment élever leurs enfants. Ainsi, mon message à ces gens vils est que jeter de la terre partout n’aura absolument aucun impact sur la science et la psychologie, c’est une perte de temps et d’énergie de leur part qui pourrait être investie de façon appropriée dans une autre activité (par exemple, courir pour perdre du poids), car la vie d’un individu n’a jamais été et ne sera jamais définie par les désirs et inventions de leurs esprits pathétiques, obsolètes et mal informés. En effet, il semble que seul un organisme avec l’intelligence d’un âne pourrait créer des mensonges comme eux, puis croire en leurs propres mensonges et danser sur eux, c’est absolument insensé et je crois qu’ils devraient cesser d’agir comme des enfants de 10 ans.

Image : Homme remettant une chaise à une femme dans un kiosque à journaux sur les Champs-Elysées, 1951 (Photo de Robert Doisneau)
Je ne suis pas le premier et certainement pas le dernier à souligner que lorsque la médiocrité et les institutions qui ont construit une entreprise et une communauté superficielle autour d’elle gouvernent, les génies souffriront et seront considérés comme dangereux, Honoré de Balzac croyait aussi que la pensée, le génie et le talent étaient toujours ce qui comptait le plus. Balzac dans ses écrits a également indiqué comment ceux qui ont du génie en eux seront en avance sur leur temps et seront incompris et verront le présent comme un palais sans âme où le génie est inconnu, comme dans “le chef d’oeuvre inconnu” de Balzac, bien que bien connu reste inconnu. Honoré de Balzac rivalisa avec les peintres de son temps et voulait rassembler et réunir tous les genres littéraires pour donner une idée de tout ce qu’un écrivain pouvait faire de son temps, et deux thèmes importants de son œuvre sont la foi et le pouvoir de la littérature; la foi dans la possibilité de trouver des solutions aux impossibilités apparentes était le but de sa littérature, inventant des fictions qui se transformeraient finalement en réalité parce que les personnages existent grâce à un acte de foi et parlent de sujets qui avant n’occupaient pas la conscience de la société. En effet, nous semblons tous les deux être du côté de la croyance que les idées révolutionnaires sont le résultat du développement de la société. Plus fortuit encore, Balzac pensait aussi que la société de son temps avait déraillé et qu’il était de son devoir de résoudre les problèmes tout en expliquant à la presse combien il était génial. Balzac voyait la société contemporaine comme une femme sans cœur qui blesse ceux qui l’aiment, et l’a comparera à une femme de cœur et avec une âme. Pourtant, comme Balzac décrivait les maladies de la société, il a également fourni les solutions pour les guérir, et une des caractéristiques principale chez Balzac c’est sont les moeurs de la société qu’il compare à l’extérieure d’une cathédrale, et de l’autre côté la philosophie de la société qu’il compare à l’intérieure de la cathédrale, et c’est seulement après cette initiation que nous sommes capables de réfléchir et rêver avec Balzac. C’est l’une des grandes contradictions de toutes les œuvres monumentales et gigantesques : la majorité des gens ne la lisent qu’en partie. Il croyait donc que le génie rencontrera toujours des problèmes parce qu’il est impossible pour la majorité de la médiocrité de tout comprendre instantanément : il faut du temps pour que les idées se diffusent et soient pleinement comprises. Le fait de ne rien voir dans une œuvre d’art ne veut pas dire qu’elle n’est pas étonnante, car elle peut tout simplement passer de l’autre côté des limites d’une certaine période de l’histoire. Au XIXe siècle, nous avions beaucoup d’artistes qui n’étaient pas connus parce qu’ils étaient en avance sur leur temps. En tant que symbolisme chrétien, Balzac pensait que le grand artiste à cause du poids de son génie souffrirait pour son art et pour le reste du monde, le même artiste qui a le monde entier dans son atelier sans limites où l’homme est un microcosme. “Ayant les oreilles pour écouter le chant des anges…. croyant exprimer la musique du ciel a des auditeurs stupéfaits… ” et ” …en regrettant que vous ne saisissiez pas la plume à une époque ou les gentilhommes doivent s’en servir aussi bien que leurs épées afin de sauver leur pays… “, sous cette belle langue se cache un phénomène commun au XIXe siècle de Balzac, celui de l’écriture collaborative où l’auteur est le directeur d’une grande entreprise littéraire qui couvrira toute la France [et éventuellement le monde] tout en y ajoutant sa touche personnelle. L’un des thèmes principaux du mouvement intellectuel des romantiques est que la littérature est l’équivalent de la noblesse ; la plume est ce qui remplace l’épée antique et cela s’est exprimé dans la littérature confuse du XIXe siècle. L’épée de l’académicien est le symbole de ce thème essentiel du remplacement de l’ancienne noblesse par l’écrivain [être du courant de pensée romantique est considéré comme être un remplaçant de l’ancien noble]. Assez inchangé depuis l’époque de Balzac, le roi n’est encore qu’une représentation de la classe moyenne médiocre : il ne représente plus les plus intelligents, courageux, sensibles, aimants, etc. Le roi de la classe moyenne représente l’intelligence moyenne de la médiocrité et le courage moyen [mis entre les plus courageux et les plus lâches]. Ainsi, l’époque contemporaine est celle où l’artiste de génie est le plus malheureux, comme l’a également souligné Balzac. Nous avons vu ce thème exploré dans “Gambara”, où un artiste musical de génie était trop talentueux pour être compris en son temps : si ses œuvres avaient été présentées à la médiocrité de la majorité, elles auraient échoué, car seuls les auditeurs de génie auraient compris, et pour Balzac, le génie a dû baisser son talent suprême pour satisfaire la médiocrité de la majorité – Balzac y a vu celà comme une sorte de prostitution pour le génie. Balzac voulait faire comprendre aux âmes grossières ce qu’est la poésie. Balzac a présenté l’opéra de Meyerbeer “Robert le diable” comme l’opéra de Satan représentant toute cette médiocrité qui empêche les choses de progresser et d’avancer, le génie du mal, et dans les mots de Michel Butor, « le grand singe qui défigure les œuvres de Dieu ». En conclusion, Balzac pensait que la démocratie de son temps n’était pas adéquate pour le génie parce que c’était une société inégale qui ne pouvait que donner un jeu au génie qui ne lui laisserait d’autre solution que de se retourner contre la société dont il fait partie, et donc de transformer la société en une société qui ne peut fonctionner que si le génie est mort – ceci n’est ni logique ni acceptable car c’est le génie qui contribue le plus à construire la société. On le voit dans “L’enfant maudit” où l’enfant que l’on croyait maudit allait inventer une nouvelle science et développer son génie : (i) un génie naturaliste pour sa relation aux fleurs, (ii) un génie poétique pour sa relation à la mer, (iii) un génie de l’amour pour sa relation à la fille, et (iv) un génie scientifique pour sa relation au monde naturel et à la botanique. “L’enfant maudit” : Une créature entre Dieu et l’Homme, un génie qui serait masculin mais aussi avec une sensibilité féminine, que Balzac décrit comme un enfant pour sa sensibilité et comme un homme pour sa science, où l’océan est un réflecteur et un laboratoire d’affectivité intérieure, immense, infini. Pour Balzac, le génie est maudit, et plus il est étonnant, plus il sera incompris par la médiocrité de son temps. Malgré connu pour être un génie de la littérature réaliste, Balzac charge ses textes de rêves et de fantaisie [comme dans les contes de Perrault] puisque la littérature réaliste fait partie de la littérature fantastique, qui est toujours interprétée d’une façon symbolique. La littérature réaliste a comme résultat une transformation de l’histoire [et donc a un effet foudroyant] et la connaissance générale qui résulte de ce foudroiement motive la société et le monde à changer. Balzac croyait fermement que la littérature et la peinture étaient un moyen de construire une peau plus forte, que l’amour était un art, et que Dante était le génie de l’amour.
“La tragédie échauffe l’âme, élève le coeur, peut et doit créer des héros.”
-Napoléon
Ainsi, venant d’un milieu littéraire, philosophique, psychologique et de penseurs sensibles, je dois dire que depuis que j’ai commencé à m’engager auprès du public, de la presse et des politiciens médiocres de notre époque en 2012 jusqu’à maintenant, j’ai, tout comme Cécile Guilbert, été complètement dégoûtée par la « bassesse du courtisan », mais aussi choquée de découvrir la réalité du système atavique qui sert à gérer la société [et qui forme la perception, le comportement, et la réalité banale de la majorité] qui est conçu de telle manière qu’il se laisse devenir le théâtre de la médiocrité en sélectionnant les personnes sans connaissance adéquate et un grand nombre d’esprits grotesques, frustrés et vils avec la bassesse d’un paysan amer et les valeurs d’un reptile à sang froid pour être à la tête de ses différents départements quand ils comprennent à peine la vie intérieure et extérieure des individus et comment favoriser la créativité, l’innovation et le progrès tout en réalisant l’équilibre, l’harmonie et la stabilité de la civilisation humaine, ce que j’appellerais en trois mots, “joie de vivre”.
Ça doit aussi être démoralisant pour les esprits les plus sophistiqués de voir ce cycle répétitif et mondain à quelques années d’intervalle lorsqu’une autre bande de primates bureaucratiques s’empare du système pour ensuite imposer leurs valeurs et leurs goûts économiques même si aucun changement n’est nécessaire. Le système imparfait de la démocratie et des partis politiques implique que l’opposition doit toujours se tromper et que l’ancien groupe ne peut jamais faire un travail décent – c’est assez irrationnel ! Croire que ces parvenus médiocres de la classe moyenne, sans aucun fondement et éducation classiques, seront capables de conduire la civilisation humaine à l’harmonie avec leur éducation mécanique et leurs politiques économique, est semblable à croire aux super-héros en spandex. Ces personnes devraient être placés dans un département financier pas au centre de la civilisation. L’économie doit s’efforcer d’améliorer et de sophistiquer l’existence humaine et la civilisation, et non l’inverse. Je trouve choquant que ce système démocratique atavique que George Orwell a décrit dans son opus Magnum, “La Ferme des animaux (1945)” – un texte qui m’a marqué en tant qu’étudiant en littérature à l’adolescence – soit en fait quelque chose que nous, êtres humains, devons accepter comme le remplacement absolu de César, Alexandre le Grand, Napoléon ou Sénèque.

Ce billet de 100 Francs Delacroix de la Banque de France a été imprimé de 1978 à 1989 / Source: Bourse du Collectionneur
Nous, les primates les plus intelligents de la planète, au sommet de la chaîne alimentaire, nous qui avons créé des hommes comme Napoléon, Balzac, Sartre, Camus, de Chazal, Darwin, Descartes, Delacroix, Bourdon le peintre, Vivaldi, Chopin, Verne, Lacan, Pasteur et inventé des satellites, des ordinateurs, des logiciels ingénieux qui créent presque tout, des pianos et des appareils mobiles sophistiqués, nous, gens extraordinaires, avons accepté et imposé à nous une organisation horrible et instable d’employés de bureau insuffisants et ignorants pour gérer notre civilisation et diriger nos vies ?

Traduction [EN]: “The important thing is not to get out of Polytechnique, but to get out of the ordinary.” – Charles de Gaulle
J’ai encore du mal à croire ce cauchemar, car tous nos leaders mythiques avaient reçu une solide éducation classique, et donc une compréhension psychologique précoce de ce qui fait avancer la vie et de ce qui crée des esprits nobles avec des valeurs parmi les hommes et les femmes, et donc ce qui crée une civilisation harmonieuse et glorieuse. L’empire de Napoléon a été fondé et s’est principalement concentré sur des sentiments, des valeurs, des idéaux et des idées français solides, pas simplement des motifs financiers et des perspectives d’affaires, ce qui n’était qu’une fraction de l’ensemble. Alexandre le Grand a eu une éducation philosophique et a étudié les grandes tragédies avec Aristote lui-même et a été considéré comme un dieu ou un homme qui était aussi proche que possible de Dieu, un ami de l’humanité qui a changé le monde entier, a cru en l’humanité et l’a prouvé en adoptant des tribus misérables pour créer un empire où tout devient possible. Alexandre a montré que le monde pouvait être gouverné par un seul dirigeant pour le bien-être de tous ses sujets. Mais plus important encore, l’empire d’Alexandre n’a pas été fondé sur des envies de terres ou de richesses mais sur des idées comme celle de Napoléon : l’idée hellénistique d’une civilisation ouverte à tous. Alexandre portait un rêve immense avec la passion de la jeunesse éternelle, complètement convaincu que nos forces collectives et notre imagination pourraient nous mener à des niveaux qu’on croyait impossibles auparavant; là où le dépassement de soi devenait facile. Quant à Sénèque, c’était un homme d’État aux valeurs fortes et aux orientations philosophiques qui incarnait la noblesse d’esprit et la vision des grands empereurs, et qui n’avait rien à voir avec l’horreur politique actuelle de la médiocrité et de la bassesse avec des animaux parvenus simples d’esprit, diplômés dans un domaine mécanique et commercial, qui se trompent sur leurs capacités et leur espoir d’être considérés comme les empereurs du monde moderne. Tous les systèmes montrent leur âge et leurs faiblesses à travers le temps, et nous avons atteint les limites des politiciens cochons comme le décrit George Orwell pour gérer notre société.
Les gens devraient se poser la question très honnête tout en regardant dans les yeux de ces représentants régionaux pathétiques, peu créatifs et médiocre élus par une masse à l’intelligence et de culture douteuse : “Cette tronche ressemble-t-elle à un bâtisseur d’empire ?” [c.-à-d. ce cerveau commun moyen a-t-il la noblesse d’esprit, les valeurs, les goûts, la finesse, la philosophie, la créativité évolutive, la vision esthétique et architecturale, les sentiments, le cœur, l’honnêteté, le courage, la passion, la volonté d’acier, la sensibilité, l’intelligence poétique, les arguments d’un vainqueur, la confiance, l’ingéniosité, le dévouement, la compréhension psychologique et psychique des êtres humains, les faits scientifiques, la connaissance, les capacités d’analyse et de débat et la créativité économique pour créer un empire humain que la grande race humaine mérite ? Un empire qui durera une éternité, générera une atmosphère humaine et positive qui nous poussera à nous dépasser, à favoriser notre développement, à créer une existence agréable et à nous étendre dans l’espace ?] La vérité est que la plupart des politiciens en vie aujourd’hui n’ont pas la passion de nos grands dirigeants historiques, parce qu’ils sont le produit d’une génération de bureaucrates impuissants, de lâcheté, de médiocrité, d’arrogance, de bassesse, de brutalité, de ragots, de corruption, de vice, de luxe bon marché et de cupidité pour l’argent. Ce ne sont pas ceux qui se sont vus comme les remplaçants des nobles bâtisseurs de l’empire, des hommes de mots, de finesse, d’intelligence, de valeurs et de philosophie, qui ont passé leurs journées et leurs nuits à réfléchir indépendamment à la vision d’un empire humain massif et à trouver la stabilité et à optimiser la race humaine pour une existence harmonieuse, minutieusement calculée et conçue pour être éternelle avec un système qui aborde et résout nos problèmes même si elle ne correspond pas au modèle politique actuel ; mais sont simplement des employés de bureau pathétiques qui se considèrent comme des hommes qui veulent être vus comme importants simplement parce qu’ils font partie d’un parti politique et qu’ils montrent leurs drôles de visages dans la presse commune qui appartient principalement à des Juifs qui l’utilisent comme un théâtre bon marché où ils commandent leurs esclaves employés pour créer une atmosphère et provoquer les types de disputes et autre frictions qui conviennent à leurs agendas, et ceux de leurs maîtres politiques.

La confiance dans les médias au plus bas depuis 32 ans / Source: L’Express

La confiance dans les médias en chute libre en France / Source: Lanceur d’Alerte [Cliquez pour aussi voir qui possède quoi]

Crédits : Jack Guez – AFP

Part des Français ayant confiance en l’information diffusée / Source: Statista

“Le sot a un grand avantage sur l’homme d’esprit : il est toujours content de lui-même.”
-Napoléon
Un théoricien de la psychologie d’élite qui s’occupe du comportement et de la sculpture cérébral au niveau granulaire n’écoutera pas les absurdités d’un esprit simple, même si les partenaires de cet esprit simple peuvent payer tous les annonceurs du monde pour publier leurs absurdités sur du papier toilette, des boîtes de céréales, la presse animale bon marché aux arrêts de bus. Nous sommes au-dessus de cela ! Chaque fois qu’un éditeur drogué d’un coin obscur d’Internet crée un titre avec une image qu’il considère dégradante, cela n’a aucun effet sur nous, aucun, zéro ; avec ses doigts moites et collants claquant sur un clavier crasseux au 10e étage d’un vieil immeuble dans un coin bondé d’une jungle urbaine polluée ? Nous sommes au-dessus de ces petites campagnes de diffamation organisées par les grands enfants de la politiques et les médias juifs qui leur sont si chers. Il ne peut être antisémite de simplement affirmer que la majorité de la presse appartient à des Juifs et est donc contrôlée par eux. Mon message à ces gens est : “Essayez de grandir ! Aucune personne intelligente au monde n’est définie par vos pulsions…. vous êtes pire que des enfants. Les gens se définissent eux-mêmes…. simple….. vos opinions, ce ne sont que de simples opinions aussi simples que votre esprit !” Je pense que puisque nous en parlons, il faut reconnaître que les Juifs et leur obsession à contrôler les médias et à corrompre les décideurs avec leur argent, et donc à causer des frictions et d’autres pressions sur les sociétés et les gouvernements pour qu’ils imposent leurs vues, dans la plupart des pays européens où ils se sont implantés, ne sont pas une pratique nouvelle pour eux, ils le font depuis des siècles, et il est peut-être aussi opportun pour des Juifs érudits et sensibles de tenter d’imaginer les raisons des décisions du Reich d’Hitler pour tous les retourner en Israël ; ce qui est vraiment surprenant même le rabbin juif Yosef Tzvi Ben Porat pensait qu’Hitler avait raison de haïr les juifs pour ce qu’ils font.

Camp de concentration à Auschwitz
En autre, la grande majorité des politiciens médiocres et leurs partenaires en propagande ne se considèrent pas comme des bâtisseurs d’empire parce qu’ils n’ont pas l’ingéniosité pour le faire, ils ne sont même pas assez créatifs pour avoir des discussions nobles et sophistiquées, ou pour remettre en question le système vieillissant et oser considérer qu’il pourrait y avoir mieux, car ces hommes ne sont pas au niveau intellectuel pour penser comme un réformateur et un créateur d’avant-garde. Ils n’ont tout simplement pas le pouvoir mental et les prouesses intellectuelles nécessaires pour défier un vieux système créé par l’homme : ils ne peuvent pas concevoir la réalité parce qu’elle est au-delà de leur compréhension – ils n’ont jamais remis en question leur propre existence ou but, mais ils ont simplement suivi et copié les médiocrités passées dont ils essaient de reproduire sans aucun sens critique. Ces ignobles créatures se considèrent comme les membres d’un groupe politique ayant une perspective unilatérale et n’ont pas les compétences créatives et la sagesse nécessaires pour penser indépendamment et prendre la responsabilité de la construction d’un empire humain éternel ; elles ne pensent qu’à court terme, c’est-à-dire comment gagner une élection ? Comment faire plaisir au leader ? Comment gagner la prochaine élection ? Comment être choisi pour être responsable d’un ministère ? Comment parler au journaliste ? Comment faire en sorte que les gens votent pour eux ? Comment harceler leurs adversaires de la manière la plus enfantine qui soit ?

Ces hommes sont des parvenus, ce que je qualifierais de sauvages du luxe qui portent un costume pour leur profession et leur environnement, mais à l’intérieur de leur esprit pourri, ils pourraient être comparés à des paysans amers pour leur esprit simple, leur comportement, leur vision, leur ignorance et leurs broutilles enfantines.

65% Insatisfait de la Démocratie en France / Source: Statista
La démocratie et le système politique ne sont pas des créations divines, mais comme tout le reste, il nous faut des mises à jour, des révisions et des réorganisations pour atteindre un système plus sophistiqué et raisonnable qui peut nous offrir un empire humain harmonieux où chacun peut rêver et réaliser ; mais aussi “vivre” et non simplement exister en étant mort de l’intérieure. Certains dans la politique semblent aussi ressentir les douleurs d’un système désuet, par exemple Claire Nouvian qui vient de mettre un terme à sa vie politique en admettant les défauts de mise en oeuvre et les dysfonctionnements humains de la machine politique, et je pense qu’elle à bien fait de citer Mauroy, « quand les dégoûtés partent, il ne reste plus que les dégoûtants » et de partir en déclarant: « Mes attentes en matière d’honnêteté et de courage ne sont pas compatibles avec la tambouille politique », expliqua Claire Nouvian, « C’est moi qui suis inadaptée à ce milieu ».
C’est clair non pas seulement pour les meilleurs intellectuels et penseurs de notre ère mais aussi pour la section du publique consciente scientifiquement, cultivée et littéraire, que les médias aujourd’hui préfèrent la médiocrité de masse conformiste, plutôt que d’inviter les élites ou les meilleurs de notre temps; je pense que c’est dangereux pour la civilisation parce que comme l’a dit Yeats, “l’éducation n’est pas le remplissage du seau, mais l’allumage d’un feu”, et comme l’a aussi dit Einstein, “l’éducation n’est pas l’apprentissage des faits, mais la formation de l’esprit à penser”, et les médias de masse juives nous donne la pensée et la vision de la médiocrité conformiste. Ces médias mensongères, ataviques et corrompus semblent préférer ces médiocrités ennuyeux et mal informés qu’ils nous forcent à consommer en forme de débats et d’opinions de bureaucrates vides sans un sens crédible du raisonnement – de la camelote bon marché en soie, costume et cravate.
En ce moment, je me concentre sur l’écriture de mes livres, car je crois qu’ils contiennent un grand nombre de découvertes et d’innovations fondamentales et décisives pour la psychologie, la philosophie et les valeurs de notre civilisation fragmentée et confuse actuelle. Une fois qu’ils auront été publiés pour un large public, allant des jeunes aux plus âgés, je crois qu’ils auront présenté ma vision, ma pensée et mon orientation aux masses. Pour moi, il est fondamental que les gens comprennent mon esprit et mon cœur avant qu’ils puissent me voir comme un leader possible, parce que Je veux que les gens me fassent confiance en se basant sur le contenu de mon cerveau, et non pour ma popularité ou pour le fait que mon visage apparaisse sur des papiers insignifiants et dans leurs rues grâce au pouvoir des portefeuilles de donateurs immoraux avec la seule intention de saigner le peuple, d’asservir l’État en l’accordant à leur agenda pour leurs comptes bancaires. Cela ne veut pas dire que je suis contre les affaires ou que je suis pour une économie faible ! Bien sûr, je veux une économie forte, mais je crois aussi fermement que de bonnes affaires peuvent être totalement éthiques en respectant les sensibilités des gens et de l’environnement. Il y a des hommes d’affaires décents qui réussissent et qui ont réalisé leur rêve tout en étant éthiques, moraux et justes. Les affaires peuvent être nobles lorsqu’elles sont faites avec les bonnes valeurs, et n’ont pas besoin d’être faites aux dépens du sang du peuple, et beaucoup d’hommes d’affaires sauvages aujourd’hui ne semblent toujours pas comprendre cela et ils trouvent des moyens d’infiltrer et de détruire le système en corrompant des politiciens immoraux qui ne peuvent résister au goût de l’argent sale. Cela conduit à la souffrance et à un système sans humanité, et je m’oppose à ces scénarios parce que mon objectif est l’harmonie dans tout le système et je sais qu’il peut être atteint avec le bon leader, les bons esprits, les bons cœurs et les bonnes valeurs.
Je déteste donc le terme politique et, pour l’instant, je me concentre sur mon devoir d’éclairer et de guider la civilisation à travers mon travail intellectuel. Mon objectif est de changer le système et de le réorganiser en quelque chose de stable, efficace et honorable tout en rendant la vie des gens meilleure, plus heureuse et plus sophistiquée. Je ne peux pas dire si l’avenir me forcera à entrer dans le monde de la politique, mais je ne me présenterai jamais comme un politicien, et c’est quelque chose que je veux que les gens connaissent et ancrent dans leur esprit et dans leur cœur. Si je suis forcé de faire de la politique, ce serait pour la changer pour toujours, et même enterrer le terme politique et politiciens pour créer quelque chose de plus grand, de meilleur, de plus noble, de plus stable, de plus organisé, de plus sophistiqué et de plus civilisé.
Donc, votre réponse à cette question semble être une réponse que seul le temps peut répondre.

Image: Alexandre le Grand (2011) . Arte
“On ne conduit le peuple qu’en lui montrant un avenir : un chef est un marchand d’espérance.”
-Napoléon
—-|—-
[EN] Answer to Question VIII. “Do you plan in getting into politics?”
After constantly criticising the political systems globally and the breed of mostly mediocre, corrupt and nasty politicians that have surfaced over the last 5-6 decades it would certainly seem controversial if I was to answer “Yes” to this question. It would come across as hypocritical to my audience. I have always thought of my duty in this lifetime to guide civilisation into the right path and firmly believe that the current model of political government is not appropriate in achieving such a goal.
Democracy is one concept that gives the people a voice, but politics is something quite different that is not safe from immoral and corrupt souls and their selfishness. Besides having constantly criticised politics as an outdated and badly applied concept that stems from the wrong application of democracy, along with politicians who throughout civilisation have played a significant part in the tragedies on human civilisation, it would certainly not be my pride to become a politician.
Organisations known as “Political parties” are at the root of a tremendous amount of problems that human civilisation faces, since it involves dividing the people into segments that fit their policies into left, centre and right. So, I would never want to be seen as a “politician”, but rather a leader of human beings without any party affiliation because they impose too much on the creative vision of a great leader and leads to far too many concessions to please donors and satisfy financial motives that are not truly for the benefit of the nation and country. I believe in science and philosophy and see people as organisms of a system that we must find a way to synchronise to achieve the dream of a noble and sophisticated civilisation. Even the logic of my Organic Theory leads to the same conclusion.
So, today in 2021, I have been able to reach minds and hearts among the people through the amazing technological tools that our modern civilisation has given us, and perhaps 200 years ago, building a public reputation and a name for oneself as a leader would be impossible without a party, donors and funds.
Yet, in order to change the life of people and the system that is used to manage them today, it is sadly not possible without taking the filthy route of politics. So, I cannot say for sure that I will never take this route, since it may be the only route until someone sophisticated and righteous changes the system and sets up a new one that can govern men and bring stability to the management of civilisation while also applying democracy in an optimal way.
Yet, if I ever get into politics, I want the people to know that I will never qualify myself as a politician, but a man who wants to lead his civilisation and his men and women to greatness. The term “politics” and “politician” are today symbols of inadequacy, corruption, nastiness, pettiness, division, selfishness, lies, deceit and so much more that are not for the benefit of mankind.
I will work towards making all this dead history and build a new system.
Today, we are living in a world where corruption is raging and even associations known as the “Free Press” have today been turned into political tools that have absolutely no values or respect for society and its citizens. Of course, I am not saying that all journalists are evil and vile beings because we do have a small section of truly hardworking, noble, genuine and professional writers and columnists out there who are masters in their specialised field, but for the majority they seem to be simply tools of mediocre writing in reporting events and puppets of defamation completely owned by the companies they work for – soulless Sunday scribblers without any literary artistry, love of the written word, depth of thought, vision, style or philosophy. This particular breed of scum tends to throw dirt on people by order and if they do it with me today, tomorrow they will do it with you, your children and the children of your children. Hence, we cannot remain docile as a society if we want to create a fair system and also pass down to our children the freedom that many died for and also the right to rise through their own efforts in a fair and noble society that believes in sophisticated debates and arguments and not mindless bullying and mockery that smothers incredible ideas and diverts attention to petty nonsense. Indeed, I have been at the receiving end of a lot of nastiness from the press who serve their political masters.
The only question that always strikes me when these imbeciles try to mock me is “What could I learn from you?”, meaning what “concrete and intelligent knowledge could they enlighten me with?” Probably nothing much! Most of the time, it is myself who feel like saying “If the limits of your intelligence and brain prevent the comprehension due to the level of the writings, a politely asked question while raising one’s hand seems like a productive move.”. So, it seems fairly obvious that a great metaphor to explain the way I perceive the corrupt, vile and cheap tools of the press, would be an “insect”, yes, in its own circus along with other insects, in a sort of comedy where mediocrity out of frustration is trying to drown noble academic, scientific, philosophical, psychological and logical debate with absolute pettiness. To quote Aymeric Caron: “An earthworm obviously does not have the same relationship to the world as a human being”, and to that I would add that it also does not have the cultural knowledge of the different milieux, the linguistic mastery, the understanding and the perception of the world of a human being. Luckily society has become smarter in 2021 and today smart people know that nothing will smother true intelligence, science, philosophy, psychology and reasoning. In fact, I cannot allow such pettiness to waste my time, indeed I know I am dealing with inferior insects because I have been a fairly known figure to the world for nearly a decade now and they still have not had the guts and the courage to face me in front of a public audience with their trembling voices and their peasant arguments to which I do not believe I would even have to prepare myself – for the majority at least.
So, my arguments are a way of saying that nobility of the mind, intelligence and class will never bow down to frustrated insects. I believe they should also stop dreaming because I owe absolutely nothing to them and their comedic circus. The only domain I owe things to are those of research, psychology, philosophy, literature, poetry and arts and there are books that I am currently working on. It seems that these people may suffer from some mild form of learning disability because they keep repeating debates that have already been sealed, as if constantly throwing their own insecurities at others to see how they react. I have already explained that the insecurities of one person do not affect the whole world, but that person only who may need psychological intervention to evolve into an enlightened being. It is as if they cannot read and understand good science and reasoning, or perhaps they “do not want to understand”. They also fail to realise that every one of their childish attempts to vilify people portrays their insecurity and fear to handle intelligent debates and more and more people are beginning to understand their filthy and abject routine and this may be reflected in the growing amount of people who do not trust the press anymore from all over the world with newspaper stands recently being vandalised by the courageous and defiant “Gillet Jaune” movement of France who gave an example and a tutorial to the sheep crowd of the world on how to stand up to political stupidity and press abuse and idiocy.
Personally, regarding the corrupt press business, I would like for them to understand that they are not at the level or league to lecture or advise me because most of them lack intelligence, culture and language, while I am among and engaging in serious discussions with the minds that award people like them academic qualifications. Yes, I am at the heart of things and I extract documents from renowned academic journals, while being linked to departments in Oxford, London, Paris, Grenoble and even the United States in terms of psychology, mental health, philosophy and society, and I explain to them how to build, educate, cultivate, improve themselves, manage their lives, stress, perceptions, behaviours, relationships, careers and how to raise their children. So, my message to these vile people is that throwing dirt all over the place will not have absolutely any impact of science and psychology, it is a waste of time and energy from them that could be invested appropriately in another activity [e.g. jogging to lose weight], because the life of an individual has never been, and will never be defined by the desires and inventions of pathetic, outdated and misinformed minds. Indeed, it seems that only an organism with the intelligence of a donkey could create lies like them, then believe in their own lies and dance to them, this is absolutely senseless and I believe that they should stop acting like 10 year old children.

Image: A newspaper kiosk (1955) / Photography by Saul Leiter
I am not the first one and definitely not the last one to point out that when mediocrity and the institutions that have built a business and a superficial community around it governs, the geniuses will suffer and be considered as dangerous, Honoré de Balzac also believed that thoughts, genius and talent were always what mattered most. Balzac in his writings also indicated how those with genius in them will be in advance on their times and will be misunderstood and see the present as a soulless palace where genius is unknown such as in Balzac’s “le chef d’oeuvre inconnu” although well known remains unknown. Honoré de Balzac competed with the painters of his time, and wanted to collect and reunite all literary genres just to give an idea of all the things a writer could do with his time, and two important themes of his were faith and the power of literature; faith in the possibility to find solutions to the apparent impossibilities was the purpose of his literature, inventing fictions that would eventually turn into reality because the characters exist due to an act of faith and speak of topics that before did not occupy the consciousness of society. Indeed, we both seem to side with the belief that revolutionary ideas are a result of the development of society. Even more coincidental, Balzac also thought that the society of his time had gone off-track and it was his duty to solve the problems, explaining to the press how incredible he was.

“Headline News” par Vladimír Takáč (2013)
Balzac likened contemporary society to a heartless woman who hurts those who love her, and contrasted it to a woman with heart and soul. Yet as Balzac described the illnesses of society, he also provided the solutions to cure them, and one of the main characteristics of Balzac is the custom of society that he compares to the exterior of a cathedral, and on the other hand the philosophy of society that he compares to the interior of the cathedral, and it is only after this initiation that we are able to reflect and dream with Balzac. This is one of the great contradictions of all works that are monumental and gigantic: the majority of people only read it in part. Hence, he believed that the genius will always encounter problems because it is impossible for the majority of the mediocrity to understand everything instantly: we need time for ideas to diffuse and be fully understood.

Image: Donkeys
The fact that we do not see anything in a work of art does not mean it is not amazing, because it may simply shift to the other side of the limits of a certain period of history. In the 19th century we had many artists who were not known because they were ahead of their time. As a Christian symbolism, Balzac thought that the great artist because of the weight of his genius would suffer for his art and for the rest of the world, the same artist who has the whole world in his limitless workshop where man is a microcosme. « Ayant les oreilles pour écouter le chant des anges… croyant exprimer la musique du ciel a des auditeurs stupéfaits… » and « …en regrettant que vous ne saisissiez pas la plume à une époque ou les gentilhommes doivent s’en servir aussi bien que leurs épées afin de sauver leur pays… » [French for: “Having ears to listen to the song of angels… believing to express the music of heaven to amazed listeners…””…regretting that you did not grasp the pen at a time when gentlemen must use it as well as their swords to save their country…”]; under this beautiful language hid a common phenomena in the 19th century, that of collaborative writing where the author is the director of a great literary enterprise that would cover the whole of France [and eventually the world] while adding his personal touch. One of the main themes of the intellectual movement of the Romantics is that literature is the equivalent of nobility; the pen is what replaces the ancient sword and this found expression in the confused literature of the 19th century. The sword of the academician is the symbol of this essential theme of the replacement of the ancient nobility by the writer [being part of the romantic school of thought is considered to be a replacement for the ancient nobleman]. Fairly unchanged since the times of Balzac, the king is still only a representation of the mediocre middle class: he no longer represents the most intelligent, courageous, sensitive, loving, etc. The middle-class king represents the average intelligence of mediocrity and the average courage [put between the bravest and the most cowardly]. Hence, the contemporary era is the era when the genius artist is the most unfortunate, as Balzac also pointed out. We saw this theme being explored in “Gambara”, where a genius musical artist was too talented to be understood in his time: if his works had been presented to the mediocrity of the majority, they would have failed, since only the genius listeners would have understood, so for Balzac, the genius was forced to lower his supreme talent to please the mediocrity of the majority – Balzac saw this as a form of prostitution for the genius.

The Right Panel representing “Hell” from “The Garden of Earthly Delights” (1490 – 1510) by Hieronymus Bosch, oil on oak panels, 205.5 cm × 384.9 cm (81 in × 152 in), Museo del Prado, Madrid
Balzac wanted to make crude souls understand what poetry is and presented Meyerbeer’s opera “Robert le diable” as the opera of Satan representing all this mediocrity that prevented things from progressing and moving forward, the genius of evil, and in the words of Michel Butor, “the great ape who disfigures the works of God”. To conclude, Balzac thought that the democracy of his time was not adequate for the genius because it was an unequal society who could only give a game to the genius that would leave him with no other solution than to turn against the society that he is a part of and hence this transforms the society into one that can only function if the genius is dead – this is not logical or acceptable because it is the genius who contributes most to the construction of society. We see this in “L’enfant maudit” where the child who was believed to be cursed would go to invent a new science and develop his genius: (i) a naturalist genius because of his relation to the flowers, (ii) a poetic genius because of his relation to the sea, (iii) a genius of love because of his relation to the girl, and (iv) a scientific genius because of his relation to the natural world and botany. “L’enfant maudit”: A creature between God and Man, a genius who would be masculine but also with a feminine sensibility, that Balzac described as a child for his sensibility and as a man for his science, where the ocean was a reflector and the laboratory of inner affectivity, immense, infinite. To Balzac, the genius is cursed, and the more amazing he is, the more he will be misunderstood by the mediocrity of his time. Despite being known as a genius of realistic literature, Balzac loaded his texts with dreams and fantasy [as in Perrault’s tales] since realistic literature is part of fantastic literature, which is always interpreted in a symbolic way. Realistic literature results in a transformation of history [and therefore has the effect of a lightning strike] and the general knowledge that results from this strike motivates society and the world to change. Balzac firmly believed that literature and painting were a way to build stronger skin, that love was an art, and that Dante was the genius of love.

Honoré de Balzac (1799 – 1850)
“Tragedy warms the soul, lifts the heart, can and must create heroes.”
-Napoleon
Thus, coming from a background of literature, philosophy, psychology and sensible thinkers, I must say that since I began engaging with the public, the press and mediocre politicians of our times in 2012 until now, I, like Cécile Guilbert, have been completely disgusted by the “bassesse du courtisan” [lowliness of the courtier], but also shocked to discover the reality of the atavistic system used to manage society [and which forms perception, behaviour, and the mundane reality of the majority] which is designed in such a way that it allows itself to become the theatre of mediocrity by selecting the people without adequate knowledge and a great amount of grotesque, frustrated & vile minds with the baseness of a bitter peasant along with the values of a cold-blooded reptile to be the heads of its various departments when they barely understand the inner and outer life of individuals and how to foster creativity, innovation and progress while achieving balance, harmony and stability for human civilization, what I would call in three words, “joie de vivre”.
It must also be demoralising to most sophisticated minds out there to see this repetitive and mundane cycle every couple of years when another bunch of bureaucratic primates take over the system to then impose their economic values and tastes even if no change is required. The imperfect system of democracy and political parties implies that the opposition must always be wrong and the former group can never do a decent job – this is quite irrational! To believe that these mediocre middle-class parvenus, without any classical foundation and education, will be able to lead human civilization to harmony with their mechanical education and economic policies, is similar to believing in superheroes in spandex. These people should be placed in a financial department not at the centre of civilization. The economy should work to improve and sophisticate human existence and civilisation not the other way round.

Pigs of Democracy from George Orwell’s « Animal Farm » animation (1954) / « La Ferme des Animaux » de George Orwell (1954) / Orwellians still find inspiration from the story as can be seen from this Trump-like pig creature published recently on Mediapart | [NOTE: The full movie can be viewed here]
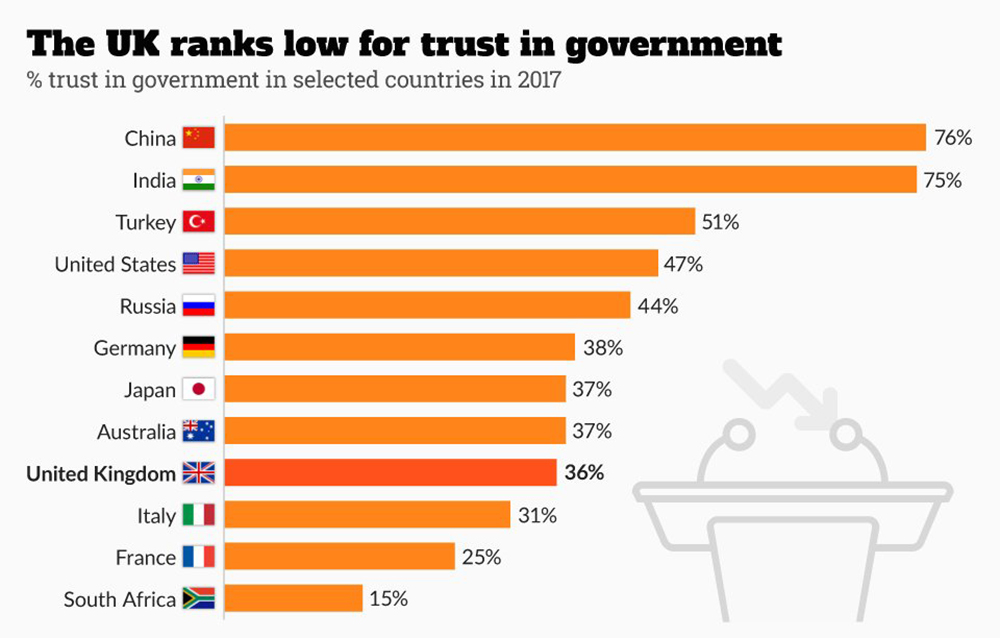
A New Era for Management may be near: UK & France rank low for trust in government / Source: Statista
I find it shocking that this atavistic system of democracy that George Orwell depicted in his Magnum opus, “Animal Farm (1945)” – a text that marked me as a literature student in my teenage years – is actually something that us human beings must accept as being the absolute replacement of Caesar, Alexander the Great, Napoleon, or Seneca. We, the most intelligent primates on the planet, at the top of the food chain, we who have created men such as Napoléon, Balzac, Sartre, Darwin, Descartes, Delacroix, Bourdon le peintre, Vivaldi, Chopin, Verne, Lacan, Pasteur and have invented satellites, computers, ingenius softwares that create almost everything, pianos and sophisticated mobile devices, we amazing people, have come to accept and impose on ourselves a horrorific and unstable organisation of inadequate and ignorant office workers to run and manage our civilisation and lives? I still have trouble to believe this nightmare, because all of our mythical leaders had strong classical education, and hence had an early psychological understanding of what drove life forward and what creates noble minds with values among men and women, and hence what creates a harmonious and glorious civilisation. Napoleon’s empire was founded and mainly focussed on strong French sentiments, values, ideals and ideas, not simply financial motives and business perspectives, which was a mere fraction of the whole. Alexander the Great had a philosophical education and studied the great tragedies with Aristotle himself and was considered as a god or a man who was as close as possible to god, a friend of humanity who changed the whole world, believed in mankind and proved it by adopting miserable tribes to create an empire where everything became possible. Alexander showed that the world could be governed by one leader for the wellbeing of all his subjects. But more importantly, Alexander’s empire was not founded on land or riches but on ideas just like Napoleon’s: the Hellenistic idea of a civilisation open to everyone. Alexander carried an immense dream with the passion of eternal youth, completely convinced that our collective forces and imagination could take us to levels once thought impossible; where surpassing onself became easy. As for Seneca, he was a statesman with strong values and philosophical orientations who embodied the nobility of mind and vision of the great emperors, and was clearly not to be compared with today’s political horror show of mediocrity and lowliness with simple minded animalistic parvenus who graduated in some mechanical and business field and are deluded in their abilities and hopes of being seen as the emperor of the modern world. All systems show their age and weaknesses through time, and we have reached the limits of the pig-like politicians as depicted by George Orwell to manage our society.
People out there should ask themselves the very honest question while looking into the eyes of these pathetic, uncreative and average regional representatives elected by a mass of questionable intelligence and culture: “Does this head look like an empire builder?” [i.e. does this common average brain have the nobility of mind, the values, the tastes, the finesse, the philosophy, the evolutionary creativity, the aesthetic and architectural vision, the feelings, the heart, the honesty, the courage, the passion, the will of steel, the sensibility, the poetic wit, the arguments of a winner, the confidence, the resourcefulness, the dedication, the psychological and psychical understanding of human beings and their needs, the scientific facts, the knowledge, the analytical and debating skills, and the economic ingenuity to create a human empire that the great human race deserves? An empire that will last an eternity, generate a humane and positive atmosphere that pushes us to exceed ourselves, foster our development, create an enjoyable existence and expand into space?] The truth is most of the politicians alive today do not have the passion of our the great historical leaders, because they are the product of a generation of impotent bureaucracry, cowardice, mediocrity, arrogance, lowliness, bully, gossip, corruption, vice, cheap luxury and greed for money. They are not those who saw themselves as the replacement of noble empire builders, men of words, finesse, intellect, values and philosophy, who spent their days and nights thinking independently about the vision of a massive human empire and how to truly find stability and optimise the human race for a harmonious existence that is meticulously calculated and engineered to be timeless with a system that addresses and solves our problems even if it does not match the current model of politics; but are instead simply pathetic office workers who see themselves as men who want to be seen as important simply for being in a political party and showing their funny faces on the common press mainly owned and orchestrated by Jews who use it as a cheap theatre where they command their employed slaves to generate an atmosphere and trigger the types of disputes that suits them, their agendas, and that of their political masters.
“The fool has a great advantage over the man of thought: he is always happy with himself.”
-Napoleon
An elite psychology theorist who deals with behaviour and brain sculpture at the granular level will not listen to the absurdities of a simple mind, even if the partners of this simple mind can pay all the advertisers in the world to publish their nonsense on toilet paper, cereal boxes, the cheap animal press to bus stops. We are above that! Every time a drugged publisher from an obscure corner of the Internet creates a title with an image he considers degrading, it has no effect on us, none, zero; with his sweaty, sticky fingers slamming on a dirty keyboard on the 10th floor of an old building in a crowded corner of a polluted urban jungle? We are above these little defamation campaigns organized by childish politicians and the Jewish media they love so much.

According to a report by the Reuters Institute, only 24% of French people trust the information provided by the media. This is 11% less than in 2018 / Source: Liberation
It cannot be anti-semitic to simply state that the majority of the press in owned, and hence controlled by Jews. My message to these people is: “Try to grow up! Not a single intelligent person in the world is defined by your impulses… you are worse than children. People define themselves… simple….. your opinions, they’re just simple opinions as simple as your mind!” I think that since we are on the subject, it must be recognized that Jews and their obsession with controlling the media and corrupting decision-makers with their money, and hence causing frictions and other strains on societies and governments to impose their views, in most European countries where they have spread to, is not a new practice for them, they have been doing it for centuries, and it may also be a good time for the learned and sensible Jews out there to try to guess what may have motivated Hitler’s Reich’s decisions to return them all to Israel; surprisingly even the Jewish Rabbi Yosef Tzvi Ben Porat thought that Hitler was right to hate the jews for what they do. Moreover, the vast majority of mediocre politicians and their propaganda partners do not consider themselves as empire builders because they do not have the ingenuity to do so, they are not even creative enough to have noble and sophisticated discussions, or to question the ageing system and dare to consider that there might be something better, because these men are not at the intellectual level to think like a reformer and creative innovator. They simply do not have the mental power and intellectual prowess to challenge an old man-made system: they cannot engineer reality because it is beyond their understanding – they themselves have never even questioned their own existence or purpose but have simply followed and copied the past mediocrities whose life they are trying to replicate uncritically. These ignoble creatures see themselves as the members of a political group with a one-sided perspective and do not have the creative skills and wisdom to think independently and take the responsibility for the construction of an eternal human empire; they are only thinking for the short term, i.e. How to win an election? How to please the leader? How to win the next election? How to be selected to be in charge of a ministry? How to speak to the journalist? How to keep the people voting for them? How to harass their opponents in sometimes the most childish of ways? These men are parvenus, what I would describe as savages of luxury who wear a suit for their profession and environment, but inside their rotten minds they could be compared to bitter peasants for their simple minds, behaviour, vision, ignorance and petty childish arguments.

Solon defends his laws against criticism from Athenian citizens, painting by Noel Coypel, 1699
Democracy and the political system are not divine creations, but just like everything else requires updates, revisions and re-organisation to become a more sophisticated and reasonable system that can offer us a harmonious human empire where everyone can dream and achieve; but also “live” and not simply exist while being dead inside. Some in politics also seem to feel the pain of an outdated system, for example Claire Nouvian who has just put an end to her political life by admitting the shortcomings in implementation and the human dysfunctions of the political machine, and I think she did well to quote Mauroy, “when the disgusted leave, all that remains are the disgusting”, and to leave stating “My expectations of honesty and courage are not compatible with political shenanigans,” explained Claire Nouvian,”I am the one who is unsuited to this environment”.
It is clear not only to the best intellectuals and thinkers of our era but also to the scientifically, culturally and literarily conscious section of the public, that the media today prefer conformist mass mediocrity rather than to invite the elites or the best of our time; I think it is dangerous for civilization because, as Yeats said, “education is not the filling of the pail, but the lighting of a fire”, and as Einstein also said, “education is not the learning of facts, but the training of the mind to think”, and the Jewish mass media gives us the thoughts and vision of conformist mediocrity. These false, atavistic and corrupt media seem to prefer the boring and ill-informed mediocrity that they force us to consume in the form of debates and opinions of empty bureaucrats without a credible sense of reasoning – cheap junk in silk, suit and tie.
At the moment, I am focused on writing my books, since I believe they contain a great amount of fundamental, life-changing and pivotal discoveries and innovations to the psychology, philosophy and values of our current fragmented and confused civilisation. Once, they are published for a wide audience, ranging from the young to the old, I believe they will have introduced my vision, train of thought and direction to the masses. To me, it is fundamental that the people understand my mind and heart before they can see me as a possible leader, because I want people to trust me based on the contents of my brain, and not for my popularity or for my face being on petty papers and their streets through the power of the purse of immoral donors with the sole intention to bleed the people, enslave the state by tuning it to their agenda for their bank accounts. This does not mean that I am against business or stand for a weak economy! Of course, I want a strong economy, but I also firmly believe that good business can be completely ethical by respecting the sensibilities of the people and the environment. There are decent businessmen out there who are successful and have achieved their dream while also being ethical, moral and righteous. Business can be noble when done with the right values, and does not need to be done at the expense of the people’s blood, and many savage businessmen today still do not seem to understand this and they find ways to infiltrate and destroy the system by corrupting immoral politicians who cannot resist the taste of dirty money. This leads to suffering, and a system without any humanity, and I am against these scenarios because my aim is harmony across the system and I know that it can be achieved with the right leader, the right minds, the right hearts and the right values.
So, I hate the term politics, and for the time being I am focussed in my duty of enlightening and guiding civilisation through my intellectual work. My aim is to change the system and re-organise it into something stable, efficient and honourable while making the life of the people better, happier and more sophisticated. I cannot tell if the future will force me into the world of politics, but I will never portray myself as a politician, and this is something I want the people to know and embed in their minds and hearts. If I am forced into politics, it would be to change it forever, and even bury the term politics and politicians to create something bigger, better, nobler, more stable, grander, and truly sophisticated and civilised.
So, your answer to this question seems one that only time can tell.
“We lead the people only by showing them a future: a leader is a merchant of hope.”
-Napoleon
_________________________________
QUESTION IX.
[FR] – Si vous avez la possibilité de le faire à l’avenir, quels changements proposeriez-vous pour un meilleur système de gestion de l’État ?
[EN] – If you have the chance to do so in the future, what changes would you propose towards a better system of management for the state?
[FR] Réponse:
Le modèle actuel du système atavique utilisé pour gérer nos sociétés est à l’origine de toute l’instabilité parce qu’il impose une rotation injustifiée et obstinée à de nombreux départements qui serait stable si ils était entièrement gérés par l’Etat lui-même par l’intermédiaire d’un expert en la matière sans aucun apport politique sauf les suggestions du chef d’Etat ; notre système actuel change toutes les 5-6 années quand un département pourrait être totalement stable sans ce changement.

“History has for sewers times like ours.” -Victor Hugo
Quand nous mettons en œuvre une nouvelle politique, cela ne commence jamais de manière stable, cela prend du temps, mais aujourd’hui nous avons une structure politique qui impose que chacun de ses départements soit repris par un nouveau cerveau tous les 5 ou 6 ans ; dans la plupart des cas, ce nouveau cerveau n’a aucune expérience ou passion pour le domaine spécifique du département mais sont surtout des diplômés en affaires et en gestion qui ont passé des années à amasser des fonds [ex. travailler pour des entreprises étrangères au Moyen-Orient], en bavardant en costume devant une machine à café [comme dans la série Caméra Café de Bruno Solo], et qui viennent ensuite passer leur temps libre dans un groupe politique avec une perspective unilatérale [de la vie sur Terre] qui leur remet un département après leur élection, et au lieu que le système s’appuie sur sa propre expérience et ne s’ajuste que par lui-même pour éliminer les erreurs et être synchronisé avec la philosophie principale de l’Etat, il permet plutôt à ce cerveau complètement nouveau, avec une perspective complètement nouvelle pour tout régler à son agenda toutes les quelques années – ce qui plonge les départements des États dans l’instabilité dans un cycle sans fin et a un impact sur tous les aspects de la société et la vie de ses habitants – sans parler du fait que ces cerveaux ont aussi des programmes personnels et financiers et ne sont donc pas guidés par une philosophie qui se concentre uniquement sur l’expansion et les priorités de l’État et l’amélioration des conditions de vie de ses citoyens.
“Le mot de “vertu politique” est un non-sens.”
-Napoléon
La démocratie était un mouvement visant à éliminer ceux qui abusaient du pouvoir pour créer un système où le peuple a son mot à dire dans la gestion de sa société, mais aujourd’hui, ces serviteurs présumés loyaux du peuple ont divisé la société [en sections qu’ils appellent gauche, droite et centre] et ont pris le pouvoir des empereurs et l’ont divisé en de si petits morceaux qu’il est devenu une poussière.

Image: Napoléon le génie impérial VS Une masse d’eunuques politiques
Cela a créé toute une congrégation d’eunuques politiques où personne n’a de pouvoir sérieux et ralentit plutôt notre évolution en raison du nombre excessif de procédures nécessaires pour déclencher le progrès, le changement systématique et l’avancement. Nous devons nous rappeler que le pouvoir lui-même ne cause aucune souffrance, c’est le pouvoir entre de mauvaises mains et appliqué par de mauvais cerveaux qui cause la souffrance. Il est peut-être juste de citer ici le regretté Christopher Hitchens : “Nous pouvons nous habituer à certains dangers et ne pas les reconnaître avant qu’il ne soit trop tard”.
Je crois fermement qu’il serait raisonnable pour nous de reconsidérer sérieusement l’importance et l’efficacité du pouvoir lorsqu’il peut être utilisé avec une liberté créative raisonnable par le cerveau convenable [un cerveau supérieur mène à une vision et une gestion supérieures], et comment choisir ce cerveau ingénieux pour diriger le navire de l’humanité sur la bonne voie vers un empire glorieux et harmonieux avec une démocratie révisée et appliquée correctement, afin qu’elle ne divise ni le peuple et n’accepte aucun groupe politique ayant des perspectives unilatérales de politique générale atavique où la corruption est présente puisque les groupes ont tendance à influencer des individus faibles et nous avons tiré les enseignements de l’expérience que dans les groupes politiques, habituellement, c’est pour le pire.
Le nouveau système ne devrait pas permettre aux partis politiques d’exister, mais devrait se concentrer uniquement sur les individus ayant des valeurs impériales ; l’État devrait jouer un rôle important en veillant à ce que ces individus aient les ressources et les voies d’accès nécessaires pour être considérés comme le chef d’un empire démocratique en réglementant strictement ses propres élections pour sa propre sécurité et stabilité.

Traduction [EN]: “When a government is dependent on bankers for money, it is the bankers and not the government leaders who are in control, since the hand that gives is above the hand that receives. Money has no homeland; financiers have no patriotism and no decency; their only objective is profit.” – Napoléon
Ce processus électoral réglementé par l’État mettrait également un terme à cette épidémie continue de riches sauvages [et d’autres employés de banque et de riches marchands de pommes de terre, de lardons, d’huile et de carburant] sans finesse et sagesse; des primates commerciaux incultes qui sont les cibles des groupes politiques, pour prendre le pouvoir dans certains pays, détruire ceux-ci et générer l’instabilité toutes les quelques années, à cause de leur manque de créativité, de connaissance et de vision, de leurs équipes, de leur agenda grotesque, de leurs programmes et de leur manque d’ingéniosité.

« Il n’y a ni justice ni liberté possibles lorsque l’argent est toujours roi. » – Albert Camus [French for: “No justice or freedom is possible when money is always king.” – Albert Camus]
Albert Camus l’a magnifiquement formulé quand il a dit : “Il n’y a ni justice ni liberté possibles lorsque l’argent est toujours roi.”. Une déclaration qui pose à juste titre la question : Un homme jugé apte à devenir le chef d’un État ou d’un empire doit-il être évalué en fonction de son compte en banque et de sa capacité à se joindre à un groupe de politiciens ayant la même perspective, ou doit-il être évalué en fonction de sa vision, de sa créativité, de son honneur, de sa sagesse, de son intelligence, de son originalité, de son esprit, de son style individuel et de sa maîtrise des facultés de discussion, de débat et d’expression ?
La nouvelle structure créerait également un système dans lequel les chefs des différents départements seraient des individus indépendants sans aucun groupe ou affiliation politique et leur permettrait de se concentrer sur leur agenda professionnel et leur héritage sans être distraits par un environnement social corrompu ; ils apprendraient également à prendre la responsabilité de leur propre travail et ne se cacheraient pas derrière un groupe politique pour supposer que quelqu’un parmi eux trouvera une solution aux problèmes alors que chacun d’entre eux espère la même chose – c’est comme regarder un groupe de saumons se rassembler pour échapper à un prédateur marin. Ces représentants régionaux élus devraient être utilisés comme des ambassadeurs de leur région, rien de plus. Il est impératif que nous commencions à nous orienter et à orienter le système vers ce modèle de gouvernance dynamique et efficace, et plus vite ce sera fait, mieux ce sera pour l’humanité.
« Chaque fois que j’entends un discours politique ou que je lis ceux de nos dirigeants, je suis horrifié de n’avoir, pendant des années, rien entendu qui ait semblé humain. Ce sont toujours les mêmes mots qui racontent les mêmes mensonges. Et le fait que les hommes acceptent cela, que la colère du peuple n’ait pas détruit ces clowns creux, me paraît la preuve que les hommes n’accordent aucune importance à la manière dont ils sont gouvernés ; qu’ils jouent – oui, jouent – avec toute une partie de leur vie et leurs soi-disant « intérêts vitaux ». »
-Albert Camus
Je pense que nous vivons l’époque d’une révolte citoyenne progressive pour un nouveau système où la démocratie n’est pas appliqué d’une façon qui permet aux sauvages bureaucratiques des communes d’accéder au pouvoir et ensuite de détruire la civilisation moderne. Nous avons besoin d’un nouveau système [régime] avec une constitution écrite et des départements indépendants qui mettent l’accent sur ses propres organismes [ceux qui s’identifient complètement à la nation], sa stabilité, son expansion et sa longévité. La démocratie ne devrait être utilisée que pour choisir de manière indépendante [sans affiliation politique] le chef de l’Etat qui orchestrera tout le système; et ensuite de façon moins importante, pour sélectionner des représentants régionaux [qui seraient les ambassadeurs de leur région] et ne seront pas transformés en chefs de département dont ils n’ont aucune connaissance dans les matières concernées. Les ministères seraient convertis en des départements indépendants pleinement fonctionnels gérés par des experts dans leurs domaines respectifs et maintenus par l’Etat lui-même sans aucune influence extérieure, à l’exception des suggestions du chef de l’Etat. Parce ce que aujourd’hui avec les grossiers des communes qu’on place dans des positions de pouvoir au delà de leurs comprehension pour prendre des départements qu’ils ne comprennent pas, on se retrouve en tant que citoyens honnêtes avec de l’instabilité dans nos sociétés sans harmonie et nos vies privées violées. La grande majorité de ces malfrats de bureau dans la politique n’ont pas de grandeur d’esprit, de morales, ou de philosophie pour leur rappeler que leur devoir c’est de prioriser la population et le pays.
“Il y a des gens qui se croient le talent de gouverner par la seule raison qu’ils gouvernent.”
-Napoléon
Le moment du grand changement et de la grande révolution approche, et j’ai l’intention de la guider pour une civilisation digne de coloniser l’univers. En effet, des mouvements comme les Gilets Jaunes en France rappellent au monde qu’il y a encore des gens qui sont prêts à donner leur vie pour combattre la corruption, l’arrogance, l’injustice, les médias enfantins et la politique du mal. Il n’est pas surprenant qu’ils aient dû être français et rappeler aux gens du monde entier le courage qui accompagne notre héritage et les limites que nous sommes prêts à repousser au nom du changement et d’un monde meilleur.
“On ne peut pas faire semblant d’être courageux.”
-Napoléon
Je vais devoir terminer cette réponse ici, car je dois aussi garder quelques idées pour plus tard m’adresser directement au public, car depuis 2012, j’ai lu, entendu et vu la plupart de mes idées être prises et reproduites dans tous les médias et le spectre politique mondial ; je me sens donc comme Jean-Paul Sartre à un moment de sa vie où il était devenu le professeur national de philosophie de toute la France, où ses pensées philosophiques et ses valeurs avaient été diffusées partout dans le paysage culturel, médiatique et politique, et que, même ceux qui ne l’avaient jamais connu, étaient inconsciemment influencés par son héritage intellectuel, car les différentes formes de médias qu’ils consommaient l’étaient.
Dans l’essai “Histoire de la philosophie occidentale, des cultures religieuses, des sciences, de la médecine et de la sécularisation“, je crois que j’ai fait comprendre clairement, par divers faits provenant de divers domaines, que le monde a changé grâce aux progrès et aux découvertes philosophiques, psychologiques et intellectuelles, et que les humains devraient continuer à changer avec lui. Il me semble que le changement est en train d’arriver progressivement.
—-|—-
[EN] Answer to Question IX. “If you have the chance to do so in the future, what changes would you propose towards a better system of management for the state?”
The current model of the atavistic system used to manage our societies is at the root of all the instability because it imposes an unjustified and stubborn rotation on many departments that would be stable if it was completely run by the state itself through an expert in the field without any political input except suggestions from the head of state; our actual system forces change every couple of years when a department could be completely stable without it. When we implement a new policy it never starts in a stable manner, it takes time for this, but nowadays we have a political structure that imposes the requirement for each of its departments to be taken over by a new brain every 5 or 6 years; in most cases this new brain does not have any experience or passion for the specific field of the department but are mostly business and management graduates who spent years amassing money [e.g. working for foreign companies in the Middle-East], who then come to spend their free time in a political group with a one-sided perspective [of life on Earth] that hands over a department to them after being elected, and instead of the system building on its own experience and only fine tuning itself to cancel out errors and be synchronised with the main philosophy of the state, it instead allows this completely new brain, with a completely new outlook to shift everything to his agenda every couple of years – this shakes the departments of the states continuously into instability in a never ending cycle and has an impact on every aspect of the society and the lives of its people – not to mention that these brains also have personal and financial agendas and hence are not guided by a philosophy that focuses solely on the expansion and priorities of the state and the betterment of its people’s lives.
“The word “political virtue” is nonsense.”
-Napoleon
Democracy was a movement to remove those who abused power to create a system where the people have an input in the way their society is managed, but today these supposedly loyal servants of the people have divided society [into sections that they call left, right and centre] and have taken the power of emperors and fragmented it into such tiny pieces that it has turned into dust. This has created a whole congregation of political eunuchs where no one has any serious power and instead slows down our evolution because of the excessive amount of procedures required to trigger progress, systematic change and advancement. We should remind ourselves that power itself does not cause any suffering, it is power in the wrong hands and being applied by the wrong brains that causes suffering. It may be right to quote the late Christopher Hitchens here, “We may become habituated to certain dangers and fail to recognise them until it’s too late.”

I firmly believe that it would be sensible for us to seriously reconsider the importance and effectiveness of power when allowed to be used with reasonable creative freedom by the right brain [a superior brain leads to a superior vision and management], and how to select this ingenious brain to steer the ship of humanity on the right path towards a glorious and harmonious empire with democracy revised and applied properly, so that it does not divide the people or accept any political groups with one-sided perspectives of atavistic mainstream politics where corruption lives, since groups tend to influence weak individuals and we have learned from history that in political groups it is usually for the worse.
The new system should not allow political parties to exist, but should solely focus on individuals with imperial values; the State should play a significant role in ensuring that those individuals have the resources and the routes to be considered as the head of a democratic empire by strictly regulating its own elections for its own security and stability.
“When a government is dependent on bankers for money, it is the bankers and not the government leaders who are in control, since the hand that gives is above the hand that receives. Money has no homeland; financiers have no patriotism and no decency; their only objective is profit.”
– Napoléon
This State regulated electoral process would also put a halt to this ongoing epidemic of wealthy savages [and other bank employees and rich merchants of potatoes, bacon, oil and fuel] without any finesse and wisdom who are the targets of political groups to take over countries, destroy them and generate instability every couple of years through their grotesque teams, agendas, lack of creativity, knowledge, vision and ingenuity.
“No justice or freedom is possible when money is always king.”
– Albert Camus
Albert Camus beautifully phrased it when he said: “No justice is possible when money is always king”. A statement that rightly asks the question: Should a person deemed fit to become the head of a state or empire be assessed on his bank account and ability to join of a group of politicians with the same perspective, or should he be assessed on his vision, creativity, honour, wisdom, intelligence, originality, wit, individual style, and mastery of discursive, debating and expressive skills?
The new structure would also create a system where the heads of the various departments are independent individuals without any political group or affiliation and allow them to focus on their professional agenda and legacy without distractions from a corrupt social environment; they would also learn to take responsibility for their own work and not hide behind a political group to assume that someone among them will find a solution to problems when every single one among them is hoping for the same thing – it is like watching a group of salmons flock together to escape a marine predator. These elected regional representatives should be used as ambassadors for their region, nothing more. It is imperative that we start start guiding ourselves and the system towards this dynamic and effective model of governance, and the faster it is done, the better for mankind.
“Every time I hear a political speech or I read those of our leaders, I am horrified at having, for years, heard nothing which sounded human. It is always the same words telling the same lies. And the fact that men accept this, that the people’s anger has not destroyed these hollow clowns, strikes me as proof that men attribute no importance to the way they are governed; that they gamble – yes, gamble – with a whole part of their life and their so called ‘vital interests’.”
– Albert Camus
I think we are living in an era of a progressive citizen revolt for a new system where democracy is not applied in a way that allows the bureaucratic savages of the commons to come to power and then destroy modern civilization. We need a new system[regime] with a written constitution and independent departments that focus on its own organisms [those that fully identify with the nation], its stability, expansion and longevity. Democracy should only be used to independently choose [without political party affiliation] the head of state who will orchestrate the entire system; and then, less importantly, to select regional representatives [who would be ambassadors for their region] and will not be transformed into heads of departments in which they have no knowledge in the matters concerned. The departments would be converted into fully functional independent departments managed by experts in their respective fields and maintained by the State itself without any external influence, except for the suggestions of the Head of State. Because today, with the rude people of the commons who are placed in positions of power beyond their comprehension to take departments that they do not understand, we find ourselves as honest citizens with instability in our societies without harmony and our private lives violated. The vast majority of these office thugs in politics have no greatness of mind, morals, or philosophy to remind them that their duty is to put the people and the country first.
“There are people who believe they have the talent to govern for the only reason they govern.”
-Napoleon

“The Reader” by Franz Von Defregger (1835 – 1921)
The moment of great change and revolution is approaching, and I intend to guide it for a civilization worthy of colonizing the universe. Indeed, movements like the Gilets Jaunes in France remind the world that we still have people out there who are willing to lay down their lives to fight corruption, arrogance, injustice, the childish media and evil politics. Unsurprisingly, they had to be French and remind people globally of the courage that comes with our heritage and the limits we are willing to push in the name of change and a better world.
“We cannot pretend to be brave.”
-Napoleon
I will have to end this answer here as I also have to keep some ideas for a later time to address the public directly, because since 2012, I have read, heard and seen most of my ideas being taken and reproducted all over the mediatic and political spectrum globally; hence I feel a little like Jean-Paul Sartre at a moment of his life when he had become the national teacher of philosophy of the whole of France, where his philosophical thoughts and values had been impregnated all over the cultural, mediatic and political scene, so that, even those who had not known him, were unconsciously influenced by his intellectual heritage because the various forms of media they consumed were.

The Private dpurb.com Grey & Orange Code of Honour for the Sensible & Evolved Super Humans Out There
In the essay, “History on Western Philosophy, Religious cultures, Science, Medicine & Secularisation” I believe that we have made it clear, through various facts from various fields, that the world has changed through philosophical, psychological and intellectual progress and discoveries, and that humans should keep changing with it. It seems to me that change is happening gradually.
________________________________
QUESTION X.
[FR] – Vous êtes croyant ? Dans l’affirmative, quelle devrait être, selon vous, la position de la religion par rapport aux questions d’État ?
[EN] – Are you religious? If so where do you think religion should stand in regards to matters of the state?
[FR] CET ARTICLE EST EN COURS D’ÉDITION ET SERA ENTIÈREMENT MIS À JOUR DANS LES ANNÉES À VENIR
Veuillez également noter que nous accordons actuellement la priorité à l’achèvement d’environ 6 livres, ainsi qu’au travail créatif en cours, à la recherche intensive, à la mise à jour, à la synthèse et à l’édition qu’ils exigent [c’est-à-dire la transcription, le référencement, l’organisation, l’esquisse, la structuration et la mise à jour… sans oublier les centaines d’études dans des journaux scientifiques à filtrer].
Ces livres seront publiés pour le public français puis pour les anglophones afin d’en maximiser l’impact. Ils nécessiteront donc également une traduction précise et méticuleuse afin de préserver le sens et la saillance initiale de la langue française vers l’anglais. Parallèlement en travaillant sur ces projets gigantesques, nous révisons et mettons à jour en permanence les ouvrages académiques sur le site web puisqu’ils sont les piliers fondateurs de nos projets.
Nous répondrons également à vos questions et compléterons cet essai lorsque nous aurons le temps d’y réfléchir et de les développer. Veuillez consulter périodiquement le site web pour les mises à jour.
Nous vous remercions sincèrement tous, nos lecteurs, disciples et sympathisants, pour votre loyauté, votre patience, votre compréhension, votre soutien moral passionné, votre confiance et votre gentillesse. N’hésitez pas à nous soutenir par un don [Cliquez Ici] afin que nous puissions maintenir dpurb.com gratuit et accessible à tous jusqu’à la fin des temps.
Ici, l’expression de nos sentiments les plus sincères,
L’équipe @ dpurb.com & Danny D’Purb

Traduction [EN]: “To make a good book, it takes a prodigious amount of time and the patience of a saint.” – Voltaire
—-|—-
[EN] THIS ARTICLE IS CURRENTLY BEING EDITED AND WILL BE FULLY UPDATED IN THE COMING YEARS
Please also note that we are currently prioritising the completion of about 6 books along with the ongoing creative work, intensive research, updating, sythesising and editing that they demand [i.e. transcribing, referencing, organising, sketching, structuring and updating… not to mention hundreds of studies in scientific journals to be filtered out]. These books will be released for the French audience and then for the Anglophones to maximise its impact, and hence will also requires precise and meticulous translation in order to preserve the initial meaning and salience from the French language to English. While working on these gigantic projects we are also constantly revising the academic works on the web site and updating them since they are the founding pillars for our projects.
We will also be answering your questions and complete this post when we have time to reflect and elaborate on them. Please check the website periodically for updates.
We sincerely thank you all, our readers, followers and supporters, for your loyalty, patience, understanding, passionate moral support, trust and kindness. Please feel free to support us with a donation [Click Here] so that we can keep dpurb.com free and accessible to all until the end of time.
Here, the expression of our most sincere feelings,
The Team @ dpurb.com & Danny D’Purb

Traduction [FR]: « Je n’ai écrit aucun livre avant mes 50 ans, et je suis ravi parce que je ne savais pas ce que je pensais avant » – Mary Midgley
*****
Bibliographie
- Berger, P.L. and Luckmann, T. (2022). La construction sociale de la réalité. 3e edn. Malakoff, France: Armand Colin.
- Benaïssa, S. (2023). Classe Bourgeoise : Les parasites de la société. BLAST. Available at: https://youtu.be/VRNTZflvaR4 (Accessed: March, 18, 2023).
- Brouillette, R. (2008). L’Encerclement – La démocratie dans les rets du néolibéralisme. Les Films du passeur. Available at: https://www.youtube.com/watch?v=VyyC7zC4huw (Accessed: December, 1, 2025).
- Dard, O. (2018) ‘« l’homme des machines » de Georges Bernanos’, L’Homme & la Société, n° 205(3), pp. 87–107.
- Dupuy, C. (2016). Journalistes, des salariés comme les autres?: Représenter, Participer, mobiliser. Rennes, France: Presses universitaires de Rennes.
- Gairin, V. (2019). Pourquoi les médiocres ont pris le pouvoir : Le philosophe québécois Alain Deneault fustige un monde où, avec la transformation des métiers en “travail”, le “moyen” est devenu la norme. Interview. Le Point. Available at: https://www.lepoint.fr/debats/pourquoi-les-mediocres-ont-pris-le-pouvoir-16-01-2016-2010535_2.php (Accessed: March, 18, 2023)
- Kelly, M. (2014) French: Precise, romantic, influential, close to English | British Council. Available at: https://www.britishcouncil.org/voices-magazine/french-precise-romantic-influential-close-english (Accessed: January 25, 2023).
- Krumrei-Mancuso, E., Haggard, M., LaBouff, J. and Rowatt, W. (2019). Links between intellectual humility and acquiring knowledge. The Journal of Positive Psychology, 15(2), pp.155-170.
- Molénat, X. (2023) La construction sociale de la réalité. Peter L. Berger et Thomas Luckmann, 1966, trad. fr. 1986, rééd. Armand Colin, coll. « Références », 1997., Sciences Humaines. Available at: https://www.scienceshumaines.com/la-construction-sociale-de-la-realite_fr_13014.html (Accessed: February 14, 2023).
- Pak, S. (2020). La démocratie du dollar. ARTE France. Available at: https://archive.org/details/la-democratie-du-dollar-2023 (Accessed: April 23, 2023).
- Porter, T. and Schumann, K. (2017). Intellectual humility and openness to the opposing view. Self and Identity, 17(2), pp.139-162.
- Rothman, J. and Treffers-Daller, J. (2014). A Prolegomenon to the Construct of the Native Speaker: Heritage Speaker Bilinguals are Natives Too!. Applied Linguistics, 35(1), pp.93-98.
- Russell, B. (2008) Principes de Reconstruction Sociale. Translated by N. Baillargeon and E.de Clermont-Tonnerre. Québec, Canada: Presses de l’Université Laval.
- Sanchez-Palencia, E. (2017). Culture, progrès scientifique et convictions. Méthode Scientifique / Libres propos d’académiciens, Académie des Sciences.
- Savage, J.E., Jansen, P.R., Stringer, S., et al. (2018). Genome-wide association meta-analysis in 269,867 individuals identifies new genetic and functional links to intelligence. Nat Genet 50, 912–919.
- Weil, S. (2017). Note sur la suppression générale des partis politiques. Paris: Editions Allia.
- Woodruff, P. (2022). Majority rule is not democracy, Oxford University Press Blog. Available at: https://blog.oup.com/2022/01/majority-rule-is-not-democracy/ (Accessed: February 9, 2023).
[Notice: If the videos embedded across dpurb.com cannot be viewed from your region, we recommend using HOLA VPN (Click Here, it is FREE!)]
D.J. d’Purb | dpurb.com
____________________________________________________
Bien que le but de la communauté de dpurb.com ait toujours été et sera toujours de se concentrer sur une culture moderne et progressiste, le progrès humain, la recherche scientifique, l’avancement philosophique et un avenir en harmonie avec notre environnement naturel, les efforts inlassables dans la recherche et la fourniture à notre précieux public des dernières et meilleures informations dans divers domaines ont malheureusement leur coût sur nos administrateurs très humains, qui malgré le temps sacrifié et le plaisir de contribuer à l’avancement de notre monde grâce aux discussions sensibles et idées novatrices, doivent gérer les contraintes qui testent même le plus fort d’esprit. Votre précieux soutien assurerait que notre travail demeure à la hauteur de ses normes et rappellerait à nos administrateurs que leurs efforts sont appréciés tout en vous permettant de ressentir une certaine fierté par notre cheminement vers une civilisation humaine éclairée. Votre soutien bénéficierait à une cause qui se concentre sur l’humanité, les générations actuelles et futures.
On vous remercie encore une fois de votre temps.
N’hésitez pas à nous soutenir en envisageant de faire un don.
Sincèrement,
L’équipe @ dpurb.com
____________________________________________________
While the aim of the community at dpurb.com has been & will always be to focus on a modern & progressive culture, human progress, scientific research, philosophical advancement & a future in harmony with our natural environment; the tireless efforts in researching & providing our valued audience the latest & finest information in various fields unfortunately takes its toll on our very human admins, who along with the time sacrificed & the pleasure of contributing in advancing our world through sensitive discussions & progressive ideas, have to deal with the stresses that test even the toughest of minds. Your valued support would ensure our work remains at its standards and remind our admins that their efforts are appreciated while also allowing you to take pride in our journey towards an enlightened human civilization. Your support would benefit a cause that focuses on mankind, current & future generations.
Thank you once again for your time.
Please feel free to support us by considering a donation.
Sincerely,
The Team @ dpurb.com
P.S.
– If you are a group/organization or individual looking for consultancy services, email: info[AT]dpurb.com
– If you need to reach Danny J. D’Purb directly for any other queries or questions, email: danny[AT]dpurb.com [Inbox checked periodically / Responses may take up to 20 days or more depending on his schedule]
Stay connected by linking up with us on Facebook , Twitter and/or Instagram














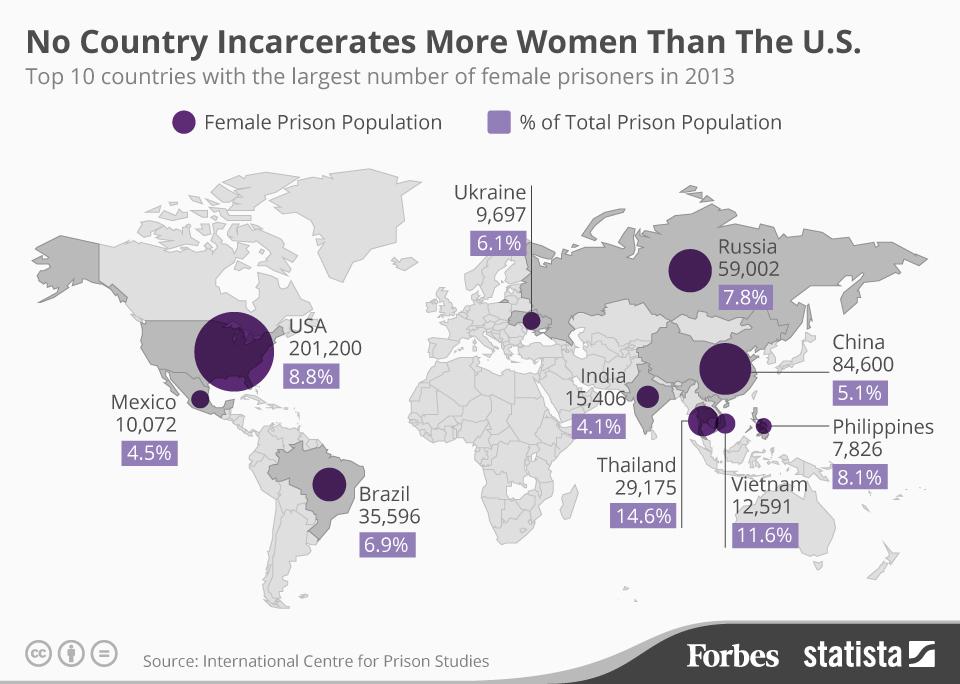








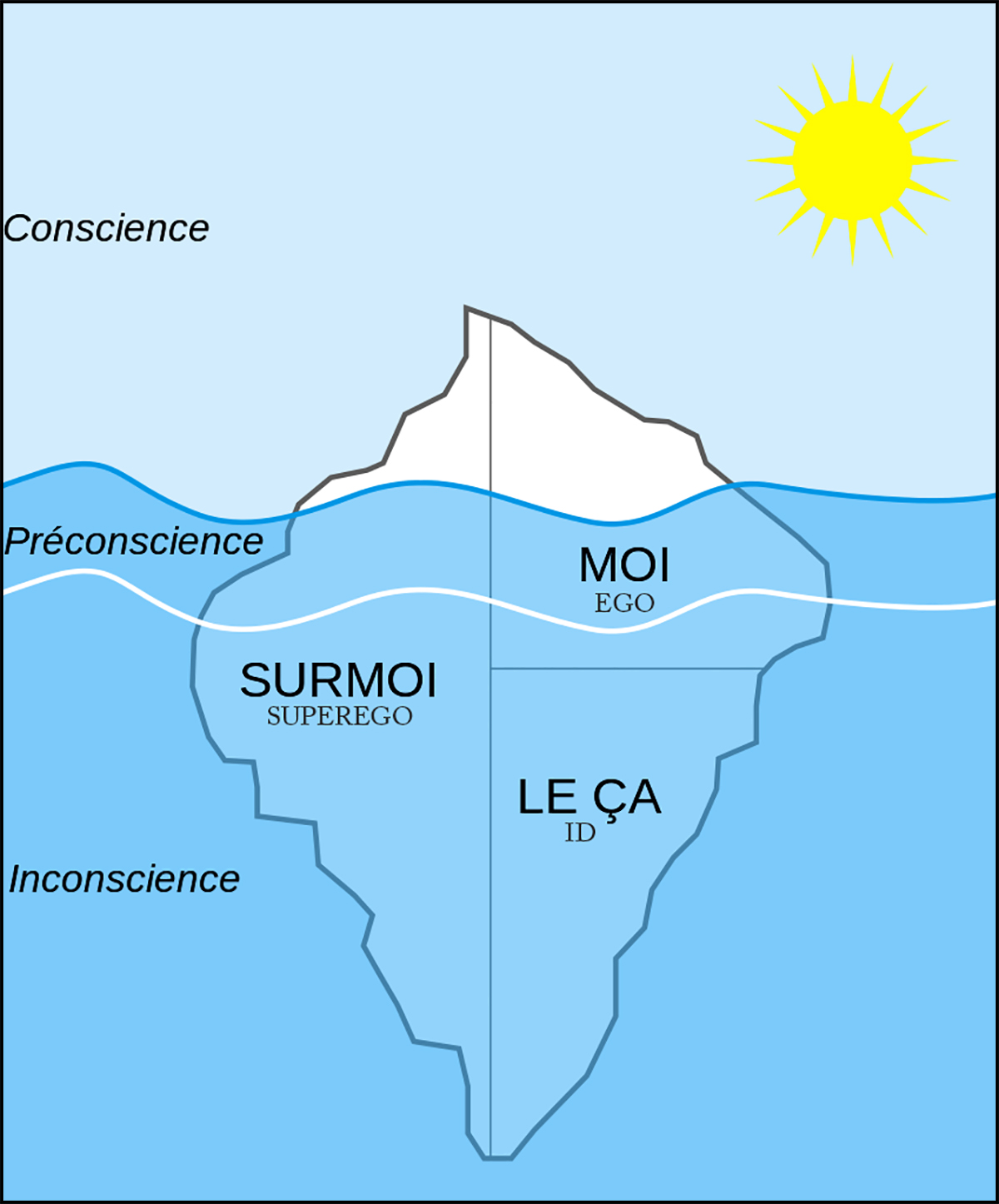




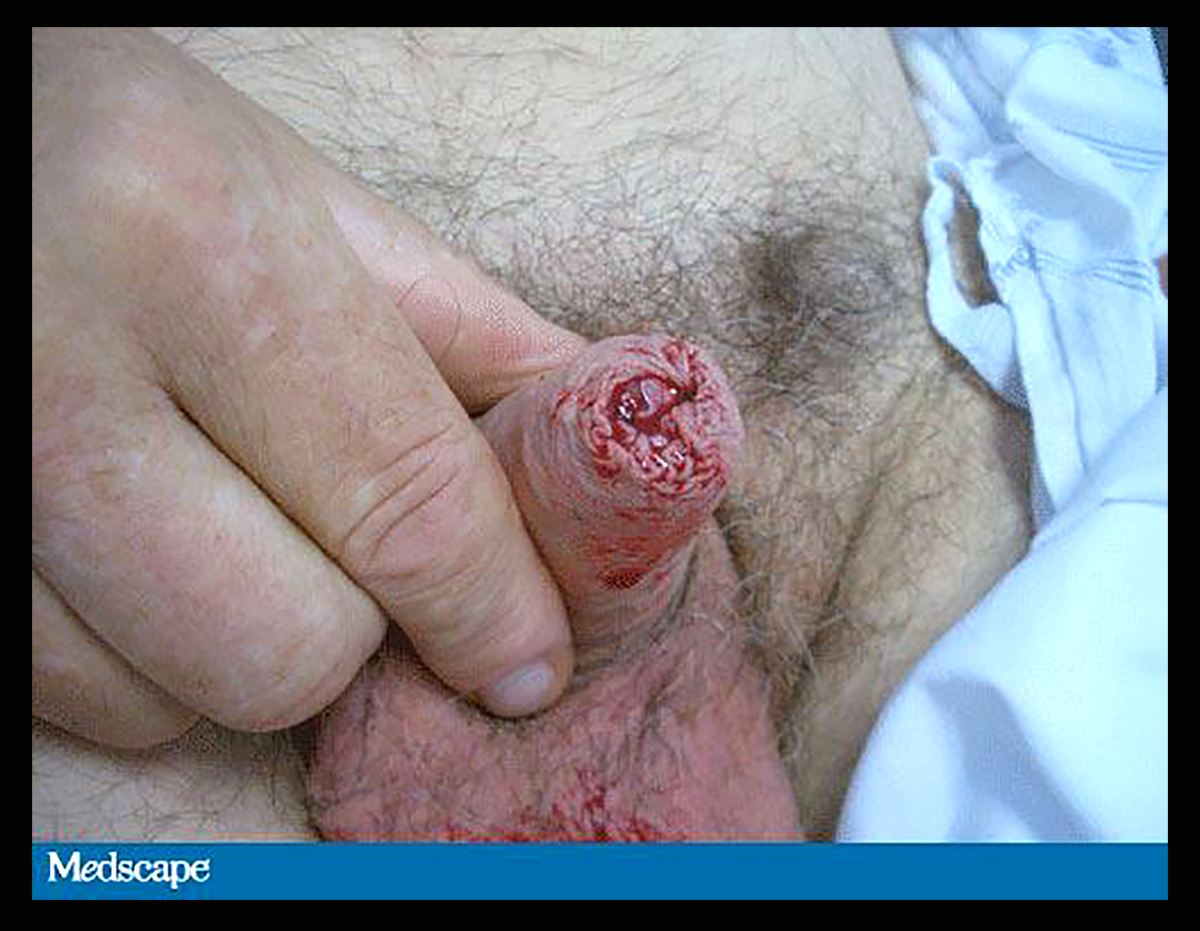

























![Les Fenêtres [Windows] par Robert_Delaunay (1912)](https://dpurb.com/wp-content/uploads/2018/11/les-fenc3aatres-windows-par-robert_delaunay-1912.jpg)













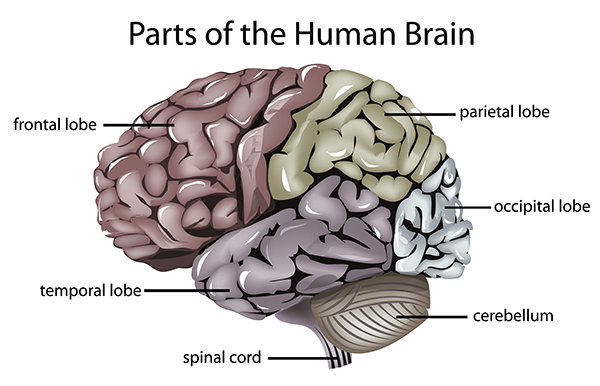 It has been noted that those with frontal lobe area damage often continue to sort according to only one particular sorting principle for 100 or more trials even after the principle has been deemed as incorrect (Demakis, 2003). The ability to correctly remember new instructions with for effective behaviour is near impossible for those with brain damage: a problem known as ‘perseveration’.
It has been noted that those with frontal lobe area damage often continue to sort according to only one particular sorting principle for 100 or more trials even after the principle has been deemed as incorrect (Demakis, 2003). The ability to correctly remember new instructions with for effective behaviour is near impossible for those with brain damage: a problem known as ‘perseveration’.